
Case Report
J Dent & Oral Disord. 2021; 7(4): 1168.
Application of High-Frequency Conduction for Persistent Apical Periodontitis: A Case Report
Toshihiko Tominaga1,2*, Eiichiro Tada1,2, Kazuki Takahira1 and Tsutomu Sugaya2
1Tominaga Dental Clinic, 197-3 Shimohonjo Akinokami Seto, Naruto, Tokushima, Japan
2Department of Periodontology and Endodontology, Hokkaido University Graduate Dental School, Sapporo, Hokkaido, Japan
*Corresponding author: Toshihiko Tominaga, Tominaga Dental Clinic, 197-3 Shimohonjo Akinokami Seto, Naruto, Tokushima, Japan; Department of Periodontology and Endodontology, Hokkaido University Graduate Dental School, Sapporo, Hokkaido, Japan
Received: May 23, 2021; Accepted: June 22, 2021; Published: June 29, 2021
Abstract
We report the case of a 39-year-old male with Persistent Apical Periodontitis (PAP) caused by infection in an uninstrumented area, wherein conventional chemical root canal treatment is not possible, which was sterilized via highfrequency conduction. He underwent root canal filling after multiple endodontic treatments for tooth #4. As symptoms recurred, he was referred to our department with the chief complaint of dull pain during mastication. Present symptoms were percussion pain of the tooth, buccal mucosa swelling at the apical portion, and grade 1 mobility. Radiography revealed inadequate root canal filling. A radiolucent image 5×6 mm in diameter and with an unclear boundary was observed around the apex. External root resorption was mainly observed in the apical foramen, with a crown root ratio of approximately 1:1. Using 6% sodium hypochlorite under dental microscopy, chemomechanical root canal preparation was performed. Passive ultrasonic irrigation and calcium hydroxide application were conducted three times; however, periapical tissue inflammation did not subside. Therefore, the patient was diagnosed with PAP, and the uninstrumented area was sterilized via high-frequency conduction. High-frequency currents were applied to the apex, root surface, and periapical lesion at 500 kHz and 90 V; periapical tissue inflammation resolved after 2 weeks. Subsequently, the root canal was filled. Follow-up radiography revealed a bone regeneration-like image at 2 months. Bone defects healed at 11 months. Although surgical endodontic therapy is conventionally performed in PAP patients, high-frequency conduction could be a minimally invasive nonsurgical endodontic treatment option for uninstrumented areas in PAP patients.
Keywords: Electromagnetic apical treatment; High-frequency conduction; Nonsurgical endodontic treatment; Periapical lesion; Persistent apical periodontitis
Introduction
Persistent Apical Periodontitis (PAP) occurs when root canal treatment of apical periodontitis has not adequately eliminated intracanal and extraradicular infections [1]. PAP is classified as symptomatic or asymptomatic as the primary diagnostic term. Since the 1980s, there has been much focus on persistent bacterial infection outside the apical foramen as one of the causes of PAP [2], and bacterial colonies and biofilm formation on the root surface near the apical foramen and in tissues and foreign bodies inside the periapical lesion have been reported [3-5]. In particular, it appears that the infection remains in the uninstrumented area, for which use of cutting instruments such as files and drugs is not possible. To date, persisting or emerging disease following root canal treatment has been regarded as an indication of surgical endodontic treatment [6]; however, not all cases are indicated owing to anatomical factors, inadequate periodontal tissue support, and systemic disease. Recently, the topical application of antibacterial agents [7] and photodynamic antimicrobial chemotherapy [8,9] have been used against bacteria present outside the apical foramen; however, their effects have been questioned owing to several reasons, including the fact that it is difficult to penetrate the agents into the biofilm. Furthermore, although laser applications are being investigated [10,11], there is still room for improving the reachability of the tip to the apical region and the accurate irradiation of the target site due to its straightness.
Previously, I demonstrated that the application of a highfrequency current significantly inhibits bactericidal activity against Gram-positive and Gram-negative bacteria, inflammatory cytokine production from THP-1 cells by Streptococcus mutans stimulation, and gingipain activity of Porphyromonas gingivalis [12]. Therefore, by applying high-frequency current to the uninstrumented area, bacteria that exist not only inside the root canal but also outside the apical foramen could be eliminated and favorable healing could be expected. We devised a treatment method called “Electromagnetic Apical Treatment (EMAT)” aiming at the extinction of periapical tissue and promotion of alveolar bone regeneration and performed it in a patient with apical periodontitis with periapical lesions, resulting in favorable clinical outcomes [13,14].
Here, we describe a case in which a high-frequency current was applied to PAP that did not improve with conventional root canal treatment.
Case Presentation
A 39 year-old male was referred to our hospital for the examination and treatment of tooth #4. Since a year, he experienced spontaneous pain, and after 10 or more endodontic treatments at another hospital, root canal filling was performed because the condition had improved. Subsequently, the patient experienced no symptoms; however, approximately 1 month prior to referral, he experienced dull pain during mastication in the same tooth. Because the patient desired to conserve the tooth, he was referred to our hospital. The patient had no remarkable medical history.
Examination and diagnosis
Intraoral examination revealed that a resin jacket crown was attached to #4; no occlusal contact was observed regarding intercuspal position and mandibular lateral movement. The present symptoms were mild percussion pain, buccal mucosa swelling at the apical portion, and slight tenderness, with grade 1 mobility and a pocket probing depth of =3 mm around the circumference.
No spontaneous or induced pain was observed. Dental radiographic examination revealed a thick metal post two-third the root length in the root canal. Root canal wall thinning was noted.
The root canal filling material was 1-2 mm under the apex and the degree of root canal filling was low (Figure 1A). Cone beam computed tomography revealed a circular radiographic image with unclear boundaries and a diameter of approximately 5×6 mm around the apex. External root absorption was observed around the apical foramen (Figure 2A and 2B). Based on the above findings, the patient was diagnosed with chronic apical abscess in tooth #4.
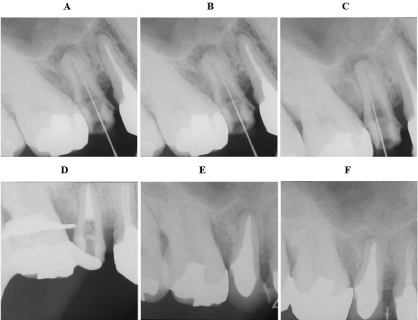
Figure 1: Dental radiography. (A) Inadequate root canal filling was performed
preoperatively and a periapical lesion was observed. (B) Root canal length
measurement during high-frequency conduction. (C) Bone defect diameter
measurement during high-frequency conduction. (D) After root canal filling.
(E) Five months after root canal filling, bone regeneration was observed in
the lesion area. (F) Healing was observed 11 months after root canal filling.
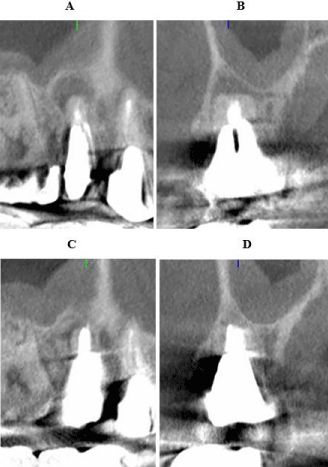
Figure 2: Cone beam computed tomography. (A) (B) Preoperatively, bone
resorption image with unclear boundaries was observed around the apex and
the apex was externally absorbed. (C) (D) At 2 months after root canal filling,
bone regeneration was observed from the bone wall.
Treatment options
Although apical surgery was considered, the case appeared to be contraindicated for such treatments as the crown ratio was already approximately 1:1. Furthermore, apicoectomy would lead to a further decrease in tooth bearing capacity, and root canal filling was inadequate. We initially planned intentional replantation; however, this treatment plan was not selected owing to root canal wall thinning and susceptibility of root canal fracture during tooth extraction. Because of the patient’s wishes, we performed nonsurgical endodontic treatment instead.
Treatment
After removing the crown and post core, a rubber dam was placed and the gutta-percha in the root canal was removed. The root canal was filled with 6% sodium hypochlorite (Antiformin, Nippon Shika Yakuhin Co., Ltd., Shimonoseki, Japan), and root canal enlargement was performed using a Ni-Ti rotary file (EndoWave LAX, J. MORITA CORP., Tokyo, Japan) and OK Micro Exca (UL0.5-45, Seto. Corp., Tsukuba, Japan). After enlargement, a Caries Detector (Kuraray Noritake Dental Inc., Tokyo, Japan) was used to confirm under the use of a dental operating microscope that no pathogenic substances such as carious dentin persisted in the root canal wall. The apical foramen was extremely dilated and edematous granulation tissue was observed outside the apical foramen. Furthermore, hemorrhage was observed in several areas (Figure 3A). Root fracture was not observed. Calcium hydroxide was applied inside the root canal and the opening was sealed with temporary filling material (Caviton, GC Corp., Tokyo, Japan). Approximately 2 weeks later, the apical swelling disappeared and the degree of mobility improved to within the normal physiologic range; however, there was no significant change regarding percussion pain and apical tenderness.
No change in the granulation tissue outside the apical foramen was observed, and hemorrhage continued. After performing Passive Ultrasonic Irrigation (PUI) for 5 min using 6% sodium hypochlorite, calcium hydroxide was applied. After 2 weeks, there were no significant changes in clinical signs and intraoral findings. After performing PUI for 5 min, calcium hydroxide was applied. Approximately 1 week later, the patient felt discomfort in the apex of #4 again; as a result, the patient again visited our hospital. Although no spontaneous pain was observed, slight swelling was observed in the area corresponding to the apex, percussion pain degree was exacerbated, and mobility was grade 2.
Although no abnormal findings were observed in the root canal wall, including the apical portion, because bacterial infection on the root surface or in the periapical tissue was suspected due to exacerbated inflammation of the periapical tissue, we decided to apply high-frequency current to sterilize the area. After explaining the treatment method, treatment time, and advantages and disadvantages of EMAT to the patient, consent for treatment was obtained.
A high-frequency conduction device (EMAT device, J. Morita Mfg. Corp., Kyoto, Japan) (Figure 4A) was used for conduction at a frequency of 500 kHz and an output voltage of 90 V once per second. Next, 6% sodium hypochlorite was injected into the root canal up to a depth of approximately 3 mm from the apical foramen. Then, a K file #10 (MANI, INC., Utsunomiya, Japan) (hereinafter, coated file) (Figure 4B), which was coated with an insulator except at the tip up to 3 mm, was used, After performing conduction of the apical foramen once, the tip of the coated file was bent by approximately 2 mm so that the tip could fit the root surface, and conduction was performed once at 2-mm intervals four times while being rotated. Moreover, considering the range of the bone defect and root apex exposed to the defect, the coverage of the root surface was set to 1-2 mm at all conductions. The granulation tissue outside the apical foramen instantly underwent thermal denaturation, and hemostasis was observed in almost all areas, excluding the palatal side. To further sterilize the lesion, a coated file was inserted into the periapical lesion approximately 2 mm from the alveolar bone wall. Then, conduction was performed once every 2 mm three times (Figure 1B, 1C, 4C). Immediately after conduction was performed, a large quantity of pale-yellow viscous exudate from the hemorrhage site on the palatal side was observed (Figure 3B-F). The exudate decreased after performing aspiration for approximately 1 min. However, as persistent exudation was observed, calcium hydroxide was applied. After 2 weeks, although slight mobility was observed, percussion pain and tenderness disappeared, and no swelling or other inflammatory symptoms were noted. The granulation tissue outside the apical foramen was improved to a semitransparent elastic tissue, and no hemorrhage or exudate was observed. White calcium carbonate deposition was observed on the palatal side, where continuing hemorrhage was present (Figure 3G). Drying was performed with sterilized paper points. Gutta-percha cones (Natural Gutta JH, TOYO CHEMICAL LABORATORIES.INC., Tokyo, Japan) and a resin sealer (SuperBond sealer, Sun Medical Co., Ltd, Moriyama, Japan) were used to perform warm vertical condensation (Figure 1D). After 3 weeks of condensation, mobility improved to within the physiological range. To prevent root fracture, the metal core was cemented with a 4-META/MMA-TBB adhesive resin (SuperBond, Sun Medical Co., Ltd), and the final prosthesis was attached to realize an appropriate occlusal relationship. Systemic antibiotic administration and local application were not performed in the present case.
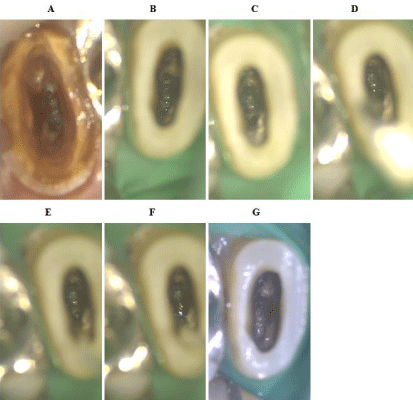
Figure 3: Microscopic images. (A) Preoperatively, there was edematous
granulation tissue in the apical foramen and hemorrhage in several areas.
(B) At 5 weeks after chemomechanical root canal preparation, no significant
changes were observed in the granulation tissue. (C) Immediately after highfrequency
conduction was applied to the root surface, thermal denaturation
of the granulation tissue occurred due to conduction. (D) A coated file was
inserted from the palatal side where hemorrhage was observed during
conduction to the periapical lesion. (E) Immediately after conduction to the
periapical lesion, hemostasis was confirmed on the palatal side. (F) Inflow of a
pale-yellow viscous exudate. (G) Two weeks after conduction, the granulation
tissue was coagulated and necrotic and a white film was observed on the
palatal side.
Follow-up
Approximately 2 months after EMAT, there were no notable clinical symptoms, and computed tomography findings indicated bone regeneration around the bone defect, with prominent shrinkage of the lesion (Figure 2C and 2D). After approximately 5 months, there was no significant change in clinical findings, and dental radiographic examination revealed slight enlargement of the periodontal ligament space surrounding the apex; however, the lesion area showed a bone-like image (Figure 1E). Approximately 11 months later, a trabecular structure was observed and the periodontal ligament space had improved to a nearly uniform thickness (Figure 1F). The posttreatment course has been favorable to the present date (Figure 1F).
Discussion
Apical periodontitis is caused by pathogenic factors in the root canal system that cannot be appropriately eliminated. Intracanal infection persisting in the complex apical root canal system, extraradicular infection, extruded root canal filling, or other exogenous materials have been reported as the causes of persistence [1]; this is mostly due to secondary infections in the root canal. Therefore, to manage PAP, it is first necessary to thoroughly eliminate root canal infections. In the present case, the root canal comprised a single root canal, which was already greatly enlarged, with dentin thinning and apical foramen dilation. Previously studies have reported that during root canal preparation, apical enlargement reduces bacterial count in the root canal [15,16]. Because excessive cutting of the apical portion frequently results in apical cracks, root canal formation should be performed up to 1 mm away from the apical foramen [17,18]. Therefore, root canal preparation using the rotary file was limited to 1 mm away from the apical foramen. The apical foramen was carefully scraped with light pressure using a handheld Micro Exca and a caries detector dye. During root canal preparation, 6% sodium hypochlorite was used in combination with mechanical cleaning.
Extraradicular infection and biofilm formation may be suspected if symptoms persist despite proper root canal cleaning [19,20]. Furthermore, extraradicular infection may exist independently of intracanal infection. It has been reported that extraradicular inflammation may persist even if intracanal infection is eradicated [21]. Surgical endodontic treatment has been reported to be essential for such extraradicular infections [20,22]. Furthermore, it has been reported that the healing period of periapical lesion can be shortened by performing surgical root canal retreatment compared with conventional orthograde retreatment [23]. However, considering the degree of surgical invasion and decrease in tooth support capacity due to root length shortening, anatomical restriction, general condition, etc., surgical endodontic treatment should be considered only for cases with nonsurgical treatment failure.
Presently, various studies for PAP treatments are being conducted. Reportedly, root maturation is observed despite persistent apical inflammation after regenerative endodontic therapy; however, the mechanism remains to be elucidated [24]. Additionally, it has been reported that the application of a long-term dressing with calcium hydroxide reduces pro-inflammatory cytokines and matrix metalloproteinases levels; therefore, they can have a bactericidal effect on root canal treatment failure cases with apical periodontitis [25]; nevertheless, questions remain regarding the bactericidal effect on non-contact sites.
We previously reported that high-frequency conduction has bactericidal effects on planktonic bacteria, including Enterococcus faecalis, which is one of the causative bacteria of PAP [12]. Furthermore, it has been reported that when a high-frequency current was applied to E. faecalis biofilms, the biofilms were destroyed and bactericidal effects were demonstrated [26]. Performing conduction with high-frequency currents results in the generation of Joule heat by increasing the current density in the exposed part of the coated file (Figure 4B). As a result, the instrumented areas can be sterilized by directly performing conduction of the inner surface of the curved root canal, fin, isthmus, outer surface of the root, within the periapical lesion, and foreign bodies outside the apical region. In the present case also, inflammatory symptoms not ameliorated by chemomechanical root canal preparation were eliminated via conduction. Furthermore, because the inflammation disappeared due to conduction of the outer surface of the root and periapical lesion, the infection in the same area could have been the cause of treatment resistance.
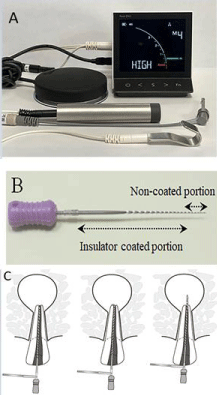
Figure 4: (A) Electromagnetic apical treatment (EMAT) device, electrosurgical
unit, active electrode, and counter electrode. (B) Coated file coated with an
insulator except for the 3-mm tip for efficient heat generation. (C) EMAT
procedure: high-frequency application of conduction to the apex, root surface,
and lesion inside the apex.
Basic research is required to clarify the bactericidal effect caused by high-frequency current in uninstrumented areas. Furthermore, how a high-frequency current affects the host response to bacterial infection is unclear. It has been reported that certain genetic markers may contribute to increased susceptibility to PAP [27]. Therefore, it will be necessary to perform genetic analysis in the future.
It is necessary to consider the damage to the bone when the electrode is inserted into the bone defect and high-frequency conduction is performed. However, in the present case, no postoperative pain or swelling was noted, and the lesion was healed. Thus, it is presumed that this procedure will not cause bone damage. Moreover, the heat conduction region of Joule heat derived via conduction was limited to a diameter of approximately 2 mm [28]. Therefore, it can be clinically applied to areas where the target has been narrowed down, and the possibility of causing adverse events is extremely low. Additionally, unlike drugs, there are no residues within the body and unforeseen side effects or appearance of resistant bacteria. Furthermore, conduction is completed in a few seconds, thereby shortening treatment length. Our results appear to have great clinical significance as almost all patients, except those who have undergone implantation (e.g., pacemaker, cochlear implant, and defibrillator), are eligible for this treatment.
As expected, the application of a high-frequency current to the uninstrumented area may be the third method of endodontic therapy following chemomechanical root canal preparation.
As EMAT is a relatively novel technique, randomized controlled trials are warranted to prove its effectiveness over the existing treatment options.
High-frequency conduction could sterilize the uninstrumented area with difficult instrumentation by generating Joule heat at the exposed part of the coated file. For PAP caused by infection in the uninstrumented area, high-frequency conduction is considered helpful.
Acknowledgement
We would like to thank K. Matoba and J. MORITA MFG. Corp. for providing the device. We would also like to thank Y. Kimura and Y. Yamaguchi for supporting this report.
References
- Nair PN. On the causes of persistent apical periodontitis: a review. Int Endod J. 2006; 39: 249-281.
- Tronstad L, Barnett F, Riso K, Slots J. Extraradicular endodontic infections. Endod Dent Traumatol. 1987; 3: 86-90.
- Leonardo MR, Rossi MA, Silva LA, Ito IY, Bonifácio KC. EM evaluation of bacterial biofilm and microorganisms on the apical external root surface of human teeth. J Endod. 2002; 28: 815-818.
- Ricucci D, Loghin S, Gonçalves LS, Rôças IN, SiqueiraJr JF. Histobacteriologic conditions of the apical root canal system and periapical tissues in teeth associated with sinus tracts. J Endod. 2018; 44: 405-413.
- Noiri Y, Ehara A, Kawahara T, Takemura N, Ebisu S. Participation of bacterial biofilms in refractory and chronic periapical periodontitis. J Endod. 2002; 28: 679-683.
- European Society of Endodontology. Quality guidelines for endodontic treatment: consensus report of the European Society of Endodontology. Int Endod J. 2006; 39: 921-930.
- Trairatvorakul C, Detsomboonrat P. Success rates of a mixture of ciprofloxacin, metronidazole, and minocycline antibiotics used in the noninstrumentation endodontic treatment of mandibular primary molars with carious pulpal involvement. Int J Paediatr Dent. 2012; 22: 217-227.
- Teixeira AH, Pereira ES, Rodrigues LK, Saxena D, Duarte S, Zanin D, et al. Effect of photodynamic antimicrobial chemotherapy on in vitro and in situ biofilms. Caries Res. 2012; 46: 549-554.
- Müller P, Guggenheim B, Schmidlin PR. Efficacy of gasiform ozone and photodynamic therapy on a multispecies oral biofilm in vitro. Eur J Oral Sci Actions. 2007; 115: 77-80.
- Mashalkar S, Pawar MG, Kolhe S, Jain DT. Comparative evaluation of root canal disinfection by conventional method and laser: an in vivo study. Niger J Clin Pract. 2014; 17: 67-74.
- Perin FM, França SC, Silva-Sousa YT, Alfredo E, Saquy P, Estrela C, et al. Evaluation of the antimicrobial effect of Er:YAG laser irradiation versus 1% sodium hypochlorite irrigation for root canal disinfection. Aust Endod J. 2004; 30: 20-22.
- Tominaga T. Application of electro-magnetic wave to endodontic treatment– EMAT (Electro-Magnetic Apical Treatment). Shikoku Dent Res. 2011; 24: 1-31.
- Tominaga T, Kitaike K, Tada E, Takahira K, Bando N, Hirao S, et al. Application of electromagnetic stimulation to apical periodontitis. J Jap Endod Ass. 2017; 38: 36-47.
- Bando N, Tominaga T, Yumoto H, Sumitomo T, Hirao S, Hirao K. Application of electro-magnetic wave irradiation for endodontic treatment -EMAT (Electromagnetic apical treatment)-. J Jap Endod Ass. 2011; 32: 184-200.
- Tan BT, Messer HH. The quality of apical canal preparation using hand and rotary instruments with specific criteria for enlargement based on initial apical file size. J Endod. 2002; 28: 658-664.
- Usman N, Baumgartner JC, Marshall JG. Influence of instrument size on root canal debridement. J Endod. 2004; 30: 110-112.
- Devale MR, Mahesh MC, Bhandary S. Effect of instrumentation length and instrumentation systems: hand versus rotary files on apical crack formation - An in vitro study. J Clin Diagn Res. 2017; 11: ZC15-ZC18.
- Kumari MR, Krishnaswamy MM. Comparative analysis of crack propagation in roots with hand and rotary instrumentation of the root canal -An ex-vivo study. J Clin Diagn Res. 2016; 10: ZC16-ZC9.
- Toubes KM, Tonelli SQ, de Oliveira BJ, Duarte G, Nunes E, Silveira FF. Apical periodontitis associated with a calculus-like deposit: A case report of a rare fan-shaped manifestation. Ann Med Surg (Lond). 2019; 41: 1-5.
- Ricucci D, Siqueira JF Jr, Lopes WSP, Vieira AR, Rôças IN. Extraradicular infection as the cause of persistent symptoms: a case series. J Endod. 2015; 41: 265-273.
- Siqueira JF, Rôças IN, Ricucci D, Hülsmann M. Causes and management of post-treatment apical periodontitis. Br Dent J. 2014; 216: 305-312.
- Alghamdi F, Alhaddad AJ, Abuzinadah. Healing of periapical lesions after surgical endodontic retreatment: A systematic review. Cureus 2020; 12: e6916.
- Lin LM, Kim SG, Martin G, Kahler B. Continued root maturation despite persistent apical periodontitis of immature permanent teeth after failed regenerative endodontic therapy. Aust Endod J. 2018; 44: 292-299.
- Barbosa-Ribeiro M, Arruda-Vasconcelos R, de-Jesus-Soares A, Zaia AA, Randi Frraz CC, Affonso de Almeida JF, et al. Effectiveness of calcium hydroxide-based intracanal medication on infectious/inflammatory contents in teeth with post-treatment apical periodontitis. Clin Oral Investig. 2019; 23: 2759-2766.
- Panariello BHD, Kindler JK, Spolnik KJ, Ehrlich Y, Eckert GJ, Duarte S. Use of electromagnetic stimulation on an Enterococcus faecalis biofilm on root canal treated teeth in vitro. Sci Rep. 2021; 11: 8306.
- Morsani JM, Aminoshariae A, Han YW, Montagnese TA, Mickel A. Genetic predisposition to persistent apical periodontitis. J Endod. 2011; 37: 455-459.
- Tominaga T, Tada E, Takahira K, Sugaya T. Heat generation and temperature increase in the root during electromagnetic apical treatment. J Dent & Oral Disord. 2020; 6: 1125.