
Case Report
J Dent & Oral Disord. 2021; 7(2): 1160.
Plexiform Unicystic Ameloblastoma - A Diagnostic Dilemma
Rai DV¹*, Guttal KS², Hallikeri K³ and Burde KN²
1Department of Oral Medicine and Radiology, AJ Institute of Dental Sciences, India
2Department of Oral Medicine and Radiology, SDM College of Dental Sciences and Hospital, India
3Department of Oral and Maxillofacial Pathology, SDM College of Dental Sciences and Hospital, Dharwad, India
*Corresponding author: Devishree Vishpal Rai, Department of Oral Medicine and Radiology, AJ Institute of Dental Sciences, Mangalore, India
Received: March 23, 2021; Accepted: April 14, 2021; Published: April 21, 2021
Abstract
The 2nd most common tumor of odontogenic origin is Ameloblastoma which develops from epithelial cellular elements and dental tissues in various phases of development. It is a slow-growing, persistent and locally aggressive neoplasm of epithelial origin, affecting the posterior area of lower jaw in 80% of cases. Unicystic Ameloblastoma (UA) is one of the less encountered variants of Ameloblastoma. Radiographically it mimics many of the odontogenic cysts and tumors and hence becomes difficult to arrive at a definitive diagnosis. We report here a case of plexiform unicystic variant of ameloblastoma in a 26 years old male patient.
Keywords: Unicystic; Ameloblastoma; Plexiform; Carnoy’s solution; Mural
Case Presentation
A 26 years old male patient had come to our department of Oral medicine and radiology with a chief complaint of painless swelling in the lower right back region of the jaw in the last five months. In the history of presenting illness, patient said that he first noticed the swelling five months back which gradually increased to present size. Extraoral examination revealed that there was mild facial asymmetry on the lower 1/3rd of the face on the left side with diffuse swelling measuring about 1×1.5 cm extending anteroposteriorly 1 cm away from corner of mouth to angle of mandible & superioinferiorly from tragus of ear to lower border of mandible (Figure 1). Color and texture of the overlying skin was normal. On palpation, there was no tenderness and local rise in temperature. There was no evidence of lymphadenopathy. On intraoral examination, bony hard swelling was present extending from 47 to retromolar region with expansion of buccal and lingual cortical plates with no tenderness (Figure 2). 48 was missing. No discharge was present from the region. Patient had no relevant past medical and dental history. A provisional diagnosis of benign odontogenic cyst was given. Differential diagnosis of Dentigerous cyst, Odontogenic keratocyst and Ameloblastoma were considered.

Figure 1: Mild extraoral swelling in the right lower third of face (right).
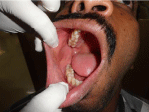
Figure 2: Mild vestibular obliteration seen in the right buccal vestibule
posteriorly irt 47 and 48.
To confirm the diagnosis radiologic investigations were performed. IOPA revealed impacted 48. Diffuse radiolucency extending posterior to 47 towards the ascending border of ramus (Figure 3). Orthopantomograph revealed unilocular radiolucency extending from distal surface of 46 involving posterior body of the mandible and ramus extending towards the sigmoid notch with thinning of the cortical bone. Root resorption was present i.r.t 46 and 47. Inferior alveolar canal is poorly delineated (Figure 4). Cone beam computerized tomography revealed expansion and thinning of the cortical bone (Figure 5).
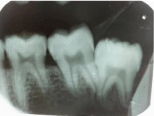
Figure 3: IOPA reveals radiolucency extending from 47, 48 region and
involving the ramus of the mandible.
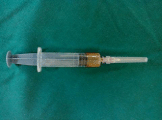
Figure 4: Aspirate revealed straw-coloured blood tinged fluid.
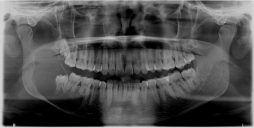
Figure 5: Orthopantomograph reveals well defined unilocular radiolucency
extending from distal root of 46 to the sigmoid notch with thinning of the
cortical bone and destruction of the mandibular nerve canal.
FNAC of the swelling was done which revealed blood-tinged clear fluid and was sent for examination. The report was not significant as it showed evidence of inflammatory and epithelial cells (Figure 6).
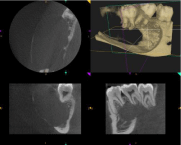
Figure 6: CBCT sections reveal thinning of the cortical plates and root
resoption wrt 46 and 47.
Incisional biopsy was advised. Histopathology sections revealed loosely arranged fibro-cellular connective tissue stroma lined by areas of discontinuous 2-4 cell layer flattened epithelial cell with evidence of intramural and intraluminal plexiform strands. In between the strands, stromal degeneration and dilated capillaries were prominent. Few sections showed oral mucosal epithelial and stromal tissue infiltration by the chronic inflammatory cells. Pathologic report confirmed Unicystic plexiform ameloblastoma (Figure 7).
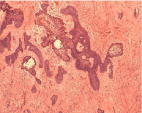
Figure 7: Histopathological sections reveals evidence of intramural and
intraluminal plexiform strands.
Treatment plan of surgical enucleation followed by application of Carnoy’s solution was done. Patient is currently under follow up (Figure 8 and Figure 9).
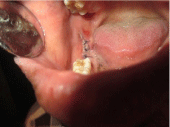
Figure 8: Post-operative clinical image.
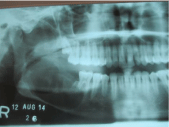
Figure 9: Post- operative radiograph.
Discussion
In 1977, Robinson and Martinez first coined the term Unicystic Ameloblastoma (UA). They considered unicystic variant has less aggressive biologic behavior than does solid or multicystic ameloblastoma [1]. The term plexiform unicystic ameloblastoma refers to a pattern of epithelial proliferation which is similar to the cystic lesions of the jaws. It does not display the histological criteria for ameloblastoma and has therefore been considered by some pathologists to be a hyperplastic epithelial proliferation rather than an ameloblastoma [2].
In a report by Gardner et al. it was seen that 46 plexiform UAs occurred in mandible and none occurred in the maxilla [2].
The tumor enlarges gradually in size, which is why patients occasionally notice it and report at the later stage, which was true in our case.
The clinical and radiographic findings in most cases of UA suggest that the lesion is an odontogenic cyst, particularly dentigerous cyst. However, few are not associated with impacted teeth which are called non-dentigerous variant [3]. Leider et al, proposed three pathogenic mechanisms for the evolution of Unicystic ameloblastoma: reduced enamel epithelium, from dentigerous cyst and due to cystic degeneration of solid ameloblastoma [4].
Ackermann [1] classified this entity into the following three histologic groups:
Group I: Luminal UA (tumor confined to the luminal surface of the cyst).
Group II: Intraluminal/plexiform UA (nodular proliferation into the lumen without infiltration of tumor cells into the connective tissue wall).
Group III: Mural UA (invasive islands of ameloblastomatous epithelium in the connective tissue wall not involving the entire epithelium).
Features of both luminal as well as mural type of ameloblastoma were apparent in our case.
Since unicystic amleloblastomas have low recurrence rate, Robinson proposed enucleation rather than partial or complete jaw resection as treatment plan which appears to constitute appropriate therapy.[1] A retrospective analysis of 29 patients (Lee 2004) with a histologically confirmed diagnosis of unicystic ameloblastoma emphasized on a treatment regime employing enucleation and application of Carnoy’s solution, which was also done in our case. Despite the finding that 93% of lesions exhibited mural invasion, a recurrence rate of 10% after treatment is reported in this analysis, suggesting a possible benefit of Carnoy’s solution against recurrence [6].
The diagnosis of Unicystic ameloblastoma is not possible only based on clinical and radiological investigations as it tends to mimic many of the odontogenic cysts and tumors. Aspiration is not confirmative in these cases. Final diagnosis of plexiform unicystic ameloblastoma could be given only after Histopathological investigations. Long term follow up is necessary.
References
- Robinson L, Martinez MG. Unicystic ameloblastoma: a prognostically distinct entity. Cancer. 1977; 40: 2278-2285.
- Gardner DG, Washington DC, Corio RL. The relationship of plexiform unicystic ameloblastoma to conventional ameloblastoma. J Oral Surg. 1983; 56: 54-60.
- Roos RE, Raubenheimer EJ, van Heerden WF. Clinico-pathological study of 30 unicystic ameloblastomas. J Dent Assoc S Afr.1994; 49: 559-562.
- Leider AS, Eversole LR, Barkin ME. Cystic ameloblastoma. A clinicopathologic analysis. Oral Surg Oral Med Oral Pathol. 1985; 60: 624-630.
- Ackermann GL, Altini M, Shear M. The unicystic ameloblastoma: a clinicopathological study of 57 cases. J Oral Pathol. 1988; 17: 541-546.
- Lee PK, Samman N. Unicystic ameloblastoma use of Carnoy’s solution after enucleation. Int J Oral Maxillofac Surg. 2004.