
Research Article
Austin Crit Care J. 2017; 4(1): 1021.
Frequency of Delirium in Non-Cardiac Surgical and Medical Intensive-Care Patients-Results from a Comparative, Prospective, Observational Study
Zeder M¹*, Müller T², Zeman F³, Schlitt HJ4, Blecha S¹, Graf BM¹ and Bein T¹
1Department of Anesthesiology, Operative Intensive Care, Regensburg University Hospital, Germany
2Department of Internal Medicine II, University Medical Center Regensburg, Germany
3Center for Clinical Studies, University Medical Center Regensburg, Germany
4Department of Surgery, University Medical Center Regensburg, Germany
*Corresponding author: Marius Zeder, Department of Anesthesiology, Operative Intensive Care, Regensburg University Hospital, Franz-Josef-Strauss-Allee 11, 93053, Regensburg, Germany
Received: August 31, 2017; Accepted: December 08, 2017; Published: December 15, 2017
Abstract
Introduction: Delirium has a high incidence in ICUs (Intensive-Care Units) and is associated with adverse outcomes. Amongst other factors, inflammation is predominantly linked to the risk of delirium. We hypothesized that the inflammatory stress of surgery/trauma leads to a higher incidence of delirium in surgical compared to medical ICUs. We performed a prospective comparative study, and determined the risk factors for delirium by multivariable analyses.
Materials and Methods: A prospective single-centre University Hospital study on two ICUs was performed. Patients were screened for delirium with the CAM–ICU (Confusion Assessment Method for the ICU) at several days (1, 3 and 5 after admission/extubation). Demographic data, laboratory values, and administered medication details were gathered. Non-cardiac surgical and medical ICU patients were compared and Odds Ratios (OR) were calculated via univariable and multivariable logistic regression models.
Results: The incidence of delirium in all patients (n=138) was 32.6% and no difference was found between surgical and medical ICU patients. Patients with delirium received significantly more psychoactive medication, benzodiazepines, propofol, and morphine. They had higher Simplified Acute Physiology Score, higher age, and longer ventilation and stay in the ICU. Patients without delirium received significantly more oxycodone/naloxone (15.4mg vs 5.3mg, p=0.041). They had higher levels of serum haemoglobin (10.9g/l vs 9.8g/l, p=0.004) and albumin (27.4g/l vs 23.7g/l, p<0.001) and lower values of urea (47.6mg/dl vs 81.2mg/dl, p<0.001), bilirubin (1.12mg/dl vs 2.3mg/dl, p=0.001), creatinine (1.5mg/dl vs 2.3mg/dl, p<0.001), CRP (C-Reactive Protein) (67.9 mg/l vs 102.6mg/l, p =0.035) and sodium (138.8mmol/l vs 142.0mmol/l, p<0.001). Multivariable logistic regression showed creatinine (p =0.028), CRP (p=0.022), and duration of ventilation (p=0.002), as independent predictors of delirium.
Discussion: Despite higher CRP as a marker of inflammation, patients in the surgical/trauma ICU did not have higher incidence of delirium. A possible explanation could be the higher administration of oxycodone/naloxone, an opioid with a trend towards a “delirium-protecting’ potency. Nevertheless, further studies are needed to prove this hypothesis, as the development of delirium seems to be a multifactorial process, and a “bundle’ for prevention is needed.
Keywords: Delirium; Intensive-Care Medicine; Incidence; Oxycodone; Non-cardiac surgical intensive care; Medical intensive care
Abbreviations
ICU: Intensive-Care Unit; DSM-IV: Diagnostic and Statistical Manual of Psychiatric Diseases IV; SICU: Surgical/trauma Intensive- Care Unit; MICU: Medical Intensive-Care Unit; CRF: Case Report Form; CAM–ICU: Confusion Assessment Method for the ICU; RASS: Richmond Agitation Scale Score; CRP: C-Reactive Protein; SAPS: Simplified Acute Physiology Score; SD: Standard Deviation; IQR: Inter Quartile Range; OR: Odds Ratio; CI: Confidence Interval
Introduction
Delirium is the most common psychiatric disorder in intensivecare patients, with an incidence varying from 10 percent to 92 percent [1-4], and is associated with a higher mortality compared to those patients not suffering from delirium [5,6]. Despite the high incidence, delirium is frequently not detected by the intensive-care unit staff [7] and screening is poorly implemented in German ICUs [8].
Delirium is defined by the Diagnostic and Statistical Manual of Psychiatric Diseases IV (DSM-IV) by impaired consciousness, perception and attention deficit, vigilance disorder and disorganization of thought processes [9]. Furthermore, the International Classification of Diseases also lists disorders of psychomotor activity, emotionality, and the sleep-wake cycle as criteria of delirium [10]. In recent studies, several risk factors for delirium have been examined and it was found that delirium was an independent factor for adverse outcome variables. Thus, prevention or early therapeutic management of delirium is an important goal in the ICU. The use of earplugs, increased input of daylight and early mobilization seem to prevent delirium [11]. Furthermore, the implementation of a so-called “ABCDE bundle’ significantly decreases the prevalence and duration of delirium [12].
The pathophysiology of delirium is poorly understood to date. There are seven mostly complementary theories for the development of delirium, which include neuroinflammatory processes, neuronal aging, oxidative stress, neurotransmitter deficiency, neuroendocrine factors, diurnal dysregulation and network disconnectivity hypotheses [13]. It was found that inflammation [14], low albumin level [15], use of analgesics [1] and increased volume load (during surgery)-predominantly in cardiac surgery patients [16]-were associated with increased risk of delirium. Surgery can lead to systemic immunosupression and pro-inflammatory periods [17]. Additionally persistent infections [18] as well as sepsis [19] are common complications in surgical ICUs. Therefore we hypothesized that the incidence of delirium would also be higher in intensive-care patients after trauma or non-cardiac surgery compared to medical intensive-care patients, if higher inflammatory stress due to previous surgery/trauma could be related to delirium [14,20].
The aims of this study were to analyze the frequency of delirium in non-cardiac surgical/trauma compared to “medical’ admissions to the ICU in a prospective single-centre University Hospital study and to determine risk factors for delirium by multivariate analyses.
Material and Methods
A prospective study was performed in two ICUs of a University Hospital: a 26-bed Surgical Intensive-Care Unit (SICU) and a 14-bed Medical Intensive-Care Unit (MICU). The approval of the regional Institutional Review Board (Ethikkommission der Universität Regensburg) was obtained (Approval No.15-101-0101).After a twoweek pilot period, during which the Case Report Form (CRF) and the study protocol were tested, all patients who were admitted to the ICUs between June and November 2015 and who were treated for at least one day and more, were screened consecutively with the Confusion Assessment Method for the ICU (CAM-ICU) at least on days one, three and five after admission to the ICU (non-ventilated patients) or after extubation (ventilated patients). The CAM-ICU is a validated tool with high specificity and good sensitivity for detecting delirium in the ICU [21]. Patients were found to be eligible for delirium assessment when fulfilling the following criteria: a Richmond Agitation Scale Score (RASS) of-3 or higher [22], the absence of mechanical ventilation and no contraindication for the screening with the CAM-ICU. If patients were transferred after day one to another ward, delirium assessment was continued there. If patients stayed in the ICU longer than five days, screening was performed every two days until transfer.
Furthermore, the following variables were recorded: C-Reactive Protein (CRP), urea, albumin and procalcitonin from serum; the arterial pH, haemoglobin, blood glucose, and electrolytes from the 8a.m. blood gas analyses were registered (all at first delirium assessment). In addition, the cumulative doses were recorded of sedative (propofol, lorazepam, midazolam) and analgesic (morphine, hydromorphone, sufentanil, oxycodone/naloxone) drugs, as well as vasoactive medications (noradrenaline, clonidine) and psychoactive drugs (levomepromazine, promethazine, quetiapine, melperone, haloperidol)-24 hours prior to every screening (days one, three and five).Administration of pain medication in the ICUs was standardized using a visual analoge scale. All this information was retrieved from pre-existing data in the patient data management system (Metavision, iMDsoft, Düsseldorf, Germany).
Body temperature, arterial oxygen saturation and mean arterial pressure during screening, as well as age, gender, SAPS of the first 24 hours after admission to ICU, the main reason for admission and the duration of previous ventilation and stay in the ICU were recorded. Additionally, the highest value of serum bilirubin and creatinine during the stay was collected. All CAM-ICU assessments were performed by one investigator (MZ) after an extended supervised training through experienced intensives (TB).
Statistical Methods
Statistical calculations were performed with SPSS Statistics 23 (IBM Corp., Armonk, New York, USA). Statistical significance was defined by p-value<0.05.
Quantitative variables are presented by arithmetic mean ± Standard Deviation (SD), median and Inter Quartile Range (IQR); categorical variables by count and percentage. Admissions to SICU/ MICU were analysed using Student’s T-test for normally distributed values and Mann-Whitney U-test for non-normally distributed values. Results of both tests are shown with mean ± SD in text and tables to improve readability. The Shapiro-Wilk test was used as a test of normality (only temperature showed normal distribution). For comparisons of categorical variables-gender, intubation, tracheotomy and administration of psychoactive drugs-Pearson’s Chi-Square test were used and Mantel-Haenszel odds ratios were calculated.
Univariable logistic regression models to identify risk factors for delirium were calculated. Independent variables were the significant variables of prior tests and the variables described as significant predictors of delirium in the literature.
Further, a multivariable logistic regression model using significant (p<0.05) predictors of the univariable models was calculated. Results from both logistic regression analyses are presented as Odds Ratios (OR) with 95% Confidence Interval (CI).
Results
142 patients were screened for delirium. Four patients were excluded from the study due to impossibility of data gathering, incomplete screenings or for fulfilling the exclusion criteria.138 patients were included in the study (SICU: 71, MICU: 67). More male patients were analyzed (n=88, 63.8%).86(62.3%) patients received mechanical ventilation through endotracheal tube and seven (5.1%) received tracheotomy. Of all the patients, 32.6% developed delirium and 3.6% died during their stay in the ICU.
The mean age was 61.7±16.3 years (median 65 years, IQR 21), with a mean SAPS of 36.5±14.4 (36, IQR 20), patients were mechanically ventilated for a mean of 2.6±4.2 days (1, IQR 3) and they stayed in the ICU for an average of 7.2±6.2 days (5, IQR 7). The characteristics of the cohort are displayed in (Table 1).
Table 1: Characteristics of patients included in the study.
The administration of any psychoactive drug was associated with a higher incidence of delirium (53.3% vs 8.6%) and patients with delirium received a higher cumulative amount of psychoactive drugs compared to patients without delirium: haloperidole (1.43±2.61mg vs 0.17±1.08mg, p<0.001), quetiapine (15.56±50.08mg vs 3.23±31.11mg, p=0.001), promethazine (4.72±17.93mg vs 0.54±5.18mg, p=0.007), clonidine (532.59±1308.62μg vs 41.21±202.26μg, p=0.009), melperone (1.78±8.27mg vs 0.00mg±0, p=0.012), levomepromazine (2.36±6.70mg vs 0.13±1.30mg, p=0.002). They also received more benzodiazepines (lorazepam, midazolam), morphine, propofoland sufentanil. Patients suffering from delirium received significantly less oxycodone/naloxone than patients without delirium.
Laboratory values and arterial blood gas analyses showed significant differences between patients without and with delirium in values of serum albumin, urea, CRP, sodium, haemoglobin, creatinine and bilirubin. Additionally, patients without delirium had significantly lower SAPS, lower age, lower duration of mechanical ventilation and shorter overall stay in the ICU. The Chi-Square test showed that patients with delirium were significantly more likely to be intubated or had undergone tracheotomy. Significant differences between patients with and without delirium are shown in (Table 2).
Table 2: Administration of psychoactive drugs, mean accumulated doses of sedative and analgesics drugs, mean results of lab values, and results of other variables in delirium and non&nddelirium patients.
We also investigated differences between SICU and MICU regarding prevalence of delirium on the separate screening days. Although there seems to be a slight trend for MICU to have higher rates of delirious patients on later days of screening, there were no significant differences (Figure 1).
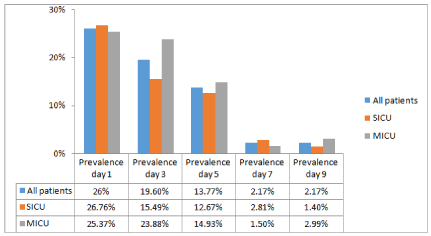
Figure 1: Prevalence of delirium comparing SICU/MICU over the screening
days.
To compare varying risk factors for delirium for the whole collective, as well as for SICU and MICU in specific, we conducted logistic regression analyses (Table 3).
Table 3: Univariable logistic regression models of factors associated with delirium in all patients, SICU and MICU.
As shown in (Table 3), significant risk factors for delirium in the complete study group were the administration of psychoactive drugs, propofol and lorazepam. Higher values of urea, CRP, sodium, creatinine and bilirubin, as well as lower values of albumin and haemoglobin, were also identified as significant factors for delirium. Other risk factors were older age, higher SAPS, and longer duration of mechanical ventilation and stay in the ICU as well as intubation and tracheotomy.
Independent risk factors for delirium were calculated by a multivariable logistic regression analysis: Serum creatinine and C-reactive protein values, as well as a longer duration of mechanical ventilation were identified as independent risk factors in the complete cohort of both groups (Table 4).
Table 4: Multivariable logistic regression model of factors associated with delirium in the whole collective.
Discussion
The incidence of delirium in intensive-care patients is high. Various factors have been detected as predictors of delirium, such as high age, cognitive impairment, history of smoking and alcohol abuse, apolipoprotein E4 polymorphism, depression and visual or hearing impairment. In addition, factors associated with critical illness-such as acidosis, anemia, fever, infection and sepsis, hypotension, and respiratory diseases-are linked to delirium [5,23-29]. Delirium can also be induced by medication like opioids and benzodiazepines, immobilisation and disturbance in sleep [30-32]. Since inflammation processes are identified as special risk factors for delirium [14,20] and an extended incidence of delirium was found in cardiac surgery patients [16], we were interested in the frequency of delirium in the patients who received non-cardiac surgery compared to the medical ICU patients. To our knowledge, no such investigation had been conducted before.
The main results of our prospective investigation were: 1) the incidence of delirium was not different between the patients in a non-cardiac surgery ICU compared to those in a medical ICU. 2) The patients with delirium received significantly more psychoactive, sedative and analgesic drugs in both groups, had lower serum albumin and haemoglobin values, but higher values of serum creatinine, urea, C-reactive protein and bilirubin. 3) In a multivariate logistic regression analysis of factors associated with delirium in the complete study group, the duration of mechanical ventilation, serum creatinine and C-reactive protein were identified as independent predictors of delirium. 4) Patients without delirium received significantly more oxycodone/naloxone, the only opioid with a trend towards a “delirium-protecting’ potency.
In a recent prospective cohort study on a population of mixed ICU, the patients with delirium showed significantly higher CRP values than those without (120.5mg/l vs57.5mg/l; P=0.0001), and CRP was an independent predictor for delirium [14]. Accordingly, in our patient cohort, nearly the same CRP pattern was observed in delirium and non-delirium patients. But, interestingly, although the patients of SICU had significantly higher CRP values compared to MICU patients, the frequency of delirium was similar in both study groups. A possible explanation for such a finding could be a significant higher use of the analgesic drug oxycodone/naloxone in SICU patients: in a recent study on cancer patients, the effect of three different opioids injected for the first time on the incidence of delirium was investigated [33]. The highest incidence was found in the morphine group (28.9%), compared to the oxycodone group (19.5%) and the fentanyl group (8.6%, not given in our study). Furthermore, Maddocks and co-workers reported in a “historic’ clinical note on the attenuation of morphine-induced delirium by substitution of oxycodone [34]. Nevertheless, our hypothesis that oxycodone/ naloxone might attenuate the frequency of delirium in ICU patients has to be tested in a specific randomized prospective study design.
In our multivariate analysis, the elevation of serum creatinine was identified as an independent predictor for delirium, especially in the SICU patients. Renal dysfunction in the surgical ICU patients is often present as acute kidney injury while patients in an MICU are often admitted with a chronically impaired renal dysfunction [35]. Similarly, in an actual prospective cohort study on 466 ICU patients, it was shown that stage 2 acute kidney injury was associated with delirium (OR 1.55; 95% CI: 1.07, 2.26) compared to patients without acute or acute-on-chronic kidney injury [36].
In our study, the SICU-patients had significantly lower serum albumin levels and the non-delirium patients were characterized by significantly higher albumin. Such a finding is not easy to interpret in the light of our main result: the incidence of delirium was not different in SICU and MICU patients. In a prospective observational cohort study of 34 cardiac surgery patients undergoing cardiopulmonary bypass, patients with delirious state showed a significantly lower albumin level 24h and 48h postoperatively than those without delirium [37]. Again, we hypothesize that the development of delirium is a multifactorial process and-in an intensive care settingdelirium is not attributable to only one variable.
Our study has some strengths and some limitations. The strengths are: We performed a precise and continuous screening of delirium in defined SICU and MICU patients by one well-trained investigator and the actual important co-variables were carefully recorded. On the other hand, the present study is a single-centre study and a relatively low number of patients in each group are recruited. Although in a limited study group, we were able to demonstrate important results by a multivariate analysis.
Conclusion
The frequency of delirium is not different between medical and non-cardiac surgery intensive-care patients, although the latter group is characterized by higher inflammation (C-reactive protein), which was identified as an independent predictor of delirium. A possible explanation is the application of a significant higher dose of oxycodone/naloxone in operative patients, which might exert a delirium-protecting property. Clearly, larger groups of patients and double-blind studies are needed to prove this hypothesis, especially as only univariable, but not (yet) multivariable logistic regression models showed significant effects.
References
- Theuerkauf N, Guenther U. Delir auf der Intensivstation. Med Klin Intensivmed Notfmed. 2014; 109: 129-136.
- Pandharipande P, Cotton BA, Shintani A, Thompson J, Pun BT, Morris JA, et al. Prevalence and risk factors for development of delirium in surgical and trauma intensive care unit patients. J Trauma. 2008; 65: 34-41.
- Pandharipande P, Cotton BA, Shintani A, Thompson J, Costabile S, Truman Pun B, et al. Motoric subtypes of delirium in mechanically ventilated surgical and trauma intensive care unit patients. Intensive Care Med. 2007; 33: 1726- 1731.
- Sieber FE, Zakriya KJ, Gottschalk A, Blute M, Lee HB, Rosenberg PB, et al. Sedation depth during spinal anesthesia and the development of postoperative delirium in elderly patients undergoing hip fracture repair. Mayo Clin Proc. 2010; 85: 18-26.
- Ouimet S, Kavanagh BP, Gottfried SB, Skrobik Y. Incidence, risk factors and consequences of ICU delirium. Intensive Care Med. 2007; 33: 66-73.
- Ely EW, Shintani A, Truman B, Speroff T, Gordon SM, Harrell FE, et al. Delirium as a predictor of mortality in mechanically ventilated patients in the intensive care unit. JAMA. 2004; 291: 1753-1762.
- Ely EW, Stephens RK, Jackson JC, Thomason JW, Truman B, Gordon S, et al. Current opinions regarding the importance, diagnosis, and management of delirium in the intensive care unit: a survey of 912 healthcare professionals. Crit Care Med. 2004; 32: 106-112.
- Saller T, Dossow VV, Hofmann-Kiefer K. Kenntnis und Umsetzung der S3- Leitlinie zum Delirmanagement in Deutschland. Der Anaesthesist. 2016; 65: 755-762.
- Sass HS, Wittchen HU, Zaudig M, Houben I. Diagnostisches und Statistisches Manual Psychischer Störungen, DSM-IV-TR. für Psychologie. 2003.
- Graubner Bernd. ICD-10-GM 2015 Systematisches Verzeichnis. Internationale statistische Klassifikation der Krankheiten und verwandter Gesundheitsprobleme. Deutscher Ärzte-Verlag. 2014.
- Zaal IJ, Slooter AJ. Delirium in Critically iII Patients: epidemiology, pathophysiology, diagnosis and management. Drugs. 2012; 72: 1457-1471.
- Bounds M, Kram S, Speroni KG, Brice K, Luschinski MA, Harte S, et al. Effect of ABCDE Bundle Implementation on Prevalence of Delirium in Intensive Care Unit Patients. Am J Crit Care. 2016; 25: 535-544.
- Maldonado JR. Neuropathogenesis of delirium: review of current etiologic theories and common pathways. Am J Geriatr Psychiatry. 2013; 21: 1190- 1222.
- Zhang Z, Pan L, Deng H, Ni H, Xu X. Prediction of delirium in critically ill patients with elevated C-reactive protein. J Crit Care. 2014; 29: 88-92.
- Horacek R, Krnacova B, Prasko J, Latalova K. Delirium as a complication of the surgical intensive care. Neuropsychiatr Dis Treat. 2016; 12: 2425-234.
- Smulter N, Lingehall HC, Gustafson Y, Olofsson B, Engström KG. Delirium after cardiac surgery: incidence and risk factors. Interact Cardiovasc Thorac Surg. 2013; 17: 790-796.
- Alazawi W, Pirmadjid N, Lahiri R, Bhattacharya S. Inflammatory and Immune Responses to Surgery and Their Clinical Impact. Ann Surg. 2016; 264: 73-80.
- Gentile LF, Cuenca AG, Efron PA, Ang D, Bihorac A, McKinley BA, et al. Persistent inflammation and immunosuppression: a common syndrome and new horizon for surgical intensive care. J Trauma Acute Care Surg. 2012; 72: 1491-1501.
- Vincent J. Update on surgical sepsis syndrome. Br J Surg. 2017.
- Pol RA, van Leeuwen, BL, Izaks GJ, Reijnen MM, Visser L, Tielliu IF, et al. C-reactive Protein Predicts Postoperative Delirium Following Vascular Surgery. Ann Vasc Surg. 2014; 28: 1923-1930.
- Gusmao-Flores D, Salluh, JI, Chalhub RA, Quarantini LC. The confusion assessment method for the intensive care unit (CAM-ICU) and intensive care delirium screening checklist (ICDSC) for the diagnosis of delirium: a systematic review and meta-analysis of clinical studies. Crit Care. 2012; 16: R115.
- Sessler CN, Gosnell MS, Grap MJ, Brophy GM, O’Neal PV, Keane KA, et al. The Richmond Agitation-Sedation Scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002; 166: 1338- 1344.
- Ely EW, Girard TD, Shintani AK, Jackson JC, Gordon SM, Thomason JW, et al. Apolipoprotein E4 polymorphism as a genetic predisposition to delirium in critically ill patients. Crit Care Med. 2007; 35: 112-117.
- Aldemir M, Ozen S, Kara IH, Sir A, Baç B. Predisposing factors for delirium in the surgical intensive care unit. Crit Care. 2001; 5: 265-270.
- Dubois MJ, Bergeron N, Dumont M, Dial S, Skrobik Y. Delirium in an intensive care unit: a study of risk factors. Intensive Care Med. 2001; 27: 1297-1304.
- Inouye SK. Precipitating Factors for Delirium in Hospitalized Elderly Persons. Predictive model and interrelationship with baseline vulnerability. JAMA. 1996; 275: 852.
- McNicoll L, Pisani MA, Zhang Y, Ely EW, Siegel MD, Inouye SK. Delirium in the intensive care unit: occurrence and clinical course in older patients. J Am Geriatr Soc. 2003; 51: 591-598.
- Pandharipande P, Shintani A, Peterson J, Pun BT, Wilkinson GR, Dittus RS, et al. Lorazepam is an independent risk factor for transitioning to delirium in intensive care unit patients. Anesthesiology. 2006; 104: 21-26.
- Schor JD, Levkoff SE, Lipsitz LA, Reilly CH, Cleary PD, Rowe JW, et al. Risk factors for delirium in hospitalized elderly. JAMA. 1992; 267: 827-831.
- Girard TD, Pandharipande PP, Ely EW. Delirium in the intensive care unit. Crit Care. 2008; 12: S3.
- Piva S, McCreadie VA, Latronico N. Neuroinflammation in sepsis: sepsis associated delirium. Cardiovasc Hematol Disord Drug Targets. 2015; 15: 10- 18.
- Mehta S, Cook D, Devlin JW, Skrobik Y, Meade M, Fergusson D, et al. Prevalence, risk factors, and outcomes of delirium in mechanically ventilated adults. Crit Care Med. 2015; 43: 557-566.
- Tanaka R, Ishikawa H, Sato T, Shino M, Matsumoto T, Mori K, et al. Incidence of Delirium Among Patients Having Cancer Injected With Different Opioids for the First Time. Am J Hosp Palliative Care. 2017; 34: 572-576.
- Maddocks I, Somogyi A, Abbott F, Hayball P, Parker D. Attenuation of morphine-induced delirium in palliative care by substitution with infusion of oxycodone. J Pain Symptom Manage. 1996; 12: 182-189.
- Ichai C, Vinsonneau C, Souweine B, Armando F, Canet E, Clec’h C, et al. Acute kidney injury in the perioperative period and in intensive care units (excluding renal replacement therapies). Ann Intensive Care. 2016; 6: 48.
- Siew ED, Fissell WH, Tripp CM, Blume JD, Wilson MD, Clark AJ, et al. Acute Kidney Injury as a Risk Factor for Delirium and Coma during Critical Illness. Am J Respir Crit Care Med. 2017; 195: 1597-1607.
- Baranyi A, Rothenhäusler H. The impact of intra- and postoperative albumin levels as a biomarker of delirium after cardiopulmonary bypass: results of an exploratory study. Psychiatry Res. 2012; 200: 957-963.