
Case Report
Austin Crit Care J. 2020; 7(1): 1031.
Central Venous Perforation Despite Non-Kinking of Guide Wire and Clinically Uneventful Catheter Placement
Schummer W¹* and Sakka SG²
¹Department of Anesthesiology, Helios Hospital Ueberlingen, Germany and Friedrich Schiller University Jena, Germany
²Department of Anesthesiology and Operative Intensive Care Medicine, University of Witten/Herdecke, Medical Centre Merheim, Cologne, Germany
*Corresponding author: Wolfram SCHUMMER, Department of Anesthesiology, Helios Hospital Ueberlingen, and Friedrich Schiller University Jena, Germany
Received: December 23, 2019; Accepted: January 20, 2020; Published: January 27, 2020
Abstract
Complication rate by central venous catheterization which is up to 15% may be related to numerous factors, e.g. physician’s experience, site of placement and use of ultrasound. Here, we present two critically ill patients with - ultrasoundguided in one and with landmark technique in the other - simultaneous placement of a central venous catheter and a hemodialysis catheter in whom despite nonkinking of the guide wire and uneventful placement in both cases resulted in a mediastinal malposition. Since potentially life-threatening complications may be associated with the misplacement further research is required.
Keywords: Central venous catheter; Vessel perforation; Complications
Introduction
Complication rate by central venous catheterization which is up to 15% may be related to numerous factors, e.g. physician’s experience, site of placement and use of ultrasound [1-3]. Here, we present two patients with - ultrasound-guided in one and with landmark technique in the other - simultaneous placement of a central venous catheter and a hemodialysis catheter in whom the latter despite uneventful placement in both cases resulted in a mediastinal malposition.
Case Reports
A 30-year old female (BMI 26.6 kg m-2) was transferred to our ICU requiring vasopressor support and renal replacement therapy. Due to clinical circumstances, a 3-lumen central venous catheter (CVC) and a double-lumen hemodialysis catheter (11F, length 20 cm) were placed. Under real-time ultrasound-guidance, the left internal jugular vein (LIJV) was punctured uneventfully twice. Ultrasound confirmed both guide wires within the LIJV. After advancement of the catheters to their final position blood could be aspirated over all lumen. Intravascular ECG was used for placement of the 3-lumen catheter, which was fixed on the skin level at 21 cm. Chest X-ray showed old and new catheters in place, however, a new homogenous loss of transparency of the left hemi-thorax was found (Figure 1A). Since injection of 0.9% saline into the hemodialysis catheter prior to renal replacement therapy caused retrosternal pain, computed tomography (CT) was performed immediately. The dialysis catheter was found with its tip in an extra luminal position in the anterior mediastinum. Fluid was seen close to the catheter tip (Figure 1B). A lesion of the aorta and a pericardial effusion were excluded. The massive left-sided pleural effusion required a chest tube which drained serous fluid. The hemodialysis catheter was removed uneventfully.
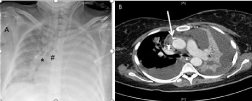
Figure 1: (A) (left) Chest X-ray (anterior-posterior) showing the left-sided
3-lumen catheter (*) and the 11F-hemodialysis catheter (#) in place. L= left (B)
(right) Computed tomography after i.v. injection of contrast medium showing
extra-vascular position of the hemodialysis catheter’s tip as indicated by the
arrow.
A 67-year old male was admitted to the ICU in shock and renal failure while receiving norepinephrine (0.3 μg kg-1 min-1) via a peripheral cannula. Besides hemodynamic instability the patient’s shape was unfavorable (BMI 49.2 kg m-2, no neck situation and a beard). Because of the high BMI and several bypass surgeries due to an arterial occlusive disease, both femoral sites were regarded not suitable for catheterization. Accordingly, the right subclavian vein (RSV) was punctured twice for placement of a multi-lumen central venous catheter (CVC) and a double-lumen dialysis catheter. Both punctures were uneventful, no resistance was met while advancing the guide wires, and after skin incisions the dilators could be inserted easily without force. While inserting the dilators to the subclavian vein the guide wires were slightly moved to and fro in order to detect a kink in the guide wire. No undue resistances were met. Under ECG-guidance the CVC was inserted 20 cm; blood could easily be aspirated via all lumen and pressure monitoring through the distal lumen confirmed venous position. The dialysis catheter was advanced to its entire length of 17.5 cm; however, surprisingly there was no return of blood. Thus, this catheter was exchanged against a 20 cm single lumen CVC over the same guide wire. Blood could be aspirated and venous position was again confirmed by pressure monitoring. Then, the CVC was exchanged against a 20 cm dialysis catheter which was inserted entirely to 20 cm. Blood return as well as venous position were confirmed. Vasopressor administration was switched to the CVC without noticeable problems. However, about 20-30 min later the patient developed respiratory arrest. During intubation vasopressor requirement increased substantially along with begin of CPR. A chest X-ray taken 15 min after begin of CPR showed both catheters in projection of the superior vena cava (SVC) (Figure 2) and a new opacity of the right hemi-thorax. Pericardial tamponade was excluded by transthoracic echocardiography (sub-xiphoid approach). Arguing that the subclavian catheters might be misplaced, venous access was sought via the femoral vessels under ultrasound guidance and finally was successful. A right-sided chest tube was inserted urgently, which drained sanguineous fluid. However, after 1.5 hours of unsuccessful CPR all efforts were suspended and the patient was declared dead. Public prosecution service was informed, however, unfortunately no forensic autopsy was ordered.
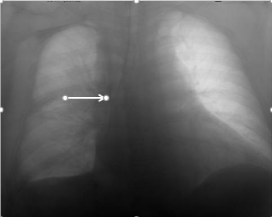
Figure 2: Chest X-ray (anterior-posterior) under CPR showing multi-lumen
central venous catheter and hemodialysis catheter with projection to the
superior vena cava (arrow).
Discussion
Central venous catheterization especially by large-bore catheters may be associated with life-threatening complications [4]. Recently, Wong et al. [5] reported migration of a central venous hemodialysis catheter inserted through the right internal jugular vein (RIJV) under fluoroscopy causing left atrial perforation. An altered mental status shortly after the first dialysis session resulted in a CT scan. Here, it could be shown that the catheter passed through the medial wall of the SVC and the posterior wall of the left atrium. In this patient, extracorporeal circulation was required to safely remove the catheter [5]. In our first patient, malposition of the hemodialysis catheter was suspected directly after insertion since pain during injection of fluid occurred. Fortunately, following immediate diagnostics the catheter was removed uneventfully.
However, our second patient unfortunately died. Despite lack of problems during insertion, the catheter caused a lethal complication. Since no autopsy was performed, we can only speculate on the reasons for misfortune. First, unknown stenosis of SVC as reported earlier [4] may have been present but seems unlikely. Second, arterial puncture seems unlikely due to definite proof of venous pressure waveform. However, right subclavian and left internal jugular veins are vessels associated with a higher complication rate when compared to others [6]. In our patients, it could be argued being due to persistent redirecting guide wire because of the variable angles between major veins. However, this explanation seems insofar unlikely too, as no difficulties or resistances were met while advancing the wires. Noteworthy, pericardial tamponade due to perforation of the SVC below the pericardial reflection was excluded by CT and transthoracic echocardiography, respectively. Thus, perforation of the brachiocephalic vein or the SVC is the most probable explanation in patient #2. It should be appreciated that stiffer devices like hemodialysis catheters and the respective dilators may not be able to follow a guide wire around tight corners (LIJV and RSV) with the risk of vein damage [7].
Common in both cases are extremely experienced operators, sites at risk (LIJV and RSV) as well as the use of non-kinking wires. Normally, one is expecting the guide-wire being kinked or distorted if a large-bore catheter is not following the guide wires path and/or excessive force had been exerted [8].
To the best of our knowledge this is the first report on venous vessel perforation while placing large-bore catheters where firstly guide wires were not kinked and secondly no undue forces were applied. Thus, we would like to draw attention on these cases and the possible underlying mechanisms.
In conclusion, our report emphasizes the need for careful management during and following insertion of a central venous catheter, even if initial placement seemed to have been uneventful – especially in hemodialysis catheters via the left internal jugular and right subclavian routes.
Authors’ Contribution and Authorship
Wolfram Schummer, MD, PhD, DEAA, EDIC: substantial contribution to conception and design, acquisition of data, or analysis and interpretation of data; drafting the article or revising it critically for important intellectual content; final approval of the version to be published; and agreement to be accountable for all aspects of the work thereby ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Samir G. Sakka, MD, PhD, DEAA, EDIC: substantial contribution to conception and design, acquisition of data, or analysis and interpretation of data; drafting the article or revising it critically for important intellectual content; final approval of the version to be published; and agreement to be accountable for all aspects of the work thereby ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
All authors have agreed and are accountable for all aspects of the work thereby ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
References
- Taylor RW, Palagiri AV. Central venous catheterization. Crit Care Med. 2007; 35: 1390-1396.
- Schummer W, Köditz JA, Schelenz C, Reinhart K, Sakka SG. Pre-procedure ultrasound increases the success and safety of central venous catheterization. Br J Anaesth. 2014; 113: 122-129.
- Smit JM, Raadsen R, Blans MJ, Petjak M, Van de Ven PM, Tuinman PR. Bedside ultrasound to detect central venous catheter misplacement and associated iatrogenic complications: a systematic review and meta-analysis. Crit Care. 2018; 22: 65.
- Schummer W, Schummer C, Fritz H. Perforation of the superior vena cava due to unrecognized stenosis. Case report of a lethal complication of central venous catheterization. Anaesthesist. 2001; 50: 772-727.
- Wong K, Marks BA, Qureshi A, Stemm JJ. Migration of a central venous catheter in a hemodialysis patient resulted in left atrial perforation and thrombus formation requiring open heart surgery. Anesth Analg Case Rep. 2016; 7: 21-23.
- Schummer W, Schummer C, Rose N, Niesen WD, Sakka SG. Mechanical complications and malpositions of central venous cannulations by experienced operators. A prospective study of 1794 catheterizations in critically ill patients. Intensive Care Med. 2007; 33: 1055-1059.
- Gibson F, Bodenham A. Misplaced central venous catheters: applied anatomy and practical management. Br J Anaesth. 2013; 110: 333-346.
- Jankovic Z, Boon A, Prasad R. Fatal haemothorax following large-bore percutaneous cannulation before liver transplantation. Br J Anaesth. 2005; 95: 472-476.