
Case Report
J Dent & Oral Disord. 2017; 3(2): 1060.
Oral and Masticatory Rehabilitation Using Osseointegrated Dental Implants After Resective Treatment of Multicystic Ameloblastoma in the Lower Jaw with a Fibula Graft – A Case Report
Deliberador TM¹, Grossi JRA¹*, Saad T¹, Scariot R², Zielak JC¹ and Giovanini AF³
¹Department of Implanthology, Positivo University, Brazil
²Department of Head and Neck Surgery, Positivo University, Brazil
³Department of Pathology, Positivo University, Brazil
*Corresponding author: Joo Ricardo Almeida Grossi, Department of Implanthology, Positivo University, Brazil
Received: March 03, 2017; Accepted: May 03, 2017; Published: May 10, 2017
Abstract
Aim: Ameloblastoma is an aggressive odontogenic tumor which typically occurs between third and fourth decade of life, that often needs resective approach. Immediate reconstruction may show better results.
Methods: The treatment of multicysticameloblastoma in the mandible, being a rare case that occurred in the late second decade of life, which was surgically removed along with the affected teeth with safety margins and the region was immediately reconstructed using a vascularized graft, removed from the fibula.
Results: Its integration, in combination with osseointegrated dental implants and fixed implant-supported prostheses, restored chewing function and aesthetics.
Conclusion: After 7 years from fibular graft and 36 months of dental implants, an excellent outcome was observed, with oral health and normal functions properly restored and the immediate reconstruction of the mandible in resective cases, associated with oral rehabilitation with dental implants, may be considered a suitable treatment option.
Keywords: Ameloblastoma; Bone Graft; Dental Implants; Prosthetic rehabilitation; Immediate fibulae reconstruction
Introduction
Ameloblastoma represents approximately 10% of odontogenic epithelial tumors [1-4] the second most prevalent neoplasm after odontomas [5], accounting for 1% of all tumors and jaw cysts that predominantly affect the mandible [2,4,6,7], in the body of the mandible and its ascending branch [2], characterized by asymptomatic slow expansion with persistent and aggressive behavior, capable of infiltrating adjacent tissues, causing cortical bone expansion, and severe facial deformities, functional impairment, paresthesia, and trismus [2,6,8]. In addition, it may induce root resorption and high rates of relapse when inadequately treated [1,8].
Ameloblastomas are classified into different types: solid or multicystic, unicystic, desmoplastic, peripheral or soft tissue [2,4,5,9], and malignant, which is the most aggressive type [2,7].
Diagnosis is achieved through radiographic examination or when the tumor leads to facial asymmetry. Radiographically, ameloblastoma shows significantly variation, but multilocular and unilocular characteristics are commonly seen, which may or may not be well defined [2], appearing as “honeycomb” or “soap bubbles” [6].
The recommended treatment for ameloblastoma relies on a surgical approach, andradical surgical treatment involves resection of the ameloblastoma with safety margins of at least 1 to 3 cm of normal bone [1,2,5,9,10]. Conservative surgery involves total tumor enucleation and subsequent curettage; however, this method leads to an increased rate of relapse, usually occurring a few years following conservative treatment [1,2,4,5,9].
These tumors usually develop between the third and the fourth decades of life [1,2,4,8]. In young patients, unicysticameloblastomas are rare and their resections may interrupts the growth and development of the anatomical structures affected by these tumors [3]. Moreover, these tumors can lead to functional and aesthetic problems, including chewing difficulties, which may benefit from more conservative treatment [5].
The aim of this study was to report a clinical case of oral rehabilitation with dental implants and fixed prostheses, after the resective treatment of a multicysticameloblastoma associated with immediate micro vascularized fibular grafting.
Case Presentation
The patient was diagnosed with endodontic periapical cyst with chronic inflammation in lower right pre-molars at 18 years of age (Figure 1), during a follow-up Rx examination at the end of orthodontic treatment and revealed the presence of a radiolucent circumscribed lesion located in the right side of the body of the mandible, with no cortical bone expansion or dental displacement.
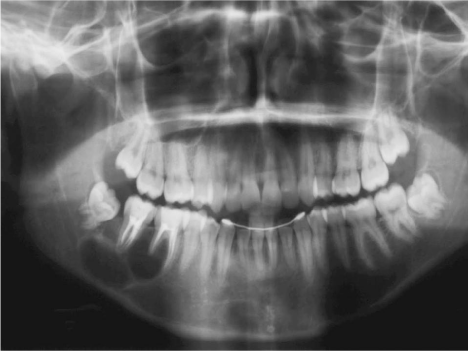
Figure 1: Initial Panoramic radiography.
For initial histopathological examination, a biopsy of the region with intra-oral bone curettage was performed and monitoring for 3 years, the patient presented with tumor relapse, which required surgical removal.
The tumor recurred, with pain and swelling that affected the body of the mandible and its ascending ramus. An irregular fragment of bone tissue was resected for a new histopathological examination (Figure 2), new imaging exams, including bone densitometry and panoramic radiography, which confirmed the diagnosis of multicysticameloblastoma.
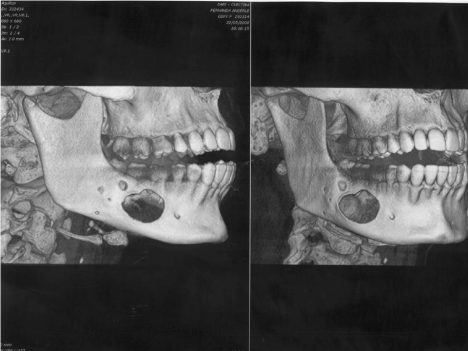
Figure 2: Computerized Tomograph 3D before fragment of bone tissue was
resected.
The patient underwent a resective hemimandibulectomy, in which five teeth adjacent to the tumor were removed and an autogenous micro vascularized fibula graft was simultaneously performed, being fixed at the remaining stumps of the jaw using plates and screws typically used in this type of surgery (Figure 3).
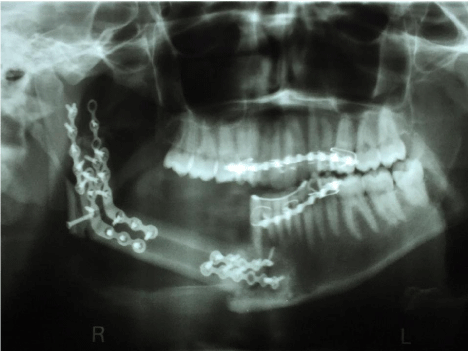
Figure 3: Panoramic radiograph withplates and screws used before resective
surgery.
A minimum follow-up of 12 months, for the incorporation and maturation of the graft, The post-surgical evolution, incorporation, and maturation of the fibular graft occurred without complications and the region appeared completely healthy, with no signs of tumor recurrence or inflammation (Figure 4). This indicated that the procedure is feasible for the reconstruction of this region with dental implants,however, the patient decided not to install the dental implants within the stipulated period.
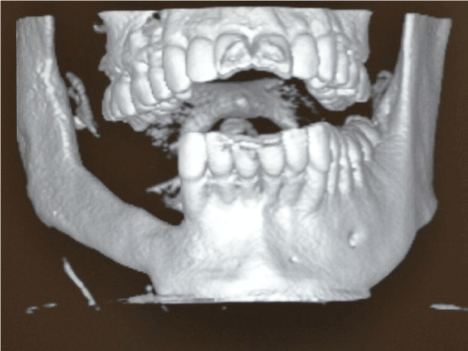
Figure 4: Computerized Tomograph 3D after implant surgery and before
removed the plates and screws.
Five years after tumor removal and the incorporation of the fibular graft, the patient began to notice the effect of partial edentulism in the right mandibular region, and the upper teeth appeared uneven. The installation of three dental implants was then planned, since the patient did not present any systemic problems.
For the surgical procedure, extra and intraoral antisepsis was achieved using 0.12% chlorhexidine and local anesthetic infiltration administered with 4% articaine hydrochloride. Total detachment of the flap was performed using a Molt periosteal elevator (Figure 5).
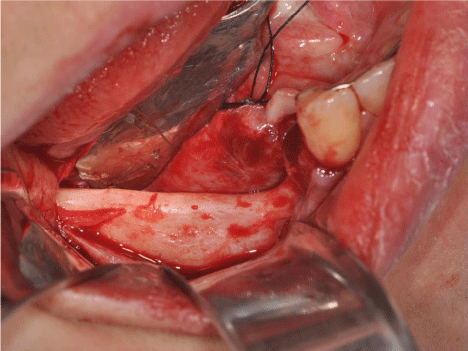
Figure 5: Fibulae graft area exposed before implant placement.
Three implants were installedfollowing the manufactor protocol an external hexagon platform 4.1-mm high, 3.75-mm thick, and 8.5- mm long was placed in the region corresponding to teeth 44, 46, and 47, and modified continuous suture technique with nylon thread 5-0 (Figure 6).
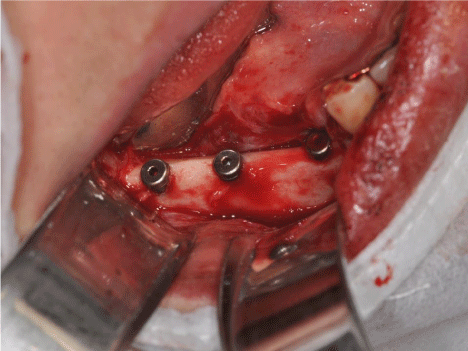
Figure 6: Implants with cover screws placed on fibulae graft.
Was prescribed 500 mg Amoxicillin every 8 h for 7 days, 400 mg Etodolac every 8 h for 3 days, and 750 mg Paracetamol every 8 h for 2 days, and mouthwashes with a solution of chlorhexidine digluconate without alcohol every 12 h for 14 days, and the sutures were removed after 10 days, and the patient was monitored monthly.
A minimum period of 90 days to allow time for osseointegration before reopening the implants and subsequent oral rehabilitation with implant-supported prostheses with an bone crest incision for the installation of healing abutments under 4% articaine hydrochloride local anesthesia, and suturing using a single circumferential suture with wire 4-0.
Dental moldings were obtained for fabrication of the implantsupported prostheses after 3 weeks, showing to the difference in height between the mandibular and the grafted edge. The prosthetic planning for the rehabilitation was established using a fixed prosthesis in porcelain fused to metal with four elements as showed on panoramic radiograph (Figure 7), and compensated with pink porcelain (Figure 8,9), which reestablished the masticatory function and aesthetics of the region (Figure 10,11).
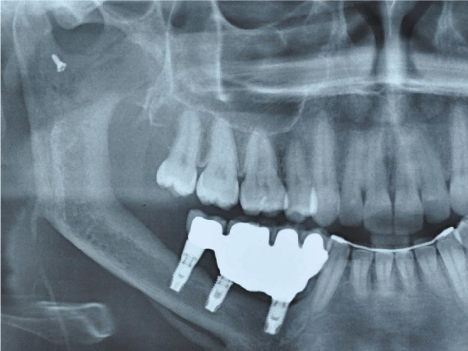
Figure 7: Final Panoramic radiograph after implant placement and prosthesis
screwed in place.
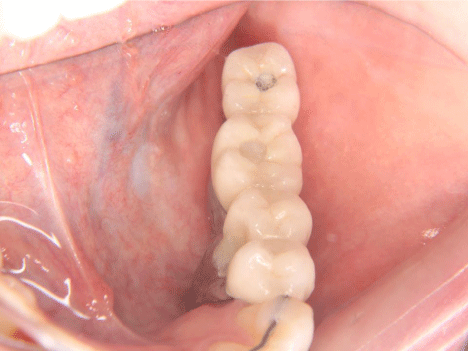
Figure 8: Close-up in occlusal view of final porcelain prosthesis in place.
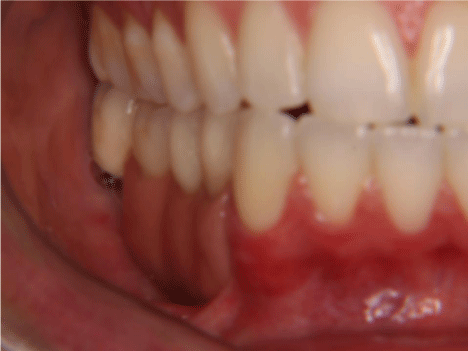
Figure 9: Close-up in lateral view of final porcelain prosthesis in place.
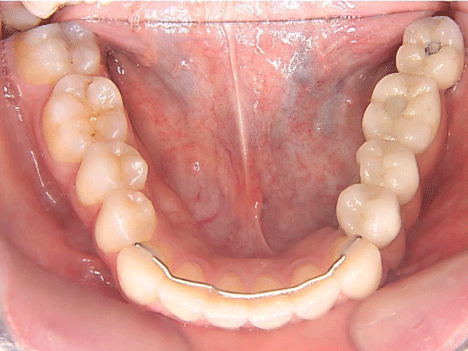
Figure 10: Full arch in occlusal view of final porcelain prosthesis in place.
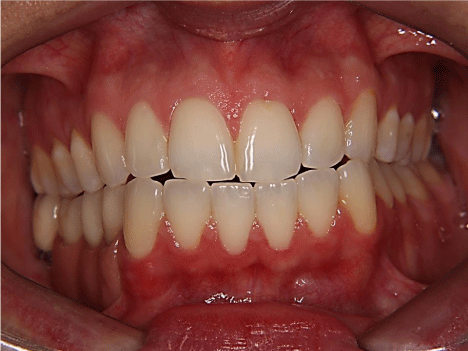
Figure 11: Close-up in frontal view with lip retractors of final porcelain
prosthesis in place.
A severe pain in the region due to chewing and biomechanical loads related to the return of the correct occlusion. Therefore this, the use of muscle relaxants was prescribed and the remission of symptoms was observed within 5 days. The patient was monitored for 36 months after prosthetic rehabilitation, with assessment of the function and aesthetics of the region. The patient was very pleased with the final outcome of this treatment, as the patient noticed a significant improvement in function, aesthetics, and phonetic quality (Figure 12).
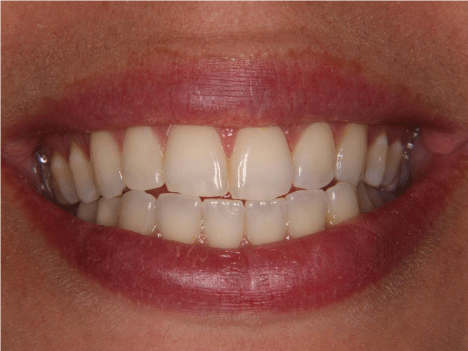
Figure 12: Full smile view of final porcelain prosthesis in place.
Discussion
According to these authors [8,10], multicystic or solid ameloblastoma more commonly develop in patients aged 44 years and was confirmed that it is rare in younger patients [4]. In this case report, the first manifestations of the disease were observed at 18 years of age.
Clinically, multicysticameloblastoma is the most aggressive variant, owing to its ability to infiltrate into bone trabeculae. In this case, tumor aggressiveness was observed during the radiographic follow-up and in a short period of time, the injury spread throughout the whole body and into the ascending ramus of the right jaw.
The choice of treatment depends on the clinical characteristics of the patient, tumor location, size, and margins as well as the age of the patient and the degree of morbidity that the treatment may cause [2]. The major problem faced with treatment of all types of ameloblastoma is their high recurrence rate, which was previously reported [1,9]. Moreover, when not removed correctly, ameloblastic islands remain within the trabecular bone or soft tissue and may continue to proliferate, thus leading to the recurrence of this type of tumor, a statement reinforced by other author [5].
In our case, three biopsies were performed before arriving at the correct diagnosis. The early diagnosis of endodontic periapical cyst resulted in two relapses and favored the proliferation of the tumor and 5 years after start the treatment, the size of the tumor had significantly increased, thus necessitating a surgical approach. Mandibular hemisection and the immediate reconstruction was performed by using a fibular graft, requiring surgical excisions with safety margin from 1 to 2 cm of healthy bone [6], as recommended by many authors before [1,5,9,10], resulting in a slight facial asymmetry and loss of sensitivity of the adjacent structures, owing to the interruption of the main nerves of this region.
Moreover, the different rates of relapse depend on the surgical technique that was used, the number of cases and the monitoring period [2,8]. The clinical and radiographic follow-up of these lesions is therefore very important, with a recurrence rate of 50% within 7 years of tumor removal [4].
Tumor recurrence depends on several factors, such as the choice of treatment for the primary tumor, the extent of the injury, the proliferation of residual portions of the tumor that were not removed with the surgery, and the implantation of tumor tissue in other organs during surgery [10].
Mandibular reconstructions are performed with reconstruction plates, bone, and skin grafts used to replace the absence of mucosa, and dental implants are installed to rehabilitate part of the dentition that was lost and to finalize the prosthetic reconstruction, according to previous cases reported [1,2,6,7].
The grafts placed immediately after tumor removal show better results [1,5], as delayed or late reconstruction may cause lingual collapse and the displacement of the remaining vertical and horizontal mandibular branches. In addition, the dissection and placement of remaining bone stumps is difficult and delicate.
Immediately, reconstruction of the region following tumor resection promotes an anatomical and functional restoration, allowing the repair of the affected area in a single surgical procedure, without distortions, deviations, atrophies, and the formation of scars inherent to secondary surgeries [11,12]. This renders the technique described more reliable, thus being considered as the best alternative treatment for ameloblastomas [2,3,5,6], as it promotes the complete removal of the tumor with aesthetic and functional rehabilitation during the same surgical procedure. Moreover, rehabilitation with dental implants can be performed after a relatively short time, thus providing the patient the return of normal chewing functions with implant prostheses on resected side were suggested to contribute to masticatory function and oral perception in those patients on the reconstructed side and the resected side may become the habitual chewing side in a few time [13].
Segmental defects of the mandible can be reconstructed by using vascularized or non-vascularized grafts, with vascular grafts being the first choice for mandibular reconstructions [2]. Nevertheless, this method is not optimal, since it increases the operating time, morbidity of the donor site, and cost.
Conclusion
In this case, a micro vascularized fibular graft was used immediately after tumor resection. It was considered the best surgical option, owing to the extent of the lesion and the favorable conditions of the patient to undergo this procedure leading to dental implants and rehabilitation with implant-supported prostheses.
Multicystic ameloblastoma requires the removal teeth with a large area of adjacent tissue for its complete removal. Nevertheless, this study concludes that excellent long-term results are observed when a correct diagnosis and treatment plan is formulated. The fibula is a good option for an immediate reconstructive surgical approach with vascularized autogenous grafts.
After its complete incorporation, this graft becomes viable to dental implants that support functions and chewing loads. Aesthetics and oral health are restored with minor or no consequences, reduced morbidity and minimal treatment time, owing to a reduced number of surgical interventions. This subsequently increases long-term functional and aesthetic prognosis.
References
- Curi MM, Dib LL, Pinto DS. Management of solid ameloblastoma of the jaws with liquid nitrogen spray cryosurgery. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997; 84: 339-344.
- Zemann W, Feichtinger M, Kowatsch E, Karcher H. Extensive ameloblastoma of the jaws: surgical management and immediate reconstruction using microvascular flaps. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007; 103: 190-196.
- Andrade NN, Shetye SP, Mhatre TS. Trends in Pediatric Ameloblastoma and its Management: A 15 year Indian Experience. J Maxillofac Oral Surg. 2013; 12: 60-67.
- Eckardt AM, Kokemuller H, Flemming P, Schultze A. Recurrent ameloblastoma following osseous reconstruction--a review of twenty years. J Craniomaxillofac Surg. 2009; 37: 36-41.
- Pogrel MA, Montes DM. Is there a role for enucleation in the management of ameloblastoma? Int J Oral Maxillofac Surg. 2009; 38: 807-812.
- Jeremic JV, Nikolic ZS, Boricic IV, Tacevic ZD, Tomanovic NR, Drcic LJ, et al. Total mandibular reconstruction after resection of rare "honeycomb-like" ameloblastic carcinoma-a case report. J Craniomaxillofac Surg. 2010; 38: 465-468.
- Gilijamse M, Leemans CR, Winters HA, Schulten EA, van der Waal I. Metastasizing ameloblastoma. Int J Oral Maxillofac Surg. 2007; 36: 462-464.
- Yoon HJ, Hong SP, Lee JI, Lee SS, Hong SD. Ameloblastic carcinoma: an analysis of 6 cases with review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009; 108: 904-913.
- Nakamura N, Higuchi Y, Mitsuyasu T, Sandra F, Ohishi M. Comparison of long-term results between different approaches to ameloblastoma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002; 93: 13-20.
- Benlyazid A, Lacroix-Triki M, Aziza R, Gomez-Brouchet A, Guichard M, Sarini J. Ameloblastic carcinoma of the maxilla: case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007; 104: e17-24.
- Bucci T, Nocini PF. Functional Reconstruction of Nonsegmental Mandibular Defect with Fresh Frozen Bone Graft and Delayed Implants Placement. J Craniofac Surg. 2017.
- Askin SB, Aksu AE, Calis M, Tulunoglu I, Safak T, Tozum TF. Report of multidisciplinary treatment of an extensive mandibular ameloblastoma with free iliac crest bone flap, dental implants, and acellular dermal matrix graft. J Oral Implantol. 2015; 41: 107-111.
- Noguchi T, Tsuchiya Y, Sarukawa S, Yamazaki Y, Hayasaka J, Sasaguri K, Jinbu Y, Mori Y. Relationship Between Oral Perception and Habitual Chewing Side for Bare Bone Graft With Dental Implants After Mandibular Reconstruction. J Craniofac Surg. 2016; 27: 1263-1266.
Citation:Deliberador TM, Grossi JRA, Saad T, Scariot R, Zielak JC and Giovanini AF. Oral and Masticatory Rehabilitation Using Osseointegrated Dental Implants After Resective Treatment of Multicystic Ameloblastoma in the Lower Jaw with a Fibula Graft – A Case Report. J Dent & Oral Disord. 2017; 3(2): 1060. ISSN:2572-7710