
Case Report
A Case Report. J Dent & Oral Disord. 2018; 4(2): 1089.
Porphyria Cutanea Tarda (PCT)
Daya S¹*, Joe CL¹, Senthil E¹ and Satish S²
¹Department of Pedodontia & Preventive Dentistry, Chettinad Dental College & Research Institute, TN Dr MGR Medical University, India
²Department of Oral Medicine & Radiology, Chettinad Dental College & Research Institute, TN Dr MGR Medical University, India
*Corresponding author: Srinivasan Daya, Department of Pedododntia & Preventive Dentistry, Chettinad Dental College & Research Institute, TN MGR Medical University, India
Received: January 08, 2018; Accepted: February 12, 2018; Published: February 23, 2018
Abstract
Porphyria is caused by deficiency in enzyme causing heme synthesis. A case of Porphyria cutaneatarda with hyper pigmentation, fragile oral mucosa, restricted mouth opening and a painful tooth which required treatment is presented here.
Keywords: Porphyria; Dental treatment; Lignocaine; Heme
Introduction
Porphyrias are group of metabolic disease caused by deficiencies of 7 sequential enzymes in the synthesis of haem. Enzyme deficiencies result in accumulation of intermediate porphyrins in tissues and their excess are excreted in urine or stool [1,2]. Porphyrins are phototoxic molecules, hence accumulation in tissues cause phototoxic reaction on exposure to light. This phototoxicity causes cutaneous lesions by generation of oxygen reactive molecules.
Based on location of excess porphyrin, it can be classified as
1. Erythropoieticporphyrias - Congenial Erythropoietic Porphyria (CEP) ,ErythropoieticProtoporphyria (EPP)
2. Hepatic porphyrias : Porphyria cutaneatarda, Hepatoerythropoietic porphyria HEP,Variegate Porphyria (VP) and Hereditary Coproporphyria (HCP)
PCT results because of inactivation of hepatic Uroporphyrinogendecarboxylase (URO-D) enzyme [3,4]. With the exception of congenital erythropoietic porphyria (CEP), which is autosomal recessive, all other porphyrias are inherited as autosomal dominant disorders. In CEP teeth discoloration is a specific clinical sign called erythrodontia. The tooth appears as bright red flourescent under Wood’s light illumination [5].
Case Presentation
A 14 year old girl came to Department of Pedodontia & Preventive Dentistry with complaint of painful tooth on lower left back side of the tooth for past 7 days. Patient had been unable to chew any food and had been taking only semisolid food for past 2 months. On history it was found that the girl was born out of non consanguineous marriage, skin lesions were present from birth. No one else in the family had been affected. There was no history of jaundice. Skin lesions were not associated with fever or joint pain. Wounds healed without scarring. Lesions were not associated with thickening of the skin on soles and palms. There was no difficulty in swallowing or breathing. Urine had been dark orange yellow color from birth. No abdominal discomfort was present. No discolouration of primary teeth was present previously.
On physical examination, blisters were noticed on sun exposed areas of the skin and found to be fragile. Crusting followed by healing was present in many areas of hand. Hyperpigmentation, were noticed in many areas of the body (Figure 1, 2). There was absence of malar rash. On intra oral examination, mouth opening was restricted to 25mm. The buccal mucosa was fragile, alveolar mucosa was inflammed, reddish and on lower left side bleeding was noticed from the gingiva. Retraction of buccal mucosa was itself very painful and evoking bleeding from the retracted site. Lower left first permanent molar (36) had decay involving the pulp. Oral pantomogram showed radiolucency involving the pulp of 36. (Figure 3) Calcification of mesial canal of 36 was noticed. There was generalized calcification of pulp canal space of lower teeth. It was decided that permanent first molar needed a root canal treatment. Blood investigations revealed 8.1gm% of Hemoglobin with normal ferritin levels. There was increased urinary uroporphyrin level and isoproporphyrin in stool.
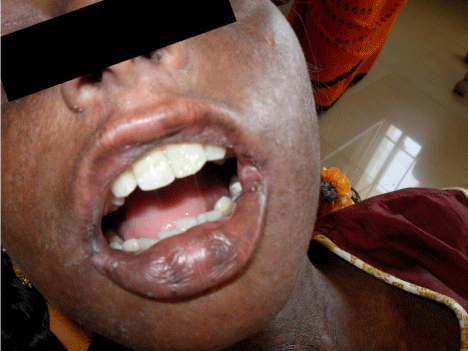
Figure 1: Restricted mouth opening.
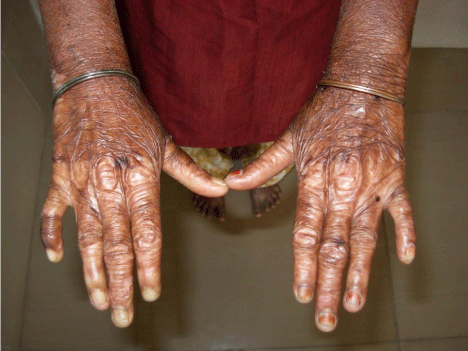
Figure 2: Hyper pigmentation of extermities.
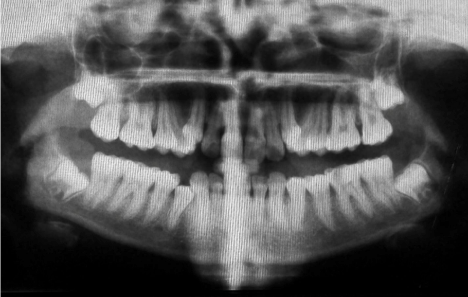
Figure 3: Orthopantomographic features.
The patient was referred to Department of Dermatology and was prescribed on sunscreen lotions and oral chloroquine tablet. Oral hygiene prophylaxis was carried out. A test dose of bupivicaine was given, when no allergic reaction was noticed local anesthesia was given with respect to lower left permanent first molar. Root canal opening was done. Both the mesial canals were calcified. RC Help (Prime dental products) was used as chelating agent and closed dressing was placed. Patient was put amoxycillin tablet and Ibuprofen analgesic. After 2 weeks there was an improvement in mouth opening to 35mm. There was less bleeding upon retraction of oral mucosa. Obturation was completed with guttapercha and permanent restoration done with posterior composite.
Discussion
Porphyria cutaneatarda (PCT) can be clinically divided into four types 6. Type I, sporadic form is caused by alcohol, estrogen, iron intake, Hepatitis C virus, HIV, SLE. They are generally associated with normal URO-D level. Type II is autosomal dominant disorder with genetic mutations of the Uro-D gene. Type III is toxic form, symptomatic with familial history. Type IV- Hepatoerythropoietic Porphyria (HEP), is severe mutilating type of porphyria caused by a homozygous defect of Uro-D3. Hemochromatosis gene (HFE) mutations and the Hepatitis C virus (HCV) are both risk factors for PCT [7,8].
Investigations include (1) Biochemical (2) Enzyme activity (3) Genetic studies. Biochemical test is done for detection of porphyrin and its precursors in urine, faeces and in RBC. Enzyme investigation measures URO-D levels in erythrocytes. Genetic studies are done in family members who have inherited porphyria, even if they do not have signs and symptoms of the disease. It is done for detection of HFE mutations in PCT, single-Nucleotide Polymorphisms of IVS3- 48C alleles1 in EPP. The case has been diagnosed as PCT based on history, absence of other symptoms which distinguishes from SLE, Epidermolysisbullosa and presence of porphyrin in urine and stool which distinguishes from other Porphyria.
There have been findings of the porphyriopathy due to lidocaine tested on animals and cell cultures. It is recommended that bupivacaine be used for infiltration local anesthesia [9]. RC Help contains EDTA and carbamide peroxide. It helps in chelating the calcium salts within root canal and thereby helps in chemico mechanical preparation of root canal. Treatment options for PCT include removal of iron by phlebotomy or low-dose chloroquine, [10] desferrioxamine infusion, cholestyramine, iron chelators, high-dose hydroxychloroquine, and erythropoietin. Chloroquine forms a water soluble complex with porphyrins and are rapidly eliminated in the urine 6 and thus prescribed in present case.
The present case is a challenge to dentist because of restricted mouth opening and handling of painful friable bleeding mucosa. Inadvertent handling of tissue can lead to ulcer, blister or lichenoid reactions. The canals are calcified making endodontic treatment difficult. Calcification of pulp canal space in Porphyria has not been reported previously in literature. Oral prophylaxis and maintenance is very critical as the patient find it difficult to brush without causing bleeding of mucosa. Most importantly lignocaine which is widely used local anesthetic drug in dentistry should be avoided. Dentists should be aware of this metabolic disorder and be equipped to deal effectively.
References
- Lecha M, Puy H, Deybach JC. Erythropoieticprotoporphyria.Orphanet J Rare Dis. 2009;4:19.
- Sies C, Florkowski C. A guide to the diagnosis of porphyria: suggested methods and case examples. N Z J Med Lab Sci 2006;60(1):7-11
- Moran-Jimenez MJ, Ged C, Romana M, et al. Uroporphyrinogen decarboxylase: complete human gene sequence and molecular study of three families with hepatoerythropoietic porphyria. Am J Hum Genet.1996;58(4):712-21.
- Elder GH, Roberts AG, de Salamanca RE. Genetics and pathogenesis of human uroporphyrinogen decarboxylase defects.Clin Biochem.1989;22(3):163-8.
- Grossman ME, Bickers DR, Poh-Fitzpatrick MB, Deleo VA, Harber LC. Porphyria cutaneatarda.Clinical features and laboratory findings in 40 patients. Am J Med.1979;67(2):277-86.
- Bulat V, Lugovic L, Situm M, Buljan M, Bradic L. Porphyria cutaneatarda as the most common porphyria. ActaDermatovenerol Croat. 2007;15(4):254-63.
- Chuang TY, Brashear R, Lewis C. Porphyria cutaneatarda and hepatitis C virus: a case control study and meta-analysis of the literature. J AmAcadDermatol 1999;41(1):31–6.
- Cribier B, Chiaverini C, Dali-Youcef N, et al. Porphyria cutaneatarda, hepatitis C, uroporphyrinogen decarboxylase and mutations of HFE gene. A casecontrol study. Dermatology.2009;218(1):15-21.
- McGovern E, Fleming P, O’Marcaigh A. The dental management of five paediatric patients with a history of acute intermittent porphyria.Eur Arch Paediatr Dent.2007;8(4):215-8.
- Kauppinen R, Timonen K, Mustajoki P. Treatment of the porphyrias. Ann Med 1994;26(1):31-8.