
Research Article
Austin Crit Care J. 2019; 6(1): 1029.
Post-Traumatic Stress Disorder after Intensive Care Unit Discharge: Prevalence and Impact on Quality of Life
Julie Fauroux, Yannis Bornemann, Isabelle Desmeulles, Désiré Samba, Gérald Viquesnel, Frédéric Ethuin, Jean-Luc Hanouz, Véronique Pottier*
Department of Anesthesia and Surgical Intensive Care, Caen University Hospital, France
*Corresponding author: Véronique Pottier, Department of Anesthesia and Surgical Intensive Care, Caen University Hospital, 14033 Caen Cedex, France
Received: October 30, 2019; Accepted: November 28, 2019; Published: December 05, 2019
Abstract
Background: Hospitalization in ICU is a trauma leading to Post Traumatic Stress Disorder (PTSD). The objective is to determine the prevalence of PTSD and its impact on quality of life.
Methods: Survivors of a before and after prospective study assessing the impact of a nurse implemented sedation algorithm on the outcome after the ICU stay, were followed up with by a phone survey.
Results: A total of 1156 ventilated patients were admitted during the study period. Among the 145 included patients, 47 died and 35 were lost or declined follow-up. Only 62 patients accepted it at 3 months (42.8%), 55 at 6 months (37.9%) and 42 at one year (29%). The prevalence of PTSD was 12.9 % at 3 months, 10.9 % at 6 months and 16.7 % at one year. ICU stay had a moderate impact on quality of life at 3 months, 6 months and 1 year. Approximately 10 % of patients had a severe impact on their quality of life at ICU discharge, up to one year. PTSD at 3 months was significantly higher than in the « before » period. There was no difference at 6 months or 1 year, nor was there a significant difference in quality of life between these 2 periods.
Conclusions: Improving the quality of care in the ICU should also take into consideration the possible deleterious consequences of the ICU stay. Follow-up is paramount in patients at risk, and increased efforts at improving their quality of life after ICU discharge are needed.
Keywords: Post-Traumatic Stress disorder; Quality of life; Impact; Delirium
Abbreviations
PTSD: Post-Traumatic Stress Disorder; ICU: Intensive Care Unit; RASS: Richmond Agitation-Sedation Scale; BPS: Behavior Pain Scale; PTSS-10: Post-Traumatic Stress Syndrome 10-Question Inventory; SAPS II: Simplified Acute Physiology Score II
Introduction
Hospitalization in the ICU department implies the use of invasive therapeutics that can be perceived as aggressive by the patient and can constitute physical or psychological pain. There are multiple sources of discomfort: noise, light, lack of sleep, pain, and patient’s misunderstanding of the environment. All of these factors can lead to Post-Traumatic Stress Disorder (PTSD) [1].
PTSD arises after an aggression. Clinical findings include symptoms of intrusion (repetitive, intrusive memories), symptoms of avoidance (avoidance of the situation, relational disorder) and neurovegetative symptoms (anger, hypervigilance and insomnia).
The prevalence of PTSD prevalence is approximately 1.2% in men and 2.7% in women [2], and can be the consequence of ICU stay trauma [3,4]. The « expected » prevalence of PTSD months after ICU discharge is approximately 14 to 41% [4-9], and a quarter of patients suffer from psychological disorders one year after ICU discharge.10 PTSD can remain many years after the ICU stay [7-11].
Psychiatric history, particularly an anxious or depressive state, high benzodiazepine consumption, frightening or psychotic experiences during the ICU stay, and delirium are documented risks factors for PTSD.8 [12-14], Other debated factors include female sex, young age, duration of mechanical ventilation and length of stay as well as agitation, physical restraint, and opioid administration [12].
Since its definition by the World Health Organization in 1994, quality of life has become a major tool for the evaluation of therapeutic effects. Patients and physicians strive for not only a longer life, but a better life.
Our objective was to evaluate the prevalence of PTSD after ICU stay and its impact on quality of life at 3 months, 6 months, and one year after discharge.
Materials and Methods
We conducted a prospective, « Before-After » interventional study in the 26-bed surgical ICU of Caen University Hospital between November 2014 and April 2017. The study was approved by the local Ethical Committee (CPP Nord Ouest III, CHU de Caen, Caen, France) under the number A14-D65-VOL.23 on December 06, 2014. The committee considered it as part of routine practice, and patient approval was not required. However, written information was systematically given to each included patient or to their next of kin. The study is recorded in ClinicalTrials with the number NCT03186521.
Inclusion criteria
Patients were included in our before/after study, entitled « ALGOSEDA », which assessed the impact of a sedation-analgesia titration algorithm in a nursing-managed surgical ICU on the complications of critical illness and on the outcome after the ICU stay. Our work concerns the second part of the study, the complications after ICU discharge. In « ALGOSEDA », patients aged 18 years or older, admitted to the ICU, and anticipated to require more than 48 hours of sedation and analgesia were eligible and assessed for enrollment.
Non-inclusion criteria
Patients were not eligible if they were under guardianship or ‹ 18 years of age, pregnant, under palliative care, experiencing brain injury, presenting with an initial Glasgow Coma score ‹ 14, receiving neuromuscular blocking agents at the time of enrollment, under therapeutic sedation (acute respiratory distress syndrome, acute severe asthma, intracranial hypertension, etc.), or admitted following resuscitated cardiac arrest.
Exclusion criteria
Patients were excluded from the study if they were extubated or dead within 48 hours after inclusion.
Study protocol
« Before » Period: Sedation and analgesia was exclusively managed by the attending physician and guided by the Richmond Agitation-Sedation Scale (RASS) [15,16] and Behavior Pain Scale (BPS) [17] and recorded every 4 hours by nurses. The dosage and choice of hypnotic drug (Propofol® or Midazolam®) was at the discretion of the physician, and the only opioid used was Sufentanil®.
« After » Period: Following medical prescription, the patient’s sedation and analgesia was managed by the ICU nurses according to the protocol displayed in each bedroom.
Every patient included in ALGOSEDA whether in the « Before » period or « After » period were contacted by phone and asked to answer two surveys at 3 months, 6 months and one year after ICU discharge.
Data collection
Booklets dedicated to the « ALGOSEDA » study were edited and completed by the department’s internal or principal investigators of the study. The anonymized data were recorded on an eCRF platform based on OpenClinica® (Open Clinica, LLC, Waltham, Massachusetts, USA).
The parameters collected and calculated were:
1) New hospitalization since ICU discharge
2) Psychotropic drug use since ICU discharge
3) PTSD assessed by Post-Traumatic Stress Syndrom-10 (PTSS- 10) [18]
4) Quality of life assessed by the WHOQOL-BREF19
PTSD was diagnosed using the Post-Traumatic Stress Syndrome 10-Question Inventory (PTSS-10) [18]. It includes ten items assessing symptoms of intrusion, avoidance and neuro-vegetative behavior related to PTSD. Each item is scored from 1 (never) to 7 points (always) with a total score ranging from 10 to 70. PTSD is defined by a score ≥ 35 (Appendix 1). PTSS-10 has a good sensibility (77%) and good specificity (97.5%) and is valid for ICU patients.
The WHOQOL-BREF is a subjective self-assessed scale of quality of life. It has been tested considerably in the French population [19]. We used the short (26 items) and more recent (2004) version of the WHOQOL-100 (WHOQOL group 1998). The WHOQOL-BREF produces a quality of life profile.
The WHOQOL-BREF is therefore based on a four-domain structure.
-Physical health (7 items): Activities related to daily living, dependence on medicinal substances and medical aids, energy and fatigue, mobility, pain and discomfort, sleep and rest, and work capacity.
-Psychological health (6 items): Body image and appearance, negative feelings, positive feelings, self-esteem, spirituality, religion, personal beliefs, thinking, learning, memory and concentration.
-Social relationships (3 items): Personal relationships, social support, sexual activity.
-Environment (8 items): Financial resources, freedom, physical safety and security, health and social care: accessibility and quality, home environment, opportunities for acquiring new information and skills, participation in and opportunities for recreation, leisure activities, physical environment (pollution/noise/traffic/climate), transport.
There are also two items that are examined separately: question 1 asks about an individual’s overall perception of quality of life and question 2 asks about an individual’s overall perception of their health.
The quotation is made on a scale of 5 points, allowing an evaluation of the intensity (« not at all-extremely »), the capacity (« not at allcompletely »), the frequency (« never-always »), the evaluation (« very satisfied/unsatisfied; very good/bad »). The final score varies from 26 to 130 (Appendix 2).
The impact of PTSD on the quality of life is split into three categories according to the severity of the damage. A score between 26 and 61 is considered as a severe impact on the quality of life, the impact is considered moderate between 62 and 96, and the impact is considered minor between 97 and 130.
Statistical analysis
Quantitative data are expressed as the mean ± SD, or median with confidence intervals at 95 % [CI 95 %] according to the normality of their distribution and were compared using the Mann–Whitney nonparametric U test when data were not normally distributed, or Student’s t-test for normally distributed data. Qualitative data are expressed as percentages and were compared using the Fisher’s exact test when data were not normally distributed, or the Chi-squared test for normally distributed data.
The normality of the distribution was determined by the D’Agostino-Pearson test. The level of significance was set at p ‹ 0.05 between the two tested periods (before/after).
All statistical analyses were performed with software R 3.4.0: A Language and Environment for Statistical Computing (R Foundation for Statistical Computing ©, Vienna, Austria).
Results
A flow chart of the study design is depicted in Figure 1. During the study period, 1156 intubated and mechanically ventilated patients were admitted to the surgical ICU of Caen University Hospital. Among the 145 eligible patients (12.5%), 47 patients died, and 36 patients were lost to follow-up before the 3rd month call or they refused to answer. Only 62 patients accepted the follow-up at 3 months, 55 patients accepted at 6 months and 42 patients accepted at one year.
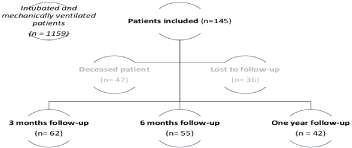
Figure 1: Flow chart of the study.
Patient characteristics
Demographic and primary characteristics of the patients are reported in (Table 1). There were no significant differences between the two periods, except for tobacco consumption, which was lower in the « After » period. There was a trend toward a shorter ICU length of stay in the « After » period. There was no significant difference in mortality between the two periods.
Baseline Characteristics
BEFORE Period
(n = 100)a
AFTER Period
(n = 45)b
p Value
Age (years)
61 ± 20
65 ± 14
0.177
Male gender
68 (68%)
38 (84%)
0.062
BMI
29 ± 8
28 ± 6
0.328
Underlying diseases
- Psychiatric illness
16 (16%)
8 (18%)
0.711
Psychotropic treatment
14 (14%)
7 (16%)
1.000
- Chronic alcoholism
25 (25%)
14 (31%)
0.259
Number of drinks per day
3.6 ± 1.8
5.7 ± 3.8
0.447
- Chronic smoking
60 (60%)
21 (47%)
0.415
Number of packs-years
39 ± 24
25 ± 14
0.033
ICU length of stay (days)
26 [16; 36]
16 [12; 30]
0.059
Hospital length of stay (days)
47.5 [30; 62]
39 [25; 57]
0.251
SAPS II
49 [38; 61]
53 [38; 64]
0.622
Death
28 (28%)
18 (40%)
0.228
Quantitative data are presented as the mean ± standard deviation or median [1st quartile; 3rd quartile], and categorical data as a number (percentages in parentheses).
a The percentage of the before group was calculated using 100 patients as the denominator.
b The percentage of the after group was calculated using 45 patients as the denominator.
BMI, body mass index; SAPS II, new simplified acute physiology score.
Table 1: Baseline characteristics according to the before and after periods.
Prevalence of post-traumatic stress disorder
New hospitalization since last contact varies from 24.2% to 29.1% but was stable at 3 months, 6 months and one year. Patients under psychotropic drugs since ICU discharge were between 25.5% and 29%. The prevalence of post-traumatic stress disorder defined by PTSS-10 ≥ 35 is approximately 12.9% at 3 months, 10.9% at 6 months, and 16.7% at one year (Table 2).
Prevalence of PTSD
3 Months
(n = 62)a
6 Months
(n = 55)b
1 year
(n=42)c
Rehospitalization
15 (24 %)
16 (29%)
12 (29%)
Psychotropic Drugs
18 (29 %)
14 (25.5%)
12 (28.5%)
PTSS-10 (median)
21 [15; 28]
18 [13; 24]
16 [11; 26]
PTSS-10 = 35
8 (13 %)
6 (11%)
7 (17%)
Quantitative data are presented as the mean ± standard deviation or median [1st quartile; 3rd quartile], and categorical data as a number (percentages in parentheses).
a The percentage of the « 3 months » group was calculated using 62 as the denominator.
b The percentage of the « 6 months » group was calculated using 55 patients as the denominator.
c The percentage of the « one year » group was calculated using 42 patients as the denominator.
PTSD, post-traumatic stress disorder; PTSS-10, Post-traumatic Stress Syndrome 10-Question Inventory.
Table 2: Prevalence of post-traumatic stress disorder.
Risk factor for post-traumatic stress disorder
Doses of sedative drugs were significantly decreased (1330 vs 315 mg, p ‹ 0.001 for hypnotics and 1803 vs 900 μg, p ‹ 0.001 for opioids, respectively) during the « After » period, and patients experienced less delirium (41% vs 26.7%, p = 0.015) (Table 3).
Risk factor for PTSD
BEFORE Period
(n = 100)a
AFTER Period
(n = 45)b
p Value
Related to Sedation
Target RASS (-2 to 0) (days)
0 [0; 2]
1 [0; 3]
0.038
RASS > -2 (days)
7 [4; 12]
3 [2; 5]
< 0.001
Target BPS (< 5) (days)
7 [4; 14]
5 [3; 7]
0.002
Total cumulative doses
Midazolam (mg)
1500 [518; 2544]
317 [15; 720]
< 0.001
Opioids (μg)
1803 [1098; 4290]
900 [450; 1680]
< 0.001
Related to Complications of Critical Illness
Delirium
41 (80%)
12 (50%)
0.015
PTSS
3 months
24 [18; 29]
16 [11; 20]
0.004
6 months
20.5 [14; 24]
15 [10.5; 18]
0.072
1 year
16.5 [12; 27]
11.5 [11; 13.5]
0.183
WHOQOL BREF
3 months
79 [69; 86]
76 [75; 87]
0.538
6 months
81 [72.5; 86]
80 [74.5; 84.5]
0.955
1 year
82 [73; 90]
81 [80; 83]
1.000
Quantitative data are presented as the mean ± standard deviation or median [1st quartile; 3rd quartile], and categorical data as a number (percentages in parentheses).
a The percentage of the before group was calculated using 100 patients as the denominator.
b The percentage of the after group was calculated using 45 patients as the denominator.
PTSD, Post-Traumatic Stress Disorder; RASS, Richmond Agitation-Sedation Scale; BPS, Behavior Pain Scale; PTSS-10, Post-Traumatic Stress Syndrome 10-Question Inventory
Table 3: Risk factors for post-traumatic stress disorder during the ICU stay.
The PTSS-10 result is higher at 3 months in the « before» period than the « after » period. There was no difference at 6 months and one year.
There was no significant difference in the quality of life as the WHOQOL-BREF result was similar between the two groups.
Quality of life assessment
During this study according to the WHOQOL-BREF results, ICU stay shows a moderate impact on the quality of life at 3 months, 6 months and one year (Table 4).
Quality of life assessment
3 Months
(n = 62)a
6 Months
(n = 55)b
1 year
(n=42)c
WHOQOL BREF (median)
78.5 [72; 87]
81 [73; 86]
81.5 [73; 88.5]
Minor Impact
(97-130)
4 (6.5%)
3 (5.5%)
3 (7%)
Moderate Impact
(62-96)
51 (82%)
48 (87%)
35 (83%)
Severe Impact
(26-61)
7 (11%)
4 (7%)
4 (9.5%)
Quantitative data are presented as the mean ± standard deviation or median [1st quartile; 3rd quartile], and categorical data as a number (percentages in parentheses).
a The percentage of the « 3 months » group was calculated using 62 as the denominator.
b The percentage of the « 6 months » group was calculated using 55 patients as the denominator.
c The percentage of the « one year » group was calculated using 42 patients as the denominator.
Table 4: Quality of life assessment.
Approximately 10% of patients present a severe impact on their quality of life (WHOQOL-BREF ≤ 61) at ICU discharge and one year after.
Discussion
PTSD is a relatively frequent consequence of a stay in the ICU and has been for too long ignored or trivialized. Preventing PTSD by controlling its risk factors should be in the mind of every physician to at least offer psychological support for patients at risk.
In this study, the prevalence of post-traumatic stress after a stay in the ICU was 12.7% at 3 months, 10.7% at 6 months and 16% at one year, which is consistent with the literature finding a prevalence ranging from 14% to 41% [4-9]. This heterogeneity is due to the difficulty in making the diagnosis because of the multiplicity of existing questionnaires. Schelling et al [4]. showed the possible relationship between the number of traumatic events occurring during the ICU stay (episode of respiratory distress, pain, panic or nightmares) and the onset of PTSD. The higher the number of events, the more patients were at risk for PTSD.
The etiology of PTSD is multifactorial. PTSD risk factors are generally classified into modifiable and non-modifiable risk factors. The main unmodifiable risk factor is the history of psychiatric pathology at admission [11,20]. Female sex and young age 21 are found to be risk factors inconsistently in the literature. Modifiable risk factors include severe agitation 22 associated with the use of physical restraint and high doses of benzodiazepines or opioids [20- 23] However, these two factors are probably related because severe agitation can lead to an increase in benzodiazepine sedation, making a causal link difficult.
In our study, the result of the PTSS-10 survey were higher at 3 months in the “before” group than in the “after” group. Sedation doses were higher in the “before” group with delirium present in 80% of patients, compared with 50% in the “after” group. These results suggest that when sedation is deeper, or when there is delirium, patients are more likely to have PTSD. This is consistent with the literature data where when patients were interviewed during their stay, a low level of actual memories of the ICU stay and the presence of false memories about the stay would be predictive factors for an increase in the prevalence of PTSD [4,6,8] Decreased sedation decreases the risk of PTSD if the decrease in sedation corresponds to an increase in the number of days awake without delirium [4-25].
A poor quality of life is probably related to the presence of a depressive syndromes or significant anxiety, with persistent symptoms present in 40% of patients at 5 years after ICU discharge [26]. In our study, resuscitation had a moderate impact on quality of life with approximately 10% of patients having a severe impact. This result is stable at 3 months, 6 months and at one year. Few studies evaluate the impact of a stay in intensive care on the quality of life or whether it is essential for patients [27]. Many patients reported no longer having somatic attacks, but having difficulty returning to work or finding their place in the home. These data are difficult to quantify given the subjective nature of these reports. The recognized risk factors for poor quality of life are high age, female gender, severity of injuries, length of stay in the ICU and total hospital stay. In a Swedish study of 2010,26 153 patients were followed over 5.5 years. They noted an improvement in quality of life over time, and 75 % of patients went back to work at one year. False memories were the most influential factor on quality of life.
Our study has several limitations, which requires prudent conclusions and interpretations. First, it was a monocentric study. Second, there was a lack of power. Indeed, among the 1159 intubated patients, only 145 patients were included because of the strong recruitment of patients with neurological involvement at admission or a predictable sedation of less than 48 hours, which were the main non-inclusion factors. At 3 months of ICU discharge, only 63 patients could be contacted, i.e., 57% of patients surviving resuscitation and 38% at 1 year. In the literature, long-term follow-up of patients after resuscitation is difficult. This is explained in by mortality in the ICU. In our study, 32.4% of patients died before the 3rd month postresuscitation. This is also explained by the difficulty of re-contacting patients either because of a move, a change of coordinates or refusal by patients, or because of the inability of patients to answer the surveys (aphasia, deafness, etc.). Some patients, probably because of anxiety related to their hospitalization in the ICU, refused follow-up. The selection bias associated with this small size is important and must be considered when interpreting the results. A review of the 2007 literature found a loss of follow-up rate ranging from 10 to 70% [5].
The third limitation is the nonrandomized nature of the study, which may limit its impact; the two groups did not show any significant difference in the criteria studied, except for the significantly lower consumption of tobacco in the « After » group, which may have a beneficial impact on the occurrence of delirium and consequently in PTSD.
Finally, the fourth limitation is the bias of telephone data collection. It is possible that the responses were influenced by the method of collection compared to filling out a written survey by the patient directly or in a face-to-face interview with specialists (psychologists/psychiatrists).
Conclusion
Studies show that early management of PTSD decreases its longterm prevalence [28]. The stressors during an ICU stay are numerous and their consequences can be very significant with symptoms that prevent the resumption of social, professional or family activities. It seems essential to question the consequences of the disease and the care provided in ICUs beyond the simple fate of patients in terms of mortality, as the quality of life rather than the quantity of life becomes more important. A way improving quality of life in the literature is the creation of a logbook [29]. This bedside book is filled daily by the family and/or the caregivers and allows a reduction of false memories by restoring in a factual way the entire stay in the ICU. This logbook combats false memories and allows reduced PTSD [30]. It also facilitates support for families who can express themselves freely. Beyond the care of the patient, resuscitation is interesting in that it presents a high incidence of psychological distress within the families of patients [31].
It seems essential to offer patients with risk factors for PTSD appropriate assistance after discharge from their ICU stay, such as a consultation with a psychologist at 3 months, in order to maximize their quality of life.
Acknowledgements
In addition to the authors of this article, we thank all other physicians in the surgical ICU for their participation in the data collection. We also thank the nursing staff, residents, and secretaries of the intensive care unit for their cooperation with the protocol.
A particularly great thanks to the Department of Clinical Research, Pr Jean-Jacques Parienti for opening the E-crf, and Jean- Jacques Dutheil for making the booklets.
References
- Querques J, Stern TA. Overview of psychiatric epidemiologic issues in intensive care units. N Horiz Sci Pract Acute Med. 1998; 6: 314-320.
- Stein MB, Walker JR, Hazen AL, Forde DR. Full and partial posttraumatic stress disorder: findings from a community survey. Am J Psychiatry. 1997; 154: 1114-1119.
- Pochard F, Bellivier F. Trouble’s psychiatriques des malades hospitalisés en Réanimation. Ann Méd Psychol. 1996; 154: 489-498.
- Schelling G, Stoll C, Haller M, Briegel J, Manert W, Hummel T, et al. Healthrelated quality of life and posttraumatic stress disorder in survivors of the acute respiratory distress syndrome. Crit Care Med. 1998; 26: 651-659.
- Jackson JC, Hart RP, Gordon SM, Hopkins RO, Girard TD, Ely EW. Posttraumatic stress disorder and post-traumatic stress symptoms following critical illness in medical intensive care unit patients: assessing the magnitude of the problem. Crit Care. 2007; 11: 27.
- Kapfhammer HP, Rothenhausler HB, Krauseneck T, Stoll C, Schelling G. Posttraumatic stress disorder and health-related quality of life in long-term survivors of acute respiratory distress syndrome. Am J Psychiatry. 2004; 161: 45-52.
- Rattray JE, Johnston M, Wildsmith JA. Predictors of emotional outcomes of intensive care. Anesthesia. 2005; 60: 1085-1092.
- Jones C, Griffiths RD, Humphris G, Skirrow PM. Memory, delusions, and the development of acute posttraumatic stress disorder-related symptoms after intensive care. Crit Care Med. 2001; 29: 573-580.
- Scragg P, Jones A, Fauvel N. Psychological problems following ICU treatment. Anesthesia. 2001; 56: 9-14.
- Schnyder U, Moergeli H, Klaghofer R, Buddeberg C. Incidence and prediction of posttraumatic stress disorder symptoms in severely injured accident victims. Am J Psychiatry. 2001; 158: 594-599.
- Cuthbertson BH, Hull A, Strachan M, Scott J. Post-traumatic stress disorder after critical illness requiring general intensive care. Intensive Care Med. 2004; 30: 450-455.
- Davydow DS, Gifford JM, Desai SV, Needham DM, Bienvenu OJ. Posttraumatic stress disorder in general intensive care unit survivors: a systematic review. Gen Hosp Psychiatry. 2008; 30: 421-434.
- Boer KR, van Ruler O, van Emmerik AA, Sprangers MA, de Rooij SE, Vroom MB, et al. Factors associated with posttraumatic stress symptoms in a prospective cohort of patients after abdominal sepsis: a nomogram. Intensive Care Med. 2008; 34: 664-674.
- Granja C, Gomes E, Amaro A, Ribeiro O, Jones C, Carneiro A, et al. Understanding posttraumatic stress disorder-related symptoms after critical care: the early illness amnesia hypothesis. Crit Care Med. 2008; 36: 2801- 2809.
- Sessler CN, Gosnell MS, Grap MJ, Brophy GM, O’Neal PV, Keane KA, et al. The Richmond agitation-sedation scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002; 166: 1338- 1344.
- Ely EW, Truman B, Shintani A, Thomason JW, Wheeler AP, Gordon S, et al. Monitoring sedation status over time in ICU patients: reliability and validity of the Richmond Agitation-Sedation Scale (RASS). JAMA. 2003; 289: 2983- 2991.
- Payen JF, Bru O, Bosson JL, Lagrasta A, Novel E, Deschaux I, et al. Assessing pain in critically ill sedated patients by using a behavioral pain scale. Crit Care Med. 2001; 29: 2258-2263.
- Stoll C, Kapfhammer HP, Rothenhausler HB, Haller M, Briegel J, Schmidt M, et al. Sensitivity and specificity of a screening test to document traumatic experiences and to diagnose post-traumatic stress disorder in ARDS patients after intensive care treatment. Intensive Care Med. 1999; 25: 697-704.
- Baumann C, Erpelding ML, Regat S, Collin JF, Briancon S. The WHOQOLBREF questionnaire: French adult population norms for the physical health, psychological health and social relationship dimensions. Rev Epidemiol Sante Publique. 2010; 58: 33-39.
- Bienvenu OJ, Gellar J, Althouse BM, Colantuoni E, Sricharoenchai T, Mendez-Tellez PA, et al. Post-traumatic stress disorder symptoms after acute lung injury: a 2-year prospective longitudinal study. Psychol Med. 2013; 43: 2657-2671.
- Wade D, Hardy R, Howell D, Mythen M. Identifying clinical and acute psychological risk factors for PTSD after critical care: a systematic review. Minerva Anestesiol. 2013; 79: 944-963.
- Samuelson KA, Lundberg D, Fridlund B. Stressful memories and psychological distress in adult mechanically ventilated intensive care patients - a 2-month follow-up study. Acta Anaesthesiol Scand. 2007; 51: 671-678.
- Girard TD, Shintani AK, Jackson JC, Gordon SM, Pun BT, Henderson MS, et al. Risk factors for post-traumatic stress disorder symptoms following critical illness requiring mechanical ventilation: a prospective cohort study. Crit Care. 2007; 11: 28.
- Hager DN, Dinglas VD, Subhas S, Rowden AM, Neufeld KJ, Bienvenu OJ, et al. Reducing deep sedation and delirium in acute lung injury patients: a quality improvement project. Crit Care Med. 2013; 41: 1435-1442.
- Weinert CR, Sprenkle M. Post-ICU consequences of patient wakefulness and sedative exposure during mechanical ventilation. Intensive Care Med. 2008; 34: 82-90.
- Ringdal M, Plos K, Ortenwall P, Bergbom I. Memories and health-related quality of life after intensive care: a follow-up study. Crit Care Med. 2010; 38: 38-44.
- Daubin C, Chevalier S, Seguin A, Gaillard C, Valette X, Prevost F, et al. Predictors of mortality and short-term physical and cognitive dependence in critically ill persons 75 years and older: a prospective cohort study. Health Qual Life Outcomes. 2011; 9: 35.
- Peris A, Bonizzoli M, Iozzelli D, Migliaccio ML, Zagli G, Bacchereti A, et al. Early intra-intensive care unit psychological intervention promotes recovery from post traumatic stress disorders, anxiety and depression symptoms in critically ill patients. Crit Care. 2011; 15: 41.
- Garrouste-Orgeas M, Coquet I, Perier A, Timsit JF, Pochard F, Lancrin F, et al. Impact of an intensive care unit diary on psychological distress in patients and relatives. Crit Care Med. 2012; 40: 2033-2040.
- Jones C, Backman C, Capuzzo M, Egerod I, Flaatten H, Granja C, et al. Intensive care diaries reduce new onset post traumatic stress disorder following critical illness: a randomised, controlled trial. Crit Care. 2010; 14: 168.
- Jones C, Skirrow P, Griffiths RD, Humphris G, Ingleby S, Eddleston J, et al. Post-traumatic stress disorder-related symptoms in relatives of patients following intensive care. Intensive Care Med. 2004; 30: 456-460.