
Research Article
Austin Crit Care J. 2020; 7(1): 1032.
Can a Video be an Effective Tool to Treat Preoperative Anxiety in Minor Procedures?
Sonzini R1, Fusetti C2, Ceruti S3*, Musiari M4, Minotti B5, Cafarotti S6, La Regina D7 and Saporito A5
1Department of General Surgery, Clinica Luganese – Lugano (CH), Switzerland
2Department of Hand Surgery Unit, Orthopaedics and Trauma Dpt, ORBV – Bellinzona (CH), Switzerland
3Department of Intensive Care, Geneva University Hospital (HUG) - Geneva (CH), Switzerland
4Service of Anesthesiology, HFR – Fribourg (CH), Switzerland
5Service of Anesthesiology, ORBV - Bellinzona (CH), Switzerland
6Department of Thoracic Surgery, ORBV - Bellinzona (CH), Switzerland
7Department of General Surgery, ORBV - Bellinzona (CH), Switzerland
*Corresponding author: Samuele Ceruti, Intensive Care Unit Geneva University Hospital (HUG) - Geneva (CH) Clinica Luganese SAVia Moncucco 10a, Switzerland
Received: December 27, 2019; Accepted: January 24, 2020; Published: January 31, 2020
Abstract
Introduction: Preoperative anxiety has an impact on surgical outcome and patient’s satisfaction. An important component could be anesthesia-related; suitable patients’ information was shown to reduce it, but data are conflicting. The aim was to assess the impact of a video on anxiety level in outpatients’ hand surgery setting.
Methods: Single-centre, before-after, case-control trial to assess the impact of a video on preoperative anxiety. Outcomes were the difference in anxiety levels measured by a structured survey, including the use of an adapted Visual Analogue Scale (VAS-A) and analysis of vital signs’ evolution.
Results: 93 consecutive patients were enrolled, 46 in control group, 47 in video group. Anxiety measured on admission did not differ; the Educational Video did not change patient anxiety level when second assessment was performed. Systolic arterial pressure measured on admission was significantly higher in the video group, while other vital signs did not differ. For each point of the satisfaction survey, mean rating did not differ significantly in video group compared to control group. In patients with VAS-A greater than 3, however, survey evaluation showed a little beneficial effect.
Conclusions: Informative video did not seem to reduce preoperative anxiety in general population, but it could have the potential to increase patients’ satisfaction in very anxious patients.
Keywords: Perioperative anxiety; Pre-anesthetic assessment; Educational video; Regional anesthesia; Ambulatory surgery
Abbreviations
ASA: American Society of Anaesthesiology; IVRA: Intravenous Regional Anaesthesia; STAI: State Trait Anxiety Inventory; VAS-A: Visual Analogue Scale – Adapted.
Introduction
Preoperative anxiety is a common state in surgical setting, reporting to have prevalence up to 60-80% [1-7]. It is burdened by clinical occurrences, like hemodynamic modifications (i.e. arterial hypertension and arrhythmias) and neurological changes, with an increasing in post-operative pain awareness and in anaesthetics amount prescription [8-10]. These elements lead to an increase of analgesics treatment and post-operative in-hospital length of stay [3,11-13], potentially getting worse overall surgical outcome. Therefore, perioperative anxiety can reduce patient’s general satisfaction about quality of perioperative care [14-17]; this satisfaction is largely based on patient’s expectations and it has concretes consequences: pleased patients are more likely to maintain good relationships with the surgeon, to abstain from the so-called “doctor shopping”, to avoid malpractice proceedings and to have a better compliance regarding postoperative prescriptions [18], attending regularly to follow-up examinations [19].
Previous studies showed that one of the main sources of preoperative anxiety was represented by the anesthesia, as well as surgery itself [20]. This distress was usually related to a lack of information about anesthetic procedure [21]. The relevance of preoperative anxiety is largely underestimated in outpatient setting, where elective minor surgical procedures are often not related as potential source of preoperative anxiety. While is shown that in the outpatient setting major complications are surgery-related, surgical outcome can be affected by psychological factors [22,23] such as anxiety, particularly in case in which patient’s compliance is crucial.
Previous trials show that better information about surgery reduces anxiety and patient’s apprehension [24]. In order to address the matter of anesthesia induced anxiety, it is needed to develop a systematic methodology to identify the patients who would benefit the most from a more detailed set of information regarding anaesthesia. Some strategies have been implemented in order to reduce preoperative stress [25-29]: together with information directly given by physicians, it is shown that also written information may have a positive impact on anxiety relief, while the correct evaluation of the information given is largely dependent on patient’s health literacy.
Multimedia information are generally easier to understand, some clinical trials shown a clear anxiolytic effect with the use educational videos [7,25,30,31], but data are conflicting [32,33], usually due to a great heterogeneity in methods and in patients’ selection. The aim of the study is to assess the effectiveness of our educational video on preoperative anxiety and on overall satisfaction levels, in patients undergoing minor elective outpatient hand surgery procedures.
Methods
This was a single centre, case-control, before-after study, whose primary outcome was to assess the impact of an educational video on perioperative anxiety level in outpatient surgical setting. Hospital Quality Service produced this video as an informational tool for patients undergoing elective outpatient hand surgery, to easily explain intravenous regional anaesthesia; indeed, in our institution these patients usually do not see any anaesthesiologist the day before surgery. Informed consent about using anonymized data was obtained prior to proceed, according to our Ethical Board commission statement. Over a period of one month after the introduction of the informational video, consecutive adult patients scheduled for elective outpatient hand surgery with an intravenous regional anesthesia (IVRA) was then assessed regarding their preoperative anxiety level and their vital signs (both before than after the video), comparing them to the cohort of consecutive patients previously seen, enrolled during the month before video introduction. The overall management of these patients during the control and treatment period was similar.
Inclusion criteria included patients of both sexes, older than 18 years, with a perioperative ASA risk I-III, undergoing elective handsurgery procedure and anesthetized by IVRA. Exclusion criteria were chosen to avoid any data-distortion due to any anxiolytic drug and were the following: on-going anxiolytic or anti-depressive therapy or regular use of anxiolytic drugs and previous diagnosis of anxiety or psychiatric disorders.
Structured survey
The evaluation of anxiety status depends on a personal; therefore subjective experience of anxiety-related aspects regarded as important to oneself. In this context, information about anxiety was obtained by a structured questionnaire which included subjective parameters like anxiety level (evaluated by a specific semi quantitative score, named VAS-score, as discussed later) and objective data like demographic information (age and sex) and vital signs (arterial pressure, heart rate, peripheral saturation). The VAS-A (Visual Analogue Scale Adapted) is semi-quantitative valid instrument used for measuring anxiety [33- 36]. It consists of a graduated scale from 0 (no anxiety) to 5 (maximal anxiety) to measure patients’ anxiety levels, requiring that each patient should identify its own level of anxiety oneself.
Educational video
Patients in the video group watched the video using a laptop and VAS score was repeated after the video. The video was shot by the Anaesthesiology department team, in order to explain and show in a detailed and yet easy way the sequence of events that occurs between the arrival of patients in the OR and the performance of IVRA as well as all the steps of which IVRA consists of. The video began with an actress interpreting a patient scheduled for an elective outpatient hand surgery procedure acceding the day hospital clinic. It showed the interaction between the patient and the nurses who explain in detail what is going to happen next and lead her through the preparation routine. The camera then followed the patient as she is accompanied to the induction room and the video showed all the details of the checks made as the patient accedes the operating room, the time-out and the preparation for the anesthetic procedure, with the monitoring of the vital parameters. Then the IVRA procedure was shown in detail with an anesthesiologist explaining it step by step. The video concluded with the patient brought to the operating room awake and pain free, as a simulated procedure begins.
Protocol procedure
In our institution outpatient hand-surgery patients’ treatment was standardized according to a detailed perioperative protocol (available as Supplementary Material). All patients were distributed into two groups. The first group (intended as control group) underwent a surgical pre-operative examination, during which received detailed information about surgical procedure but not regarding anesthetic technique. Standard allocated time for each preoperative visit was around 15 minutes. Patients were then admitted the day of surgery to the day hospital clinic, 2-3 hours before the operation; vital signs (like non-invasive arterial blood pressure, heart rate and respiratory rate) were checked and patients were asked to evaluate their preoperative anxiety level on a visual analogue scale (VAS). Patients belonging to the control group didn’t watch the educational video about anesthesia techniques and proceed directly to operating theatre for anesthetic procedure, as usual. Instead, the video group received the same preoperative preparation procedure, watching in addition the 6-minute educational video about IVRA. At the end of this video, and at least 30 minutes before the transfer to the operating theatre, video-group patients reassessed their own anxiety level with the VAS-A scale and vital signs. Finally, in both groups vital signs were recorded once again on arrival in the operating theatre, monitored and registered throughout the entire anesthetic procedure. At the end of the procedure, when patients were transferred to the operating room, VAS-A score and vital signs were recorded for the last time.
IVRA was performed by an anesthesiologist in the induction room outside the operating theatre, using a standardized procedure. Two intravenous lines were placed on each hand; after proximal tourniquet inflation at 300 mmHg, a total volume of 40 ml of chloroprocaine 0.5% was injected intravenously in the operated limb until complete arm anesthesia is achieved. At this point, the tourniquet is deflated, vital signs are constantly monitored and the patient was then transferred to the OR; 10 minutes after local anesthetic injection, the surgeon tested loss of sensitivity with a pinprick test, after which surgery began.
Outcomes
Primary outcome was the difference in preoperative anxiety levels between two groups, measured on a visual analogue scale, like the VAS-A score. Secondary outcomes were any differences in perioperative vital signs that are usually affected by anxiety (like arterial blood pressure [mmHg], breath rate [breath per minute] and heart rate [beat per minute]). This outcome was further analysed in a subgroup of subjectively anxious patients.
Statistic
A power analysis was conducted; according to Ayral et al37, and to clinically estimated relevance of diminution for anxiety, assuming a reduction of at least 50% in preoperative anxiety level as clinically significant, 45 patients per group were necessary (allowing for dropouts) to reach a 95% level of significance with a power of 90%. We conducted a statistical frequency analysis regarding common vitals parameters and anxiety level according to VAS-scale at arrival in the hospital, before to go to the pre-operative room and at arrival at the pre-operative room, performing a statistical frequency analysis comparing all these three steps and all subgroup according to secondary outcomes. All numeric variables were shown as mean and standard deviation, or as number and percentage. All data were registered and stored in a specific and protected archive in Anesthesia Department, accessible only by investigators; they were than anonymously transferred into an electronic database in order to be analysed.
Results
Between February 2013 and May 2013, 46 consecutive hand surgery patients operated in our Institute as outpatients saw the informative video; they were examined regarding anxiety levels and vital signs. The control group consisted of 47 consecutive patients admitted between September 2012 and December 2012, using the same inclusion/exclusion criteria. During the control period, patients didn’t see any educational video. Throughout the screening phase, 59 patients were excluded due to their chronic use of anxiolytics, according to previous defined criteria (Figure 1).
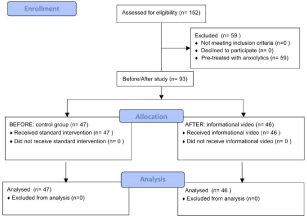
Figure 1: Study flow-chart.
Population characteristics did not differ in age, gender and level of anxiety on admission (Table 1). Anxiety level measured on admission in the hospital did not differ between two groups (1.22 vs 1.02, p 0.417) and the Patient Education Video did not significantly change this level when the second assessment was performed (1.22 vs 1.29, p 0.774). Systolic arterial pressure measured on admission in the day-hospital clinic was significantly higher in the video group (140 mmHg vs 129 mmHg), while other measured parameters like diastolic blood pressure heart rate and respiratory rate did not differ between the two groups (Table 1).
TABLECREATED
Table 1: Baseline patients’ characteristics. Data are expressed as “mean (SD)”. SAP: Systolic Arterial Pressure, DAP: Diastolic Arterial Pressure, HR: Heart Rate, RR: Respiratory Rate.
In video-group patients, after the video was shown and patients were transferred to the operating theatre, systolic and diastolic blood pressure as well as respiratory rate did not change significantly (vs 2), while heart rate did significantly increase and was significantly higher than in the control group at the same moment (from 75 to 90 bpm, p < 0.001). In the control group, all vital signs measured pre/post- anaesthesia did not change significantly (Figure 2). Other parameters did not diverge significantly between two groups (Figure 3). Finally, mean rating for each point of the satisfaction survey did not differ significantly in video group compared to control group (Table 2). When a subgroup analysis was performed about all patients self-evaluated as “anxious person” (N=26), some differences were highlighted in patients to whom the video was shown: systolic arterial blood pressure measured at induction point was significantly lower in patients after they watched the video (150 mmHg vs 129 mmHg, p 0.04).
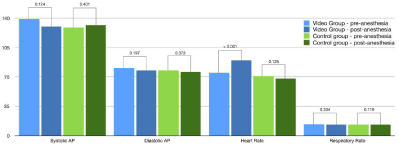
Figure 2: Pre/post-anesthesia intra-group comparison about main vital signs. The only significant difference was in the video-group with an isolate increase in
heart rate. Please refer to the text for more details.

Figure 3: Inter-group comparison about vital signs before the anesthesia (Figure 3A) and just after regional anesthesia (Figure 3B). Both groups showed no
significant differences, except for an increase in post-anesthesia heart rate in video-group patients. Please refer to the text for more details.
TABLECREATED
Table 2: Satisfaction survey results. All items were rated on a 0 to 10 numeric scale (0 worse, 10 best). Data are expressed as “mean (SD)”. As discussed in the text, there was no significant difference between two groups.
Discussion
The effect of educational video on patient anxiety level has already been debated in the last decade; some studies showed encouraging effects in reducing anxiety and improving satisfaction in patients undergoing many different surgical procedures [7,37-44] while some others denied these results [45-47]. To the best of our knowledge, this was the first before-after trial addressing this particular topic in local anesthesia setting just before minor hand surgery.
Our results did not confirm the hypothesis of a positive effect of Patient Education Video on preoperative anxiety: in fact, patients who watched our video did not significantly differ in own anxiety levels from control patients. On the other hand, the video did not increase patient discomfort, as shown by other Authors, like Pager et al [18]. This difference in studies results can be addressed to several factors, not last the disparities in the health literacy levels of the population, determining a degree of variability in managing stress or in the comprehension of information conveyed by the video.
In our trial the absence of an anxiolytic effect by the video can be explained by further circumstances, as established by other Authors [48]. In our clinical context, patients met the surgeon before admission, and were informed at the same time about the whole procedure and other aspects of their perioperative management; this could have mitigated effects of further information conveyed by the video. However, even if the surgeon cited the type of anesthesia (IVRA), he did not go into details and, at the time of surgical assessment, patients were not informed about what the anesthetic technique consists of.
Patients who looked the video displayed subsequent significant increase in heart rate, but this fact didn’t correlate with a change of anxiety score. However, a subconscious increase in anxiety awareness cannot be excluded; in this case, the video would have deleterious effects. Nevertheless, many confounding factors could have determined these results and the lack of significant differences in all other vital signs tends to exclude this hypothesis. With this trial we chose to focus on the role of anesthesia and we did not explore the effects of other potential sources of anxiety, as surgical techniques, success rate of the operation, specific surgery complication rate, information provided by the surgeon about the procedure, surgeonpatient relationship, cultural milieu, etc…
As found by Yellen et al [47], the overall level of patient satisfaction was not affected by the video, except for self-reported anxious patients. In this specific subgroup, the video was particularly appreciated and concurred to significantly increase the satisfaction. One can speculate that in this context, informative videos can thus be integrated into the preoperative educational process to increase patient satisfaction.
This study had several limitations. First, there is currently no clear consensus on clinical impact neither about preoperative anxiety, nor about a standardized technique to estimate it. In order to measure anxiety levels with a simple and reproducible method, we adopted the VAS score: this method can be less subtle in detecting minimal changes in anxiety level compared to other scores [36] but allows an effective and clear measurement of preoperative subjective anxiety, even in patients with reading or comprehension difficulties [34]. Second, the type of surgery has been shown to influence anxiety levels; our study population consisted completely of day-hospital patients undergoing minor hand surgery procedures and thus likely to have lower starting level of anxiety. It is possible that the effectiveness of the video was cushioned, given that patients started from lower anxiety levels. Third, the statistical significance of this before-after study was not strong enough to obtain definitive conclusions; in this context, further prospective randomized trials will be required to confirm these results. Finally, this study didn’t evaluate the personality traits of the patients in relationship with their level of anxiety and the analysis of anxiety and satisfaction levels was limited at the time of a day-hospital clinic stay. A follow-up to assess long-term impact on satisfaction was not performed and could be the topic for another study.
Conclusion
Pre-operative educational video doesn’t appear an effective method capable to reduce preoperative anxiety and to change global patient satisfaction in outpatients setting. A subgroup of patients, however, with very high levels of anxiety showed a little trend toward a positive effect of this educational video on their overall satisfaction. Therefore, actually the use of a video education cannot be justified in the perioperative phase; further studies will be necessary to better identify further subgroups of patients that could benefit from this methodology.
Acknowledgement
Ethic approval and consent to participate
A verbal informed consent was obtained from all patients about use of their anonymized data. We previously contacted our local Ethic Committee (“Comitato Etico Cantonale”, Via Orico 4, 6500 Bellinzona). Due to the nature of this retrospective study, about a video already approved by local Hospital Quality Service, local Ethic Committee ruled out no formal ethics approval in this particular case. All study complies with national guidelines, in this case SwissEthic (https://www.swissethics.ch/gesetzrichtl_f.html).
Consent to publish
All Authors give their consents to publish this study. Corresponding author attests that the manuscript submitted and all related materials are, unless noted, original and have not been published elsewhere.Furthermore, the corresponding author attests that the submission is not under consideration for publication elsewhere, in whole or in any significant part.No substantial part of a paper may have been published elsewhere, except as a scientific abstract.
References
- Johnston M. Anxiety in surgical patients. Psychol Med. 1980; 10: 145-152.
- Domar AD, Everett LL, Keller MG. Preoperative anxiety: is it a predictable entity? Anesth Analg. 1989; 69: 763-767.
- Badner NH, Nielson WR, Munk S, Kwiatkowska C, Gelb AW. Preoperative anxiety: detection and contributing factors. Can J Anaesth. 1990; 37: 444- 447.
- Macario A, Weinger M, Carney S, Kim A. Which clinical anesthesia outcomes are important to avoid? The perspective of patients. Anesth Analg. 1999; 89: 652-658.
- Oldman M, Moore D, Collins S. Drug patient information leaflets in anaestanesthesia: effect on anxiety and patient satisfaction. Br J Anaesth. 2004; 92: 854-858.
- Norris W, Baird WL. Pre-operative anxiety: a study of the incidence and aetiology. Br J Anaesth. 1967; 39: 503-509.
- Doering S, Katzlberger F, Rumpold G, Krismer M, Luz G, Innerhofer P, et al. Videotape preparation of patients before hip replacement surgery reduces stress. Psychosom Med. 2000; 62: 365-373.
- Williams JG, Jones JR. Psychophysiological responses to anesthesia and operation. J Am Med Assoc. 1968; 203: 415-417.
- McCleane GJ, Cooper R. The nature of pre-operative anxiety. Anaesthesia. 1990; 45: 153-155.
- Goldmann L, Ogg TW, Levey AB. Hypnosis and daycase anaesthesia. A study to reduce pre-operative anxiety and intra-operative anaesthetic requirements. Anaesthesia. 1988; 43: 466-469.
- Ip HY, Abrishami A, Peng PW, Wong J, Chung F. Predictors of postoperative pain and analgesic consumption: a qualitative systematic review. Anesthesiology. 2009; 111: 657-677.
- Thomas T, Robinson C, Champion D, McKell M, Pell M. Prediction and assessment of the severity of post-operative pain and of satisfaction with management. Pain. 1998; 75: 177-185.
- Lee A, Chui PT, Gin T. Educating patients about anesthesia: a systematic review of randomized controlled trials of media-based interventions. Anesth Analg. 2003; 96: 1424-1431.
- Caumo W, Schmidt AP, Bergamann J, Ivamoto CW, Adamatti LC, Ferreira MB, et al. Risk factors for preoperative anxiety in adults. Acta Anaesthesiology Scandinavica. 2001; 45; 298-307.
- Grossi G, Perski A, Feleke E, Jacobson U. State anxiety predicts poor psychosocial outcome after coronary bypass surgery. International Journal Behavioral Medicine. 1998; 5: 1-16.
- Jones MP, Ebert CC, Sloan T, Spanier J, Bansal A, Howden CW, et al. Patient anxiety and elective gastrointestinal endoscopy. Journal of Clinic Gastroenterology. 2004; 38: 35-40.
- Takahashi Y, Tanaka H, Kinjo M, Sakumoto K. Prospective evaluation of factors predicting difficulty and pain during sedation-free colonoscopy. Disease of the Colon & Rectum. 2005; 48:1295-1300.
- Pager CK. Randomised controlled trial of preoperative information to improve satisfaction with cataract surgery. British Journal of Ophtalmology. 2005; 89: 10-13.
- Freed LH, Ellen JM, Irwin CE, Millinstein SG. Determinants of adolescents’ satisfaction with health care providers and intentions to keep follow-up appointments. J Adolesc Health. 1998; 22: 475-479.
- Rohaiyem ME, Alshehri AA, Saade M, Shoabi TA, Zaboor H, Tawfeeg NA. Fear of going under general anesthesia: a cross-sectional study. Saudi J Anaesth. 2016; 10: 317-321.
- Ramsay MA. survey of pre-operative fear. Anaesthesia. 1972; 27: 396-402.
- Baker WH. Medical meeting: the real value. Bull Am Coll Surg. 2001; 86: 13-18.
- Sigdel S. Perioperative anxiety: a short review. Glob Anesth Perioper Med. 2015; 1: 107-108.
- Kiyohara LY, Kavano LK, Oliveira LM, Yamamoto MU, Inagaki MM, Ogawa NY, et al. Surgery information reduces anxiety in the pre-operative period. Rev Hosp Clin Fac Med Sao Paulo. 2004; 59: 51-56.
- Bondy LR, Sims N, Schroeder DR, Offord KP, Narr BJ. The effect of anesthetic patient education on preoperative patient anxiety. Reg Anesth Pain Med. 1999; 24: 158-164.
- Hughes S. The effects of giving patients pre-operative information. Nurs Stand. 2002; 16: 33-37.
- Klopfenstein CE, Forster A, Van Gessel E. Anesthetic assessment in an outpatient consultation clinic reduces preoperative anxiety. Can J Anaesth. 2000; 47: 511-515.
- Olver IN, Turrell SJ, Olszewski NA, Willson KJ. Impact of an information and consent form on patients having chemotherapy. Med J Aust. 1995; 162: 82- 83.
- Stanley BM, Walters DJ, Maddern GJ. Informed consent: how much information is enough? Aust N Z J Surg. 1998; 68: 788-791.
- Crowe J, Henderson J. Pre-arthroplasty rehabilitation is effective in reducing hospital stay. Can J Occup Ther. 2003; 70: 88-96.
- Lee A, Gin T. Educating patients about anaesthesia: effect of various modes on patients’ knowledge, anxiety and satisfaction. Curr Opin Anaesthesiol. 2005; 18: 205-208.
- Done ML, Lee A. The use of a video to convey preanesthetic information to patients undergoing ambulatory surgery. Anesth Analg. 1998; 87: 531-536.
- Jlala HA, French Jl, Foxall GL, Hardman JG, Bedforth NM. Effect of preoperative multimedia information on preoperative anxiety in patients undergoing procedures under regional anaesthesia. British Journal of Anesthesia. 2010; 104: 369-374.
- Kindler CH, Harms C, Amsler F, Ihde-Scholl T, Scheidegger D. The visual analogue scale allows effective measurement of pre- operative anxiety and detection of patients’ anesthetic concerns. Anesth Analg. 2000; 90: 706 -712.
- Facco E, Stellini E, Bacci C, Manani G, Pavan C, Cavallin F, et al. Validation of visual analogue scale for anxiety (VAS-A) in preanesthesia evaluation. Minerva Anestesiol. 2013; 79: 1389-1395.
- Spielberger CD, Lushene RE, Jacobs GA. Manual for the State-Trait Anxiety Inventory, STAI (Form Y). Palo Alto, CA: Consulting Psychologists Press, 1983.
- Ayral X, Gicquere C, Duhalde A, Boucheny D, Dougados M. Effects of video information on preoperative anxiety level and tolerability of joint lavage in knee osteoarthritis. Arthritis & Rheumatology. 2002; 47: 380-382.
- Arabul M, Candemir A, Celik M, Alper E, Akpinar Z, Aslan F, et al. Impact of an information video before colonoscopy on patient satisfaction and anxiety. The Turkish Journal of Gastroenterology. 2012; 23: 523-529.
- Crabtree TD, Puri V, Bell JM, Bontumasi N, Kreisel D, Krupnick AS, et al. Outcomes and perception of lung surgery with implementation of a patient video education module: a prospective cohort study. Journal of American College of Surgeons. 2014; 214: 816-821.
- Cornoiu A, Beischer AD, Donnan L. Multimedia patient education to assist the informed consent process for knee arthroscopy. ANZ Journal of Surgery. 2011; 81: 176-180.
- Chahraoui K, Frachebois L, Jebrane A, Moutel G, Herve C. Effects of an informational CD-ROM on anxiety and knowledge before aesthetic surgery: a randomised trial. British Journal of Plastic Surgery. 2005; 58: 379-383.
- Luck A, Pearson S, Maddem G, Hewett P. Effects of video information on precolonoscopy anxiety and knowledge: a randomised trial. Lancet. 1999; 354: 2032-2035.
- Zieren J, Menenakos C, Mueller JM. Does an informative video before inguinal hernia surgical repair influence postoperative quality of life? Results of a prospective randomized study. Quality of Life Research. 2007; 16: 725- 729.
- Eley VA, Searles T, Donovan K, Walters E. Effect of an anaesthesia information video on preoperative maternal anxiety and postoperative satisfaction in elective caesarean section: a prospective randomized trial. Anesthesia Intensive Care Journal. 2013; 41: 774-781.
- Harrison R, Dey P, Slevin NJ, Gibbs A, Cowan R, Logue JP, et al. Randomized controlled trial to assess the effectiveness of a videotape about radiotherapy. British Journal of Cancer. 2005; 84: 8-10.
- Yellen EA, Ricard R. The effect of a preadmission videotape on patient satisfaction. Association of perioperative Registered Nurse Journal. 2005; 81: 831-842.
- Sorlie T, Busund R, Sexton J, Sexton H, Sorlie D. Video information combined with individualized information sessions: effects upon emotional well-being following coronary artery bypass surgery. A randomized trial. Patient Education and Counseling Journal. 2007; 65: 180-188.
- Rosiek A. Evaluation of Stress Intensity and Anxiety Level in Preoperative Period of Cardiac Patients, BioMed Research International. 2016.