
Special Article – Dental Case Reports
J Dent App. 2016; 3(2): 322-324.
Bone Regeneration of Atrophic Posterior Maxilla with BMP-2
Queiroz TP¹, Margonar R¹, Silva de Oliveira JC2*, Betoni-Júnior W³, Marcantonio E4, Sanches-Neto F5 and Luvizuto ER2
¹Department of Health Sciences, Implantology Post Graduation Course, Dental School, University Center of Araraquara, UNIARA, So Paulo, Brazil
²Department of Surgery and Integrated Clinic, Araçatuba Dental School, Universidade Estadual Paulista, Brazil
3Department of Oral Surgery, Dental School, University of Cuiaba, MatoGrosso and Dental School, University of Cuiaba, MatoGrosso, Brazil
4Department of Oral Diagnosis, Discipline of Period ontology, Araraquara Dental School, Universidade Estadual Paulista, Brazil
5Especialist in Implantology from Dental School, University of Cuiaba, MatoGrosso, Brazil
*Corresponding author: Julio Cesar Silva de Oliveira, Department of Surgery and Integrated Clinic, Araçatuba Dental School, Universidade Estadual Paulista, Rua José Bonifácio 1193CEP: 16015-050, Araçatuba, SP, Brazil
Received: August 06, 2016; Accepted: September 26, 2016; Published: September 28, 2016
Abstract
The insertion of implants in the posterior maxilla can present some limitations such as the maxillary sinus pneumatization. To reverse this situation, it is necessary to use some type of graft, as synthetic materials and growth factors, since the autogenous bone has some disadvantages such as risk of infection and morbidity post higher operative. The ability of BMP-2 to induce bone formation is clearly well proven in a wide variety of experimental models and clinical studies, presenting precise information. The authors present a clinical case of bone regeneration of atrophic posterior maxilla with BMP-2 associated with bovine bone mineral matrix in a patient who refused autologous bone graft because of surgical morbidity, achieved excellent results both in height and bone width for implant placement in a second surgical procedure.
Keywords: BMP-2; Bovine bone mineral matrix; Sinus-lifting; Biomaterials; Graft
Introduction
The use of grafts in surgery of dental implants has as main objective the restoration of bone volume in height and width. Although the autograft is considered as the gold standard in sinus lifts [1], many biomaterials have been used with high success rates and less morbidity compared with intraoral or extraoralautogenous bone [1-3].
The use of biomaterials in extraction socket preservation, implant site development (guided bone regeneration) and sinus lift procedures are currently a well-documented and reliable approach [2-4].
Over the years, different bone substitutes have been proposed in an attempt to avoid the donor site morbidity associated with autogenous bone grafts, and to provide suitable alternatives when insufficient donor bone is available [5]. Many clinical studies have been carried out with signaling molecules, such as recombinant human bone morphogenetic protein (rhBMP), for inducing bone formation to overcome the drawbacks of the procedures for vertical ridge augmentation [6].
The BMPs (except for BMP-1) are members of the transforming growth factor-β super family of polypeptide growth factors [7] and play a crucial role in the regulation of bone induction, maintenance, and repair [4].
The authors present a clinical case of bone regeneration of atrophic posterior maxilla with BMP-2 associated with bovine bone mineral matrix in a patient who refused autologous bone graft because of surgical morbidity. Subsequently, three implants were installed in a second surgical procedure achieving good functional and aesthetic results.
Case Presentation
A 67-year-old woman was referred to the University Center of Araraquara - UNIARA, for oral rehabilitation of the posterior region of the right maxilla which had absence of premolars and molars and vertical bone loss with 1 mm (Figure 1A and 1B). The patient reported being a carrier of non-smoking, high blood pressure controlled by medication, and absence of bruxism. Upon request of imaging studies, it was observed on CT pneumatization of the maxillary sinus with total absence of bone height for placing dental implants (Figure 1C).
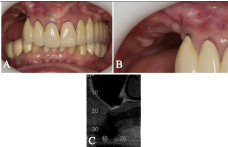
Figure 1: A- Front view of the occlusion of the patient. B- Closer view of
the clinical edentulous region that was subjected to maxillary sinus lifting.
C- Panoramic radiograph of the maxilla.
Several possibilities of bone grafting for maxillary sinus lifting were presented to the patient, including the use of autograft and osteoinductives biomaterials, with their advantages and disadvantages. The patient refused autograft because of surgical morbidity, hence the choice of performing surgery of maxillary sinus using Infuse® (Medtronic Sofamor Danek USA, Inc) associated with Bio-Oss® (GeistlichPharma Group Ltd., Switzerland) and subsequent installation of three implants in a second surgical procedure.
One hour prior to surgery, the patient was pre-treated with 2 g amoxicillin, 5 mg diazepam. Local anesthesia with prilocaine hydrochloride with felypressin 0.03 IU/ml was administered. An incision on the crest of the right maxillary ridge with a relaxing in the canine distal preserving its papilla and relaxing in the posterior region of the right maxilla was performed with a scalpel bladen 15. With the peeler of Molt, the detachment of total retail to expose the bone tissue was performed. Through a round bur was performed in a window and maxillary sinus mucosa was detached (Figure 2A). The maxillary sinus was first filled with Infuse® which was prepared according to the manufacturer’s recommendations and was subsequently added Bio-Oss® (Figure 2B). A resorbable membrane of type I collagen (BioMend, Zimmer Dental Inc. Carlsbad, CA) was positioned protecting rhBMP-2 from soft tissue invagination in the reconstructed area (Figure 2C). The flap was sutured with 5-0 nylon (Figure 2D). The immediate postoperative period was uneventful. The prosthesis was worn out and retrofitted with soft resin 15 days after the surgical procedure.
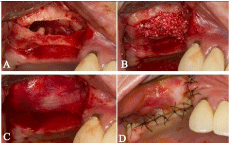
Figure 2: A- Exposure of the sinus floor after detachment of the membrane.
B- Introduction and adaptation of Bioss® + Infuse® in the surgical cavity.
C- Adaptation of collagen type I membrane. D- Replacement of the flap by
means of suture isolated.
A second CT scan was performed after 5 postoperative months for planning of implants and a bone height of 13 mm was achieved after grafting. A new surgical intervention was performed for the installation of 3 implants in the grafted area (AR Conn., 3.75 x 13 mm, Connection Implant Systems Arujá, So Paulo, Brazil). A new CT scan was performed after the installation of the implants, which can be compared before and after (Figure 3A and 3B), in which there was a considerable increase in bone height. The period of osseointegration of implants was expected and fixed porcelain prostheses were fabricated and installed (Figure 4). The case is presented with one year follow up after installation and prosthetic patient is satisfied.
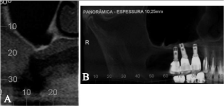
Figure 3: A- Sagittal CT scan showing complete lack of bone height for
installation of dental implants. B- Image of the panoramic radiograph of the
right hand after the procedure of bone grafting and implant placement.
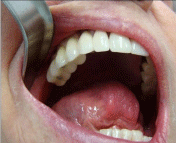
Figure 4: Final prosthesis fabricated and installed in the patient’s right
posterior maxillary region with good aesthetic and functional results.
Discussion
Rehabilitation of partial or complete edentulous maxilla using implants is often limited by the quantity and quality of available bone and requires endosinus graft procedures to create space between the maxillary sinus floor and the Schneider membrane [8].
Surgical methods for vertical ridge augmentation include autogenous bone block grafting, guided bone regeneration (GBR), distraction osteogenesis, and forced tooth eruption, of which autogenous bone block grafting using bone with osteogenic potential is the most reliable method [6]. In the case of sinus lifting, the standard surgical technique involves raising the sinus mucous membrane and filling the cavity with either bone or biomaterials, or a combination of these [9].
Despite the cortico-medullary autogenous bone graft is the material of choice for bone grafting, mainly due to its osteoconductive, osteoinductive, osteogenic properties, it is associated with limiting the amount, in addition to donor site morbidity, infection, pain and blood loss [4,10,11], including the need for general anesthesia extraoral cases. However, alternatives for autogenous transplantation can be created by Tissue Engineering by means of the proliferation of autogenous osteoblast-like cells in combination with growth factors and biomaterials to generate functional tissues [9].
In this scenario, animal experiments [7] and clinical trials [12,13] have shown that bone morphogenic proteins (BMP) support bone repair, confirming that the administration of recombinant BMP- 2 proteins induces orthopic and ectopic bone formation [5], being highly osteoinductive. Furthermore, Bio-Oss®, xenogenic material from which all organic components have been removed, is similar to human cancellous bone [14]. It is considered an excellent osteoconductive material and has been successfully tested both in preclinical studies in an animal model and in clinical trials with excellent prognosis for the implants positioned in the regenerated sites8, both used successfully in this clinical case.
Differentiation factors such as rhBMP-2, may be useful in stimulating osseous regeneration when native bone is desired to maintain an alveolar ridge following tooth extraction [12]. The combination of an osteoinductive protein (rhBMP-2) with a clinically well-established osteoconductive material would allow one to overcome some of the difficulties encountered with the present bone regeneration techniques [13,15].
The authors believe that the union of the osteoconductive properties of the Bio-Oss® as best bone scaffold with growth factors of the Infuse®, as presented in this clinical case, we emphasize the unique characteristics of each, favoring the subsequent installation of dental implants.
References
- Antoun H, Bouk H, Ameur G. Bilateral sinus graft with either bovine hydroxyapatite or beta tricalcium phosphate, in combination with platelet-rich plasma: a case report. Implant Dent. 2008; 17: 350-359.
- Lambert F, Lecloux G, Léonard A, Sourice S, Layrolle P, Rompen E. Bone regeneration using porous titanium particles versus bovine hydroxyapatite: a sinus lift study in rabbits. Clin Implant Dent Relat Res 2013; 15: 412-426.
- Chaves MD, Nunes LSS, de Oliveira RV, Holgado LA, Nary Filho H, Matsumoto MA, et al. Bovine hydroxyapatite (Bio-Oss®) induces osteocalcin, RANK-L and osteoprotegerin expression in sinus lift of rabbits. J Craniomaxillofac Surg. 2012; 40: e315-e320.
- Schmitt C, Lutz R, Doering H, Lell M, Ratky J, Schlegel KA. Bio-Oss® blocks combined with BMP-2 and VEGF for the regeneration of bony defects and vertical augmentation. Clin Oral Implants Res. 2013; 24: 450-460.
- Szpalski M, Gunzburg R. Recombinant human bone morphogenetic protein-2: a novel osteoinductive alternative to autogenous bone graft? Acta Orthop Belg. 2005; 71: 133-148.
- Kim SJ, Shin HS, Shin SW. Effect of bone block graft with rhBMP-2 on vertical bone augmentation. Int J Oral Maxillofac Surg. 2010; 39: 883-888.
- Arosarena O, Collins W. Comparison of BMP-2 and -4 for rat mandibular bone regeneration at various doses. Orthod Craniofac Res. 2005; 8: 267-276.
- Y Baena RR, Lupi SM, Pastorino R, Maiorana C, Lucchese A, Rizzo S. Radiographic evaluation of regenerated bone following poly (lactic-co-glycolic) acid/hydroxyapatite and deproteinized bovine bone graft in sinus lifting. J Craniofac Surg. 2013; 24: 845-848.
- Gutwald R, Haberstroh J, Stricker A, Rüther E, Otto F, Xavier SP, et al. Influence of rhBMP-2 on bone formation and osseointegration in different implant systems after sinus-floor elevation. An in vivo study on sheep. J Craniomaxillofac Surg. 2010; 38: 571-579.
- Marukawa K, Ueki K, Okabe K, Nagakawa K, Yamamoto E. Use of self-setting alpha-tricalcium phosphate for maxillary sinus augmentation in rabbit. Clin Oral Implants Res. 2011; 22: 606-612.
- Ewers R, Goriwoda W, Schopper C, Moser D, Spassova E. Histologic findings at augmented bone areas supplied with two different bone substitute materials combined with sinus floor lifting. Report of one case. Clin Oral Implants Res. 2004; 15: 96-100.
- Cochran DL, Jones AA, Lilly LC, Fiorellini JP, Howell H. Evaluation of recombinant human bone morphogenetic protein-2 in oral applications including the use of endosseous implants: 3-year results of a pilot study in humans. J Periodontol. 2000; 71: 1241-1257.
- Jung RE, Glauser R, Schärer P, Hämmerle CHF, Sailer HF, Weber FE. Effect of rhBMP-2 on guided bone regeneration in humans. Clin Oral Implants Res. 2003; 14: 556-568.
- Scarano A, Pecora G, Piatelli M, Piatelli A. Osseointegration in a sinus augmented with bovine porous bone mineral: histological results in an implant retrieved 4 years after insertion. A case report. J Periodontol. 2004; 75: 1161-1166.
- Boyne PJ, Shabahang S. An evaluation of bone induction delivery materials in conjunction with root-form implant placement. Int J Periodontics Restorative Dent. 2001; 21: 333-343.