
Research Article
Austin J Clin Neurol 2018; 5(1): 1131.
Non-Compliance with Follow-up Visits: Analysis of the First Year of Patient’s Attendance to a Second Level Headache Centre in Italy
Catarci T*
Azienda Sanitaria Locale Roma1, Presidio Luzzatti Headache Centre, Rome, Italy
*Corresponding author: Catarci T, Outpatient Clinic ASL Roma1, Rome, Italy
Received: April 19, 2018; Accepted: May 15, 2018; Published: June 12, 2018
Abstract
The management of headache patients is a complex process where many factors may play a crucial role, as for example, the compliance with followup visits. In order to monitor the first 12 months of activity of our secondary headache outpatient clinic, we have analysed the dropout frequency after the first visit. We retrospectively analysed 101 consecutive case records and found a drop-out rate of 45% (12 males, 33 females, mean age 38 ± 13 years, 39% foreigners), mostly not attending the first follow-up visit (74%) and suffering from chronic headache (60%). Migraine without aura was diagnosed in 56% of the patients while neither trigeminal autonomic cephalalgias nor secondary headache was suspected. We conclude that, even though our drop-out rates are similar to those already reported in the licterature and probably due to headache severity and/or language barriers, still we ought to improve in order to deliver better standards of headache care.
Keywords: Headache care; Dropout rates; Patient’s management
Introduction
The management of headache patients is a complex process that includes many variables such as patient-clinician relationship, complete history collection, general and neurological examination and last, but not least, timely schedule of follow-up visits [1].
Recently, a multidimensional definition of quality of headache care has been proposed, where the following criteria ought to be achieved: accurate diagnosis and individualised management, appropriate referral pathways, education of patients about their headache and their management, convenience and comfort, patient’s satisfaction, efficiency and equitability, outcome assessment and safety [2]. Moreover, in order to make a correct headache diagnosis, all patients seen for the first time should be given a follow-up visit after a short period of time (normally no more than two months) in order to check headache diary and eventually be treated with preventive medications. Such interval should be even shorter in case the patients suffer from chronic headache with or without medication overuse.
Therefore, non-compliance with the first follow-up visit can be an important barrier to optimal management of headache patients and contribute to inappropriate multiple uses of other healthcare services.
In order to study this possible caveat concerning correct management of our patients, we analysed the dropout frequency after the first visit, during the very first year of activity of our headache outpatient clinic.
Methods
The outpatient clinic opened on October 2014 as a public secondary headache care centre, within the Azienda Sanitaria Locale (Regional Health Service of Lazio) in the city centre of Rome, Italy. One day per week was dedicated to the visits (on Thursdays); staff included an acceptance nurse and a Neurologist with headache specialty (TC). Follow-up visits were scheduled by the nurse, following the clinician indication and in agreement with the patient.
We retrospectively analysed daily worksheets and case records of the 101 consecutive patients where follow up visits had been scheduled within the next year (that is until October 2015) in order to pick up those who did not present at follow-up. The following data where then gathered: diagnosis [3] and headache attacks frequency, type of dropout (at first follow-up or later, later follow-up visit after one drop-out), time scheduled for follow-up visit (1, 2 or more than 2 months).
Results
Forty-six patients did not return for follow-up visit out of 101 (45%), 12 males, 34 females mean age 38 + 13 years, 18 out of 46 (39%) where not Italian. Fourteen patients (30%) did not return at first scheduled follow-up visit and were lost, 20 (43%) returned within one year, 10 (22%) returned at first follow-up but failed to return at the second and were subsequently lost. Therefore, 24/46 (52%) patients were totally lost at some time during one year time.
Headache frequency was more than 15 days per month in 29/46 patients (60%). Headache diagnosis was possible to be done in all but two patients and none was suspected to have secondary headache. Twenty-six out of 46 patients (56%) had migraine without aura see Figure 1 for all diagnosis. Fourteen out of 46 patients (30%) had been asked to return for follow-up after one month, 20/46 (41%) after two months and 10/46 (22%) after more than 2 months (Figure 2). We decided to analyse also the distribution of patients’ dropout, considering a specific time period during the year and calculated the ratio between number of dropouts and number of sessions per month. It was found that the months where most of the patients failed to return for follow-up visits were May, July, September and October with a ratio bigger than 1 while March and November had a ratio equal to 0.5 (Figure 3).

Figure 1: Diagnosis of headaches in 46 patients who were not compliant with
follow-up visits.
MWoA: Migraine Without Aura; MWA: Migraine With Aura; PROB: Probable
Migraine; TTH: Tension Type Headache; TAC: Trigeminal Autonomic
Cephalalgia
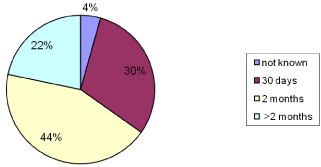
Figure 2: Length of scheduled follow-up.
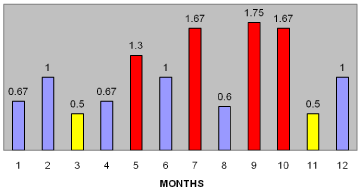
Figure 3: Distribution of patients’ drop-out considering (Ratio between
number of drop-outs and number of sessions per month).
Discussion
Our second level headache centre had a dropout rate of 45%, mostly at first follow-up visit (74%). A previous study performed on 316 consecutive patients of a third level headache centre in Boston, reported a similar rate of 40% where reasons for the non-compliance (through a telephone interview) most frequently mentioned were dislike of the clinician and seeking care elsewhere [4].
We did not enquire our patients about reason of not presenting at follow-up visits, but we can speculate possible contributing factors by analysing the clinical features of the patients. In fact, the majority of the non-compliant patients had chronic headache (60%) and more than one third where foreigners. In addition, the majority of followup visits had been scheduled at two months and most patients did not come back on months with hot weather in Italy, like July and September.
Therefore, we feel that cultural and language barriers might have played and important role together with disability due to chronic headache, but we cannot exclude a sub-optimal clinician-patients relationship, since most of the non-compliance to follow-up was at first visit.
One limit of the present study is that we did not consider the distance that the dropout patients had to travel to reach our centre. In fact, public transport in Rome is far from being efficient and car traffic can be extremely chaotic, not to mention the frequent occasions of strikes.
In conclusion the dropout rate of follow-up visits of our centre was similar to that previously reported in another study; still the figures are quite high if we aim at delivering a good standard of headache care. A recent study evaluated several indicators to measure headache quality of care in 3rd level headache centres in Europe and found, among other improvable factors, that there were restricted opportunities for follow-up visits [5]. In our opinion it is critical to keep dropout rates at follow-up visits low, particularly in second level headache centres, since third level centres should be mostly devoted to diagnosis and management of difficult cases.
References
- Sances G, Catarci T. Management of headache patients. G. Nappi and M. Moskowitz editors. In: Handbook of Clinical Neurology: Headache volume. Elsevier. 2010; 127-135.
- Peters M, Perera S, Loder E, Jenkinson C, Gouveia RG, Jensen R, et al. Quality in the provision of headache care. 1: systematic review of the literature and commentary. J Headache Pain. 2012; 13: 437-447.
- The International Classification of Headache Disorders, 2nd edition. Cephalalgia 2004;24:1-160.
- Spierings EL, Miree LF. Non-compliance with follow-up and improvement after treatment at a headache center. Headache. 1993; 33: 205-209.
- Schramm S, Uluduz D, Gouveia RG, Jensen R, Siva A, Uygunoglu U et al. Headache service quality: evaluation of quality indicators in 14 specialist-care centres. J Headache Pain. 2016; 17: 111.