
Clinical Image
Austin Crit Care J. 2019; 6(1): 1025.
Guidewire Induced Cardiac Tamponade with Coronary Obstruction
Philipp Solbach1*, Katja Hueper2, Bernhard MW Schmidt3 and Sascha David3
1Department of Gastroenterology, Hepatology and Endocrinology, Hannover Medical School, Germany
2Institute for Diagnostic and Interventional Radiology, Hannover Medical School, Germany
3Department of Nephrology and Hypertension, Hannover Medical School, Germany
*Corresponding author: Philipp Solbach, Department of Gastroenterology, Hepatology and Endocrinology Carl- Neuberg-Str. 1, 30625 Hannover, Germany
Received: May 02, 2019; Accepted: May 13, 2019; Published: May 20, 2019
Clinical Image
We report the case of a young patient who received heart transplantation 28 years ago, who was hospitalized due to Post- Transplant Lymphoproliferative Disorder (PTLD). Shortly after initiation of hemodialysis due to septic acute kidney injury, the patient developed progressive dyspnea, hypotension and tachycardia. Laboratory tests revealed massive elevation of cardiac troponin T (5,538 ng/l) and NT-proBNP (>35,000 ng/l). Diagnostic echocardiography showed a compression of the right ventricle. Thoracic CT scan led to the diagnosis of a hematoma (10.8 x 5.4 x 5.8 cm) with right ventricular tamponade (Figure 1A, black arrows) and long-segmented close vicinity to the right coronary artery (Figure 1, white arrow). The patient was stabilized with Veno-Arterial Extracorporeal Membrane Oxygenation (VA-ECMO) circuit and the surgeons closed a small hole in the inferior vena cava. We assume that the guidewire induced the injury during placement of the dialysis catheter and that the local restriction of this tamponade was due to post-transplant adhesions.
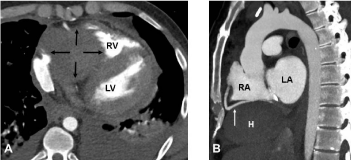
Figure 1: Large hematoma (A) and its long-segmented close vicinity to the
right coronary artery (B).
Abbreviations: H=hematoma, LV=left ventricular, RV=right ventricular,
LA=left atrium, RA=right atrium