
Case Report
J Dent App. 2017; 4(1): 385-388.
Early Interception of Digit-Sucking Habit Using Maxillary Expansion and a Palatal Crib
Machado AW¹* and Fonseca LM²
1Associate Professor, Section of Orthodontics, Federal University of Bahia; Visiting Professor, Section of Orthodontics, University of California, Los Angeles, USA
2Specialist in Orthodontics, UFBa, Visiting Professor of Orthodontics at the University of Brasilia, Brazil
*Corresponding author: Andre Wilson Machado, Associate Professor, Section of Orthodontics, Federal University of Bahia; Visiting Professor, Section of Orthodontics, University of California, Los Angeles, USA
Received: September 12, 2017; Accepted: October 05, 2017; Published: October 12, 2017
Abstract
Non-nutritive digital sucking is a deleterious habit that interferes with normal occlusion development and constitutes a common etiologic agent in anterior open bite and posterior crossbite. Given that these malocclusions also harm patients in additional ways, early intervention and correction are of paramount importance. This study aimed to report a clinical case which presented these malocclusions in combination with digit-sucking habit. The latter was successfully treated through maxillary expansion and a palatal crib. Finally, the study emphasizes that dentists, especially pediatric dentists and orthodontists, should diagnose and help patients break this habit as early as possible to avert negative effects in the development of occlusion.
Keywords: Sucking habit; Maxillary expansion; Early interception
Introduction
In its first year an infant’s nutrition is provided by means of breastfeeding performed through mandibular movements and suction, which ensures proper growth and development of the jaws [1]. Furthermore, when the sucking habit does not involve feeding it is called a non-nutritive sucking habit (NNSH).
Habit onset may occur prematurely - as early as intrauterine life - and may persist throughout childhood and, in extreme situations, even into adulthood. It often manifests itself by the patient sucking on a pacifier or a finger, predominantly the thumb. Although the literature does not consider as harmful the presence of this habit during primary dentition, but only when it persists throughout permanent1 or mixed dentition, recent studies show that when NNSH is present after 2 years of age the likelihood of developing malocclusions is increased [2].
Malocclusions caused by NNSH are characterized by diastema, flaring of maxillary incisors, retroclination of lower incisors, posterior crossbite and anterior open bite [3,4]. Moreover, anterior open bite tends to self-correct when the habit is dropped [5,6] while the same is not true of posterior crossbite [3].
These findings underscore the need to intervene as early as possible in NNSHs and maxillary atresia, thus allowing a normal development of occlusion. Given that these malocclusions can occur concurrently with NNSH, the aim of this article is to present the clinical case of a patient who had a finger-sucking habit, mixed dentition, with posterior crossbite and anterior open bite. Treatment consisted in the use of a modified Haas rapid maxillary expansion appliance combined with a palatal crib.
Clinical Case Report
Female patient, 7 years and 3 months old, whose presenting complaint was that “my front teeth are open”. Their parents/ legal guardians reported that the she had a finger-sucking habit. Her medical history showed no contraindication to orthodontic treatment.
The analysis showed facial symmetry within normal limits, vertical facial pattern and straight facial profile. An intraoral evaluation revealed that the patient was in the mixed dentition stage, had a Class I malocclusion associated with posterior crossbite and anterior open bite. In front view the presence of a median diastema was observed, associated with an enlarged labial frenum. After a clinical evaluation, the primary etiological factor associated with the malocclusion was found to be a digit-sucking habit. Furthermore, due to the anterior open bite, the patient began to develop anterior tongue thrust at rest and swallowing (Figure 1).
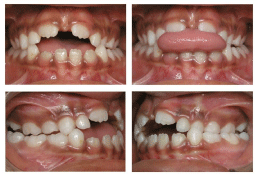
Figure 1: Initial intraoral photographs.
Interceptive treatment planning was conducted. Its key aim was to clarify matters for the patient and their legal guardians regarding the harmful effects of NNSH as well as the need to break such habits to restore normal occlusion development. A modified Haas rapid maxillary expansion appliance was then combined with a fixed palatal crib. Initially, the appliance was put in place and kept idle for 4 weeks to wait for the inhibitory effect of the habit while allowing the patient to adapt to it. Thereafter, the parents were instructed to activate the screw by 2/4 of a turn twice a day. After 7 days of activation the posterior crossbite was corrected. The appliance however was maintained for another 6 months as a retainer to ensure that the results once achieved would be preserved, as well as to preserve the effects of the palatal crib in controlling the NNSH and tongue thrust (Figure 2).
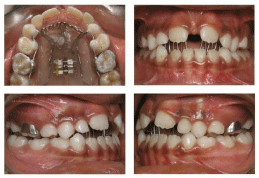
Figure 2: Pre-treatment intra oral photographs with appliance.
After the retention period, the habit had been altogether broken and the transverse and vertical dental relations were within normal limits. At that time, it was noted that due to the presence of a median diastema associated with the enlarged frenum there was not enough space for the physiological eruption of the maxillary lateral incisors (Figure 3A-3C). Thus, brackets were bonded to the maxillary central incisors to close the diastema thereby creating space for the eruption of the laterals (Figure 3D). After 3 months, the diastema was closed, the brackets were kept for retention and periodic appointments were scheduled. Three months later the lateral incisors erupted physiologically, the orthodontic brackets were debonded and an orthodontic wire was bonded to the palatal surface of the upper centrals to function as a retainer.
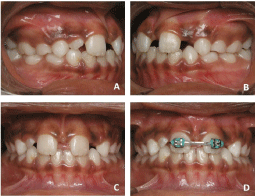
Figure 3: Six months retention (A-C) with brackets placed (D).
Eighteen months after treatment completion (Figure 4) the transverse and vertical relationships were within normal limits, and the patient was referred for evaluation of possible surgical treatment of the enlarged labial frenum. Thirty nine months after backets removal, arches width and incisors overbite were stable (Figure 5).
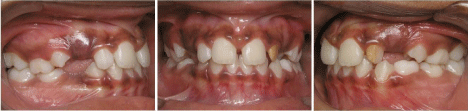
Figure 4: Intraoral photos 18 months after brackets removal.
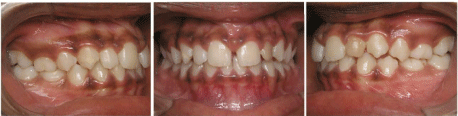
Figure 5: Intraoral photos 39 months after brackets removal.
Discussion
There is a general consensus in the literature regarding an association between non-nutritive sucking habits (NNSHs) and the etiology of malocclusions - specifically anterior open bite and posterior crossbite – which is corroborated by the clinical case presented in this article [3,4,7].
Although these habits are prevalent in infants and considered normal until two years of age, after this period they may play a role in dentofacial changes. The correlation between NNSHs and the development of malocclusions depends on the combination of three factors: a) The frequency with which the patient cultivates the habit, b) Habit duration as well as how intensely the patient sucks on his/ her finger(s) [3,8].
According to the literature, NNSHs are harder to break than the use of a pacifier [3], which is understandable given that fingers are conveniently accessible to the patient, but not to his/her parents. Furthermore, children who have both types of NNSH are 6 times more likely to develop a malocclusion when compared with those who do not have an NNSH [2,5].
Treatment should therefore be performed at an early stage of development, and with effective patient compliance, thereby preventing dentoalveolar changes from evolving into permanent skeletal deformities, which are difficult to treat. Failure to correct posterior crossbite at an early stage may increase the risk of developing facial and skeletal [9,10] asymmetries, as well as cause important muscle changes [11]. Moreover, some children with open bite associated with an NNSH undergo self-correction after removal of the habit [6].
One point of disagreement on the effects of palate-splitting appliances refers to mandibular rotation, which could be in a counterclockwise direction, favoring the correction of open bite [12], or a clockwise direction, opening the mandibular plane and compromising overbite correction [13], which should be considered in cases with a hyperdivergent face.
In the case presented in this paper, the primary etiological factor of the malocclusion was the presence of a thumb-sucking habit. In these situations the therapeutic approach aims not only to break the habit but also to correct dentoalveolar changes resulting from the habit.
NNSHs can be difficult to abandon [3,6], and children often need help. Several techniques can be used to help them break the habit. Parents and children should be made aware of the habit and its harmful effects; reward techniques should be applied; nail varnish or other substances with a nasty taste [14] should be used. Such approaches seek to educate the patient or reduce any pleasure they may derive from the NNSH. Once they are made aware of the issue and a psychological approach is adopted, the malocclusion should be orthodontically corrected. In many clinical situations braces can be used not only to correct the malocclusion but also to assist the patient in controlling the habit.
The literature suggests different appliances for these purposes such as upper removable plates, removable or fixed palatal crib, and spurs [15-18]. Besides these, other appliances used to correct posterior crossbite also play an important role in controlling the habit, such as Porter Arch, quad-helix, Haas and Hyrax expanders, removable expanders, as well as a combination of these [16-18]. Appliance selection should be made based on habit severity, type of malocclusion, degree of patient compliance, comfort and predictability provided by the appliance, the clinical experience of the pediatric dentist or orthodontist, and the time required to solve the problem. Moreover, fixed appliances are more efficient than removable appliances while achieving similar clinical results in half the treatment time [19].
The case described in this article was in the mixed dentition phase and already showed some occlusal changes in the vertical and transverse directions. The initial interception aimed to educate patients about the importance of breaking the habit. This approach is vital if one is to boost the chances of achieving better results through patient cooperation.
After this stage, a modified Haas palatal expansion appliance was placed to correct the posterior crossbite. A palatal crib was incorporated into the expander, which according to the literature plays different roles: (1) It constantly reminds the child about the need to break the habit, (2) It works as a retainer preventing tongue thrust at rest and swallowing, and (3) It is a mechanical resource for rapid maxillary expansion and consequently posterior crossbite correction [1,8,20,21].
In some clinical situations relapse of anterior open bite occurs and is often due to negligence when diagnosing the etiology of the malocclusion. Moreover, improper tongue posture at rest is the key etiological factor behind this relapse [22]. Changing the tongue posture therefore enhances treatment stability. It is also recommended that any devices used to retrain the tongue be held in place from 6 months to 1 year for retention [1,23] since according to the literature the motor response must be altered and new stretch reflexes created [1,22,23-25]. Therefore, in the case described in this article the lingual grid was maintained, thus maximizing result stability while corroborating other findings in the literature [23-25].
Conclusion
Finger-sucking habits exert a deleterious impact on the normal development of occlusion and if not intercepted in the early stages of development can produce negative skeletal and dental effects. As a result, diagnosis and intervention - as early as mixed dentition - are essential if one is to achieve good clinical results. It is noteworthy that the modified Haas expander used in this case proved a versatile appliance which can be adapted to correct transverse problems as well as assist in the interception of oral habits, thereby correcting anterior open bites.
References
- Profit WR, Fields JR, HW, Sarver DM. Contemporary Orthodontics. Fourth edition. St. Louis, Mosby Elsevier. 2006.
- Góis EGO, Ribeiro-Júnior HC, Vale MPP, Paiva SM, Serra-Negra JMC, Ramos-Jorge ML, et al. Influence of Nonnutritive Sucking Habits, Breathing Pattern and Adenoid Size on the Development of Malocclusion. Angle Orthodontist. 2008; 78: 647-654.
- Duncan K, McNamara C, Ireland AJ, Sandy JR. Sucking habits in childhood and the effects on the primary dentition: findings of the Avon Longitudinal Study of Pregnancy and Childhood. Inter J Paediatric Dent. 2008; 18: 178– 188.
- Singh SP, Utreja A, Chawla HS. Distribution of malocclusion types among thumb suckers seeking orthodontic treatment. J Indian Soc Pedod Prevent Dentistry–Supplement. 2008; 26: S114-S117.
- Heimer MV, Katz CRT, Rosenblatt A. Anterior open bite: a case–control study. Inter J of Paediatr Dent. 2010; 20: 59–64.
- Katz CRT, Rosenblatt A. Nonnutritive Sucking Habits and Anterior Open Bite in Brazilian Children: A Longitudinal Study. Pediatr Dent. 2005; 27: 369-373.
- Heimer MV, Katz, CRT, Rosenblatt A. Non-nutritive sucking habits, dental malocclusions, and facial morphology in Brazilian children: a longitudinal study. Eur J of Orthod. 2008; 30: 580–585.
- Graber TM, Vanarsdall RL. Orthodontics: Principles and practice. 2nd edition. Philadelphia. W.B.Sounders Company. 1966.
- Kilic N, Kiki A, Oktay H. Condylar asymmetry in unilateral posterior crossbite patients. Am J Orthod Dentofacial Orthop. 2008; 133: 382-387.
- Primozic J, Ovesenik M, Richmond S, Kau CH, Zhurov A. Early cross bite correction: a three-dimensional evaluation. Eur J Orthod. 2009; 32: 352-356.
- Alarcón JA, Martín C, Palma JC. Effect of unilateral posterior crossbite on the electromyographic activity of human masticatory muscles. Am J Orthod Dentofacial Orthop. 2000; 118: 328-334.
- Sankey WL, Buschang PH, English J, Owen AH. Early treatment of vertical skeletal dysplasia: The hiperdivergent phenotype. Am J Orthod and Dentofacial Orthop. 2000; 118: 317-327.
- Chung CH, Font B. Skeletal and dental changes in the sagittal, vertical, and transverse dimensions after rapid palatal expansion. Am J Orthod and Dentofacial Orthop. 2004; 126: 569-575.
- Patel A, Moles D, O’Neil J, Noar J. Digit sucking in children resident in Kettering (UK). J Orthod. 2008; 35: 255–261.
- Greenleaf S, Mink J. A retrospective study of the use of the bluegrass appliance in the cessation of thumb habits. Pediatric Dent. 2003; 25: 587-590.
- Giuntini V, Franchi L, Baccetti T, Mucedero M, Cozza P. Dento skeletal changes associates with fixed and removable appliances with a crib in openbite patients in the mixed dentition. Am J Orthod and Dentofacial Orthop. 2008; 133: 77-80.
- Kulkami GV, Lau D. A single appliance for the correction of digit-sucking, tongue-thust, and posterior crossbite. Pediatric Dent. 2010; 30: 61-63.
- Cozza P, Baccetti T, Franchi L, McNamara Jr JA. Treatment effects of a modified quad-helix in patients with dento skeletal open bites. Am J Orthod Dentofacial Orthop. 2006; 129: 734-739.
- Erdinç AE, Ugur T, Erbay EA. Comparison of different treatment techniques for posterior crossbite in mixed dentition. Am J Orthod Dentofac Orthop. 1999; 116: 287-300.
- Machado AW, Vianna AP, Ambrósio AR, Gandini Jr LG. Aparelho expansor Haas com molas digitais para correção da mordida cruzada anterior e posterior. Rev Clin Ortod Dental Press. 2011; 10: 60-67.
- Moyers R.E. Ortodontia. Fourth edition. Michigan. Year book medical publishers. 1988.
- Huang G, Justus R, Kennedy DB, Kokich VG. Stability of anterior open bite treated with crib therapy. Angle Orthodontics. 1990; 60: 17-24.
- Justus R. Treatment of anterior open bite: a cephalometric and clinical study. ADM. 1976; 33: 17-40.
- Nascimento MHA, Araújo TM, Machado AW. Severe anterior open bite during transitional dentition treated with palatal spurs. J Clin Ped Dent. 2016; 40: 247-250.
- Primozic J, Ovesenik M, Richmond S, Kau C.H, Zhurov A. Early crossbite correction: a three-dimensional evaluation. Eur J Orthod. 2009; 32: 352-356.