
Case Report
J Dent App. 2015;2(4): 202-204.
Identification of Mucosal Malignant Melanoma on The Root; A Rare Case
Nihat Demirtas1*, Erol Senturk2, Hakki Oguz Kazancioglu1 and Emre Aytugar3
1Department of Oral and Maxillofacial Surgery, Faculty of Dentistry, Bezmialem Vakif University, Istanbul, Turkey
2Department of Otorhinolargeryngology Head and Neck Surgery, Faculty of Medicine, Bezmialem Vakif University, Istanbul, Turkey
3Department of Oral and Maxillofacial Radiology, Faculty of Dentistry, Bezmialem Vakif University, Istanbul, Turkey
*Corresponding author: Nihat Demirtas, Bezmialem Vakif University, Faculty of Dentistry, Department of Oral and Maxillofacial Surgery 34093-Istanbul,Turkey
Received: February 09, 2015; Accepted: March 11, 2015; Published: March 13, 2015;
Abstract
Mucosal malignant melanoma of the head and neck regionis a very rare entity.It can occur in oral soft tissues such as gingival regions, buccal mucosa, tongue and floor of the mouth. In additionparanasal sinuses and sinonasal tract may be affected. In the literature, great mortality and morbidity rates were reported because of itsaggressive metastatic character.Thus, it is important to note that early diagnosisand treatment play a key rolein the management of these lesions.Here, we presenta case of mucosal malignant melanomathatdetectedin the sinonasal cavity following tooth extraction. The lesion was treated by surgical excision and radiotherapy. The patient is well without any symptoms or signs of recurrence one year after treatment. We aimed to report thisrare case of malignant melanomawith emphasis on its unusualpresentation.
Keywords: Malignant melanoma; Tooth extraction; Sinonasal cavity; Diagnosis
Introduction
Malignant melanomawhich should be present with mucosal involvement is a serious cancer. It has great morbidity and mortality rates [1,7]. Primary mucosal malignant melanomas can occur in sinonasal and oral cavites and account for 1.3%–1.4% of all melanomas[2]. It was first reported in the English literature by Lincoln et al. [3].
The etiology of the mucosal malignant melanoma is not clear. However, many factors have been suggested as risk factors including tobacco and alcohol habits, nutritional deficiencies and infections [4]. On the other hand, C-kit gene mutations are reported in 21% of mucosal melanoma [5].
The frequency of malignant melanomas in the sinonasal cavity is approximately 1 in 500,000 to 1 in 1,000,000 people in the general population[6]. Diagnosis may be missed or delayed because of asymptomatic presentation in the early stages[7,8].Additionally, primary mucosal melanomas in the maxillary sinus and nasal cavityhave an aggressive character and poor prognosis due to complex anatomic location and rich vascularisation [9].
This paper aims to emphasize the importance ofearly identification and intervention in mucosal malignant melanoma of the sinonasal cavity.
Case Report
A 32-year-old woman was admittedto our faculty. Her chief complaint was chewing difficulty. The patient was normally healthy and taking no medications. Clinical examination revealed advanced stage periodontal disease, toothmobility and missing teeth. During a panoramic examination, progressive dental caries and bone resorption were identified in the interdental regions (Figure 1). After prosthetic treatment planning, it was determined thatmaxillary right lateral, second premolar and second molar teethhadto be extracteddue to intrabony defects and caries. The informed consent was given by the patient, and a posterior superior alveolar block and infiltrating anaesthesia of the hard and soft tissues were done to extract maxillary right second molar. After extraction, a black lesion was observed on the apical region of the root (Figure 2). Moreover, oro-antral communication occurred. We suspected a mucosal disease of the maxillary sinus and requested ahistopathological examination. Biopsy specimens were obtained from the maxillary sinus mucosa. According to the results of the histopathological examination, the lesion was diagnosed as mucosal malignant melanoma (Figure 3). The patient referred to otolaryngology examination, and large melanocytic lesions within the right nasal cavity and paranasal sinus weredetected. At this stage Cone Beam Computed Tomography (CBCT) scans were obtained to evaluate the growth pattern of the lesion. Focal perforations in buccal cortex and lateral nasal wall were observed in 3-dimensional reconstructed images (Figure 4a). Axial and cross section images also revealedthe involvement of maxillary sinus and nasal cavity (Figure 4b and 4c).
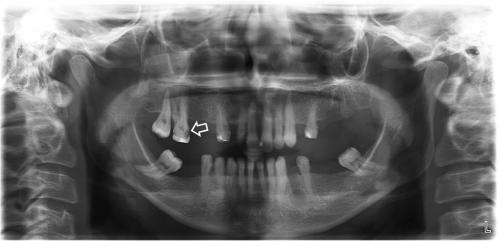
Figure 1: Panoramic view of the patient. White arrow shows the extracted
teeth number 17.
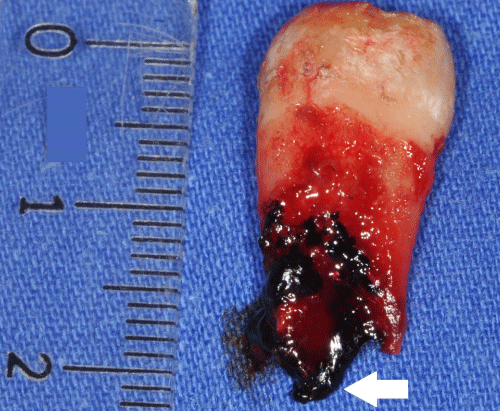
Figure 2: Black lesion on the apical region of the root in the extracted
maxillary second molar (white arrow).
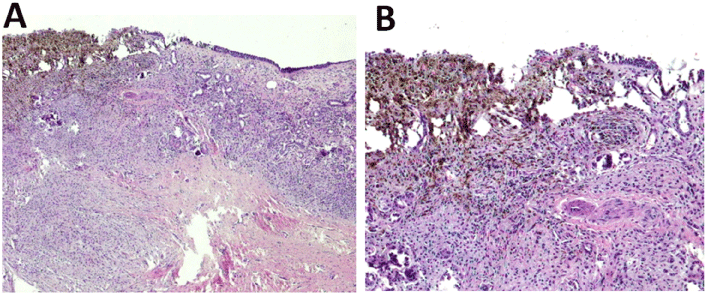
Figure 3: Histopathology of the lesion. (a) Malignant melanoma adjacent to
the normal sinus mucosa (H&E X 40) (b) In higher magnification, pigmented
area of malignant melanoma adjacent to the normal sinus mucosa (H&E X
100).

Figure 1: (a) 3-D reconstructed image showing perforation of buccal cortex
and nasal cavity, (b) Axial CBCT scan shows the position of the lesion in
proximity to nasal cavity and maxillary sinus, (c) Cross sectional CBCT image
showing the lesion and it is relation with right maxillary second and third
molars (red arrows).
Surgical excision, including right total maxillectomy and radical neck dissection, were performed for treatment. Next,radiotherapy was given. A year after initial diagnosis the patient was free of any recurrence ormetastasis.
Discussion
In the cases of mucosal malignant melanoma, the diagnostic tools consist of physical examination, CT scan, MRI, and biopsy [10,11]. However, the diagnosis can be difficult due to most cases beingasymptomatic. In the present case, the lesion originated in the right maxillary sinus and was detected accidentally after tooth extraction. Furthermore, part of the lesion on the maxillary sinus mucosa was slightly attached to the roots of the second molar. While the extraction was being performed, the lesion appeared with sinus mucosa. We could not find any reports in the literature about sinonasal and/or mucosal malignant melanoma, which is detected by extracted teeth.
Manolidis et al. [12] reported 5-year survival rate as 31% for patients with nasal mucosal melanoma. However, they reported that sinus melanoma patients had a 0% 5-year survival rate.Koivunen et al. [13] suggested that 3 and 5-year overall survival rates in 50 cases of sinonasal mucosal melanomaare 44% and 27%, respectively. Lazzeri et al. [14] reported a case of malignant melanoma of the nasal septum which had the frontal sinus floor involvement. Hence they suggested that early diagnosis is critical because of extremely aggressive character of these lesions.
Radical surgical excision and radiation therapy with adequate follow-up are recommended for the treatment of mucosal malign melanoma [6,10]. Besides surgical treatment, it has been reported that chemotherapy and high-dose proton beam therapy have a substantial therapeutic role in the patients [15]. On the other hand, high dose radiation therapy is impossible because of adjacent organs such as eyes and brain [11]. The main goal of the treatment is tocomplete resection of the mucosal melanoma and providing the absence of distant metastases. Sun et al. evaluated the outcome of the sixtyeight patients with sinonasal mucosal melanomaretrospectively. He reported that patients who underwent surgery had better survival rate than the patients treated without surgery. However, distant metastasis is directly related to a poor prognosis in all ofthe patients [16].
Conclusion
In conclusion,early diagnosis and treatment is the most important strategy for the control of oral malignancies. The identification of pigmented lesions ispossible with inspection of oral mucosa. However,it may be difficult in the cases of malignant mucosal melanoma of the paranasal sinuses owing to complex anatomic location. We believe that similar cases of mucosal melanomas can invade periodontal tissues. Thus, clinicians should perform biopsy and refer their patients to medical specialists, if they suspect atypical conditions.
References
- Hicks MJ, Flaitz CM. Oral mucosal melanoma: Epidemiology and pathobiology. Oral Oncol 2000; 36:152-169.
- McLaughlin C C, Wu X C, Jemal A, Martin H J, Roche L M, et al. Incidence of noncutaneous melanomas in the U.S. Cancer 2005;103:1000–1007.
- Lincoln RP. A case of melano-sarcoma of the nose cured by galvanocauterization. N Y Med J 1885;42:406–407.
- Rapidis AD, Apostolidis C, Vilos G, Valsamis S. Primary malignant melanoma of the oral mucosa. J Oral Maxillofac Surg 2003; 61:1132–1139.
- Woodman SE, Davies MA. Targeting KIT in melanoma: a paradigm of molecular medicine and targeted therapeutics. Biochem Pharmacol 2010; 80:568–574.
- Patel SG, Prasad ML, Escrig M, Singh B, Shaha AR, et al. Primary mucosal malignant melanoma of the head and neck. Head Neck 2002; 24:247–257.
- Matsuoka K. Oral malignant melanoma detected after resection of amelanotic pulmonary metastasis. Int J Surg Case Rep 2013; 4:1169–1172.
- Gasparyan A, Amiri F, Safdieh J, Reid V, Cirincione E, et al. Malignant mucosal melanoma of the paranasal sinuses: Two case presentations. World J ClinOncol 2011; 2: 344–347.
- Sun C, Hu Z, Wang H, Xi Y, Li G, et al. Treatment and prognosis of sinonasal mucosal melanoma. Lin Chung Er Bi Yan HouTou Jing WaiKeZaZhi 2013; 27:1135-1138.
- Cheng YF, Lai CC, Ho CY, Shu CH, Lin CZ. Toward a better understanding of sinonasal mucosal melanoma: clinical review of 23 cases. J Chin Med Assoc 2007; 70:24-29.
- Ziólkowska M, Bien S, Klimas A, Zylka S. The epidemiology and clinical characteristics of malignant melanoma localized in nasal cavity and paranasal sinuses--analysis of 6 cases. Otolaryngol Pol 2008; 62:500-503.
- Manolidis S, Donald PJ. Malignant mucosal melanoma of the head and neck: Review of the literature and report of 14 patients. Cancer. 1997;80:1373–1386.
- Koivunen P, Bäck L, Pukkila M, Laranne J, Kinnunen I, et al. Accuracy of the current TNM classification in predicting survival in patients with sinonasal mucosal melanoma. Laryngoscope 2012; 122:1734-1738.
- Lazzeri D, Agostini T, Giacomina A, Giannotti G, Colizzi L, et al. Malignant melanoma of the nasal septum. J CraniofacSurg 2010; 21:1957-1960.
- Fuji H, Yoshikawa S, Kasami M, Murayama S, Onitsuka T, et al. High-dose proton beam therapy for sinonasal mucosal malignant melanoma. RadiatOncol 2014; 23:162.
- Sun CZ, Li QL, Hu ZD, Jiang YE, Song M, et al. Treatment and prognosis in sinonasal mucosal melanoma: A retrospective analysis of 65 patients from a single cancer center.Head Neck 2014; 36:675-681.