
Research Article
Austin Crit Care J. 2015;2(1): 1008.
Impact of Clinical Nutritional Education for Fifth Year Medical Students through the Attendance of NST Rounds for Critically Ill Patients: A Prospective Interventional Study in Japan
Tomomichi Kan’o*, Yuichi Kataoka, Kazui Soma and Yasushi Asari
Department of Emergency & Critical Care Medicine, Kitasato University, Japan
*Corresponding author: Tomomichi Kan’o, Department of Emergency & Critical Care Medicine Kitasato University Japan, 1-15-1 Kitasato, Minami, Sagamihara, Kanagawa, Japan,
Received: March 10, 2015; Accepted: June 09, 2015; Published: June 10, 2015
Abstract
Objective: Most physicians consider clinical nutrition education important, but it is difficult for medical students to be provided. The aim of this prospective study was to evaluate the effectiveness of clinical nutritional management on fifth year medical students.
Methods: All fifth year medical students (n=200), who made rounds for bedside learning between April 2010 and March 2012, took part in our emergency centre NST for two and a half hours as clinical nutrition education. We compared questionnaires (maximum 100 points) about nutritional management for critically ill patients, nutritional interests (maximum 5 points) and the necessity of NST rounds (maximum 5 points) during clinical practice of emergency medicine before and after attendance. All analyses were performed with the Wilcoxon signed-rank test and the chi-square test.
Results: The average points were significantly improved (questionnaires about nutritional management for critically ill patients: 46.4±18.2→72.5±17.1 (Mean±SD); p<0.001, nutritional interests: 3.76±0.59→4.05±0.60; p<0.001, the necessity of NST rounds: 3.90±0.61→4.21±0.60; p<0.001).
Conclusion: Fifth year medical students’ knowledge about nutritional management for critically ill patients, nutritional interests and the necessity of NST rounds during clinical practice of emergency medicine were improved by attending NST rounds at an emergency centre.
Keywords: Nutrition education; Medical student; Critically ill patient; NST round
Abbreviations
NST: Nutrition Support Team; JPEN: Journal of Parenteral and Enteral Nutrition; SCCM: Society of Critical Care Medicine; JSPEN: Japanese Society for Parenteral And Enteral Nutrition
Background
Nutrition is a vital component of health promotion and disease prevention [1]. However, Nightingale JM et al. reported that knowledge about the assessment and management of under nutrition among doctors was poor [2]. McWhirther J et al. reported that a high prevalence of under nutrition and inadequate nutritional support are common among institutionalized patients in Europe [3]. We consider that this can be attributed to two things. One is that nutritional management is difficult to produce the effectiveness in the short term, unlike respiratory and circulatory management, and the other is a lack of nutritional education.
It has been over a quarter-century since the National Academy of Sciences published its groundbreaking report highlighting the insufficiency of nutritional education in the medical school curriculum [4]. However, the teaching of nutrition in US medical schools still appears to be in a precarious position, lacking a firm, secure place in the medical curricula of most medical schools [5]. Besides, only 3 out of 57 medical schools offered clinical nutrition courses in Japan [6].
We had fifth year medical students participate in our Nutrition Support Team (NST) at the tertiary emergency centre for 2.5 hours during their one-week clinical practice. The aim of this study was to investigate the effectiveness of the program toward their nutritional knowledge and interests.
Methods
Participants
We designated 200 fifth year medical students who had received one week’s clinical practice in emergency and critical care medicine, which was held between April 2010 and March 2012 at the tertiary emergency centre.
Schedule of clinical practice
The schedule of their clinical practice is shown in (Table 1).
09:00-10:30
10:40-12:10
13:00-14:30
14:40-16:10
M
Emergency Medicine
JATEC1
JATEC2
Emergency Radiology
*
Tu
Professor’s Round
11:00-Burn
NST
15:30-Journal Club
*
W
Thoracico-Abdominal Trauma
Orthopedic Trauma
Advanced Cardiac Life Support
*
Th
Circulatory Management
Psychiatric Emergency
Conference
*
F
Environmental Emergency
Pediatric Emergency
Emergency Room
Examination
M: Monday, Tu: Tuesday, W: Wednesday, Th: Thursday, F: Friday
JATEC: Japan Advanced Trauma Evaluation & Care
※ on duty
Table 1: Schedule of clinical practice.
Our facility
We attended the tertiary emergency centre of Kitasato University Hospital. We treated 2,385 Patients in 2011 and 2,300 in 2010. We possess two tertiary emergency rooms, 25 intensive care units and 24 backward beds.
Our NST
We established the NST in 1999. Our team includes multidisciplinary staff, such as doctors, nurses, nutritionists, pharmacists, medical technologists, a physical therapist and an occupational therapist.
Regardless of the attendance of medical students, the members discuss all patients, who number about 40, in the emergency centre, and make their rounds every Thursday afternoon.
Intervention
The author instigated communication with medical students by introducing them to each other and to the author before the NST round. Then they took a test and completed a questionnaire. The test is shown in an additional file. After that, they attended the NST round. They got an explanation from an NST member during the round. After NST round, they took the same test and completed the questionnaire. Finally, the author gave them the answer, the description and the quintessence of the clinical nutrition guideline which was published in the Journal of Parenteral and Enteral Nutrition (JPEN) and the Society of Critical Care Medicine (SCCM) on 2009 [7].
Nutritional interests and the necessity of NST round during clinical practice of emergency medicine
To measure their views in terms of personal nutritional interests and how they regarded the necessity of the NST round during clinical practice of emergency medicine, we asked them to mark their answers on a scale from 1 (complete no interest, complete no necessity) to5 (extreme interest, extreme necessity) together with the pre and post tests.
Statistical analysis
All analyses were performed by Dr. SPSS for Windows (SPSS Japan Inc). Analysis included descriptive analyses, the Wilcoxon signed-rank test for comparisons of means of continuous variables between groups, and the chi-square test for testing the association between categorical variables. Person correlation coefficients were calculated where both variables were continuous. A p-value of < 0.05 was considered to indicate statistical significance; all tests were twotailed.
Ethics
The requirement for signed written consent was waived, as consent was implied by participants completing and submitting the survey. We didn’t obtain the ethical approval because we performed the study as a series of classes for medical students.
Results
No students were disqualified due to missing information. The average test score is shown in (Figure 1). This was significantly improved from 46.4±18.2 to 72.5±17.1 (Mean±SD) points (p<0.001). Each right answer rate is shown in (Figure 2). All results, except for target calorie and dysphagia after extubation, were significantly improved. Also the average score indicating their nutritional interests was significantly improved from 3.76±0.59 to 4.05±0.60 (p<0.001) as shown in (Figure 3). Finally, the point average of the necessity of NST roundduring clinical practice of emergency medicine was also significantly improved from 3.90±0.61 to 4.21±0.60 (p<0.001) as shown in (Figure 4).

Figure 1: The change of the questionnaire scores both pre and post round.
These average scores were significantly improved from 46.4±18.2 to
72.5±17.1 (Mean±SD) points (P<0.001) with the Wilcoxon signed-rank test.
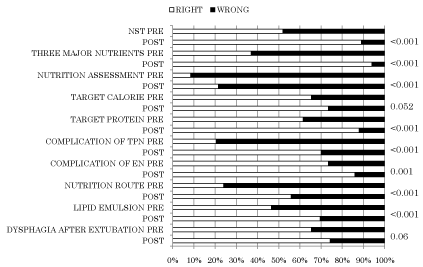
Figure 2: The change of right answer rate of the questionnaire both pre and
post round.
All results, except for target calorie and dysphagia after extubation, were
significantly improved with the Wilcoxon signed-rank test.
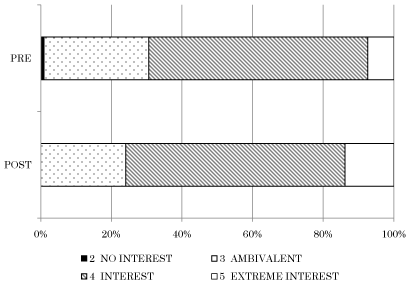
Figure 3: The change of nutritional interests both pre and post round.
The average score indicating their nutritional interests was significantly
improved from 3.76±0.59 to 4.05±0.60 (P<0.001) with the chi-square test.
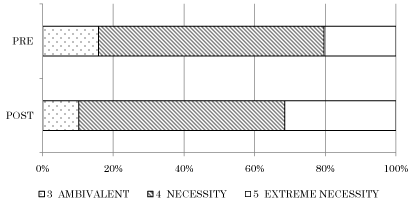
Figure 4: The change of necessity of NST Round during clinical practice of
emergency medicine both pre and post round.
The point average of the necessity of NST roundduring clinical practice
of emergency medicine was also significantly improved from 3.90±0.61 to
4.21±0.60 (P<0.001) with the chi-square test.
Discussion
Fifth year medical students’ knowledge and interest about nutritional management for critically ill patients were improved by attending NST rounds at an emergency centre without selection bias for a short period in this study.
Preclinical setting
Shai I et al. reported that students rated the importance of nutrition treatment more highly than did physicians [8]. So, early exposure may be effective. Then, Gramlich LM et al. reported that over 80 percent of medical students felt a nutritional lecture in a classroom setting was preferable [9]. We will consider a nutritional lecture in a classroom setting during the preclinical year.
Clinical year
Adams KM et al. showed that only 38 out of 106 US medical schools offered more than 5 hours of nutrition teaching [10]. Our clinical practice offered two and a half hours of nutritional teaching by attending NST rounds. So, by attending NST rounds in other departments, it is possible to increase clinical nutrition lessons.
Online lecture
Online lectures are increasing in the US. A case-based integrated nutrition curriculum was provided for medical students through a web site [11]. A free comprehensive, online nutrition curriculum was provided for undergraduate and postgraduate learners [12]. In Japan, there was an e-learning site which the Japanese Society for Parenteral and Enteral Nutrition (JSPEN) established for medical staff [13]. It may be possible to provide online lectures for students who have a lot of interests about nutrition.
Elective system
In Europe and the US, nutrition elective courses are effective for students who are motivated to increase their awareness of nutrition. Ray S et al. reported that a 2-day workshop for applicant medical students was effective in terms of fostering a positive attitude toward nutrition and improved knowledge [14]. Also Guagnano MT et al. reported more medical students who took a clinical nutrition course passed the test than those medical students who did not take one [15]. We will consider a clinical nutrition elective system in the future.
Limitations
We have to mention some of the limitations of this study. First, we only focused on nutrition for critically ill field. Second, we haven’t confirmed the effectiveness in the long term.
Conclusion
Fifth year medical students’ knowledge and interest about nutritional management for critically ill patients were improved by attending NST rounds at an emergency centre without selection bias for a short period. We need to examine whether this is effective over a long term period.
Acknowledgement
We would like to thank Dr. Guoqin Wang (Kitasato Clinical Research Center Kitasato University School of Medicine, Japan) for her kind suggestions about statistics.
References
- Mowe M, Bosaeus I, Rasmussen HH, Kondrup J, Unosson M, Rothenberg E, et al. Insufficient nutritional knowledge among health care workers? Clin Nutr. 2008; 27: 196-202.
- Nightingale JM, Reeves J. Knowledge about the assessment and management of undernutrition: a pilot questionnaire in a UK teaching hospital. Clin Nutr. 1999; 18: 23-27.
- McWhirther J, Pennington C. Incidence and recognition of malnutrition in hospital. BMJ. 1994; 308: 945-948.
- National Research Council Committee on Nutrition in Medical Education. Nutrition Education in U.S. Medical Schools. Washington, DC: National Academy Press. 1985.
- Adams KM, Kohlmeier M, Powell M, Zeisel SH. Nutrition education in U.S. medical schools: latest update of a national survey. Acad Med. 2010; 85: 1537-1542.
- Orimo H, Shimura T, Shimada T. Nutrition education in medical schools in Japan: results from a questionnaire survey. Asia Pac J ClinNutr. 2006; 15: 323-328.
- McClave SA, Martindale RG, Vanek VW, McCarthy M, Roberts P, Taylor B, et al. Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Adult Critically Ill Patient: Society of Critical Care Medicine (SCCM) and American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.). J Parenter Enteral Nutr. 2009; 33: 277-316.
- Shai I, Shahar D, Fraser D. Attitudes of physicians and medical students toward nutrition's place in patient care and education at Ben-Gurion University. Educ Health. 2001; 14: 405-415.
- Gramlich LM, Olstad DL, Nasser R, Goonewardene L, Raman M, Innis S, et al. Medical students' perceptions of nutrition education in Canadian universities. Appl Physiol Nutr Metab. 2010; 35: 336-343.
- Adams KM, Lindell KC, Kohlmeier M, Zeisel SH. Status of nutrition education in medical schools. Am J Clin Nutr. 2006; 83: 941S-944S.
- Hark LA, Morrison G. Development of a case-based integrated nutrition curriculum for medical students. Am J Clin Nutr. 2000; 72: 890S-897S.
- Adams KM, Kohlmeier M, Powell M, Zeisel SH. Nutrition in medicine: nutrition education for medical students and residents. Nutr Clin Pract. 2010; 25: 471-480.
- Virtual clinical nutrition college.
- Ray S, Udumyan R, Rajput-Ray M, Thompson B, Lodge KM, Douglas P, et al. Evaluation of a novel nutrition education intervention for medical students from across England. BMJ Open. 2012; 2: e000417.
- Guagnano MT, Merlitti D, Pace-Palitti V, Manigrasso MR, Sensi S. Clinical nutrition: inadequate teaching in medical schools. Nutr Metab Cardiovasc Dis. 2001; 11: 104-107.