Case Report
Austin J Clin Ophthalmol. 2014;1(6): 1027.
A Case of Scleritis Associated with Immunoglobulin G4-Related Aseptic Meningitis
Fukuyama H, Hashida N* and Nishida K
Department of Ophthalmology, Osaka University Graduate School of Medicine, Japan
*Corresponding author: Hashida N, Department of Ophthalmology, Osaka University Graduate School of Medicine, E7, 2-2 Yamadaoka, Suita, Osaka, 565-0871, Japan
Received: June 20, 2014; Accepted: July 18, 2014; Published: July 21, 2014
Abstract
Purpose: The aim of this study was to report a case of scleritis associated with immunoglobulin G4 (IgG4)-related aseptic meningitis.
Case report: A 63-year-old man, who was referred to our clinic with refractory uveitis, presented initially with severe headache, fever and ocular inflammations. Slit-lamp examination revealed bilateral scleritis, an increase of scleral thickness was also observed by anterior segment optical coherence tomography (CASIA SS-1000, Tomey, Japan). After the investigation for a fever of unknown origin, IgG4-related aseptic meningitis was diagnosed with a cerebrospinal fluid (CSF) examination and bone marrow biopsy. After the definite diagnosis, the patient was treated with oral prednisolone (initial dose 30 mg/day). After the treatments, all symptoms including inflammation of the sclera, headache, and laboratory data were improved. The scleral thickness also decreased markedly. With treatment, ocular inflammation was controlled during the following 7 months, but the scleritis recurred during steroid tapering. Currently, the patient continues to be followed untreated without complications.
Conclusion: The clinical findings of ocular inflammation strongly suggested scleritis in this patient. To our knowledge, this is the first report of scleritis associated with IgG4-related aseptic meningitis. It is necessary to consider the IgG4-related disease as a differential diagnosis of scleritis.
Keywords: Scleritis; Immunoglobulin IgG4; Meningitis
Introduction
IgG4-related disease (IgG4-RD) is an unknown disease entity characterized by elevated serum IgG4 concentration, tumefaction, a dense lymphoplasmacytic infiltrate rich in IgG4-positive plasma cells, storiform fibrosis, obliterative phlebitis, mild to moderate eosinophilic, and elevated serum IgG4 levels [1]. IgG4-RD can affect almost any organ: the biliary tract, salivary glands, per orbital tissues, kidneys, lungs, lymph nodes, meninges, aorta, breast, prostate, thyroid, pericardium, and skin.
Diagnosis of IgG4-RD is based on identification of a combination of reported histologic patterns and increased numbers of IgG4 polyclonal plasma cells [2]. The underlying pathologic mechanism of IgG4-RD is unclear; however, enriched lymphoplasmacytic infiltration of IgG4-positive plasma cells, fibrosis in the involved organs, and elevated levels of serum IgG4 were thought to be involved in the pathogenesis. Glucocorticoid had been shown to have clinical efficacy [3,4]. Despite a good response to steroid therapy, the lesion often recurs during steroid tapering or following the withdrawal of steroid treatment [4,5] Rituximab (an anti-CD20 monoclonal antibody) has also been effectively used in patients with refractory to corticosteroids and immunosuppressive agents [5].
Mikulicz’s disease, characterized by swelling of lacrimal and salivary glands, has been identified as part of the spectrum of IgG4- RD [6,7]. Since then, many studies on IgG4-RD in the ophthalmic region have focused to a large extent on the lacrimal gland. However, IgG4-RD has been reported to affect several ophthalmic region not only the lacrimal gland but also other ocular adnexa, such as extraocular muscles, branches of the trigeminal nerve [8- 11]. Ocular manifestations of IgG4-RD are reported to as external ophthalmoplegia, ptosis, exophthalmos, intraocular pressure elevation, and ophthalmalgia.
IgG4-RD also involves the sclera, it occurs bilaterally and presents with anterior chamber inflammation in middle age [12,13]. The prognosis is good, because systemic rituximab and steroid have been reported to well control ocular inflammation [13,14], however; its etiology still remained to be elucidated. There are few cases which IgG4-RD caused scleritis [13,15]. However, to the best of our knowledge, there is no report of scleritis associated with IgG4-related aseptic meningitis. In the current study, we report and discuss a rare association with these diseases.
Case Presentation
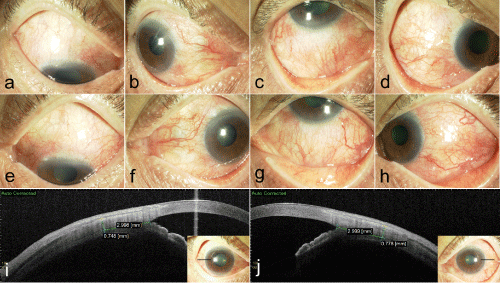
The patient was a 63-year-old man with 1 month history of refractory uveitis and consulted a local ophthalmologist. He was diagnosed with scleritis and referred to our department. At first visit, he complained of severe headache, fever, blurred vision and bilateral inflamed eyes. There was no previous ophthalmic history and his general health was good. His best corrected visual acuity (BCVA) was 1.2 bilaterally and his intraocular pressures were normal. A slit-lamp examination revealed bilateral conjunctival/ciliary injection, scleritis, and 2+ anterior chamber cells (Figure 1a, b). Increase of scleral thickness was observed by anterior segment optical coherence tomography (AS-OCT) (CASIA SS-1000, Tomey, Japan) (Figure 1c). According to the previous report, the mean scleral thickness of forty normal healthy controls was 0.53±0.08 mm [16].
Figure 1 : Slitlamp photograph of the right eye (a-d) and left eye (e-h) showing engorged episcleral and scleral vessels. The sclera was imaged 3 mm from the detected scleral spur using an AS-OCT system (CASIA SS-1000, Tomey, Japan) showing the increase of temporal scleral thickness of the right eye (i) and left eye (j).
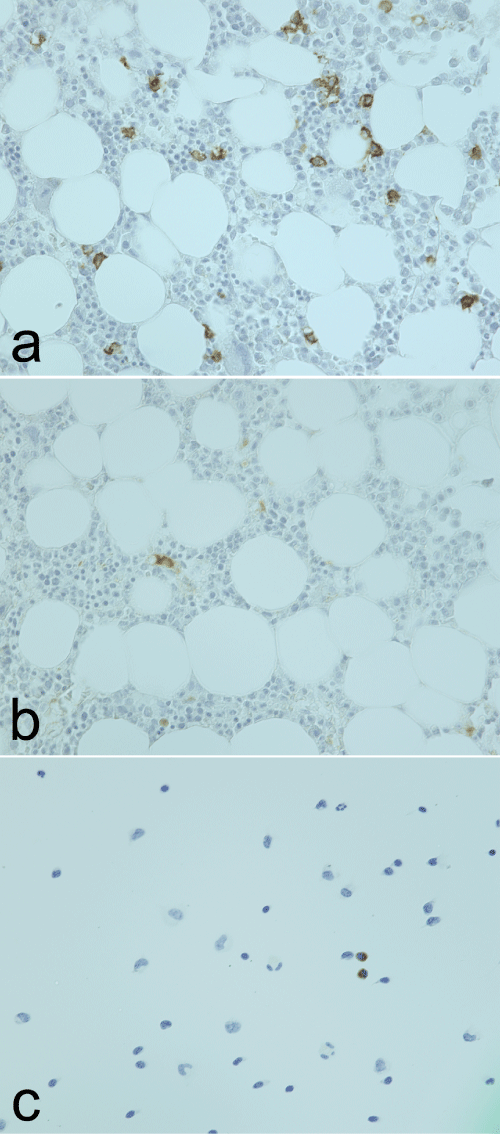
On peripheral blood tests, erythrocyte sedimentation rate and C-reactive protein were elevated. Serum autoantibody was all negative. There was no finding suggestive of inflammatory diseases and tuberculosis. And, there were no findings in head MRI, chest X-ray, and computed tomography. In spite of intensive examination, the etiology of the disease remained unclear. He was admitted into our hospital to investigate the cause of headache and unidentified fever. A cerebrospinal fluid (CSF) examination showed negative viral antibodies, increased protein concentration, lymphocytic pleocytosis, and presence of eosinophils. Hematological examination shows elevated serum IgG4 concentrations; histopathologic examination of bone marrow shows the fibrosis and infiltrations of IgG4-positive plasma cells (Figure 2), thus the patient was diagnosed with IgG4- related aseptic meningitis according to the diagnostic criteria [1].
Figure 2 : Histopathological analyses at 40X. (a) Immunohistochemistry for CD138, marker characteristically positive for plasma cells, shows numerous positive cells in bone marrow biopsy. (b) IgG4 immunohistochemistry demonstrating IgG4 positive plasma cells in bone marrow. (c) Immunohistochemical staining for IgG4 in spinal fluid showing strong staining in plasma cells.
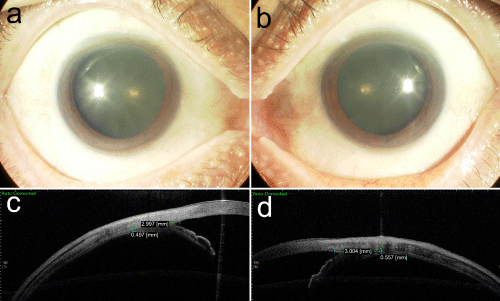
Initially, the patient was treated with topical steroids for eye symptom, but there was no improvement. After the definite diagnosis, the patient was treated with oral prednisolone (initial dose 30 mg/ day). After the treatments, all symptoms including inflammation of the sclera and laboratory test results were improved (Figure 3). Two months after the therapy, systemic signs of inflammation and scleritis were alleviated, accompanied by reduction of serum IgG4 concentration to normal range. Unexpectedly, after seven months, headache, tinnitus and scleritis reappeared and systemic steroid was resumed, resulting in lesion and symptom control after ten months. At the last examination after sixteen months of follow-up, the BCVA was 1.5 with no evidence of active inflammation. The patient continues to be followed untreated without complications.
Figure 3 : Slitlamp photograph of the right eye (a,) and left eye (b) after the treatment, showing the local control of ocular inflammation. The sclera was imaged 3 mm from the detected scleral spur using an AS-OCT system, showing the significant decrease of temporal scleral thickness of the right eye (c) and left eye (d).
Discussion
IgG4-RD is a novel clinical disease entity characterized by elevated serum IgG4 concentration and tumefaction or tissue infiltration by IgG4-positive plasma cells. The diagnosis of IgG4-RD is based upon biopsy findings demonstrating the characteristic histopathologic findings and immune histological staining. A diagnosis of IgG4-RD is definitive in patient with clinical examination showing characteristic diffuse/localized swelling or masses in single or multiple organs, elevated serum IgG4 concentrations, and marked lymphocyte and/or plasmacyte infiltration and fibrosis and infiltration of IgG4-positive plasma cells [1]. It is significant for the diagnosis of IgG4-RD to confirm swelling or thickening the affected lesions. In the current case, we could observe the thickening of the sclera by using AS-OCT, the increase of eosinophils and infiltrations of IgG4-positive plasma cells in the cerebrospinal fluid, elevated serum IgG4 concentrations, and histological findings. Many systemic diseases such as rheumatoid arthritis, ANCA-associated vasculitis, and systemic lupus erythematosus had been reported to cause scleritis [17]. Moreover, there are a few reports of scleritis caused by IgG4-RD. However; to the best of our knowledge, this is the first report of scleritis associated with IgG4-RD aseptic meningitis.
Glucocorticoids are typically the first line of therapy for IgG4- RD. Most patients respond well to oral glucocorticoid within several weeks [5], but the lesion sometimes recurs during tapering of steroid. For patients with recurrent or refractory IgG4-RD, B-cell depletion with rituximab has also been a useful approach [13,14]. And there is report of successful use of rituximab in a patient with IgG4-RD and refractory scleritis [12]. At first, we speculated that topical steroids only cannot prevent production of IgG4 because immunological reactions in bone marrow caused ocular inflammation. Therefore, we treated with topical steroids only for eye symptoms not to prevent intensive examination, but there was no improvement. After the definite diagnosis and starting treatment with systemic steroids, the improvement of symptoms including inflammation of sclera and laboratory test results was achieved.
Pathologically, IgG4-RD is reported be caused by T helper (Th2)- cells immune responses stimulated with autoimmunity and infectious agents. In addition to Th2-cells, activation of regulatory T cells (Treg) is also characteristic of IgG4-RD. Interleukin (IL)-4, 5, 10, 13, and transforming growth factor β (TGF-β) are over expressed through an immune reactions. These cytokines activate B cells, eosinophils, and fibroblasts which contribute to the eosinophilia, elevated serum IgG4, Ig E concentrations, and progression of fibrosis [5]. Meanwhile, pathogenesis of scleritis is reported to be caused by autoimmunity and infectious agents as well as IgG4-RD. Cytokines and chemokines produced by dendritic cells (DCs) attract T cells and B cells, and involved in the pathogenesis. IL-8, 17, 23, and TNF-α are produced and activate immune reaction. T cells, plasma cells, macrophages, DCs and fibroblasts localized in the sclera could release tissue-destructive matrix metalloproteinase (MMP) and inhibit tissue inhibitor of matrix metalloproteinase (TIMP), resulting in tissue destruction [17]. Concerning the pathogenesis of diseases, both diseases share the same mechanisms of immunological reactions such as the activation of T and B cells. It is likely that elevation of eosinophils followed by increases of Th2 and Treg cells in IgG4-related aseptic meningitis lead to the activation of T and B cell and caused severe scleritis in this patient.
In conclusion, we here report the first case of scleritis associated with IgG4-related aseptic meningitis. And it suggests that there is something in common immune mechanisms between IgG4-RD and scleritis.
References
- Umehara H, Okazaki K, Masaki Y, Kawano M, Yamamoto M, Saeki T, et al. Research Program for Intractable Disease by Ministry of Health, Labor and Welfare (MHLW) Japan G4 team: A novel clinical entity, IgG4-related disease (IgG4RD): general concept and details. Mod Rheumatol. 2012; 22: 1-14.
- Kamisawa T, Okazaki K, Kawa S, Shimosegawa T, Tanaka M. Research Committee for Intractable Pancreatic Disease and Japan Pancreas Society: Japanese consensus guidelines for management of autoimmune pancreatitis. III. Treatment and prognosis of AIP. J Gastroenterol. 2010; 45: 471-477.
- Sato Y, Ohshima K, Ichimura K, Sato M, Yamadori I, Tanaka T, et al. Ocular adnexal IgG4-related disease has uniform clinicopathology. Pathol Int. 2008; 58: 465–470.
- Khosroshahi A, Carruthers MN, Deshpande V, Unizony S, Bloch DB, Stone JH. Rituximab for the treatment of IgG4-related disease: lessons from 10 consecutive patients. Medicine (Baltimore). 2012; 91: 57-66.
- Stone JH, Zen Y, Deshpande V. IgG4-related disease. N Engl J Med. 2012; 366: 539-551.
- Yamamoto M, Ohara M, Suzuki C, Naishiro Y, Yamamoto H, Takahashi H, et al. Elevated IgG4 concentrations in serum of patients with Mikulicz's disease. Scand J Rheumatol. 2004; 33: 432-433.
- Yamamoto M, Harada S, Ohara M, Suzuki C, Naishiro Y, Yamamoto H, et al. Clinical and pathological differences between Mikulicz's disease and Sjögren's syndrome. Rheumatology (Oxford). 2005; 44: 227-234.
- Kubota T, Moritani S, Katayama M, Terasaki H. Ocular adnexal IgG4-related lymphoplasmacytic infiltrative disorder. Arch Ophthalmol. 2010; 128: 577-584.
- Wallace ZS, Khosroshahi A, Jakobiec FA, Deshpande V, Hatton MP, Ritter J, et al. IgG4-related systemic disease as a cause of ‘‘idiopathic’’ orbital inflammation, including orbital myositis, and trigeminal nerve involvement. Surv Ophthalmol. 2012; 57: 26–33.
- Mehta M, Jakobiec F, Fay A. Idiopathic fibroinflammatory disease of the face, eyelids, and periorbital membrane with immunoglobulin G4-positive plasma cells. Arch Pathol Lab Med. 2009; 133: 1251-1255.
- Japanese study group of IgG4-related ophthalmic disease. A prevalence study of IgG4-related ophthalmic disease in Japan. Jpn J Ophthalmol. 2013; 57: 573-579.
- Caso F, Fiocco U, Costa L, Sfriso P, Punzi L, Doria A. Successful use of rituximab in a young patient with immunoglobulin G4-related disease and refractory scleritis. Joint Bone Spine. 2014; 81: 190-192.
- Ohno K, Sato Y, Ohshima K, Takata K, Ando M, Abd Al-Kader L, et al. IgG4-related disease involving the sclera. Mod Rheumatol. 2014; 24: 195-198.
- Khosroshahi A, Bloch DB, Deshpande V, Stone JH. Rituximab therapy leads to rapid decline of serum IgG4 levels and prompt clinical improvement in IgG4-related systemic disease. Arthritis Rheum. 2010; 62: 1755-1762.
- Wallace ZS, Deshpande V, Stone JH. Ophthalmic manifestations of IgG4-related disease: Single-center experience and literature review. Semin Arthritis Rheum. 2014; 43: 806-817.
- Hashida N, Nishida K. Anterior-segment optical coherence tomography findings in eyes with scleritis. ARVO 2014 annual meeting; 2014, May 4-May 8; FL, USA, 2014.
- Wakefield D, Di Girolamo N, Thurau S, Wildner G, McCluskey P. Scleritis: Immunopathogenesis and molecular basis for therapy. Prog Retin Eye Res. 2013; 35: 44-62.