
Research Article
Austin J Clin Ophthalmol. 2019; 6(1): 1100.
Topical Ketolorac is Effective and Safe for Post- Vitrectomy Surgery Treatment
Ching J1,3, Iqbal T² and Saidkasimova S¹*
¹Department of Ophthalmology, Norfolk and Norwich University Hospital, Norwich, UK
²Norwich Medical School, University of East Anglia, Norwich, UK
³John Van Geest Centre for Brain Repair, E.D. Adrian Building, Cambridge, CB2 0PY, UK
*Corresponding author: Shohista Saidkasimova, Department of Ophthalmology, Norfolk and Norwich University Hospital, Norwich, NR4 7UJ, UK
Received: December 05, 2018; Accepted: January 23, 2019; Published: January 30, 2019
Abstract
Purpose: The aim of this study was to assess the efficacy of the nonsteroidal topical drug monotherapy on post-vitrectomy clinical recovery.
Methods: Retrospective analysis of case notes and post-operative Optical Coherence Tomography (OCT) of 128 eye of 128 consecutive patients undergoing primary vitrectomy for primary rhegmatogenous retinal detachment (RRD) [n = 72], full thickness macular hole (MH) [n = 42], and epi-retinal membrane (ERM) [n = 15] at a single tertiary centre between 2011 and 2015.
Results: Average LogMAR best-corrected visual acuity improved from 1.04 at baseline to 0.68 (95% CI 0.14 to -0.54, p = 0.001) at 20 weeks follow up for all indications. Average IOP did not change at follow up. Central retinal thickness (CRT) on OCT assessment did not change significantly in RRD patients postoperatively but reduced significantly in patients with MH from 389.81μm at baseline to 295.85μm at 20 weeks follow up compared to baseline (p< 0.0001). Patients with ERM had a significant reduction in CRT from 476.71μm at baseline to 388.86μm at 12 weeks (p < 0.05).
Post-operative CMO was detectable on OCT in 3 of 72 patients with RRD, 1 of 43 patients with MH and 2 of 15 patients with ERM. Overall, 6 (4.7%) patients were found to have post-operative CMO. There were few complications including 6 (4.0%) patients with persistent post-operative CMO requiring treatment beyond 20 weeks follow-up.
Conclusion: Topical ketorolac alone is an effective and safe post-operative therapy following vitrectomy surgery.
Keywords: Topical ketolorac; Vitrectomy; Post-operative; Topical steroids
Introduction
A combination or single therapy of either topical steroid and/ or non-steroidal anti-inflammatory drug (NSAID) has become the typical post-operative paradigm for intraocular surgery, following the elucidation of underlying inflammatory mechanisms [1-3]. It is well known that topical corticosteroids are associated with numerous side-effects including raised intraocular pressure (IOP), development of cataract and impaired corneal epithelial healing [4,5]. The efficacy of topical NSAID monotherapy, including ketolorac, for the treatment of cystoid macular oedema following cataract surgery has been established in a meta-analysis and randomized controlled trials in the past [3,6]. A more recent meta-analysis advocates NSAID over steroid as standard treatment for pseudophakic macular oedema [7]. The role of sole use these agents following vitrectomy surgery, however, is not as clear due to the paucity of large prospective studies on use of anti-inflammatory topical medication.
The efficacy of topical NSAIDs in combination with steroids following vitrectomy has been investigated recently in randomized controlled trials for nepafenac and ketolorac versus placebo [8,9]. These studies have shown that topical NSAIDs reduce post operative pain and improve post-operative inflammation. However, nepafenac was not shown to improve visual acuity, whereas ketolorac use was associated with statistically significant improvements in visual acuity. Neither agent demonstrated any reduction in post-operative cystoid macular oedema compared to placebo when utilizing central macular thickness from optical coherence data. Importantly, both studies included topical prednisolone in both arms of each study and therefore do not demonstrate the effect of topical NSAID monotherapy.
A recent randomised trial including 80 eyes comparing topical nepafenac and prednisolone post-vitrectomy demonstrated no significant difference in visual outcomes, tolerability or inflammatory signs [10]. This study did not include an analysis of intraocular pressure, optical coherence findings and was confounded by giving patients in both treatment arms oral diclofenac sodium 50mg twice a day for 5 days, therefore limiting wider clinical application.
Herein, we perform a retrospective analysis on a series of patients treated with topical ketolorac alone following vitrectomy surgery. We demonstrate for the first time that ketolorac monotherapy is well tolerated and safe without the need for additional anti-inflammatory agents.
Methods
Retrospective analysis of case notes and post-operative Optical Coherence Tomography (OCT) scans of 128 eyes of 128 consecutive patients undergoing vitrectomy for primary rhegmatogenous retinal detachment (RRD) [n=72], full thickness macular hole (MH) (n=42], and epi-retinal membrane (ERM) [n=14] at a single tertiary centre between December 2011 and June 2015. All patients provided valid consent to proceed with surgery and this study was registered with the local Audit Department.
Patients with previous vitrectomy surgery, oil tamponade, combined phacovitrectomy, diabetes, and combined vitrectomy with scleral buckle were excluded. All patients underwent 23 gauge three port pars plana vitrectomy under local anaesthesia as a day case. Internal limiting membranes and epiretinal membranes were stained with Dual blue dye, DORG, prior to peeling. All patients were given subconjunctival injection of 0.5ml dexamethasone at the end of vitrectomy procedure. Postoperatively they were treated with a course of topical ketolorac tromethamine 0.5% ophthalmic solution (Allergan, Dublin, Ireland) four times a day for one month to the affected eye and topical chloramphenicol four times a day for one week.
Patients were reviewed at 2 weeks, 8 weeks and 20 weeks postoperatively. Day one review was not routinely conducted. At each visit postoperative best-corrected visual acuities (BCVA), Intraocular pressure (IOP), patient’s comfort, and optical coherence tomography (OCT) image data was collected. The presence of CMO was determined on clinical appearance of the OCT of each patient and not using the central retinal thickness of controls to identify its presence as previously utilised by other authors [9,11].
Continuous variables expressed as mean ± standard deviation. Categorical variables expressed as percentages. LogMAR values expressed in decimal form were converted from Snellen Acuity. The paired and independent t-test was used to analyse differences between related and independent continuous variables, respectively. Correlation was measured using Pearson’s method.
Statistical significance was considered a p value of <0.05. Analysis was performed using GraphPad Prism 7, GraphPad Software Inc., California, for Mac.
Results
128 patients treated between December 2011 and June 2015 met the inclusion criteria utilizing the local software package Medisoft, UK, database search filters. Baseline characteristics of our study group are summarized in Table 1. Average LogMAR BCVA for all indications improved from 1.04 at baseline to 0.68 (95% CI 0.14 to -0.54, p = 0.001) at 20 weeks follow up for all indications (Figure 1). Patients treated for RRD and MH demonstrated significant improvements in BCVA, however there were no significant changes for patients with ERM (Figure 2. a-c).
Baseline Demographics
Number ± Standard Deviation (Percentage)
Age
66.31 ± 11.68
Male
67 (52.34%)
Female
61 (47.65%)
Central Retinal thickness (μm)
379.08 ± 108.53
Average Retinal Volume (μm3)
9.03 ± 2.64
Indication for surgery:
Primary Rhegmatogenous Retinal Detachment
72 (56.25%)
Full Thickness Macular Hole
42 (32.81%)
Epiretinal Membrane
14 (10.93%)
Table 1: Baseline Demongraphics.
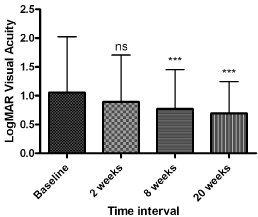
Figure 1: Average LogMAR visual acuity across all patients included in this
study.
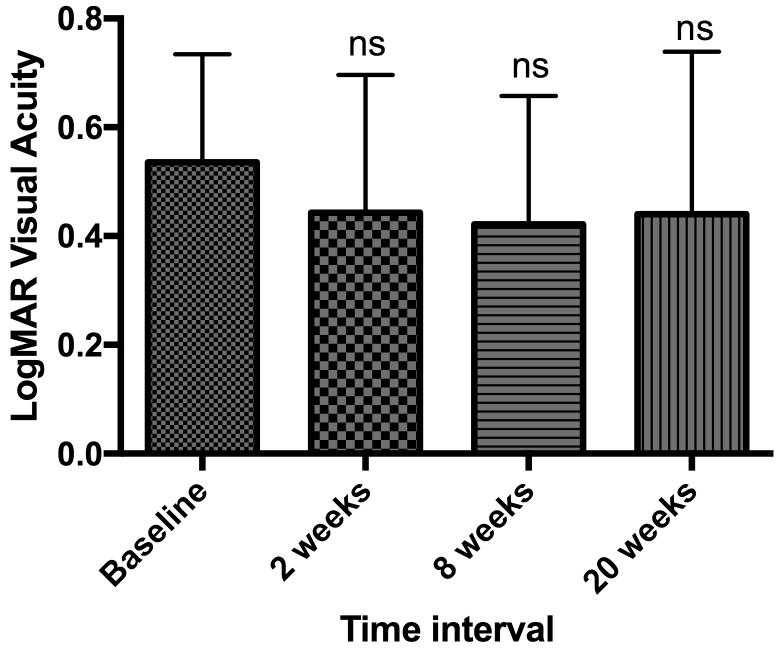
Figure 2a: Best corrected LogMAR visual acuity in patients with epiretinal
membranes.
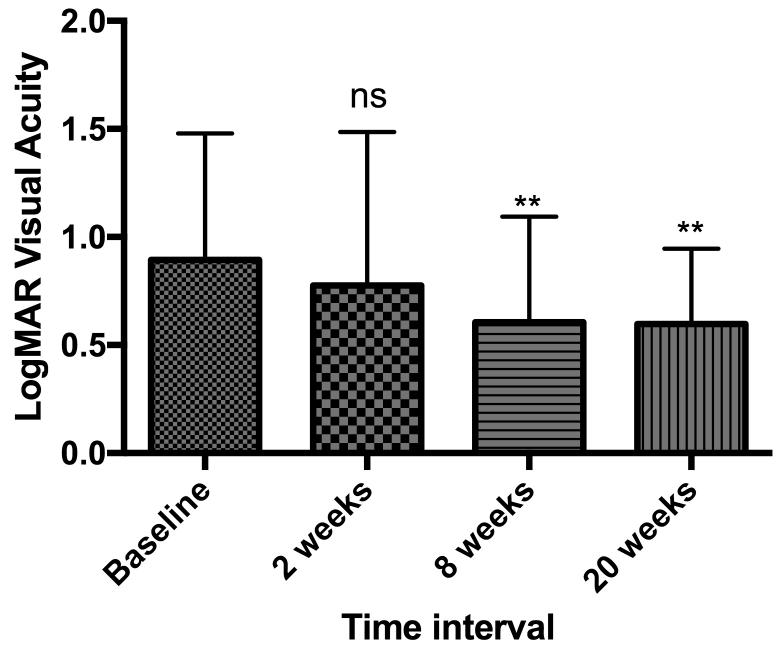
Figure 2b: Best corrected LogMAR visual acuity in patients with macular
holes.
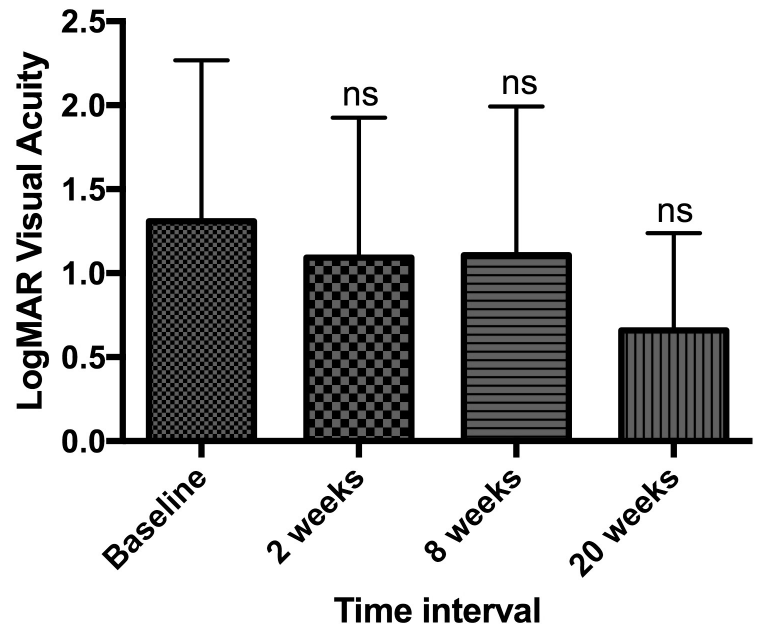
Figure 42c: Best corrected LogMAR visual acuity in patients with retinal
detachments.
Average IOP at baseline was 16.00mmHg (5.00-29.00mmHg), 16.38mmHg (4-43mmHg), 16.00 (6-35mmHg) and 16.05mmHg (10- 25mmHg) at 2, 8 and 20 weeks respectively (Figure 3). It should be noted 1 patient had an IOP above 29mmHg at weeks 2 and 8. When separating patients into their underlying pathologies, no significant change in IOP was found (data not shown).
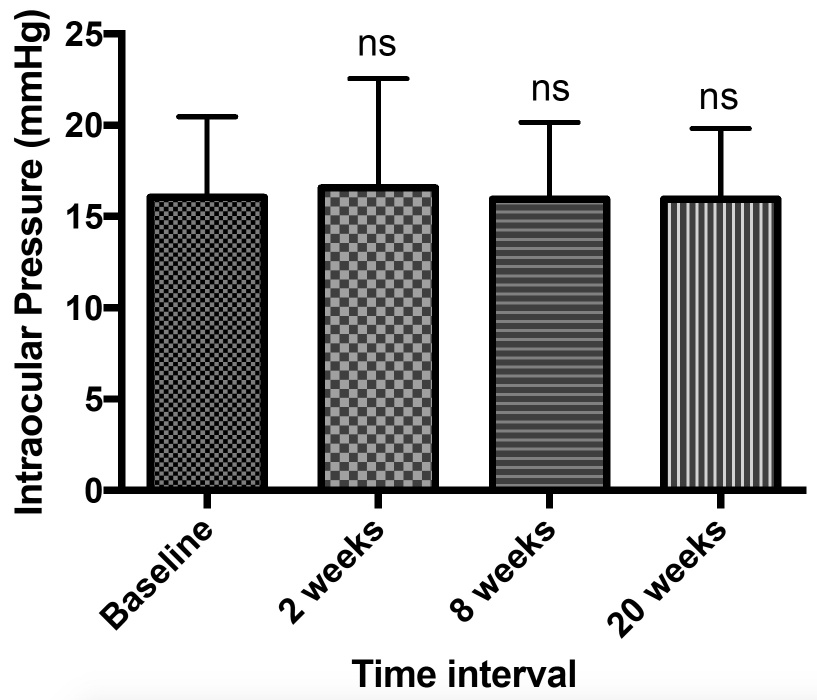
Figure 3: Average intra-ocular pressure across all patients included in this
study.
Central retinal thickness (CRT) on OCT assessment did not change significantly in RRD patients but reduced significantly in patients with MH from 389.81μm at baseline to 295.85μm at 20 weeks follow up compared to baseline (p< 0.0001) (Figure 4). a-c. Patients with ERM had a significant reduction in CRT from 476.71μm at baseline to 388.86μm at 12 weeks (p < 0.05).
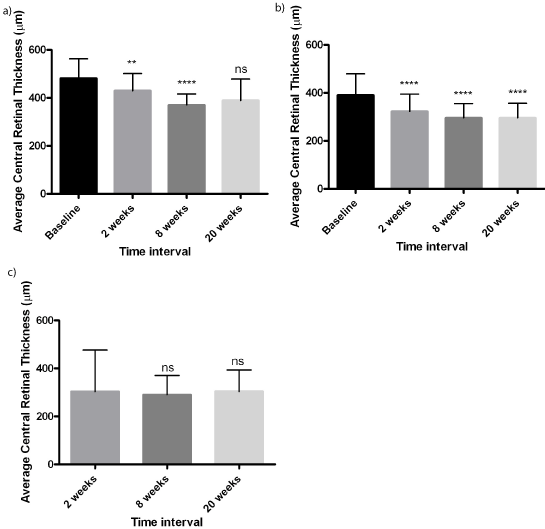
Figure 4: Average Central Retinal Thickness calculated from optical
coherence scans as measured for each indication.
Clinically apparent fovea involving CMO on OCT scans was observed in 13 (10.15%) of 72 patients with RRD at 2 weeks postoperatively compared to 3 (4.16%) patients at 20 weeks. CMO was detected in 34 of 42 (81%) patients with MH at baseline, which reduced to 1 (2.40%) patients at 20 weeks follow up. CMO was present in 6 of 14 (42.85%) patients with ERM pre-operatively and reduced to 2 (14.28%) patients postoperatively at 20 weeks. Data summarised in Figure 5. Overall, 6 (4.7%) patients from the total study group were found to have persistent post-operative CMO (Table 2).
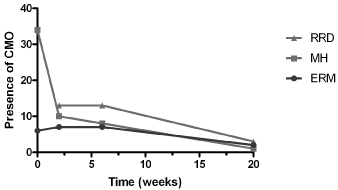
Figure 5: Number of patients with clinically apparent cystoid macular oedema
following vitrectomy surgery separated into each indication for surgery.
Complications in this study included six (4.7%) patients with persistent CMO requiring further treatment beyond 20 weeks post-operatively, 1 (0.8%) patients developed secondary glaucoma post-operatively, 1 (0.8%) patients developed ocular hypertension needing topical treatment, and 1 patient (0.8%) had an adverse reaction to preservatives (Table 2).
Complication
Number (%)
Transient CMO (resolved by 20 week follow up)
23 (18.0%)
Persistent post-operative CMO (Persisted beyond 20 week follow up)
6 (4.0%)
Secondary glaucoma
1 (0.8%)
Ocular hypertension
1 (0.8%)
Preservative reaction
1 (0.8%)
FIGURE LEGENDS
Figure 1: Average LogMAR visual acuity across all patients included in this study.
Figure 2a: Best corrected LogMAR visual acuity in patients with epiretinal membranes.
Figure 2b: Best corrected LogMAR visual acuity in patients with macular holes.
Figure 2c: Best corrected LogMAR visual acuity in patients with retinal detachments.
Figure 3: Average intra-ocular pressure across all patients included in this study.
Figure 4: Average Central Retinal Thickness calculated from optical coherence scans as measured for each indication.
Figure 5: Number of patients with clinically apparent cystoid macular oedema following vitrectomy surgery separated into each indication for surgery.
Table 2: Complications post-vitrectomy surgery.
Discussion
The average BCVA improved by -0.36 LogMAR in our patient sample. This compares well to Kim and Colleagues study where patients on combined topical NSAID and steroid showed BCVA improvement by -0.43 at follow up [8]. Patients treated post operatively with topical and oral NSAID showed BCVA -0.50 improvement at follow up in Nagpal and Colleagues study [10]. Given the heterogeneity of patient groups in these studies and comparative conservative approach with NSAID monotherapy, results in our study compare well with these trials. This indicates that topical ketolorac as a single post operative therapy is likely to be appropriate in a large proportion of patients with few co-morbidities.
Raised intraocular pressure above 29mmHg following vitrectomy has been shown to occur in 14.8% of patients on day 1 post vitrectomy (n = 202) [12]. Another study demonstrated that 11.3% of post-vitrectomy eyes required glaucoma surgery, where one of the risk factors for post-operative glaucoma was accrued to topical corticosteroid use [13]. Herein, we demonstrate that early post-operative reviews are not required when avoiding topical steroidal therapy, in keeping with Brennan and colleagues [14]. Furthermore, only 1 (0.8%) of patients developed post-operative ocular hypertension, which responded well to topical IOP lowering agents, apraclonidine drops in this case. Only 1 (0.8%) patient developed secondary glaucoma that required medical treatment without surgical intervention. Related studies have not included an analysis of IOP postoperatively [8-10].
CRT was improved in the present study by approximately -17% compared to an -8% and -21% reduction in Kim and Naithani and colleagues studies respectively [8]. This is a favourable comparison as both the aforementioned studies provided a combination of topical NSAID and steroid, indicating that NSAID monotherapy is a safe conservative regiment post-vitrectomy.
Our patient group demonstrated 22.7% occurrence of CMO, where 4.7% of patients required further treatment. This is comparable to Naithrini and colleagues who demonstrate 13% of their patients at 8 weeks follow up had persistent CMO when treated with topical steroid or in combination with nepafenac, however it should be noted RRD was not included in their group of patients [9]. Shocket and colleagues previously demonstrated a 12% CMO incidence following RRD repair in small study (n=17) [15]. Notably, of the patients with persistent CMO in the present study, 1 had pre-existing multifocal choroiditis and another had pre-existing primary open angle glaucoma and cataract extraction within the follow up period. One patient required intravitreal triamcinolone following a RRD repair for CMO. The heterogeneity of patient groups in recent clinical trials makes it difficult to directly compare rates of CMO, however the results of our retrospective study demonstrate comparable outcomes to both topical steroid monotherapy and a combination of steroid and NSAID [9,10]. An ideal model to determine the efficacy of anti-inflammatory therapies following vitrectomy surgery is the floaterectomy model as published by De Nie et al [16].
Other studies have included subjective pain scores on post operative day 1. As patients are not reviewed on day 1, this data was not available. However, on questioning patients at first follow up, no patients complained of significant pain. Ketolorac is known to have analgesic properties in addition to anti-inflammatory effects [17,18].
In all patients, there were no signs of clinically significant inflammatory activity in the anterior chamber indicating that ketolorac monotherapy may sufficiently treat post-operative inflammation without the need for topical steroid.
A Cochrane meta-analysis found that two studies showed efficacy of ketolorac post-cataract surgery against chronic CMO, however, two other studies did not show a difference [19]. The review concludes that the role of topical NSAIDs is unclear and requires further investigation. Indeed, the efficacy of ketolorac as a monotherapy following vitrectomy requires more detailed investigation, however in our experience this has been a satisfactory treatment regimen.
Penetration of topical NSAIDs has been shown to be greater in pseudophakic patients post-vitrectomy [20]. However this series of 50 patients was randomized to bromfenac, nepafenac, or indomethacin, but not ketolorac. While it might be inferred that topical NSAIDs will have favourable vitreal penetration, without specific data on ketolorac, it cannot be assumed that there will be greater efficacy in preventing or treating post-vitrectomy CMO. The majority of patients in this study were phakic and as such an analysis of this was not included. A prospective study would be required to investigate this.
Conclusion
Topical NSAID alone post-vitrectomy is associated with comparable BCVA recovery to combined treatments with steroids alone or combined with topical and/or oral NSAIDs. Topical NSAID monotherapy post-vitrectomy was not associated with significant post-operative rises in intra-ocular pressure. We demonstrate that next day post-operative reviews are not required when avoiding topical steroidal therapy. The occurrence of persistent CMO was not higher than previously reported with combined therapies. Therefore we conclude that ketorolac monotherapy is a satisfactory regimen following vitrectomy. Further prospective studies are required to confirm our conclusions.
References
- Miyake K, Ibaraki N. Prostaglandins and cystoid macular edema. Surv Ophthalmol. 2002; 47: S203-218.
- Mentes J, Erakgun T, Afrashi F, Kerci G. Incidence of cystoid macular edema after uncomplicated phacoemulsification. Ophthalmologica. 2003; 217: 408- 412.
- Rossetti L, Chaudhuri J, Dickersin K. Medical Prophylaxis and treatment of Cystoid Macula Oedema after cataract surgery. The results of metaanalysis. Ophthalmology, 1998; 105: 397-405.
- McGhee CN. Pharmacokinetics of ophthalmic corticosteroids. Br J Ophthalmol. 1992; 76: 681-684.
- Y�lek F, Ozdek S, G�relik G, Hasanreisoglu B. Effect of topical steroids on corneal epithelial healing after vitreoretinal surgery. Acta Ophthalmol Scand. 2006; 84: 319-322.
- Flach AJ, Jampol LM, Weinberg D, Kraff MC, Yannuzzi LA, Campo RV, et al. Improvement in visual acuity in chronic aphakic and pseudophakic cystoid macular edema after treatment with topical 0.5% ketorolac tromethamine. Am J Ophthalmol. 1991; 112: 514-519.
- Kessel L, Tendal B, J�rgensen KJ, Erngaard D, Flesner P, Andresen JL, et al. Post-cataract prevention of inflammation and macular edema by steroid and nonsteroidal anti-inflammatory eye drops: a systematic review. Ophthalmology. 2014; 121: 1915-1924.
- Kim SJ, Lo WR, Hubbard GB, Srivastava SK, Denny JP, Martin DF, et al. Topical ketorolac in vitreoretinal surgery: a prospective, randomized, placebocontrolled, double-masked trial. Arch Ophthalmol. 2008; 126: 1203-1208.
- Naithani P, Puranik S, Vashisht N, Khanduja S, Kumar S, Garg S. Role of topical nepafenac in prevention and treatment of macular edema after vitreoretinal surgery. Retina. 2012; 32: 250-255.
- Nagpal M, Lambat S, Mehrotra N, Paranjpe G, Yadav H, Bhardwaj S. Topical nepafenac 0.1% alone versus prednisolone acetate 1% as postoperative antiinflammatory agents in small gauge vitrectomy. Indian J Ophthalmol. 2014; 62: pp. 606-609.
- Tewari HK, Wagh VB, Sony P, Venkatesh P, Singh R. Macular thickness evaluation using the optical coherence tomography in normal Indian eyes. Indian J Ophthalmol. 2004; 52: 199-204.
- Anderson NG, Fineman MS, Brown GC. Incidence of intraocular pressure spike and other adverse events after vitreoretinal surgery. Ophthalmology. 2006; 113: 42-47.
- Han DP, Lewis H, Lambrou FH, Mieler WF, Hartz A. Mechanisms of intraocular pressure elevation after pars plana vitrectomy. Ophthalmology. 1989; 96: 1357-1362.
- Brennan N, Reekie I, Ezra E, Barton K, Viswanathan A, Muqit MM. The role of day one postoperative review of intraocular pressure in modern vitrectomy surgery. Br J Ophthalmol. 2017; 101: 1281-1284.
- Schocket LS, Witkin AJ, Fujimoto JG, Ko TH, Schuman JS, Rogers AH, et al. Ultrahigh-resolution optical coherence tomography in patients with decreased visual acuity after retinal detachment repair. Ophthalmology. 2006; 113: 666- 672.
- de Nie KF, Crama N, Tilanus MA, Klevering BJ, Boon CJ. Pars plana vitrectomy for disturbing primary vitreous floaters: clinical outcome and patient satisfaction. Graefes Arch Clin Exp Ophthalmol. 2013; 251: 1373-1382.
- Heier J, Cheetham JK, Degryse R, Dirks MS, Caldwell DR, Silverstone DE, et al. Ketorolac tromethamine 0.5% ophthalmic solution in the treatment of moderate to severe ocular inflammation after cataract surgery: a randomized, vehicle-controlled clinical trial. Am J Ophthalmol. 1999; 127: 253-259.
- Simone JN, Pendelton RA, Jenkins JE. Comparison of the efficacy and safety of ketorolac tromethamine 0.5% and prednisolone acetate 1% after cataract surgery. J Cataract Refract Surg. 1999; 25: 699-704.
- Sivaprasad S, Bunce C, Roxanne C-N. Non-steroidal anti-inflammatory drugs versus corticosteroids for controlling inflammation after uncomplicated cataract surgery. Cochrane Database of Systematic Reviews. 2012.
- Turano R, Russo A, Vezzoli S, Morescalchi F, Bernini M, De Ferrari F, et al. Vitreous Nonsteroidal Anti-Inflammatory Drug Levels in Vitrectomy Patients Treated with Topical Indomethacin 0.5%, Nepafenac 0.1%, and Bromfenac 0.09%. Investigative Ophthalmology & Visual Science. 2015; pp. 5739.