
Case Report
Austin J Clin Neurol 2016; 3(1): 1088.
Multiple Enhancing Brain Mass as Initial Presentation of Varicella Zoster Virus Encephalitis
Schmidt E, Yonaty SA, Jubelt B and Latorre JG*
Department of Neurology, SUNY Upstate Medical University Hospital, USA
*Corresponding author: Latorre JG, Department of Neurology and Neurosurgery, Neurocritical Care Service, SUNY Upstate Medical University Hospital, 750 East Adams Street, Syracuse, NY 13210, USA
Received: July 01, 2016; Accepted: August 06, 2016; Published: August 08, 2016
Abstract
Viral encephalitis causes a myriad of neurologic symptoms that can mimic many acute central nervous system disorders. The clinical manifestation is dependent on a number of factors including the predominant cell types affected by the virus or viral tissue tropism, the virulence of the virus and the localization of the infection to a particular brain region. For instance, Herpes simplex virus (HSV) tends to localize to the mesial temporal and orbitofrontal lobes and presents with characteristic clinico-pathologic and imaging findings. Varicella Zoster Virus (VZV) is an exclusively neurotropic human virus which produces an initial infection typically in childhood– chickenpox, followed by dormant persistence in the ganglionic neurons. Reactivation of the virus, most commonly in immunocompromised patients but also in immunocompetent individuals typically produces “shingles”, a painful vesicular rash in a dermatomal area. Most recently, the entity of neurological complications of VZV reactivation, in absence of a skin rash has been recognized. What makes this virus stand out is its unique ability of replication in the arteries, with resultant vasculopathy, affecting both large and small vessels, manifesting clinically and radiologically as acute ischemic or hemorrhagic infarction. We present an atypical manifestation of VZV encephalitis mimicking a metastatic brain tumor, with unusual pathological findings.
Keywords: Varicella; Encephalitis; Tumor; Metastatic; PCR
Abbreviations
VZV: Varicella Zoster Virus; HSV: Herpes Simplex Virus; CSF: Cerebral Spinal Fluid; CMV: Cytomegalo Virus; EBV: Epstein Barr Virus; HHV 6: Human Herpes Virus 6; WNV: West Nile Virus; EEEV: Eastern Equine Encephalitis Virus; SLE: St. Louis Encephalitis; IgG: Immunoglobulin G; PCR: Polymerase Chain Reaction
Case Presentation
A 42 year old African American woman with history of hypertension presented with 1-week complaints of nausea and vomiting. She later developed headache, photophobia, vertigo, diplopia and neck stiffness prompting admission to a local hospital. Initial brain imaging showed multiple enhancing brain lesions within the right periventricular region, the bilateral cerebellar peduncles and the right lateral medulla (Figure 1). The patient was transferred to our hospital in August 2010 for an elective brain biopsy after a negative metastatic tumor work-up.
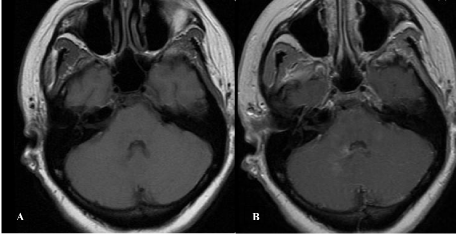
Figure 1: T1 (A) and T1 (B) with gadolinium sequences on the outside MRI
brain, showing enhancement in the bilateral cerebellar peduncles.
At the time of transfer, examination showed an obese woman with normal alertness and orientation. She had gaze-evoked nystagmus, limited upward gaze and bilateral upper extremity ataxia. Within the first few days of the hospital stay, she developed fever. As part of the infectious work-up, lumbar puncture was done, on day 3 of hospitalization in our institution. Cerebral Spinal Fluid (CSF) study showed normal glucose (42 mg/dL), high protein (82 mg/dL) and elevated white cell count (1050/mm3) with 54% polymorphonuclear cells, while red cell count was at a low 2/mm3. Cytology was negative for malignancy. While waiting for brain biopsy, she developed progressive confusion leading to stupor. Repeat brain imaging on day 5 showed cerebellar herniation, hydrocephalus and increasing mass effect, prompting emergent posterior decompressive craniectomy (Figure 2 and 3). Her symptoms improved after surgery. Brain tissue pathology showed perivascular lymphocytosis and florid lymphohistiocytic infiltration of the cerebellum and focal necrosis. Majority of the lymphocytes were CD3+ T cells, with a paucity of B cells, which favored an inflammatory process rather than lymphoma. No tumor cells were identified. There was no accompanying vasculitic or granulomatous component, or any viral cytopathic effects. Although there was myelin loss in areas of histiocytic infiltration, the impression was not of a selectively demyelinating process. Additional testing of the brain tissue included PCR for HSV, 1 and 2, CMV, VZV, EBV, HHV6, Adenovirus, WNV, EEE, SLE and Enterovirus, all negative. Fluorochrome stain did not show any acid fast bacilli and bacterial culture was negative. After two weeks of incubation, Varicella zoster virus was isolated from viral culture. The original CSF and 3 subsequent CSF samples done post operatively during her over 2 months prolonged hospital stay were negative for VZV PCR. The serum Varicella IgG antibody was positive.
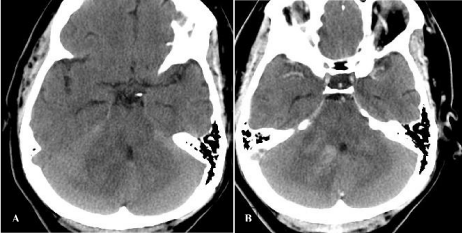
Figure 2: CT head without (A) and with contrast (B) showing enhancing
lesion within the right cerebellar peduncle with surrounding edema, creating
mass effect on the 4th ventricle and the quadrigeminal cisterns.
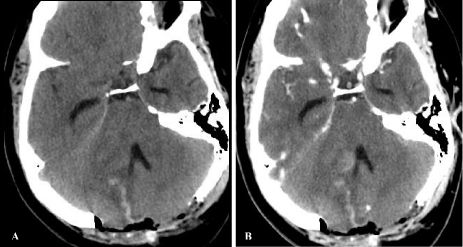
Figure 3: CT head without (A) and with contrast (B) showing post-surgical
changes after posterior suboccipital decompression craniectomy, including
hemorrhage in the surgical tract with persistent enhancement in the right
cerebellar peduncle.
The patient denied any skin rash prior to hospitalization, although the whole body bone scan report showed increased uptake in the mandible and maxillary areas, thought to be related to recent oral ulcerations. Further investigation did not show any immune deficiency, including a negative HIV test. The patient was treated with acyclovir i.v., at 10mg/kg/dose, Q8hrs for 6 weeks and was eventually discharged to rehabilitation with residual ataxia.
Discussion
Multiple enhancing mass lesions mimicking a metastatic brain cancer may be a rare manifestation of viral encephalitis. Unless clinically suspected, the management of viral encephalitis in patient with enhancing brain lesion may be delayed and complicated by unnecessary diagnostic testing. More importantly, the delay in institution of potentially lifesaving antiviral therapy may lead to death or permanent neurological sequelae. Review of literature revealed a number of reports of HSV [1,2] and EBV [3,4] encephalitis presenting as brain tumor or brain tumor progression [5,6]. Majority of patients are immunocompromised although immunocompetent hosts have been reported [7-9]. To our knowledge, this is the first described case of Varicella zoster encephalitis mimicking metastatic brain cancer in an immunocompetent patient.
One remarkable case was reported recently, describing a previously healthy young man who developed, about 6 months after varicella vaccination, a single left temporal mass which tested positive for VZV immune-staining [9]. Further DNA analysis revealed wild type strain, leading the investigators to believe that the recent prior vaccination was merely coincidental, as patient did have exposure to varicella via his sister, at 6 months of age.
Notably, one other case report described a previously healthy middle-aged man with rapid onset of coma, found to have multiple bilateral hemorrhagic lesions with enhancement, in addition to intraventricular and subarachnoid hemorrhages [8]. In one more recent case report, an immunocompromised female, previously diagnosed and treated for cerebral toxoplasmosis, was reported to have new multiple hemorrhagic and gadolinium enhancing lesions, mimicking recurrence of Toxoplasmosis, while CSF tested positive for VZV PCR [10]. The enhancement noted in these cases is not surprising in setting of hemorrhagic lesions.
Our case provides a few new insights into the pathophysiology and natural behavior of this virus, in an immunocompetent host. Because of the natural ability of the VZV to infect both large and small intracranial arteries, the resulting vasculopathy is naturally considered to be responsible for the unifocal or multifocal ischemic or hemorrhagic infarctions, and the subsequent clinical manifestations commonly found in VZV encephalitis. This is the reason why even the term “encephalitis” is challenged, in favor of the term “vasculopathy” [11].
In our patient’s case, at pathological level, there was no evidence of a vasculitic process; however, there were significant peri-vascular inflammatory changes, which likely affected the blood brain barrier, resulting in positive gadolinium enhancement on MRI. It is probably because of the same lack of vasculitic process that the imaging studies did not show any hemorrhagic lesions. The vasogenic and cytotoxic edema resulting from inflammation as well as tissue necrosis potentially from direct viral infection in the tight posterior fossa in our patient led to the rapid deterioration due to acute intracranial hypertension, prompting emergent decompressive craniectomy that ultimately led to the definitive diagnosis. It is notable that during the subsequent testing, the brain tissue sample and the CSF samples tested negative for VZV PCR, underlying the limitations of the PCR testing (less than 100% sensitive). Alternatively, the negative results may suggest positive response to therapy.
This report expands the range of clinical presentation that may be associated with Varicella zoster encephalitis to warrant empiric antiviral therapy. We also stress the value of brain biopsy, the limitation of viral DNA PCR testing and the utility of viral culture in the diagnosis and definitive management of multiple brain lesion of unclear etiology.
Conclusion
- Multiple enhancing brain lesions may be a manifestation of Varicella zoster encephalitis.
- Viral DNA PCR may be negative in CSF especially in cases with minimal or no meningeal involvement.
- Brain biopsy in selected patients may aid in the diagnosis and definitive treatment.
- Although the yield is low, viral culture should always be done as part of the complete work-up.
- Rose JW, Stroop WG, Matsuo F, Henkel J. Atypical herpes simplex encephalitis: clinical, virologic, and neuropathologic evaluation. Neurology. 1992; 42: 1809-1812.
- Fiol M, Mora A, Cervio A, Romero C, Taratuto A, Sevlever G, et al. Brain tumor or infectious disease? Arq Neuropsiquiatr. 2009; 67: 302-304.
- Angelini L, Bugiani M, Zibordi F, Cinque P, Bizzi A. Brainstem encephalitis resulting from Epstein-Barr virus mimicking an infiltrating tumor in a child. Pediatr Neurol. 2000; 22: 130-132.
- Khalil M, Enzinger C, Wallner-Blazek M, Scarpatetti M, Barth A, Horn S, et al. Epstein-Barr virus encephalitis presenting with a tumor-like lesion in an immunosuppressed transplant recipient. J Neurovirol. 2008; 14: 574-578.
- Lins H, Kanakis D, Heinrichs T, Dietzmann K, Wallesch CW, Mawrin C. Sudden progression of a glioblastoma in partial remission? Clin Neurol Neurosurg. 2004; 106: 335-336.
- Perez-Saldana MT, Vilar C, Geffner-Sclarsky D, Belenguer-Benavides A, Del Villar-Igea A, Gil-Fortuno M, et al. Meningoencephalomyelitis as the initial symptom of a brain tumour mimicking encephalitis due to herpes simplex virus: a case report. Rev Neurol. 2007; 44: 348-352.
- Kleinschmidt-DeMasters BK, Amlie-Lefond C, Gilden DH. The patterns of varicella zoster virus encephalitis. Hum Pathol. 1996; 27: 927-938.
- Mpaka M, Karantanas AH, Zakynthinos E. Atypical presentation of varicellazoster virus encephalitis in an immunocompetent adult. Heart Lung. 2008; 37: 61-66.
- Halling G, Giannini C, Britton JW, Lee RW, Watson RE, Terrell CL, et al. Focal encephalitis following varicella-zoster virus reactivation without rash in a healthy immunized young adult. J Infect Dis. 2014; 210: 713-716.
- Marques IB, Flanagan S, Noble H, Giovannoni G, Marta M. Varicella-zoster virus encephalitis mimicking toxoplasmosis relapse. Neurol Neuroimmunol Neuroinflamm. 2015; 2: e74.
- Gilden D, Cohrs RJ, Mahalingam R, Nagel MA. Varicella zoster virus vasculopathies: diverse clinical manifestations, laboratory features, pathogenesis, and treatment. Lancet Neurol. 2009; 8: 731-740.
References