
Review Article
Austin Crit Care J. 2021; 8(1): 1034.
Current Nutritional Support in Critical Ill Covid-19 Patients: A Brief Review
Pahlavani N1,2* and Navashenaq JG3
1Social Development and Health Promotion Research Center, Gonabad University of Medical Sciences, Iran
2Cellular and Molecular Research Center, Research Institute for Health Development, Kurdistan University of Medical Sciences, Sanandaj, Iran
3Noncommunicable Diseases Research Center, Bam University of Medical Sciences, Bam, Iran
*Corresponding author: Naseh Pahlavani, Social Development and Health Promotion Research Center, Gonabad University of Medical Sciences, Gonabad, Iran
Received: March 17, 2021; Accepted: April 05, 2021; Published: April 12, 2021
Abstract
Covid-19 is a high prevalence of pneumonia of pathless cause in that started in 2019 in Wuhan, Hubei Province, China. Five to 10% of the coronavirus SARSCoV- 2-infected patients, i.e., with new coronavirus disease 2019 (COVID-19), are presenting with an Acute Respiratory Distress Syndrome (ARDS) requiring urgent respiratory and hemodynamic support in the Intensive Care Unit (ICU). However, nutrition is an important element of care. The nutritional assessment and the early nutritional care management of COVID-19 patients must be integrated into the overall therapeutic strategy. Absence of treatment for this new virus, finding alternative methods to prevent and control the disease is important. Having a well-functioning immune system is essential for the host’s defense against pathogenic organisms. Malnutrition can lead to an impaired immune system during life. Even though the immune system response to infection is itself a factor that could lead to nutritional status impairment. Deficiency of some nutrients can lead to disorders of immune system. Adequate intake of vitamins (A, D, Bs, C and E), minerals (selenium, zinc and iron) and omega-3 fatty acids are among the essential factors in proper immune system function and the international recommendations on nutrition in the ICU should be followed. Some specific issues about the nutrition of the COVID-19 patients in the ICU should be emphasized. We propose a flow chart and ten key issues for optimizing the nutrition management of COVID-19 patients in the ICU.
Keywords: COVID-19; Critical ill; Nutritional support
Introduction
In December 2019, there was a prevalence of pneumonia of pathless cause in Wuhan, Hubei Province, China, which affected more than 70 people on the twentieth of that month. On 31 December, the Wuhan Municipal Health Committee informed the World Health Organization (WHO) that 27 people had been diagnosed with pneumonia of unknown cause, being 7 of them critically ill [1]. Coronavirus is a large family of viruses and a subset of coronaviruses that range from the common cold virus to the cause of more serious illnesses such as SARS and MERS coronavirus [2]. SARS-CoV-2 which is a single-stranded RNA and, like SARS and MERS, belongs to the beta-coronavirus family is a highly contagious disease that can be transmitted from one person to another through close contact [3,4]. COVID 19 patients most likely to require ICU support tend to be older , also ~25-40 % have at least one comorbidity such as hypertension, diabetes, heart disease, or chronic obstructive pulmonary disease and almost 75% are overweight or obese [5]. Most common reason for admission to ICU is; respiratory failure and around two-thirds of patients meeting criteria for a diagnosis of ARDS. The disease can be asymptomatic or present mild affection of the upper respiratory tract, while in the most severe cases is characterized by acute respiratory distress syndrome, heart failure, and septic shock [6]. Nutritional support using different methods has always played a crucial role in reducing inflammation and oxidative stress in the prevention, control and treatment of infectious and pulmonary diseases, and it seems that meeting the nutritional needs of patients with Covid-19 can help improve the disease process [7-13]. This mini-review study provides perspective on the nutritional implications and management of coronavirus disease 2019 (COVID-19), the resulting illness from SARS-CoV-2, by drawing on available clinical data for patients with COVID-19, as well as the literature from Acute Respiratory Distress Syndrome (ARDS). It considers the implications of a global pandemic on caseload, resourcing, supply chain shortages, and the logistics of managing highly infectious patients.
Dietary Nutrients Role on Immune System Function and COVID-19 Disease
The influence of nutrition in the immune system has been widely reported. In addition, recent studies have also highlighted the influence of both, an adequate nutritional status and the appropriate intake of specific nutrients in COVID-19. Nevertheless, due to the novelty of the disease, information regarding the effects of some nutrients is scarce, and in some cases, this information comes from ecological studies. Therefore, it seems plausible that part of the information included in this section may be updated in the upcoming months as the result of the research that is currently ongoing. Protein deficiency is linked to impaired immune system function, mainly due to its negative effects on both, the amount of functional immunoglobulins and Gut-Associated Lymphoid Tissue (GALT) [14-16]. Besides quantity, the quality of proteins is also an important factor with regard to the relationship of this macronutrient with immune system. In this line, it has been highlighted that including proteins of high biological value (those present in eggs, lean meat, fish, and dairy) containing all the essential amino acids may exert an anti-inflammatory effect. In addition, some amino acids, such as arginine and glutamine are well known for their ability to modulate the immune system [14].
Protein-Energy Malnutrition
When addressing COVID-19 disease, the study of nutritional status is very relevant since it plays an important role on the functionality of immune system, necessary to face the virus infection. Indeed, malnutrition is associated with immune dysfunction and thus it is likely to assume that this condition could make individuals more vulnerable to the viral infection [1]. On the other hand, nutritional status can be negatively affected by the SARS-CoV-2 itself, as well as by the applied treatments. Hospitalized patients with COVID-19 tend to present malnutrition at the time of hospitalization. Chronic diseases that are commonly present in patients with COVID-19 (mainly diabetes, chronic obstructive pulmonary disease, renal insufficiency, cardiovascular diseases or dementia), as well as other risk factors such as socio-economic status or frailty, have negative effects on the nutritional status of these patients. In addition, during hospital stay, the prolonged immobilization, mainly in long stays in Intensive Care Units (ICU), leads to muscle mass losses, making the recovery of these subjects harder. Furthermore, the need for assisted breathing during prolonged periods also contributes to the development of sarcopenia and malnutrition [1]. This deteriorated nutritional status seems to be involved in the virulence of the virus, and probably in the clinical outcome. In this regard, studies conducted in Italy have demonstrated the importance of maintaining/recovering an adequate nutritional status in the clinical outcomes of the patients [17]. Due to fluid administration and rapid wasting of lean tissues, weight and BMI changes do not accurately reflect malnutrition in COVID-19 patients. Thus, the loss of lean body mass is of more concern than that of the BMI. Indeed, loss of muscle and sarcopenia have to be detected, since the larger the muscle mass decrease is, the more severe the malnutrition will be [17]. Malnutrition is probably due to anorexia, nausea, vomiting, and diarrhea (which impair food intake and absorption), hypoalbuminemia, hypermetabolism, and excessive nitrogen loss [18]. These effects are clearly associated with the increase in pro-inflammatory cytokines observed in these patients. Moreover, anorexia can also be related to dysgeusia. Lechien et al. conducted a study devoted to analyzing the effect of COVID-19 infection on gustatory disorders [19]. For this purpose, 417 mild-to-moderate COVID-19 patients (164 males and 263 females) with a mean age of 37 years old were recruited from 12 European hospitals. More than 88% of the patients reported gustatory dysfunction, which was characterized by impairment of salty, sweet, bitter, and sour tastes. When data were adjusted for age, sex, presence of co-morbidities and BMI, NRS 2002, MNA-sf, and NRI methods demonstrated that patients from the nutritional risk group showed longer hospital stay, lower appetite, and worse severity of the disease, and greater weight loss than the patients in the normal group. By using NRS 2002 and NRI methods, patients with nutritional risk also showed higher hospital expenses than normal patients.
Nutritional Treatment
Although nowadays, the knowledge regarding the nutritional support during hospital stay of COVID-19 patients is still limited, nutritional therapy appears as first-line treatment and should be implemented into standard practice [20]. In spite of that, due to the priority assigned to urgent pathologies like respiratory issues, the nutritional status of patients has been relegated to a second place. In fact, almost half of the hospitalized polymorbid and 23-60% of patients in acute care are not correctly nourished [21]. Other facts that have also exacerbated this situation are that medical teams cannot invest enough time to grant an optimal nourishment due to work overload, staff shortages (healthcare personnel have suffered a high infection rate) or insufficient availability of personal protective equipment. Additionally, a restriction to family visits has been applied in most affected countries, removing a support in nourishment. Moreover, in most hospitals clinical teams and structures have been reorganized resulting in provisional limitations of dietetic support. The general recommendation for COVID-19 patients is to follow healthy diets to maintain a correct immune function [22]. Optimal intake of all nutrients, mainly those that play crucial roles in immune system, should be assured through a diverse and well-balanced diet. However, current data suggest that there is a prevalent micronutrient and omega-3 fatty acid deficiency in several population groups [23]. On the other hand, in the review reported by Calder et al. [24], based on several meta-analysis [25]. The authors state that in order to promote the optimum functioning of the immune system and to reduce the risk and consequences of infections, the intakes for some micronutrients may exceed the recommended dietary allowances since infections and other stressors can reduce micronutrient status. Thus, supplements may help restoring their normal blood levels [24,26,27]. With regard to supplementation, it is important to advise the general public to always consult a medical doctor prior consuming such products, as they can interact with other nutrients, drugs, and medical treatments; indeed, they can turn into toxic elements causing several disorders and aggravating certain conditions.
Nutritional Support in Critically Ill COVID-19 Patients
Some evidence suggests that the development of GI symptoms indicates greater disease severity. The presence of viral RNA components has been documented in the feces and respiratory specimens of such patients. Although the exact mechanism of COVID-19-induced GI symptoms largely remains elusive, when present early use of PN should be considered, transitioning to EN when GI symptoms subside [5]. Critically ill patients with COVID-19 disease have been reported to be older with multiple comorbidities. Such patients are often at-risk of refeeding syndrome. Thus, identifying pre-existing malnutrition or other risk factors for refeeding syndrome in critically ill patients is vital. If refeeding syndrome risk is present, we recommend starting at approximately 25% of caloric goal, in either EN or PN fed patients, combined with frequent monitoring of serum phosphate, magnesium and potassium levels as calories are slowly increased and first 72 hours of feeding is the period of highest risk. Feeding should be initiated with low dose EN, defined as hypocaloric or trophic, advancing to full dose EN slowly over the first week of critical illness to meet energy goal of 15- 20 kcal/kg Actual Body Weight (ABW)/day (which should be 70-80 % of caloric requirements) and protein goal of 1.2-2.0 gm/kg ABW/day [5,28]. If PN is necessary, conservative dextrose content and volume should be used in the early phase of critical illness, slowly advancing to meet the same energy goals Nutrition requirements should take into consideration the use of propofol in terms of lipid calories and total calories needed (Figure 1) [28,29].
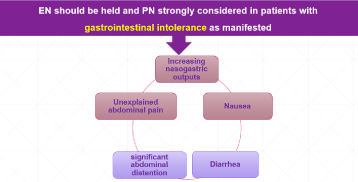
Figure 1: Conditions that require parenteral nutrition in critical ill Covid-19
patients.
Some COVID-19 patients experience severe respiratory symptoms and/or multi-organ failure, being very ill at hospital admission and thus needing specialized support [30]. Indeed, acute respiratory complications, requiring prolonged ICU stays, are a major cause of morbidity and mortality in COVID-19 patients. Most of these patients rapidly progress from cough to dyspnea, and then to respiratory failure requiring mechanical ventilation. Consequently, the timing of nutritional intervention appears to be critical [31]. Therefore, nutritionists should choose the most appropriate way to recover the subject’s health. As with any other critically ill patients, nutritional management is an integral component of good supportive care. The European Society for Clinical Nutrition and Metabolism (ESPEN) has recently published some guidelines for the nutritional management of patients with SARS-CoV-2 infection. In these guidelines specific recommendations are included for patients hospitalized in ICUs, among them early enteral nutrition (when possible), use of agents that promote gastric emptying, initiation of peripheral nutrition in situations in which enteral nutrition is not possible/tolerated and use of enteral nutrition after extubation when oral feeding is not tolerated. According to these ESPEN guidelines, enteral nutrition is preferred for patients in the ICU who receive mechanical ventilation [17]. However, the specific needs of patients with COVID-19 may require the adoption of prone ventilation or neuromuscular blockade, and consequently enteral nutrition implementation in daily practice could be difficult [32]. Further, a delay of enteral nutrition can be mandatory when life-threatening hypoxemia occurs [32]. On the other hand, the changes induced by the disease itself in the gastrointestinal tract of the patients, along with the elevated sedation required for these patients, makes difficult to provide adequate nutritional support. Bearing this in mind, Arkin et al. (2020) provided information regarding several of the considerations that have to be taken into account when nutrition is provided to critically ill patients of COVID-19 [33]. One such consideration is related to the gastrointestinal hypomotility that is commonly found in these patients, which in turn results in enteral feeding intolerance. Indeed, this situation seems not to be derived from the high-doses of sedatives and opioids that are needed to facilitate mechanical ventilation, since other patients under similar conditions do not present feeding intolerance. Thus, the authors suggest that the enteral feeding intolerance is related to the infection produced by the SARS-CoV-2. Moreover, despite several pharmacological agents devoted to promoting gastrointestinal motility are provided to COVID-19 patients at the time of ICU admission, their intestinal motility remains impaired. Additionally, even in the cases in which gastrointestinal motility is maintained/recovered (by studying gastric residuals and stool output), impaired nutrient absorption has been described. In the case of the patients in which gastric residuals are >500mL, the use of a post-pyloric feeding tube is recommended by the ESPEN guidelines. However, this approach involves technical challenges in the placement as well as increased exposure of the staff to viral infection and obvious difficulties when proning of the patient is required. Besides the gastrointestinal features of critically ill COVID-19 patients, severe lung injury is also common in these subjects. This condition makes necessary strategies devoted to avoiding aspirations. In this regard, the authors suggest holding tube feeding 1h prior proning as an effective approach to avoid aspirations. Indeed, the authors state that due to the challenges related to aspiration in prone patients, continuous tube feeding is maintained (instead of using bolus tube feeding). As far as diet is concerned, the ESPEN guidelines recommend hypocaloric nutrition in the first week of ICU stay. However, since the patients normally spend days/weeks sick at their homes before being admitted in a hospital, the risk of developing malnutrition increases. Moreover, the life-threatening features that are common on these patients at the time of ICU admission produces further delay in enteral nutrition, increasing even more the risk of malnutrition. Due to these facts, critically ill COVID-19 patients may have poor nutritional status, which in turn may increase the severity of the infection. In this regard, the authors point towards the necessity of a more aggressive early total parenteral nutritional support in these patients. Taking all that into account, and considering that COVID-19 patients need more energy than normal, the nutritional management of the critically ill patient in the longterm should avoid underfeeding or overfeeding. It is recommended to supply around 20 or 30 kcal/kg body weight/day for polymorbid patients aged >65 years or for severely underweight polymorbid patients respectively [34,35]. These values should be adjusted with regard to nutritional status, disease status, and tolerance [36]. It is important to take into account that in severely underweight patients, the target of 30kcal/kg body weight/day should be slowly achieved (in the case of artificial nutrition, target speed must be reached in 3-4 days) due to the high risk of refeeding syndrome of this population [20]. Protein needs are higher in the critically ill patient due to the protein catabolism driven by inflammatory mediators [35]. It is estimated as 1g protein/kg body weight/day in older people (133), or 1.3g protein/kg body weight/day with increased supply of branched chain amino acids (up to 50% in polymorbid medical inpatients), in order to prevent muscle loss and to strength respiratory muscles [35]. Other authors increased these recommendations to 1.5g protein/kg body weight/day [35]. These amounts should be individually adjusted with regard to nutritional status, disease status, and tolerance [34]. The needs of fat and carbohydrate have to be adapted to the energy requirements, considering an energy ratio from fat and carbohydrates between 30:70 % for individuals with no respiratory deficiency and to 50:50 % for ventilated patients [20]. Fat requirement in the critically ill patient is around 1.5g/kg body weight/day, giving priority to the usage of medium and long chain fatty acids. As far as carbohydrates requirement is concerned, a supply of 2g/kg body weight/day, not exceeding 150g/day, must be considered. This is due to their high CO2 production rate that should be limited in case of respiratory failure [20]. With regard to micronutrients in ICU patients, mineral and vitamin supply with routine supplements must be considered depending on the nutritional therapy used. Administration of doses higher than recommendations of vitamin D can be used because of their positive effects [20]. Certainly, it has been reported that high doses of Vitamin D in infected patients may improve immunologic recovery during antiretroviral treatment, reduce levels of inflammation and immune activation, and increase immunity against pathogens [37]. In turn, vitamin C supplementation significantly reduces mortality in critically ill patients [37]. In the case of enteral nutrition, attention must be paid to the needs of specific nutrients to be included in the formula. Thus, enteral diets containing EPA, gamma-linolenic acid, and antioxidant agents may offer a clinical benefit in oxygenation and days of ventilation in patients with acute respiratory distress syndrome [17]. Further, specific lipid emulsions could offer additional benefits over corticosteroid and anti-IL-6 drugs in the modulation of the inflammatory response. However, COVID-19 patients’ response to specific enteral diets remains to be determined [31].
Conclusion
Patients who are admitted to the ICU with COVID-19 are at high nutritional risk, due to their presenting condition, the intensive care management strategies required to treat the disease and the likely course of the treatment. Alteration in metabolism and gastrointestinal function, coupled with nutritional deficits during critical illness and following, are all likely to contribute to a decline in nutrition status and poorer functional ability. Also optimized nutrition care of the critical ill COVID-19 patients is important to maintain GI tract function, sustain immune defenses, and avoid severe loss of muscle mass and function. As for any other ICU patients, the latter is crucial to promote short- and long-term recovery. Dedicated studies about the nutrition in the COVID-19 patients are now awaited to enrich our knowledge about the metabolism of this new disease and adapt the nutrition support strategy.
References
- Fernández-Quintela A, Milton-Laskibar I, Trepiana J, Gómez-Zorita S, Kajarabille N, Léniz A, et al. Key aspects in nutritional management of COVID-19 patients. Journal of clinical medicine. 2020; 9: 2589.
- Banerjee A, Kulcsar K, Misra V, Frieman M, Mossman K. Bats and coronaviruses. Viruses. 2019; 11: 41.
- Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, et al. A novel coronavirus from patients with pneumonia in China, 2019. New England journal of medicine. 2020; 382: 727-733.
- Chen Y, Liu Q, Guo D. Emerging coronaviruses: genome structure, replication, and pathogenesis. Journal of medical virology. 2020; 92: 418-423.
- Thibault R, Seguin P, Tamion F, Pichard C, Singer P. Nutrition of the COVID-19 patient in the Intensive Care Unit (ICU): a practical guidance. Critical Care. 2020; 24: 447.
- Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. The lancet. 2020; 395: 1054-1062.
- Pahlavani N, Sadeghi A, Rasad H, Azizi Soleiman F. Relation of inflammation and oxidative stress with blood glucose, lipids and BMI, fat mass and body weight in people with type 2 diabetes. Journal of Zabol Diabetic Nursing. 2014; 2: 42-51.
- Pahlavani N, Roudi F, Zakerian M, Ferns GA, Navashenaq JG, Mashkouri A, et al. Possible molecular mechanisms of glucose-lowering activities of Momordica charantia (karela) in diabetes. Journal of cellular biochemistry. 2019; 120: 10921-10929.
- Collins PF, Stratton RJ, Elia M. Nutritional support in chronic obstructive pulmonary disease: a systematic review and meta-analysis. The American journal of clinical nutrition. 2012; 95: 1385-1395.
- Harvey SE, Parrott F, Harrison DA, Bear DE, Segaran E, Beale R, et al. Trial of the route of early nutritional support in critically ill adults. New England Journal of Medicine. 2014; 371: 1673-1684.
- Stachowska E, Folwarski M, Jamiol-Milc D, Maciejewska D, SkoniecznaZydecka K. Nutritional support in coronavirus 2019 disease. Medicina. 2020; 56: 289.
- Pahlavani N, Sedaghat A, Moghaddam AB, Kiapey SSM, Navashenaq JG, Jarahi L, et al. Effects of propolis and melatonin on oxidative stress, inflammation, and clinical status in patients with primary sepsis: Study protocol and review on previous studies. Clinical nutrition ESPEN. 2019; 33: 125-131.
- Ebrahimi F, Aryaeian N, Pahlavani N, Abbasi D, Hosseini AF, Fallah S, et al. The effect of saffron (Crocus sativus L.) supplementation on blood pressure, and renal and liver function in patients with type 2 diabetes mellitus: A doubleblinded, randomized clinical trial. Avicenna journal of phytomedicine. 2019; 9: 322-333.
- Iddir M, Brito A, Dingeo G, Fernandez Del Campo SS, Samouda H, La Frano MR, et al. Strengthening the immune system and reducing inflammation and oxidative stress through diet and nutrition: considerations during the COVID-19 crisis. Nutrients. 2020; 12: 1562.
- Rasad H, Dashtabi A, Khansari M, Chaboksavar F, Pahlavani N, Maghsoudi Z, et al. The effect of honey consumption compared with sucrose on blood pressure and fasting blood glucose in healthy young subjects. Global Journal of Medicine Research and Studies. 2014; 1: 117-121.
- Dunn CG, Kenney E, Fleischhacker SE, Bleich SN. Feeding low-income children during the Covid-19 pandemic. New England Journal of Medicine. 2020; 382: e40.
- Singer P. Preserving the quality of life: nutrition in the ICU. Critical Care. 2019; 23: 139.
- Zhou S, Ye B, Fu P, Li S, Yuan P, Yang L, et al. Double Burden of Malnutrition: Examining the Growth Profile and Coexistence of Undernutrition, Overweight, and Obesity among School-Aged Children and Adolescents in Urban and Rural Counties in Henan Province, China. Journal of obesity. 2020; 2020.
- Lechien JR, Chiesa-Estomba CM, De Siati DR, Horoi M, Le Bon SD, Rodriguez A, et al. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): a multicenter European study. European Archives of Oto-Rhino-Laryngology. 2020; 277: 2251-2261.
- Barazzoni R, Bischoff SC, Breda J, Wickramasinghe K, Krznaric Z, Nitzan D, et al. ESPEN expert statements and practical guidance for nutritional management of individuals with SARS-CoV-2 infection. Elsevier. 2020; 39: P1631-P1638.
- Jie B, Jiang Z-M, Nolan MT, Efron DT, Zhu S-N, Yu K, et al. Impact of nutritional support on clinical outcome in patients at nutritional risk: a multicenter, prospective cohort study in Baltimore and Beijing teaching hospitals. Nutrition (Burbank, Los Angeles County, Calif). 2010; 26: 1088-1093.
- Zabetakis I, Lordan R, Norton C, Tsoupras A. COVID-19: the inflammation link and the role of nutrition in potential mitigation. Nutrients. 2020; 12: 1466.
- Stark KD, Van Elswyk ME, Higgins MR, Weatherford CA, Salem N. Global survey of the omega-3 fatty acids, docosahexaenoic acid and eicosapentaenoic acid in the blood stream of healthy adults. Progress in lipid research. 2016; 63: 132-152.
- Calder PC, Carr AC, Gombart AF, Eggersdorfer M. Optimal nutritional status for a well-functioning immune system is an important factor to protect against viral infections. Nutrients. 2020; 12: 1181.
- Autier P, Mullie P, Macacu A, Dragomir M, Boniol M, Coppens K, et al. Effect of vitamin D supplementation on non-skeletal disorders: a systematic review of meta-analyses and randomized trials. The lancet Diabetes & endocrinology. 2017; 5: 986-1004.
- Carr AC, Maggini S. Vitamin C and immune function. Nutrients. 2017; 9: 1211.
- Hunt C, Chakravorty N, Annan G, Habibzadeh N, Schorah C. The clinical effects of vitamin C supplementation in elderly hospitalised patients with acute respiratory infections. International journal for vitamin and nutrition research. 1994; 64: 212-219.
- Zhao X, Li Y, Ge Y, Shi Y, Lv P, Zhang J, et al. Evaluation of nutrition risk and its association with mortality risk in severely and critically ill COVID-19 patients. Journal of Parenteral and Enteral Nutrition. 2021; 45: 32-42.
- Zhang P, He Z, Yu G, Peng D, Feng Y, Ling J, et al. The modified NUTRIC score can be used for nutritional risk assessment as well as prognosis prediction in critically ill COVID-19 patients. Clinical Nutrition. 2021; 40: P534-P541.
- Li X, Du B, Wang Y, Kang H, Wang F, Sun B, et al. The keypoints in treatment of the critical coronavirus disease 2019 patient. Zhonghua jie he he hu xi za zhi. 2020; 43: 277-281.
- Laviano A, Koverech A, Zanetti M. Nutrition support in the time of SARSCoV- 2 (COVID-19). Nutrition (Burbank, Los Angeles County, Calif). 2020; 74: 110834.
- Anderson L. Providing nutritional support for the patient with COVID-19. British Journal of Nursing. 2020; 29: 458-459.
- Arkin N, Krishnan K, Chang MG, Bittner EA. Nutrition in critically ill patients with COVID-19: challenges and special considerations. Clinical nutrition (Edinburgh, Scotland). 2020; 39: 2327-2328.
- Gomes F, Baumgartner A, Bounoure L, Bally M, Deutz NE, Greenwald JL, et al. Association of nutritional support with clinical outcomes among medical inpatients who are malnourished or at nutritional risk: an updated systematic review and meta-analysis. JAMA network open. 2019; 2: e1915138.
- Romano L, Bilotta F, Dauri M, Macheda S, Pujia A, De Santis G, et al. Short Report-Medical nutrition therapy for critically ill patients with COVID-19. European review for medical and pharmacological sciences. 2020; 24: 4035- 4039.
- Volkert D, Beck AM, Cederholm T, Cruz-Jentoft A, Goisser S, Hooper L, et al. ESPEN guideline on clinical nutrition and hydration in geriatrics. Clinical nutrition. 2019; 38: 10-47.
- Caccialanza R, Laviano A, Lobascio F, Montagna E, Bruno R, Ludovisi S, et al. Early nutritional supplementation in non-critically ill patients hospitalized for the 2019 novel coronavirus disease (COVID-19): Rationale and feasibility of a shared pragmatic protocol. Nutrition (Burbank, Los Angeles County, Calif). 2020; 74: 110835.