
Case Presentation
J Dent App. 2016; 3(4): 358-360.
Recurrent Sialadenitis with Sialolithiasis of Submandibular Gland: A Case Report
Tulasi Lakshmi D¹, Firoz Babu P², Negi LS¹ and Nayyar AS¹*
¹Department of Oral Medicine and Radiology, Saraswati Dhanwantari Dental College and Hospital and Post- Graduate Research Institute, Parbhani, Maharashtra, India
²Department of Orthodontics and Dentofacial Orthopedics, Rama Dental College and Hospital, Kanpur, Uttar Pradesh, India
*Corresponding author: Abhishek Singh Nayyar, 44, Behind Singla Nursing Home, New Friends’ Colony, Model Town, Panipat-132 103, Haryana, India
Received: December 02, 2016; Accepted: December 28, 2016; Published: December 30, 2016
Abstract
Sialoliths are calcareous concretions that may be found in the ducts of the major or, minor salivary glands or, within the glands themselves. The condition is found more commonly in middle-aged adults. The salivary gland most commonly affected is the submandibular gland. Clinically, it presents like an acute, painful, and intermittent swelling of the gland, especially during a meal, when the saliva flow is increased. In this report, we have reported a case of 21 year old male patient with sialolithiasis of the left submandibular duct. The treatment consisted of the use of lemon and orange drop candies, which stimulated the salivary flow and in turn, resulted in the expulsion of stone.
Keywords: Sialolith; Sialadenitis; Salivary Gland
Introduction
Sialolithiasis is the most common cause of salivary gland obstruction, and is found in approximately 65% of the patients with chronic sialadenitis. Sialoliths are calcified structures that develop within the salivary ductal system. These are usually hard formations and may be round or, oval in shape and may have a variety of sizes. 80- 90% of the salivary gland duct calculi are found in the submandibular gland, 5-10% in the parotid gland and approximately 0-5% in the sublingual and other minor salivary glands. The obstruction can be complete or, partial, and may exhibit recurrence once removed. The incidence of sialolithiasis is shown to peak in the third to sixth decade of life. Submandibular gland sialolithiasis is more common because of the anatomical factors associated with formation of sialoliths in this gland. The Wharton’s duct of the submandibular gland is the longest duct amongst all salivary gland ducts with the path of the duct going in an upward direction (anti-gravity flow). Also, the main portion of the duct is wider than its orifice. Along with these anatomical factors, the submandibular gland saliva is alkaline in nature and rich in mucin, which can promote the formation of a sialolith [1-3]. The aim of this case report is to present a case of sialolithiasis of the submandibular gland in a 21 year old male patient.
Case Presentation
A 21 year old male patient reported to the Department of Oral Medicine and Radiology with a chief complaint of swelling and pain in the region below the tongue on left side since 3 days. Intensity of pain and size of the swelling increased during meals and decreased gradually on its own after an hour. The swelling was, also, associated with pus discharge. He, also, complained of dryness of mouth on left side. There was a history of recurrence of the swelling and occasional pus discharge over the past 6 months for which he used to take medication and the pain and swelling used to get relieved. Patient had difficulty while eating and speaking. He, also, had a history of pan chewing since 3 years. On general examination, patient was conscious and cooperative. Vital signs were within normal limits with the exception of a temperature of 38.9°C (102°F). Submental and submandibular lymph nodes were palpable on left side. Intraorally, there was a solitary, diffuse swelling in the floor of the mouth on left side. It measured 0.6×1.8 cm in dimensions and extended from the lingual frenum to the second premolar region along the course of the Wharton’s duct on left side. The mucosa was red and erythematous with pus discharge from the duct orifice. Wharton’s duct orifice was inflamed and there was an ulcer noted over the swelling anteriorly above the duct orifice (Figure 1). On palpation, the swelling was tender with local rise in temperature. It was firm in consistency with a hard area appreciated along the course of the Wharton’s duct anteriorly close to the duct orifice. On milking, there was pus discharge through the duct orifice. On the basis of history and clinical findings, a provisional diagnosis of recurrent sialadenitis was arrived-at. A true mandibular occlusal radiograph was advised which revealed a solitary homogenous cigar shaped radiopacity measuring approximately 0.4×1.2 cm in dimensions with distinct borders seen mesial to the body of the mandible at premolar region on left side (Figure 2). Based on the above mentioned clinical and radiographic findings, a final diagnosis of recurrent sialadenitis with sialolithiasis of the submandibular gland was given. Patient was put on Tab Amoxycillin-Clavulinic acid 375mg tds, Tab Metrogyl 200mg tds, Tab Paracetamol 200mg tds and chlorhexidine mouthwash for 5 days. A non-surgical management by giving hydration, simultaneous milking of the gland from posterior to anterior direction pushing the calculi towards the orifice, using lemon or, orange drop candy and application of moist heat to the left submandibular region was planned. After 5 days, the patient came with the sialolith expulsed out of the Wharton’s duct orifice with regressed swelling (Figure 3). Clinically, the swelling resolved with no pain. Intra-oral examination demonstrated non-edematous, patent left Wharton’s duct with free flowing saliva. The patient was advised to follow the above mentioned home care instructions for another week. On follow-up examination 1 year later, the patient remained asymptomatic without recurrence of the sialolith.
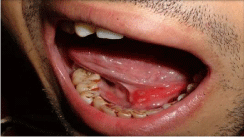
Figure 1: Clinical presentation of sialolith in left Wharton’s duct with an intraoral
swelling along the course of duct and inflamed duct orifice with an ulcer
seen on the mucosa above the duct orifice.
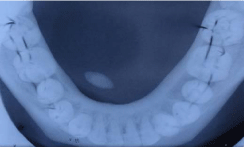
Figure 2: Occlusal radiograph showing a well defined solitary cigar shaped
radiopacity seen on left side.

Figure 3: Sialolith that had spontaneously expulsed out of the duct.
Discussion
The etiology of sialolith formation is still unknown. However, there are several factors that contribute to it. Inflammation, irregularities in the duct system, local irritants, and anti-cholinergic medications may cause pooling of saliva within the duct which is thought to promote stone formation [4]. Clinically, it presents like an acute, painful, and intermittent swelling of the gland, especially during a meal, when the saliva flow is increased. The degree of symptoms is dependent on the extent of salivary ductal obstruction and the presence of secondary infection. The lith may totally or, partially block the flow of saliva, causing salivary pooling within the duct and gland body. The enlargement of the gland consequently causes pain [5]. The involved gland is usually enlarged and tender, pus may be seen draining from the duct and signs of systemic infection may be present. Stasis of the saliva may lead to infection, fibrosis and glandular atrophy. Fistulae, a sinus tract, or, ulceration may occur over the stone in chronic cases. When the secretory capacity is destroyed and normal secretions cannot flush the ducts, a retrograde infection ensues. In these instances, pyogenic infections can result in swelling with acute persistent pain, fever, and malaise. Often, the affected gland and distended ducts become filled with purulent exudates [6]. An examination of the soft tissue surrounding the duct may show a severe inflammatory reaction. Palpation along the pathway of the duct may confirm the presence of the lith. Bacterial infections may or, may not be superimposed and are more common with chronic obstructions. Other complications that may arise from sialoliths are acute sialadenitis, ductal stricture, ductal dilatation, and bacterial infections [7,8]. If the calculus is large, it can be palpated and sometimes even seen at the ductal orifice. Plain film radiography often serves as the initial imaging modality for evaluation of the major salivary glands due to its availability. It is useful particularly for the visualization of the radiopaque sialoliths and the evaluation of bony destruction associated with malignant neoplasms. It can, also, provide a background for interpretation of the sialogram. Sialoliths obstructing the submandibular gland may be visualized by panoramic, occlusal, or, lateral oblique views [9]. In the present, case true occlusal radiograph was taken. Smaller stones or, poorly calcified sialoliths may not be visible on plain films. If a stone is not evident with plain film radiography but clinical evaluation and history are suggestive of salivary gland obstruction, additional imaging (generally accompanied with sialography) might be considered. Sialography is the recommended method for evaluating intrinsic and acquired abnormalities of the ductal system (e.g., ductal stricture, obstruction, dilatation, and ruptures) and for identifying and localizing sialoliths because it provides the clearest visualization of the branching ducts and acinar end pieces. Sialography may, also, be a valuable tool in the pre-surgical planning for removal of salivary masses. Digital subtraction sialography (DSS), whereby the image taken before contrast is injected, is “subtracted” from the image taken after injection, continues to be the standard technique for high-resolution imaging of the extra-glandular and intraglandular salivary ductal system. DSS provides enhanced contrast resolution and therefore, permits the detection of smaller liths. The principle weaknesses of DSS are that it is invasive (since it requires ductal cannulation), uses contrast and ionizing radiation, and has a high incidence of technical failure. Two major contraindications to sialography are active infection and allergy to contrast media [10,11]. Due to the inflammation of the duct and the location of the sialolith in the anterior portion of the duct, sialography was not performed. Ultrasound (US) is widely used as a first-line imaging modality to assess the presence of salivary gland calculi. However, US may not be able to allow for correct assessment of the precise number of calculi where multiple stones are present and calculi less than 2mm may not produce an acoustic shadow [11,12]. Scintigraphy is indicated for the evaluation of patients when sialography is contraindicated or, cannot be performed (i.e., in cases of acute glandular infections or, iodine allergy) or, when the major duct cannot be cannulated successfully. It has, also, been used to aid in the diagnosis of ductal obstruction, sialolithiasis, gland aplasia, Bell’s palsy, and Sjogren’s syndrome (SS) [12,13]. Computed tomography (CT) is the technique of choice for identification of small calculi within the salivary glands or, ducts but at the expense of high radiation exposure. Non-contrast CT images using a slice thickness of 0.2-0.5 mm may be used for the detection of sialoliths and have a 10-fold greater sensitivity than plain film radiography for detecting calcifications. Cone Beam Computed Tomography (CBCT) provides the advantages of reduced superimpositions and distortions of anatomical structures and high sensitivities over two-dimensional radiography and reduced radiation exposure over medical CT. CBCT, also, offers superior imaging of the ductal system over conventional sialography. Magnetic Resonance Imaging (MRI) sialography, although contraindicated in individuals with pacemakers or, claustrophobia, can be used in those with iodine or, contrast media allergies or, acute infections because it does not employ a contrast medium. It, also, does not employ ionizing radiation [14]. Sialendoscopy has emerged as a diagnostic and therapeutic technique for many salivary gland disorders. Its advantages include allowing for access to deeper segments of a duct and potentially the inner areas of the gland and, where feasible, simultaneous visualization and removal of sialoliths. Sialendoscopy may, also, be combined with sialography in the diagnosis and treatment of salivary gland obstructions [15]. During acute phases of sialolithiasis, therapy is primarily supportive. Standard treatment during this phase often involves the use of analgesics, hydration, antibiotics, and antipyretics, as necessary. Sialogogues, massage and moist heat applied to the affected area may, also, be beneficial. Stones at or, near the orifice of the duct can often be removed trans-orally by milking the gland, but deeper stones require intervention with conventional surgery or, sialendoscopy. In this case, increased salivary flow resulted in the expulsion of the stone from the duct orifice as seen in other cases [4,16]. Sialodochoplasty can be performed to remove submandibular sialoliths which are located close to the orifice of Warthin’s duct. Location within the duct determines the type of surgery required for the removal of the stone. If the stone lies in the intra-glandular portion of the duct, it is recommended that the entire gland be removed. For larger sialoliths which are located in the close proximal duct, extracorporeal shock wave lithotripsy (ESWL) can be considered. ESWL is, also, gaining importance because of less damage to the adjacent tissues during procedure [17,18]. Sialendoscopy, which is a noninvasive technique, can be used to manage large sialoliths as well as ductal obliteration. CO2 lasers are, also, gaining popularity in the treatment of sialolithiasis because of their advantages of minimal bleeding, less scarring, clear vision and minimal post-operative complications.
Conclusion
Although various advanced diagnostic and treatment modalities have emerged in the management of sialoliths, the conventional techniques retain their popularity to date. This case of submandibular gland sialolith reported to the Department and was diagnosed clinically and radiographically. In the present case, the patient was instructed to use lemon or, orange drop candy to stimulate salivary flow, and also, to apply moist heat to the left submandibular region. A follow-up appointment was given after 5 days. On the 4th day, the patient felt slight discomfort although after 5 days, it resulted in the expulsion of the stone from the affected salivary gland. This case report demonstrates that non-surgical treatment in resolution of the obstruction may lead to full recovery and normal function of the salivary gland.
References
- Mandel ID, Wotman S. The salivary secretions in health and disease. Oral Sci Rev. 1976; 8: 25-47.
- Haring JI. Diagnosing salivary stones. J Am Dent Assoc. 1991; 122: 75-76.
- Levy DM, Remine WH, Devine KD. Salivary gland calculi. J Am Med Assoc. 1962; 181: 1115-1119.
- Cornell McCullom III, S Cameron, YS Lee, David I Blaustein. Sialolithiasis in an 8-year-old child: Case report. Pediatr Dent. 1991; 13: 231-233.
- Lustman J, Regeve E, Malamed Y. Sialolithiasis: A survey of 245 patients and review of literature. Int J Oral Maxillofac Surg. 1990; 19: 135-138.
- Philip J, Eversole L, Wysocki G. Salivary gland disorders. 1st edition. Contemp Oral Maxillofac Pathol USA: Mosby. 1997; 319.
- Harrison JD. Causes, natural history and incidence of salivary stones and obstructions. Otolaryngol Clin North Am. 2009; 42: 927-947.
- Stanley MW, Bardales RH, Beneke J, Korourian S, Stern SJ. Sialolithiasis: Differential diagnostic problems in fine-needle aspiration cytology. Am J Clin Pathol. 1996; 106: 229-233.
- Greenberg, Glick, Ship. Burket’s Oral Medicine. Diagnosis and treatment. 10th edition. 1992; 238-246.
- Del Balso A. Salivary imaging. Oral Maxillofac Surg Clin North Am. 1995; 7: 387-422.
- Murray ME, Buckenham TM, Joseph AEA. The role of ultrasound in screening patients referred for Sialography: A possible protocol. Clin Otolaryngol. 1996; 21: 21-23.
- Weber AL. Imaging of the salivary glands. Curr Opin Radiol. 1992; 4: 117-122.
- Umehara I, Yamada I, Murata Y. Quantitative evaluation of salivary gland scintigraphy in Sjogren’s syndrome. J Nucl Med. 1999; 40: 64-69.
- CasselmanJW, Mancuso AA. Major salivary gland masses: Comparison of MR imaging and CT. Radiol. 1987; 165: 183-189.
- Nahlieli O, Baruchin AM. Sialoendoscopy: Three years experience as a diagnostic and treatment modality. J Oral Maxillofac Surg. 1997; 55: 912-918.
- Marwaha M, Nanda KS. Sialolithiasis in a 10 year old child. Indian J Dent Res. 2012; 23: 546-549.
- Iro H, Zenk J, Benzel W. Laser lithotripsy of salivary duct stones. Adv Otolaryngol. 1995; 49: 148-152.
- Aidan P, de Kerviler E, Le Duc A, Monteil JP. Treatment of salivary stones by extra-corporeal lithotripsy. Am J Otolaryngol. 1996; 17: 246-250.