Case Report
J Dent App. 2014;1(3): 40-42.
Adenomatoid Odontogenic Tumor of Mandible - 'Master of Disguise'
Manoj Kumar Jain* and Sheetal Oswal K
Department of Oral and Maxillofacial Surgery, Sri Hasanamba Dental College and Hospital, Vidyanagar, Hassan (Karnataka), India
*Corresponding author: Dr. Manoj Kumar Jain, Department of Oral and Maxillofacial Surgery, Sri Hasanamba Dental College and Hospital, Vidyanagar, Hassan (Karnataka), India
Received: July 04, 2014; Accepted: Aug 06, 2014; Published: Aug 08, 2014
Abstract
Adenomatoid odontogenic tumor (AOT) is a relatively uncommon distinct odontogenic neoplasm. It is rightfully called as 'Master of Disguise' and 'perfect imitator of dentigerous cyst'. It has three well recognized clinicopathological variants and has been described as "two thirds Tumor" because it occurs in maxilla in about two third cases, about two third cases arise in young females, two third cases are associated with unerupted tooth and two third affected teeth are canines. An unusual case of follicular adenomatoid odontogenic tumor of the mandible associated with two impacted teeth is presented here.
Keywords: Adenomatoid odontogenic tumor (AOT); Mandible; Adenoameloblastoma; Adenomatoid odontogenic cyst
Adenomatoid odontogenic tumor (AOT) is a relatively uncommon distinct odontogenic neoplasm that was first described by Steensland in 1905 [1]. However, a variety of terms have been used to describe this tumor. Unal et al. [2] produced a list containing all nomenclatures for AOT reported in the literatures. Many different names like adenoameloblastoma, ameloblastic adenomatoid tumor, adamantinoma, epithelioma adamantinum or teratomatous odontoma have been used before to define the lesion currently called AOT. Recently, textbook of oral and maxillofacial pathology by Robert Marx and Diane Stern [3] updated the term AOT and other related terms to Adenomatoid odontogenic cyst. However, the above term (AOT), has been adopted by the WHO classification of odontogenic tumor in 2005 [4].
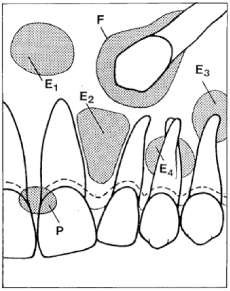
Three clinicopathological variants of AOT are well recognized: follicular, extra-follicular, and peripheral (Figure 1). Follicular and extra follicular variants are both intrabony or central tumors and account for 97% of all AOTs of which 73% are of the follicular type. The extra follicular variant is not associated with an unerupted tooth like the follicular variant, and the well-defined, unilocular radioluscency is found between, above, or superimposed on the roots of erupted teeth. It is characteristic that the rare sub variant mimicking a periapical lesion is, in fact, located palatal (or lingual) to the "involved" tooth [5].
Figure 1: Radiographic appearance of AOT variants. F, Follicular type; the tumor is located around the crown and often, as shown here, including part of the root of an unerupted tooth (envelopmental). E1-E4, extrafollicular types: E1, without relation to tooth structures either erupted or unerupted; E2 , interradicular; adjacent roots diverge apically as a result of tumor expansion (mimicking a "globulo-maxillary" cyst); E3, superimposed on root at apex level (mimicking a radicular cyst); E4, superimposed at midroot level. P, peripheral or epulis type (with slight erosion or "saucerization" of bone crest).
We report a case of follicular Adenomatoid odontogenic tumor of the mandible associated with two impacted teeth.
Case Report
A 17 year old girl presented with asymptomatic swelling in left chin region of 6 months' duration. Swelling was gradual in onset which progressively increased to current size of about 5x4 centimeters. Extra oral swelling was located on lower one third of face extending slightly to left side, which measured approximately 5x4 cm. Swelling was ill defined with no surface changes over the skin. Intraoral lower labial vestibular obliteration was noticed in relation to 43, 42,41,31,32, retained D74 with left mandibular canine and 1st premolar missing. On palpation swelling was bony hard, non tender and immobile. Aspiration biopsy carried out revealed nothing from the lesion. Provisional diagnosis of dentigerous cyst with differential diagnosis of AOT, Unicystic ameloblastoma, Odontogenic Keratocyst OKC (Keratocystic Odontogenic Tumor KOT) was made.
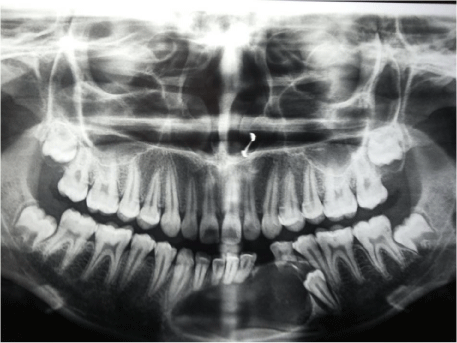
Radiographically, Orthopantomograph (OPG) showed a well defined unilocular ovoid radiolucent lesion of about 5x4cm with sclerotic borders extending anteroposteriorly from distal aspect of 43 to mesial aspect of 35 and supero- inferiorly from 1 cm inferior to alveolar crest to inferior border of mandible. It also revealed horizontal impacted 33 at the inferior border of mandible and vertically impacted 34 at the periapical region of retained deciduous D74 and resorbed apical one third of roots of 42,41,31,32 (Figure 2).
Figure 2: OPG showing a well defined unilocular ovoid radiolucent lesion of about 5x4cm with sclerotic borders. It also revealed horizontal impacted 33 at the inferior border of mandible and verticaly impacted 34 at the periapical region of retained decidous D and resorbed apical one third of roots of 42,41,31,32.
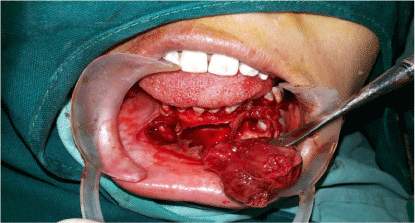
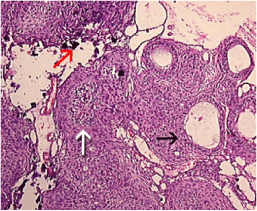
Complete enucleation of the lesion was done under general anesthesia with removal of impacted 33 and 34 (Figure 3). 6 months postoperative follow up did not show any signs of recurrence or complications. Histopathological examination (H&E) showed polyhedral darkly staining cells resembling odontogenic epithelial cells arranged in sheets and ductal pattern. Few cells were arranged in rosette pattern with a central eosinophilic coagulum. Lot of calcified areas was seen among sheets of cells and lesion tissue appears well encapsulated with bundles of mature collagen fibers, all suggestive of AOT (Figure 4).
Figure 3: Complete enucleation of the lesion was done under general anesthesia.
Figure 4: Photomicrograph showing solid nodules of cuboidal epithelium arranged in sheets, rosettes (white arrow), and duct like areas (black arrow), together with focal areas of basophilic calcification (red arrow) (haematoxylin and eosin, original magnificationx100).
Discussion
AOT is a benign, non invasive odontogenic lesion showing slow growth. It is rightfully called as 'Master of Disguise' and 'Perfect imitator of dentigerous cyst' as noted in the present case [1-7]. Sixty-nine percent of AOTs are diagnosed in the second decade of life, and more than half of the cases (53%) occur during the teenage years (mean - 13 years, range 3 to 28 years of age) [3-5]. The female to male ratio for all age groups and AOT variants together is very close to 2:1 [3-5]. AOT has been described as " two thirds Tumor" because it occurs in maxilla in about two third cases, about two third cases arise in young females, two third cases are associated withunerupted tooth and two third affected teeth are canine [4]. Larsson et al. [6] reported a case where multiple multifocal AOT were identified at different times and at different sites. Present case was seen in anterior mandible associated with 2 impacted teeth (Table 1).
Typical findings of AOT
Unusual findings in present case
Common site is anterior� maxilla
was seen in anterior mandible
Size usually does not exceed� 1-3cm
Present case size was of about 5x3cm
Root resorption extremely rare:
Root resorption of the� mandibular anteriors noted
radiopaque specks associated with
impacted teeth
no radiopaque specks were seen and was associated with 2 impacted teeth
Cortical plate penetration rare
Cortical perforation seen
Table 1: Unusual findings seen in our case related to typical features of an Adenomatoid odontogenic tumor.
According to Philipsen et al. the fact that all AOT variants show identical histologic characteristics points to a common origin. The pathogenesis of this odontogenic tumor appears to involve persistence of remnants of the dental lamina, especially after odontogenesis of the successional and accessional laminae. These remnants give rise to epithelial rests that proliferate in response to an unknown stimulus [7].
The radiographic findings of AOT frequently resemble other odontogenic lesions such as dentigerous cysts, calcifying odontogenic cysts, calcifying odontogenic tumors,globule-maxillary cysts, ameloblastomas, odontogenickeratocysts and periapical disease [8-9]. Comparing diagnostic accuracy betweenintraoral periapical and panoramic radiographs, Dare et al. [10] found that intraoral periapical radiographs allow perception of the radiopacities in AOT as discrete foci having a flocculent pattern within radioluscency even with minimal calcified deposits while panoramic often do not. Those calcified deposits are seen in approximately 78% of AOT [8-10].
Immunhistological features
During the last few years several studies have been published dealing with the immunhistological properties of AOT. Immunohistochemically, the classical AOT phenotype is characterized by a cytokeratin (CK) profile similar to follicular cyst and/or oral or gingival epithelium based on positive staining with CK5, CK17 and CK19 [11-13]. On the other hand the classical AOT is negative for CK4, 10, 13 and 18. Recently, Crivelini et al. [12] detected the expression of cytokeratin 14 in AOT and concluded that this probably indicate its origin in the reduced dental epithelium which is also positive for staining with cytokeratin 14 antibodies. Positive reactions for amelogenin in limited areas in AOT are also reported as well as in amel-oblasts and in the immature enamel matrix. Interestingly, Takahashi et al. [13] observed a positive staining for iron-binding proteins (transferring, ferritin) and proteinase inhibitor (alpha-one-antitrypsin) in various cells of AOT indicating their role to the pathogenesis of AOT.
Conservative surgical enucleation is the treatment modality of choice. For periodontal intrabony defects caused by AOT guided tissue regeneration with membrane technique is suggested after complete removal of the tumor [14]. Recurrence of AOT is exceptionally rare. Only three cases in Japanese patients are reported in which the recurrence of this tumor occurred [15]. Therefore, the prognosis is excellent. No recurrence was seen in the present case.
To conclude, AOT is a relatively uncommon distinct odontogenic neoplasm and is rightfully called as 'Master of Disguise' and 'Perfect imitator of dentigerous cyst'. It should be a part of differential diagnosis whenever we encounter a lesion in young patients with unerupted tooth (Two Third's Tumor).
References
- Steensland HS. Epithelioma adamantinum. J Exper Med. 1905; 6: 377-389.
- Unal T, Cetingul E, Gunbay T. Peripheral adenomatoid odon-togenic tumor: Birth of a term. J Clin Pediatr Dent. 1995; 19: 139-142.
- Philipsen HP, Reichart PA. Adenomatoid odontogenic tumour: facts and figures. Oral Oncol. 1998; 35: 125-131.
- Robert E. Marx, Diane Stern. Oral and Maxillofacial Pathology - A rationale for diagnosis and treatment. Quintessence publishing co. 2003; 609-611&877.
- Adenomatoid odontogenic tumor mimicking a periapical (radicular) cyst: A case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002; 94: 246-248.
- Larsson A, Swartz K, Heikinheimo K. A case of multiple AOT-like jawbone lesions in a young patient- a new odontogenic entity? J Oral Pathol Med. 2003; 32: 55-62.
- Philipsen HE, Samman N, Ormiston IW, Reichart PA. Variants of the adenomatoid odontogenic tumor with a note on tumor origin. J Oral Pathol Med. 1992; 21: 348-352.
- Philipsen HP, Reichart PA, Zhang KH, Nikai H, Yu QX. Adenomatoid odontogenic tumor: biologic profile based on 499 cases. J Oral Pathol Med. 1991; 20: 149-158.
- Konouchi H, Asaumi J, Yanagi Y, Hisatomi M, Kishi K. Adenomatoidodontogenic tumor: correlation of MRI with histopathological findings. Eur J Rad. 2002; 44: 19-23.
- Dare A, Yamaguchi A, Yoshiki S, Okano T. Limitation of panoramic radiography in diagnosing adenomatoid odontogenictumors. Oral Surg Oral Med Oral Pathol. 1994; 77: 662-668.
- Philipsen HP, Reichart PA. The adenomatoid odontogenic tumour: ultrastructure of tumour cells and non-calcified amorphous masses. J Oral Pathol Med. 1996; 25: 491-496.
- Crivelini MM, de Araujo VC, de Sousa SO, de Araujo NS. Cytokeratins in epithelia of odontogenic neoplasms. Oral Dis. 2003; 9: 1-6.
- Takahashi H, Fujita S, Shibata Y, Yamaguchi A. Adenomatoid odontogenic tumour: immunohistochemical demonstration of transferring, ferritin and alpha-one-antitrypsin. J Oral Pathol Med. 2001; 30: 237-244.
- Blumenthal NM, Mostofi R. Repair of an intrabony defect from an adenomatoid odontogenic tumor. J Periodontol. 2000; 71: 1637-1640.
- Toida M, Hyodo I, Okuda T, Tatematsu N. Adenomatoid odontogenic tumor: report of two cases and survey of 126 cases in Japan. J Oral Maxillofac Surg. 1990; 48: 404-408.