
Special Article - Pediatric Dentistry
J Dent App. 2016; 3(1): 312-314.
A Simplified Method for Eruption of the Ectopic Molars: A Case Report
Haznedaroglu E and Mentes A*
Department of Pediatric Dentistry, School of Dentistry, Marmara University, Istanbul, Turkey
*Corresponding author: Ali Mentes, Department of Pediatric Dentistry, School of Dentistry, Marmara University, Basibuyuk Campus, 34854, Basibuyuk- Maltepe, Istanbul, Turkey
Received: August 05, 2016; Accepted: September 20, 2016; Published: September 22, 2016
Abstract
Ectopic eruption of the first permanent molars is a common problem of the developing dentition. Early diagnosis and treatment can prevent from a more complicated malocclusion. Correction of ectopically erupting permanent molars is critical for the development of a stable occlusion and is an important component of interceptive orthodontic treatment. The pediatric dentist can choose from a variety of effective treatment modalities to successfully manage ectopically erupting permanent molars. This case report described a treatment for an 8-year-old girl with bilateral ectopic molars. The treatment included strip of the second primary molars and using a removable appliance, which was a compliance-independent and alternative to the methods previously used.
Keywords: Ectopic eruption; Permanent maxillary first molars; Modified Hawley appliance
Case Presentation
The cause of ectopic eruptions of the permanent maxillary first molars is not well known and is considered to have a multifactorial etiology. Among the factors that could cause this abnormality are discrepancies in bone size and tooth size and/or a difference in the chronology of bone growth in the tuberosity region in relation to the calcification and eruption of the molars. Other dental causes are unfavorable primary second molar crown morphology or an abnormal eruption angle of the permanent first molar. Heredity is another of the factors considered [1–3]. Tu et al. demonstrated three cases in a single family, including twins and an elder sister, indicating a familial tendency or a genetic background [4]. According to Young, ectopic eruptions of the permanent first molars are classified into two forms: reversible and irreversible. In the reversible form, the ectopically erupting permanent first molar frees itself naturally from a locked position and erupts into occlusion. This reversible pattern occurs in approximately 66% of ectopically erupting permanent maxillary first molars. In the irreversible form, due to the abnormal mesioangular eruption path of permanent first molars, this occurrence may result in impaction at the distal prominence of the primary second molar’s crown, and the permanent first molar remains in a locked position until active treatment is provided or premature exfoliation of a primary second molar occurs [2].
By the ages of seven and eight years, any ectopic eruption of a permanent first molar should be considered irreversibly locked. Young observed that ectopic eruptions of the permanent first molars occurred 52 times in 1,612 children (3%); with the problem seen more frequently in boys (33 times) than in girls (19 times) [5]. Early diagnosis and treatment can prevent a more complicated malocclusion. For severe impactions, treatment is required. Otherwise, this occurrence can result in early loss of the primary second molar and/or space loss [1]. Irreversible ectopic molars that remain locked, if untreated, can lead to premature loss of the primary second molar with a resultant decrease in quadrant arch length, asymmetric shifting of the permanent upper first molar toward class II positioning, and supraeruption of the opposing molar with distortion of the lower curve of Speed and potential occlusal interferences [5].
An eight-year-old girl was brought to Marmara University’s Department of Pediatric Dentistry for initial examination. In her medical history, she had no systemic diseases. An oral examination revealed a mixed dentition with evidence of bilateral semi eruption of the permanent maxillary first molars with different degrees (Figure 1). All other extraoral and intraoral clinical findings were within normal limits. The patient had panoramic X-rays taken initially (Figure 2), and then additional cone beam computed tomography was taken for a three-dimensional evaluation of the degrees and the angulations of mesioinclination of the permanent maxillary first molars and the extent of root resorption of the primary second molars due to their ectopic eruption (Figure 3).
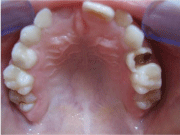
Figure 1: Eruption of the upper first permanent molars with different degrees.
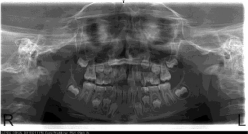
Figure 2: Panoramic x-rays
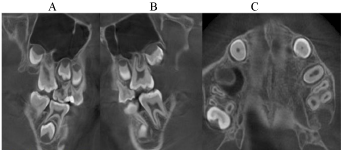
Figure 3: Cone beam computed tomography. The Left maxillary permanent
molar is seen locked (A); The Right maxillary permanent molar is seen locked
(B); Eruption of maxillary permanent molar with different degrees (C).
A CT examination revealed that resorptive changes were on the distal root of the left and right primary maxillary second molars and did not extend to the pulpal tissues, and they were considered still vital. The primary maxillary second molars were neither mobile nor sensitive to percussion or digital manipulation. There was no observable periodontal pathology. So a decision was made to keep both primary molars intact.
In the first appointment, an alginate impression was made. The eruption technique included two steps: stripping about 2 mm of the distal ends of both primary second molars, followed by a specially designed removable modified Hawley appliance (Figure 4). Enamel reductions were made with safe-tipped crosscut carbide stripping burs (Dentsply) under local anesthesia.
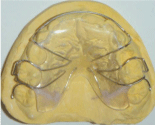
Figure 4: Specially designed removable modified Hawley appliance.
The appliance can be used both as a passive retainer (for retaining or stabilizing teeth in their new positions following the treatment) and as an active appliance in order to achieve minor tooth movements for distalization. The difference from a traditional Hawley appliance was the presence of C-shaped clasps at the distal end of both arches. These clasps were engaging the mesiobuccal undercuts of the permanent maxillary first molars and were activated to compensate for the reduced amount of the upper arch, achieving proper tooth distalization and occlusion. The clasps were adjusted 1.5 to 2 mm a month for a tooth movement of approximately 1 mm/month. The patient used the appliance all day long except during eating, and patient compliance was excellent due to the simple design of the appliance. The eruptions of both permanent maxillary first molars were achieved at the end of a five-month period. Eventually, a proper occlusion was established as seen in (Figure 5,6).
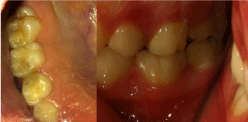
Figure 5: Establishing the proper occlusion of right side, after 6 months of
treatment.
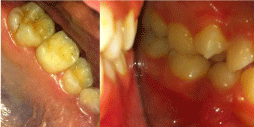
Figure 6: Establishing the proper occlusion of left side, after 6 months of
treatment.
Conclusion
A number of corrective procedures have been reported with treatments varying according to the extent of blockage, degree of primary tooth resorption, direction of displacement, timing, arch length status, and patient cooperation. Approaches included separators and distalizing appliances [5].
In general, a permanent molar with a minor degree of impaction will naturally correct itself. However, if there is a greater degree of impaction, including the complete marginal border, it usually cannot self-correct.
This case report emphasized that the early correction of an ectopic eruption was essential, critical for the development of a stable occlusion, and an important component of interceptive orthodontic treatment. If early interception was not initiated, extraction of primary second molars, exposition of the permanent first molar surgically, distalization, or waiting for the permanent first molar to erupt, then distalizing it later by using a fixed or removable appliance are the options for the treatment of severe cases [6–9].
The pediatric dentist can choose from a variety of effective treatment modalities to successfully manage ectopically erupting permanent molars. The appliance used in this treatment was preferred when compared to those of the other methods, especially in cases where permanent first molars were locked on the distal end of primary molars and the child patient was unwilling to use a complicated appliance. The Humphrey’s appliances had a distally directed S-shaped loop that was actively engaged onto the occlusal surface of the ectopically erupting permanent molar. Problems in activation and adjustment of the spring and possible reciprocal movement of primary molars were all disadvantages. The Halterman appliance used elastomeric chains rather than springs as the distalizing force [5]. A fixed unilateral appliance was described by Croll and Barney [9]. Nagaveni and Radhika [10] applied a modified Humphrey’s appliance. A removable appliance that is easy to use could be less irritating than fixed appliances in children, but patient compliance is essential in order to get a satisfactory result. This treatment has shown that early intervention in a pediatric setting may reduce further aggressive orthodontic treatment if diagnosed properly.
References
- AAPD Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry Reference Manual. 2009; 34: 12-13.
- Young DH. Ectopic eruption of permanent first molar. J Dent Child. 1957; 24: 153–162.
- Yaseen SM, Naik S, Uloopi KS. Ectopic eruption - A review and case report. Contemp Clin Dent. 2011; 2: 3–7.
- Tu HH, Wang YL, Chou HF. Ectopic eruption of first maxillary permanent molars in siblings- Case report. Chin Dent J. 2002; 21: 177-182.
- Dean JA, Avery DR, McDonald RE. Dentistry for the Child and Adolescent. 9th Edition. 2011: 590-594.
- Barberia-Leache E, Suarez-Clua MC, Saavedra-Ontiveros D. Ectopic eruption of the maxillary first permanent molar: Characteristics and occurrence in growing children. Angle Orthod. 2005; 75: 610-615.
- Seehra J, Winchester L, DiBiase AT, Cobourne MT. Orthodontic management of ectopic maxillary first permanent molars: a case report. Aust Orthod J. 2011; 27: 57-62.
- Corbett MC. Slow and continuous maxillary expansion, molar rotation, and molar distalization. J Clin Orthod. 1997; 73: 253-263.
- Croll TP, Barney JI. An acid etch composite resin retained wire for correction of an ectopically erupting permanent first molar. Am Acad Pedodontics. 1982; 4: 61-63.
- Nagaveni NB, Radhika NB. Interceptive orthodontic correction of ectopically erupting permanent maxillary first molar. A case report. VJ Orthodontics. 2010; 8: 1-13.