
Special Article – Eating Disorders
J Dent App. 2016; 3(4): 353-357.
Exploring the Impact of Oral Health on Quality of Life of Eating Disorders Patients
Vecchiattini R¹, Scardovelli I², Pisani FA³, Mobilio N¹, Trombelli L4 and Manzato E5*
¹Dental Clinic, Dental School, Department of Biomedical and Specialty Surgical Sciences, University Hospital, University of Ferrara, Ferrara, Italy
²Private Practice, Ferrara, Italy
³Private Practice, San Giovanni di Casarsa (PN), Italy
4Professor and Chairman, Dental Clinic, Research Centre for the Study of Periodontal and Peri-implant Diseases, University Hospital, University of Ferrara, Italy
5Psychiatrist, Private Practice, Ferrara, Former Chief of Eating Disorders Unit, University Hospital, Ferrara, Italy
*Corresponding author: Manzato E, Psychiatrist, University of Ferrara, Viale Cavour 190, 44121 Ferrara, Italy
Received: November 16, 2016; Accepted: December 26, 2016; Published: December 28, 2016
Abstract
Introduction: Eating Disorders (ED) are psychiatric conditions complicated by multiple organ dysfunctions that require multidisciplinary and integrated care strategies. ED can lead to severe physical complications and tend to be persistent. ED patients often present extensive dental health problems, with worsening in their oral health-related quality of life (OHRQoL), and then in patient’s well-being. Although regarded primarily as a mental health issue, ED can result in many serious systemic health conditions.
Objective: To assess the impact of OH outcomes on QoL in a population of ED patients compared to healthy subjects and, for patients undergoing dental examination and treatment, to assess the impact of non surgical periodontal treatment on oral health and QoL.
Methods: The Italian version of the Oral Health Impact Profile (OHIP-49) was administered to 37 patients (24 diagnosed for ED, 13 healthy). Between those diagnosed for ED, 12 patients underwent to dental examination and periodontal treatment. After 90 days OHIP-49 was administered again.
Results: ED patients showed significantly higher scores of OHIP-total score when compared to healthy patients. Considering ED patients, there was a significant difference in the psychological dimension of OHRQoL for those refusing dental procedures, indicating a worse well-being. Also significant difference of OHRQoL was reported for patients undergoing dental procedures, when compared to ED patients who refused.
Conclusion: ED diagnosis may have a negative effect on the impact of oral health on OHRQoL. Periodontal treatment, motivation, counseling and psychological approach may have a positive effect on OHRQoL of ED diagnosed patients.
Keywords: Eating Disorders; Oral Health-Related Quality of Life; Secondary Prevention; Oral Health Impact Profile
Abbreviations
ED: Eating Disorders; AN: Anorexia Nervosa; BN: Bulimia Nervosa; BED: Binge Eating Disorder; OHRQoL: Oral Health Related Quality of Life; OHIP: Oral Health Impact Profile
Introduction
Eating Disorders (ED) are psychiatric conditions complicated by multiple organ dysfunctions due to malnutrition, binging, purging and excessive compulsive exercise, potentially leading to a variety of severe, life threatening medical consequences.
The 5th edition of Diagnostic and Statistic Manual of Mental Disorders [1] defined ED as “a persistent disturbance of eating or eating – related behaviour that results in the altered consumption or absorption of food and that significantly impairs physical health or psychosocial functioning.
“Feeding and Eating disorders” are classified in: Anorexia Nervosa (AN), Bulimia Nervosa (BN), Binge Eating Disorder (BED), Other Specified Feeding and Eating disorders and Unspecified Feeding and Eating disorders.
The patients with AN shows a persistent energy intake restriction, intense fear of gaining, and a significant disturbance in the perception of their shape.
The weight loss could be accomplished through dieting, fasting, excessive exercise, and/or by self-induced vomiting, laxatives, diuretics, and/or enemas misuse.
The essential features of BN are binge eating and inappropriate compensatory methods to prevent weight gain. In addition, the selfevaluation of individuals with BN is excessively influenced by body shape and weight.
BED is characterized by recurrent episodes of binge eating without compensative behaviours. It is often associated with overweight or obesity.
Many patients with ED present serious oral manifestations strictly connected to illness. The complications can be both aesthetic and functional and give different symptoms, like tooth erosion, sensitivity and oral ache.
Persistent vomiting can lead to esophagitis, esophageal ulcers, or esophageal rupture (life threatening event), emathemesis and to severe chronic gastroesophageal reflux disease (GERD), that is the predisposing factor to the Barrett’s Esophagus.
Also the anorexic malnutrition increases the risk of oral complications, in fact chronic starvation leads to a significant decrease in resistance to infections resulting in a progressive inflammatory status [2].
Furthermore Binge Eating Disorders- often associated with increased weight gain and severe obesity- could have an important impact on oral health through the development of metabolic syndrome [3].
Main oral manifestations for ED patients are dental erosion. Erosion damages are caused by acid dissolution of dental hard tissues. Dental erosion is observed in 8.8% of healthy patients, compared to 45.0% of ED patients [4]. The inner causes include all diseases and/ or habits, such as self-induced vomiting that allow acid substances from the stomach to the oral cavity. Besides stomach content, the erosive potential is also affected by diet, such as regular consumption of acidic or sweetened foods [5]. Aggressive tooth brushing after vomiting contributes to enhance erosive damages [6].
Another common symptom from dental erosion is toothache and/or hypersensitivity. Frequently vomiting can cause salivary glands inflammation, usually for parotid glands. Saliva flow rate is reduced, as inner buffering capacity [5]. Hyposalivation can induce an increased risk rate and progression in developing caries.
Because the oral manifestations from AN and BN are quite specific, Otolaryngologists, Dentist and/or Dental Hygienist can be the first identifying a patient with ED, when aware of the related oral signs. Increasing the levels of knowledge of these specialists about the oral and physical clues of AN and BN could lead to efficient and early diagnosis for ED.
Specifically the dental hygienist, due to the length of time spent with the patient, could be in a favourable condition to develop a strong relationship so encouraging the motivation to care [7].
Failure to make an early diagnosis of these oral health manifestations may not only increase the likelihood of irreversible damage to the oral cavity, but also may lead to the development of additional serious systemic health problems [8].
Unfortunately many patients avoid going to the Dentist and/or Dental Hygienist until the damages are irreversible and symptomatic [5].
A study on a sample of dentists investigating their ability to correctly diagnose the patients with ED showed that less than half of dentists reported currently assessing patients for ED and only 19% reported that they communicated with the patient’s PCP about suspected ED [9].
The fear of offending patient, the lack of training in patient approach and lack of interdisciplinary communication were considered by dentists as obstacles to investigate the presence of ED.
But often this important opportunity to improve the secondary prevention is lost. Early detection of ED could have a positive prognostic value in both sexes [10], could prevent severe complications and could improve the global outcome (secondary prevention).
Furthermore it could have an important role to reducing oral and medical complications associated with purging behavious.
Actually the diagnosis may still be more difficult and delayed so an efficient secondary prevention of ED is a challenge.
The ED early diagnosis is still difficult due to many factors.
ED patients are generally characterized by low levels of awareness about their illness and- unlike patients with other psychiatric conditions - they do not experience their symptoms as distressing, consequently they may not be motivated to treatment.
Furthermore physicians are not enough skilled in recognizing the signs and symptoms of ED and therefore they are not able to engage the patients in a diagnostic and therapeutic process.
In fact some studies show a failure of physicians in recognizing ED, so that ED may be undetected for about 50% of the cases [11].
To confirm this finding a study done by Hoek [12] in Holland revealed that, in an estimated number of ED in the population, only 43% of patients with AN goes to their General Practitioner (GP) and only 79% of these arrives to specialized centres.
As regards BN the percentages are even more dramatic: only 11% see a GP and only 51% of these reaches a specialized centre.
So a long time passes between onset of an ED and the treatment: Bulimia last for about 4 years for women, and 8 years for males before to be diagnosed.
Because a long duration of the disorder is associated with a worse prognosis it could be important to make the correct diagnosis as soon as possible, improving secondary prevention strategies.
Therefore all specialists who may come into contact with patients with ED may help to improve secondary prevention.
Dental treatment for ED patients is focused on eliminating pain and prevents further complications.
It is also very important to inform ED patients about the causes and why the risk of oral damages is so high for them. Information and instructions in oral health care for ED patients decrease the progression of dental erosion [5].
Planning dental treatment for ED patients it is important to primarily focus on the general health. Concerns around the dental health often have to wait until the illness is under control. Oral health- related quality of life (OHRQoL) has important implications for the clinical practice [13]. OHRQoL is an integral part of general health and well-being and is recognized by the WHO as an important segment of the Global Oral Health Program [14].
Quality of life (QoL), or individuals “perceptions of their position in life in the context of culture and value systems in which they live, and in relation to their goals, expectations, standards, and concerns” [15], is now recognized as a valid parameter in patient assessment in nearly every area of physical and mental healthcare, including oral health.
Oral health has been traditionally assessed based on normative clinical indicators. However, normative approach has been criticized because they neither catch nor document the full impact of oral disease and disorders on affected individuals. Questionnaires are good methods to objectify many aspects, both reated to oral health and QoL. Thus, OHRQoL measures have emerged as an important health outcome in clinical trials and healthcare research.
Assessment of OHRQoL allows for a shift from traditional normative approach to assessment and care that focus on patients’ social and emotional experience and physical functioning in defining appropriate treatment goals and outcomes [13].
OHRQoL can be useful in measuring the impact of oral health disparities on overall health and QoL.
There are more and more tools to measure the OHRQoL. In Dentistry too, OHRQoL has been gradually emphasised [16].
Knowing patients’ QoL allows to evaluate subjective feeling. Compared with various clinical indexes, patients subjective feeling about the disease and treatment has more significant influence on their QoL [16].
The tool most frequently used for telling OHRQoL is Oral Health Impact Profile (OHIP), developed by Slade and Spencer [17]. The measure content of OHIP is asking patients whether their quality of life has been affected by oral health problems. There are seven categories in the measure content which are functional limitation, physical discomfort, psychological discomfort, physical disability, psychological disability, social disability and handicap [16,18].
The aim of our study was to investigate the correlation between oral health and quality of life among ED patients. The study investigated:
- The impact of oral health outcomes on QoL in a population of ED patients compared to healthy patients;
- The impact of non surgical periodontal treatment on oral health and QoL in a population of ED patients undergoing dental treatment.
- Waiting room of Dental Clinic, University of Ferrara, including both healthy and ED patients;
- Waiting room of Eating Disorders Unit, University Hospital, Ferrara, including ED patients.
- American Psychiatric Association: Diagnostic and Statistical manual of Mental Disorders. 5th edn. Arlington, VA: American Psychiatric Association, 2013.
- Malgorzata Lotwinska S, Slotwinski R. Host response, malnutrition and oral diseases. part 1. Centr Eur J Immunol. 2014; 39: 518-521.
- Marchetti E, Monaco A, Procaccini L, Mummolo S, Gatto R, Tetè S, et al. Periodontal disease: the influence of metabolic Syndrome. Nutrition & Metabolism. 2012; 9: 88.
- Hermont AP, Pordeus IA, Paiva SM, Abreu MH, Auad SM. Eating disorder risk behavior and dental implications among adolescents. Int J Eat Disord. 2013; 46: 677–683.
- DeBate RD, Shuman D, Tedesco LA, Johansson AK, Carlsson EG. Dental erosion. Stockholm: Författarna och Förlagshuset Gothia AB. 2006; 157: 27-33, 39-47, 115-138.
- Otsu et al. Factors affecting the dental erosion severity of patients with eating disorders. BioPsychoSocial Medicine. 2014; 8: 25.
- DiGioacchino DeBate R, Tedesco L. Increasing dentists’ capacity for secondary prevention of eating disorders: identification of training, network, and professional contingencies. J of Dental Education. 2006; 70: 1066-1075.
- DeBate RD, Shuman D, Tedesco LA. Eating Disorders in the Oral Health Curriculum. J of Dental Education. 2007; 71: 655-663.
- DeBate RD, Plichta S, Tedesco LA, Kerschbaum WE. Integration of oral health care and mental health services: dental hygienists’ readiness and capacity for secondary prevention of eating disorders. J Behav Health Serv Res. 2005; 33: 113-125.
- Manzato E, Gualandi M, Zanetti T, Strumia R. Eating Disorders in Males. New York: Nova Science edn, 2011.
- King MB. Eating disorders in a general practice population: prevalence, characteristics and follow-up at 12 to 18 months. Psychol Med (Monogr. Suppl.). 1989; 14: 1-34.
- Hoek HW. The incidence and prevalence of anorexia nervosa and bulimia nervosa in primary care. Psychol Med.1991; 21: 455-460.
- Sischo L, Broder HL. Oral health-related quality of life: what, why, how, and future implications. J Dent Res. 2011; 90: 1264-1270.
- WHO. The World Oral Health Report 2003: continuous improvement of oral health in the 21st century—the approach of the WHO Global Oral Health Programmed. Geneva, Switzerland: World Health Organization. 2003.
- WHOQOL. The World Health Organization quality of life assessment (WHOQOL): position paper from the World Health Organization. Soc Sci Med. 1995; 41: 1403-1409.
- Lee IC, Yang YH, Ho PS, Lee IC. Exploring the quality of life after denture-wearing within elders in Kaohsiung. Gerodontology. 2012; 29: e1067-e1077.
- Slade GD, Spencer AJ. Development and evaluation of the Oral Health Impact Profile. Community Dent Health. 1994; 11: 3–11.
- Castrejón-Pérez RC1, Borges-Yáez SA, Irigoyen-Camacho ME. Validaciòn de un instrumento para medir el efecto de la salud bucal en la calidad de la vida de adultos mayores mexicanos. Rev Panam Salud Publica. 2010; 27: 321-329.
- Ainamo J, Bay I. Problems and proposals for recording gingivitis and plaque. Int Dent J. 1975; 25: 229–235.
- Silness J, Löe H. Correlation between oral hygiene and periodontal condition. Acta Odontol Scand. 1964; 22: 121–135.
- Bartlett D, Ganss C, Lussi A. Basic Erosive Wear Examination (BEWE): a new scoring system for scientific and clinical needs. Clin Oral Invest. 2008; 12: 65–68.
Materials and Methods
Ethics clearance was provided by the Local Human Research Ethics Committee of the University Hospital and University of Ferrara.
The OHIP-49 was the evaluation tool for measuring the OHRQoL, with 49 questions and seven dimensions to measure.
The Italian version of OHIP-49 was administered to patients in different places:
The higher score indicated that oral health condition had a greater (more significant) impact on patients’ life. For each of the 49 questions, patients were asked how frequently they had experienced impact in the preceding 30 days using a Likert-like scale coded 4 = very often, 3 = fairly often, 2 = occasionally, 1 = hardly ever and 0 = never. The responses were scored by counting the number of items, with codes indicating an impact by coding response levels and summing these coded responses across all items. Higher OHIP scores indicate poorer OHRQoL. The scores of the seven dimensions were calculated and combined into a total score with Additive method (ADD-Method) [17].
For all patients the same protocol was followed, according to their willing through dental treatment (Figure 1).
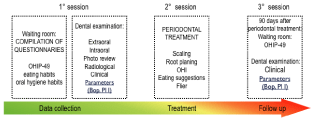
Figure 1: Study protocol. All ED and healthy patients filled OHIP-49 in waiting
room. For those patients with ED who underwent clinical exam and dental
treatment, is was possible to compare also periodontal parameters and
OHIP-49 scores after 90 days from 1st session.
The periodontal condition was evaluated by gingival bleeding on probing [19] and the modified version of the Silness and Löe plaque index (1964) [20].
Bleeding on probing was recorded ten seconds after probing the mesial, distal, buccal, palatine and lingual surfaces of the index teeth using a periodontal probe (PCP-UNC 15, Hu-Friedy®, Chicago, IL, USA). The presence of plaque on the buccal, lingual, mesial and distal surfaces of the index teeth was recorded according to the Silness and Löe plaque index [19,20]. For each patient a full mouth score was recorded as percentage of full dentition. Erosive tooth wear was measured using the Basic Erosive Wear Examination Index (BEWE, 0–18) index [21]. All tooth surfaces were examined and the highest score for each sextant was recorded.
All variables (gender, age, BEWE, clinical periodontal indexes, OHIP-49 scores) were initially included in bivariate analyses (chisquare test), and the variables that were statistically significantly associated with OHIP were included. The statistical analysis of this research was conducted by using the software package SPSS version 10 for Macintosh (SPSS Inc., Chicago, IL, USA). The Mann-Whitney test was used to present the score distribution of variables in the total OHIP score. A P-value <0.05 was considered statistically significant.
Results and Discussion
A total of 37 patients (7 males and 30 females) constituted the study sample. The test was administered at the Dental Clinic, University of Ferrara, and at the Eating Disorders Unit, University Hospital, Ferrara.
24 subjects were diagnosed for ED, 13 subjects were healthy. The exclusion criteria used for healthy patients were: abuse of alcohol, drugs or medication and a present or pre-existing ED diagnose.
According to the diagnostic criteria of Diagnostic and Statistic Manual of Mental Disorders ED patients were divided by diagnosis (Figure 2). Patients were distinguished based on diagnosis, meanwhile severity of the ED was not described. Oral symptoms caused by ED vary depending on which kind of eating disorder the person suffers from. All ED patients in this study were included if ED was present or was preexisting; then ED patients were considered as homogeneous group. This was done because the aim of this study was not to investigate the link between severity of ED and oral health, but to investigate OHRQoL in this specific group.
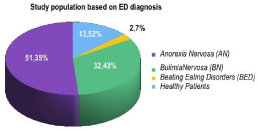
Figure 2: Patients distribution according to ED diagnosis.
Between those diagnosed for ED, 12 patients (4 males and 8 females) underwent to specific non surgical periodontal treatment. Due to the small sample, all these patients were diagnosed for AN.
After 90 day OHIP-49 was administered again to these 12 patients and results were compared. The age and dental status of the ED patients and Healthy patients were quite similar and comparable (Table 1). Considering clinical parameters for ED patients undergoing dental treatment, BoP Score and Pl Index Score were similar to healthy patients, and after periodontal treatment slight reduction was observed for both of them (Figure 3).
AGE (mean)
SEX
BEWE
Bleeding on Probing
Plaque Index
ED patients
28
M (4)
F (9)
0,75
16%
45%
Healthy Patients
23
M (3)
F (21)
4,85
18%
37%
Table 1: Statistics over dental status and age of ED patients and healthy patients group presented as an average value.
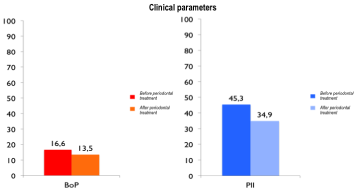
Figure 3: Clinical parameters such as Bleeding on Probing (BoP) and Plaque
Index (PlI) were slightly reduced by treatment (P>0.05). BoP and PlI low rate
were registered before and after treatment, confirming that OHRQoL is not
only related to clinical parameters.
The ED patients group had a higher total average score from OHIP-49 compared to the healthy patients group (Figure 4). The total average for the ED patients group was 38, 26 and for the healthy patients group it was 15, 08. In every section of OHIP-49 (functional limitation, physical pain, psychological discomfort, physical disability, social disability and handicap) the ED patients group showed a higher average than the healthy patients group.
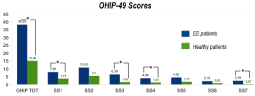
Figure 4: Distribution of average OHIP-49 scores. Comparison between ED
patients and healthy patients. The association between OHRQoL and ED
diagnosis was investigated with the Mann-Whitney test. ED patients showed
significantly (P<0.05) higher scores of OHIP-total score and OHIP subscales
1, 3, 4 and 7 (functional limitation, psychological discomfort, physical disability
and handicap) when compared to healthy patients.
ED patients showed significantly (P<0.05) higher scores of OHIPtotal score and OHIP subscales 1, 3, 4 and 7 (functional limitation, psychological discomfort, physical disability and handicap) when compared to healthy patients. Considering ED patients, there is a statistically significant difference in the psychological dimension of OHRQoL (P<0.05) for those refusing dental procedures, which have higher OHIP subscale 3 (psychological discomfort) when compared to healthy patients, indicating a worse well-being. Considering ED patients, there is a statistically significant difference in the psychological dimension of OHRQoL (P<0.05) for those patients undergoing dental procedures, when compared to ED patients who refused treatment (Figure 5).
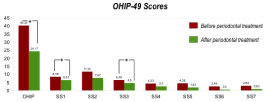
Figure 5: Comparison between ED patients OHIP-49 scores before and after
periodontal treatment. The association between OHRQoL and ED diagnosis
was investigated with the Mann-Whitney test. Considering ED patients,
there is a statistically significant difference in the psychological dimension of
OHRQoL (P<0.05) for those refusing dental procedures, which have higher
OHIP subscale 3 (psychological discomfort) when compared to healthy
patients, indicating a worse well-being.
This study confirmed that OHIP-49 was a reliable and valid questionnaire to measure the social impact of oral complications and was useful for both clinical decision-making and research [17].
Conclusion
ED diagnosis may have a negative effect on the impact of oral health on quality of life (OHRQoL). Nonsurgical periodontal treatment, motivation, counseling and psychological approach may have a positive effect on OHRQoL of ED diagnosed patients. Dental hygienists’ role in these patients management is crucial and needs to be investigated in further studies.
References