
Case Report
Austin Crit Care J. 2019; 6(1): 1026.
Cardiac Arrest in a Young Patient Triggered due to Pepper Spray: A Case Report
Arora N*
1Hospital Dr, CE 545, Columbia MO 65212, USA
*Corresponding author: Niraj Arora, 1 Hospital Dr, CE 545, Columbia MO 65212, USA
Received: April 15, 2019; Accepted: May 22, 2019; Published: May 29, 2019
Abstract
Pepper spray is commonly used agent used by defense personnel. Active component Capsiacin has not been proven to cause cardiac arrest. Here, we report a case where exposure to pepper spray triggered cardiac arrest in a healthy young patient. The case description is followed by review of the systemic effects of pepper spray and a possible mechanism of arrhythmias.
Introduction
Pepper spray is a common agent used for self-defense training in policing, riot control or crowd control [1,2]. The active component Oleoresin Capsicum causes local inflammatory response at the point of contact. The effect is usually transient without significant systemic effects. Here we report a case of young male with no previous cardiorespiratory co-morbidity in whom exposure to pepper spray triggered cardiac arrest. This is the first case to our knowledge documenting the effect of pepper spray in causing cardiac arrest due to ventricular fibrillation.
Case
21 year old male with no past medical history presented to the emergency department in cardiac arrest. Patient had competed in a police training pepper spray event and decontamination at the police academy without issues with no obvious distress per witnesses. Immediately after the event, he collapsed and become unresponsive. Patient was foaming at the mouth with generalized shaking without loss of bowel or bladder at the time. He had absent pulses and so Cardiopulmonary Resuscitation (CPR) was started. When paramedics arrived on the scene, he received DC cardioversion three times, intravenous epinephrine and amiodarone without Return of Spontaneous Circulation (ROSC). Intubation was unsuccessful in the field. At the Emergency Department, CPR was continued with several DC cardioversion attempts along with intravenous epinephrine, amiodarone, lidocaine, calcium, magnesium, and bicarbonate. He achieved ROSC after a total 35 minutes of CPR. Glasgow Coma Scale (GCS) was 9 after ROSC. He was started on lidocaine drip and intubated and sedated. CT head showed no acute abnormality. Acute Kidney Injury (AKI) and lactic acidosis improved with intravenous hydration. Bedside echocardiogram on admission. (Day 1) showed severe global hypokinesis of left ventricle with Ejection Fraction (EF) 5%. CT chest showed no evidence of pulmonary emboli. Neurology evaluation revealed bilateral pupils 3mm reactive to light, corneal reflex intact, cough and gag reflex present, no spontaneous motor movements. Electroencephalogram (EEG) did not show seizure activity.
Day 2-4
Repeat echocardiogram showed moderate improvement of EF to 29. Left heart catheterization done on day 3 showed normal coronary arteries. MRI brain done on day 3 showed findings consistent with hypoxic/anoxic brain injury, worst in the bilateral occipital lobes, caudate heads (Figure 1). Day 4, patient started having intermittent rigid spasms of truncal region with dystonic arch like posturing, related to tactile stimuli. Levetiracetam was started with no response and there was no EEG correlate for these episodes.
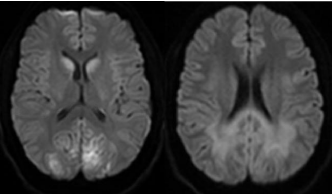
Figure 1: MRI Brain showing restricted diffusion in the bilateral occipital lobes
and bilateral caudate nuclei.
Day 5-10
Patient continued to have intermittent posturing and was subsequently switched to midazolam infusion (Day 7) which was continued for 4 days and slowly weaned off over next 3 days under EEG guidance. Patient was started on clonazepam, baclofen and gabapentin while midazolam was weaned down. Cardiac MRI was inconclusive for hypertrophic cardiomyopathy with complete recovery of left ventricular EF. Patient had tracheostomy and PEG tube placement on day 10.
Day 11-17
Patient was continued on oral clonazepam0.5mg every 8 hours and gabapentin 800mg every 8 hours which was titrated as need to control agitation and posturing. Hospital course was complicated by aspiration pneumonitis, transaminitis and acute renal failure which were managed appropriately.
Day 18-38
Patient continued to improve and was more awake, alert and following commands. He was weaned off from mechanical ventilation. A subcutaneous implantable cardioverter defibrillator was placed on day 30. He was discharged to a rehabilitation facility in a stable condition. His mRS at discharge was 4.
On 3 month follow up in neurology clinic, patient had shortterm memory impairment with mRS of 2 and is legally blind. Genetic testing for hypertrophic cardiomyopathy was negative.
Discussion
Pepper spray (Oleoresin Capsicum) contains active ingredient capsaicin, which is derived from the fruit of plants in the genus Capsicum [3]. Percentage of total capsaicinoids and not only the capsaicin within the formulation indicate pepper spray strength [4]. Civilian and law enforcement pepper sprays range from 0.18% to 1.33% major capsaicinoids [4]. Lethal oral dose of capsaicin in humans is 0.5-5g/kg [3]. Duration of effects varies between 20 minutes to 2 hours [3]. Effects usually disappear within 1-2 days [3].
Most common effects of pepper spray is on skin, eyes and mucous membrane. It causes intense pain but prolonged treatment causes analgesic effect by depleting the reserves of “substance P” in the nociceptive afferent nerve fibers and induces degeneration of primary sensory neurons [5]. Exposurein eyes produces intense tearing, redness and blepharospasm [6]. Contact of capsaicin with respiratory mucosa causes coughing or sneezing and can precipitate bronchospasm in susceptible individuals with asthma [1]. With severe toxicity, it can cause respiratory distress, pulmonary edema, chest pain and hypotension [3]. Capsaicin can cause transient increase in blood pressure (usually less than 10mmHg) which quickly returns to normal in 2 hours on discontinuation of the exposure [3]. Patients with unstable or poorly controlled hypertension or a recent history of cardiovascular or cerebrovascular events may be at an increased risk of adverse cardiovascular effects.
In healthy individuals, the effects are temporary and usually resolve with removing the subject from the exposure and washing the surface with warm water [3]. In some cases, magnesium-aluminum hydroxide-simethicone suspension as a dressing to the skin to provide immediate pain relief. In case of bronchospasm, bronchodilators with steroids as needed provide immediate relief.
Pepper spray in combination with cocaine use could be a lethal combination as capsaicin potentiates the effects of cocaine [7]. Capsaicin interacts with the Transient Receptor Potential Vanilloid subtype 1 (TRPV1) receptors in dopaminergic neurons preventing its degeneration and blocking reuptake of dopamine (which is a downstream signal of cocaine) causing a dopamine overdose that leads to death [8].
In effect, capsaicin can cause sudden development of bronchospasm with abnormalities in gas exchanges due to alveolar edema [2]. This causes excess stress on the myocardium which inturn could lead to arrhythmia. Our patient had heart failure with low ejection fraction on admission which gradually improved over weeks. There were no structural abnormality in the myocardium and no evidence of coronary artery disease. No other predisposing factors were identified. This is the first case in the medical literature where pepper spray has triggered ventricular arrhythmias leading to cardiac arrest.
Conclusion
Note of caution should be mentioned on the manufacturer label on the possible side effect of pepper spray in causing cardiac arrest in susceptible subjects.
References
- The effectiveness and safety of Pepper Spray, in National Institute for Justice: Research for Practice.
- Final report on the safety assessment of capsicum annuum extract, capsicum annuum fruit extract, capsicum annuum resin, capsicum annuum fruit powder, capsicum frutescens fruit, capsicum frutescens fruit extract, capsicum frutescens resin, and capsaicin. Int J Toxicol. 2007; 26: 3-106.
- Capsaicin. Available from: https://toxnet.nlm.nih.gov/cgi-bin/sis/search2/ r?dbs+hsdb:@term+@DOCNO+954.
- Available from: https://www.sabrered.com/pepper-spray-frequently-askedquestions- 0.
- Smith J, Greaves I. The use of chemical incapacitant sprays: a review. J Trauma, 2002. 52: 595-600.
- Oleoresin Capsicum: Pepper Spray as a Force Alternative, in National Institute of Justice: Technology Assessment Program. 1994.
- Mendelson JE, Tolliver BK, Delucchi KL, Baggott MJ, Flower K, Harris WC. Capsaicin, an active ingredient in pepper sprays, increases the lethality of cocaine. Forensic Toxicology. 2009; 28: 33-37.
- Chung, YC, Baek JY, Kim SR, Ko H, Bok E, Shin WH, et al. Capsaicin prevents degeneration of dopamine neurons by inhibiting glial activation and oxidative stress in the MPTP model of Parkinson’s disease. Exp Mol Med. 2017; 49: e298.