
Case Presentation
J Dent App. 2016; 3(4): 361-364.
Full Mouth Rehabilitation of Localized Aggressive Periodontitis: A Case Report of 36 Months Follow-Up
Polepalle T¹, Chaitanya A¹, Firoz Babu P², Boggarapu S¹ and Nayyar AS³*
¹Department of Periodontics and Implantology, Sibar Institute of Dental Sciences, Guntur, Andhra Pradesh, India
²Department of Orthodontics and Dentofacial Orthopedics, Rama Dental College and Hospital, Kanpur, Uttar Pradesh, India
³Department of Oral Medicine and Radiology, Saraswati- Dhanwantari Dental College and Hospital and Post- Graduate Research Institute, Parbhani, Maharashtra, India
*Corresponding author: Abhishek Singh Nayyar, 44, Behind Singla Nursing Home, New Friends’ Colony, Zodel Town, Panipat-132 103, Haryana, India
Received: December 02, 2016; Accepted: December 29, 2016; Published: December 30, 2016
Abstract
Localized Aggressive Periodontitis is characterized by deep vertical osseous defects that affect molars and incisors. This case report is of a 35 years male patient diagnosed with localized aggressive periodontitis with intrabony defects. Regeneration of intra-bony defects was carried-out with use of composite grafts [(FDBA, Biograft HA, Osseograft, Sybograft, Autogenous graft) + Gengigel]. After 6 months, all grafts showed radiographic bone fill but at 36 months, FDBA, Osseograft along with Gengigel showed better radiographic bone fill than the other composite grafts. Buccal bone augmentation was done in 12 regions to receive prosthesis. Thus, full mouth rehabilitation was achieved.
Keywords: Localized Aggressive Periodontitis; Regeneration; Bone grafts; Buccal ridge augmentation
Introduction
Regeneration of lost tissues to its pre-disease state is the desired goal for clinicians in periodontitis. Various procedures like open flap debridement alone or, combined with bone grafts and GTR are employed to accomplish the ultimate goal of periodontal therapy [1]. Autogenous graft is an ideal graft material for regeneration but its major disadvantage is that it requires a second surgical site to procure the graft tissue [2]. FDBA is a mineralized bone graft which promotes regeneration by osteoconduction and is suitable for space maintenance [3]. Xenografts are the alternatives but because of the risk of immunogenic reactions and rejection by host tissue, they are not as successful as autografts [4]. Alloplastic materials are used as fillers and as scaffolds and are biocompatible. BioGraft HA is a composite bioactive material for periodontal osseous defect reconstructions and regeneration. The particle size of Biograft HA is 150-700 μ with an internal pore size of 100-200 μ, used specifically, for periodontal applications [5]. Nano-crystalline hydroxyapatite (NcHA) bone graft was introduced commercially as Sybograft. The advantages are osteoconductivity, bioresorbability and the presence of high number of molecules on the surface [6]. Hyaluronic acid (hyaluronan) is a widely distributed glycosaminoglycan in the extracellular matrix of mammalian connective tissues. Gengigel contains Hyaluronic acid in 0.8% concentration in gel formulation and is suitable for bone regeneration [7]. In the present case report, we tried to explore the beneficial effects of composite grafts [(FDBA, Biograft HA, Osseograft, Sybograft, Autogenous graft) + Gengigel] in intra-bony osseous defects.
Case Presentation
A 35 years old male patient reported with the chief complaint of deposits on teeth. On clinical examination, patient was diagnosed with localized aggressive periodontitis based on the clinical and radiographic features. Clinical parameters were recorded pre- operatively and after 6, 12, 24 and 36 months by a trained examiner. The pocket probing depth (PD) and clinical attachment level (CAL) were recorded to the nearest millimeter with a UNC-15 probe (Hu- Friedy probe) at the deepest point of the periodontal pocket. In radiographic examination, an orthopantomograph (OPG) was used to evaluate the radiographic level of bone wherein deep intra-bony defects were observed in the molar and incisal regions (Figure 1 and 2).
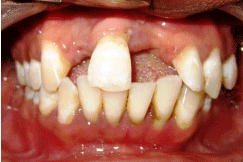
Figure 1: Pre-operative view.
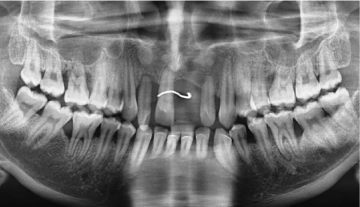
Figure 2: Pre-operative orthopantomograph (OPG).
Surgical procedure
Phase I therapy of scaling and root planning was done. Phase II therapy proceeded with an open flap debridement followed by regeneration of the intra-bony defects. Local anesthesia with 2% lignocaine was achieved followed by buccal and then, palatal/ lingual crevicular incisions using surgical blade no.15. Full thickness mucoperiosteal flap was elevated and after meticulous debridement of the defect, composite graft with Gengigel was placed up to the vertical height of corresponding adjacent bone level as follows:
- In first quadrant: FDBA + Biograft HA;
- In second quadrant: Osseograft + Biograft HA;
- In third quadrant: Sybograft + Autogenous graft; while
- In fourth quadrant: Sybograft + Biograft HA
The above respective composite grafts were used along with Gengigel and surgical flaps were repositioned using 3-0 silk. Postoperative instructions were provided followed by antibiotics and analgesics which were prescribed for 5 days and the patient was discharged with a recall after 1 week for suture removal (Figure 3 and 4). Buccal ridge augmentation was done to place prosthesis that would exhibit primary stability in 12 region. In the recipient site, a midcrestal incision in the keratinized tissue followed by two vertical relieving incisions was given and full thickness mucoperiosteal flap was elevated. Buccal cortical deficiency was measured as 4x3mm and with the help of BS-2R piezo bone cutting bur under copious saline irrigation, the measured buccal cortical bone was procured from the symphysis region. The procured bone was placed in the recipient site and stabilized with titanium screws. The recipient and donor sites were subsequently sutured. The clinical and radiographic parameters were recorded after 6, 12, 24 and 36 months (Figure 5-7).
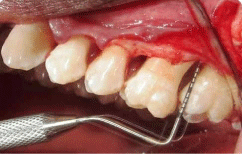
Figure 3: Pre-operative probing depth.
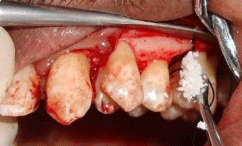
Figure 4: Placement of composite graft.
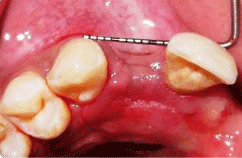
Figure 5: Pre-operative site for buccal ridge augmentation.
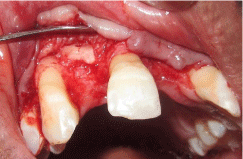
Figure 6: Procured autogenous bone graft placed in the recipient site.
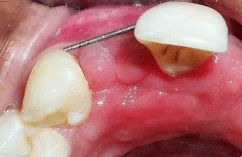
Figure 7: Post-operative site for ridge augmentation.
Results
Pre-operatively, the mean probing depth was found to be 10mm while after 6 months, the clinical probing depth was measured at 3mm in all the defect sites. First and second quadrants showed 3mm after 12, 24 and 36 months whereas third and fourth quadrants showed a mean probing depth of 4.5mm at 36 months. On radiographic examination, the bone fill was found to be more in the first and second quadrants post-operatively than in third and fourth quadrants. The bone buccolingual dimension of the alveolar ridge was increased by 2mm (Figure 8-10).
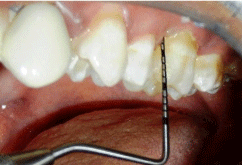
Figure 8: Post-operative probing depth.
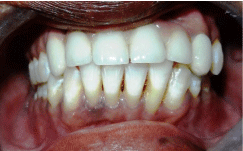
Figure 9: Post-operative view after 36 months.
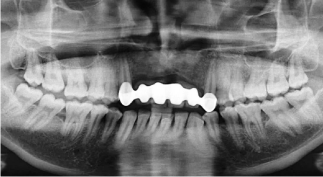
Figure 10: Post-operative orthopantomograph (OPG) after 36 months.
Discussion
The aim of periodontal treatment is to induce bone regeneration in intra-bony defects. The present case report suggests that smaller particle size of FDBA (100-300 μm) provided better bone fill of 2mm at 36 months follow-up and showed better clinical outcome in the form of reduced probing depth (baseline 10mm to 3mm at 36 months follow-up post-operatively). According to Rivault AF et al, FDBA (100-300 μm) was better compared to the larger particle size of FDBA (1000-2000 μm) than using DFDBA [8]. Mabry TW et al stated FDBA showed reduced probing depth [9]. Osseograft is a xenograft of demineralized bone matrix with a particle size is of 250μm and is replaced by host bone within 4-24 weeks. In the present case report, there was observed a bone fill within 24 weeks as osseograft contains type 1 collagen and is made from bovine cortical samples.
The probing depth (PD) reduced to 3mm at 6 months and the same result was sustained at 36 months. Sonis ST et al evaluated the efficacy of demineralized bone in periodontal defects and stated that there was a radiographic bone fill of 60% at 6 months [10]. The present case report identified good bone fill, evidenced radiographically, with use of composite grafts (FDBA + Biograft HA + Gengigel) and (Osseograft + Biograft HA + Gengigel) which provided improvement in clinical and radiographic parameters when reviewed in a 36 months postoperative follow-up superior to other composite grafts. Zybutz M et al compared clinical and radiographic measurements of vertical defects using Biograft HA and concluded that there was greater radiographic bone fill after 12 months [11]. Sybograft in this case report revealed that there was a bone fill of 1.5mm after 36 months. Kasaj A et al evaluated the clinical efficacy of Nano-crystalline hydroxyapatite (NcHA) in intra-bony defects [12]. Autogenous bone grafts provide a reliable treatment modality for the reconstruction of bone defects for aesthetic and functional results in the treatment of intra-bony defects [13]. The bone scrapings from the adjacent site were taken and placed in the bone defect area in the present case. The results revealed that there was a bone fill of 2mm after 36 months. Gengigel was placed in all the bone defects along with other bone grafts to provide additional bone formation. Fawzy El-Sayed KM et al, in a randomized controlled trial, evaluated the efficacy of Gengigel which contains Hyaluronic acid in 0.8% concentration in gel formulation in conjunct with periodontal surgical procedures and noted statistically significant differences in clinical attachment level (CAL) [14]. The hard tissue augmentation achieved with buccal ridge augmentation improved esthetic and functional demands in areas where hard and soft tissue defects were present. This case report presented a useful treatment for correcting the buccal volume of hard tissue in 12 regions to receive prosthesis. Thus, the buccal ridge augmentation with autogenous bone graft allowed improvement in the hard tissue contours and emergence profile [15]. As the present case is an ideal case for vertical defects, different bone grafts in combination with hyaluronan gel were used to know their efficacy in bone formation. The limitation of the present case report is that the patient was unwilling for implant placement, so, fixed prosthesis was given in the ridge augmented area.
Conclusion
This case report revealed that treatment with composite grafts (FDBA + Biograft HA + Gengigel) and (Osseograft + Biograft HA + Gengigel) provided improvement in clinical and radiographic parameters when reviewed in a 36 months post-operative follow-up superior to other composite grafts.
References
- Gupta G. Clinical and radiographic evaluation of intra bony defects in localized aggressive periodontitis patients with platelet rich plasma/hydroxyapatitegraft: A comparative controlled clinical trial. Contemp Clin Dent. 2014; 5: 445-451.
- Nabers CL, O’Leary TJ. Autogenous bone transplant in the treatment of osseous defects. J Periodontol. 1965; 36: 5-14.
- Schallhorn RG, Hiatt WH. Human allografts of iliac cancellous bone and marrow in periodontal osseous defects. Part II. Clinical observations. J Periodontol. 1972; 43: 67-81.
- Scoop IW, Morgan FH, Dooner JJ. Bovine bone (Boplant) implants for infra-bony oral lesions (clinical trials in humans). Periodontics. 1966; 4: 169-178.
- Debnath T, Chakraborty A, Kanti Pal T. A clinical study on the efficacy of hydroxyapatite: Bioactive glass composite granules in the management of periodontal bony defects. J Indian Soc Periodontol. 2014; 5: 593-600.
- Chris Arts JJ, Verdonschot N, Schreurs BW, Buma P. The use of a bio-resorbable nano-crystalline hydroxyapatite paste in acetabular bone impaction grafting. Biomaterials. 2006; 27: 1110-1118.
- Bansal J, Kedige SD, Anand S. Hyaluronic acid: A promising mediator for periodontal regeneration. Indian J Dent Res. 2010; 21: 575-578.
- Rivault AF, Toto PD, Levy S, Gargiulo A. Autogenous bone grafts, osseous coagulum and osseous retrograde procedures in primates. J Periodontol. 1972; 42: 787-794.
- Mabry TW, Yukna RA, Sepe WW. Freeze dried bone allografts combined with tetracycline in the treatment of juvenile periodontitis. J Periodontol. 1985; 56: 74-81.
- Sonis ST, Kaban LB, Glowacki J. Clinical trial of demineralized bone powder in the treatment of periodontal defects. J Oral Med. 1983; 38: 117-122.
- Zybutz M, Rapoport D, Laurell L, Persson GR. Comparisons of clinical and radiographic measurements of interproximal vertical defects before and 1-year after surgical treatments. J Clin Periodontol. 2000; 27: 179-186.
- Kasaj A, Rohrig B, Zafiropoulos GG, Willershausen B. Clinical evaluation of nanocrystalline hydroxyapatite paste in the treatment of human periodontal bony defects: A randomized controlled clinical trial: 6-month results. J Periodontol. 2008; 79: 394-400.
- Miranda T. Connective tissue graft combined with autogenous bone graft in the treatment of peri-implant soft and hard tissue defect. Quint Int. 2015; 46: 139-144.
- Fawzy El-Sayed KM, Dahaba MA, Aboul-Ela S, Darhous MS. Local application of hyaluronan gel in conjunction with periodontal surgery: A randomized controlled trial. Clin Oral Investig. 2012; 16: 1229-1236.
- Fugazzotto P. Report of 302 Consecutive Ridge Augmentation Procedures: Technical Considerations and Clinical Results. Int J Oral Maxillofac Implants. 1998; 13: 358-368.