
Case Report
Austin J Dent. 2015;2(1): 1013.
Keratocystic Odontogenic Tumor of the Mandible – A Case Report
Siddique Sabin1, Kumar Anoop2*, Maya Anoop3, Meera M4
1Department of Public Health Dentistry, Yenepoya University, India
2Department of Oral Pathology and Microbiology, Kerala University of Health Sciences, India
3Chief Dental Surgeon Anwi”s Multispeciality Dental Clinic, India
4Resident Medical Officer Anwi”s Multispeciality Dental Clinic, India
*Corresponding author: Kumar Anoop, Department of Oral Pathology and Microbiology Kerala University of Health Sciences, P S M College of Dental Sciences and research Akkikavu Trichur Dt Kerala, 680519, India
Received: December 30, 2014; Accepted: January 28, 2015; Published: January 30, 2015
Abstract
Odontogenic keratocyst has been renamed as the World Health Organization in 2005. It is a benign intraosseous neoplasm of the jaw. They develop from the dental lamina remenants in the mandible and maxilla. Keratocystic odontogenic tumor is of particular interest because of its recurrence rate and aggressive behavior. We present a case in a middle aged lady patient.
Keywords: Keratocyst odontogenic tumor; Mandible; Radiolucency
Introduction
Keratocyst Odonogenic Tumor (KCOT) is a benign odontogenic tumor with aggressive behavior and a high recurrence rate [1,2]. In the 2005 edition of the World Health Organization Classification of the Head and Neck Tumors, the odontogenic keratocyst was reclassified from a cystic to a neoplastic lesion, and the term “keratocystic odontogenic tumor” (KCOT) was coined [3]. The KCOT contributes approximately 11% of cysts of the jaws & is most commonly located in the mandibular ramus & angle [4]. Most common site is the mandibular third molar region. Remnants of odontogenic epithelium persisits in oral tissues after odontogenesis is complete and a variety of tumor and cysts may arise from these remnants [5].
Case Report
A 34 year old female patient came to the dental clinic complaining of pain and discharge in relation to the extraction site in the right lower posterior region. Pain was localized and dull in nature. There was no facial asymmetry or evidence of swelling over the cheek extra orally (Figure 1).The patient underwent an extraction of 48. But the pain persisted and there was also a discharge from the extracted site.
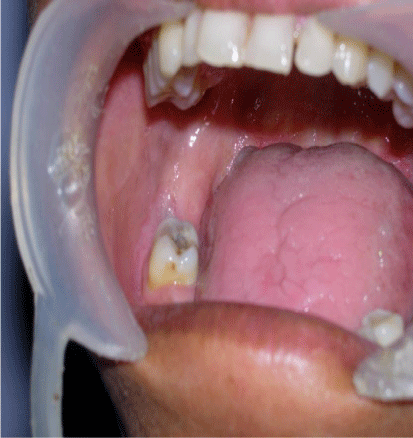
Figure 1: Swelling over the cheek extra orally.
On intra oral examination an unhealed socket in relation to 48 was seen and there was tenderness on palpation. Ortho pantamograph revealed a radiolucency in relation to the 47, 48 region (Figure 2).The lower border was intact and there was no evidence of any bone expansion.
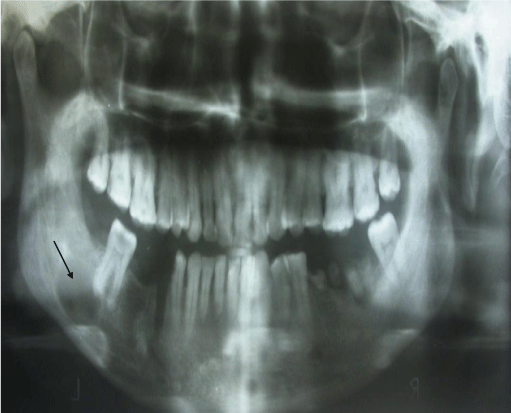
Figure 2: OPG revealing radiolucency in relation to 47 and 48 region.
An Excisional biopsy was performed and 3x1.5cm in size, firm in consistency was obtained. According to histopathological examination lesion was diagnosed as Keratocystic odontogenic tumor. Microscopic features of excised tissue showed odontogenic epithelial lining and connective tissue wall. The cyst is lined by parakeratinized stratified squamous epithelium which is about 4-6 layers thick without rete ridges (Figure 3).The parakeratotic layer has corrugated surface (Figure 4-a).and there is evidence of columnar palisaded basal cell layer (Figure 4-b).
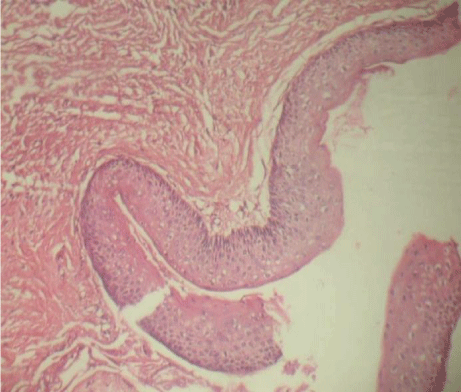
Figure 3: H & E stained section in lower magnification showing parakeratinized
stratified squamous epithelium which is about 4-6 layers thick without rete
ridges.
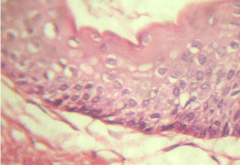
Figure 4-a: H & E stained section in higher magnification showing corrugated
surface in the parakeratotic layer.
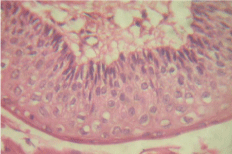
Figure 4-b: H & E stained section in higher magnification showing palisading
basal layer in the cyst lining.
Discussion
The term Odontogenic Keratocyst was introduced by Philipsen in 1956 [6]. Keratocystic odontogenic tumor is believed to be a developmental cyst which originates from the dental lamina or its remnants [5]. The first description of a solid variant of KCOT was reported by Ide et al in 2003 [7]. KCOT is more common in males than females and occurs over a wide age range and is diagnosed during second to fourth decade [8,9]. KCOT has a predilection for occurring in the mandible as compared to maxilla [1]. KCOT has extension through the bone much more than bone expansion, thus until tumor does not reach its significant dimensions, expansion is less important [10]. KCOT is difficult to diagnose clinically due to lack of specific clinical and radiographic characteristics [4]. Radiographically KCOT presents as a unilocular or a multilocular radiolucency with scalloped and well defined margins [11].
Histologically KCOT shows an epithelial lining consisting of a uniform layer of stratified squamous epithelium usually six to eight cells in thickness. Cystic lumen may contain a clear liquid or it may be filled with a cheesy substance that coexists of keratinaceous debris. Basal epithelial layer consists in a palisaded layer of cuboidal or columnar epithelial cells, which are often hyperchromatic. Small daughter cysts, cords or islands of odontogenic epithelium may be observed within fibrous wall [9,12]. The treatment options for keratocystic odontogenic tumors varies from simple curettage, enucleation (in combination with cryotherapy or Carnoy`s solution), marsupialization, decompression and secondary enucleation, and resection (marginal or segmental) [13,14]. Decompression and marsupialization are the most common used procedures in cases of a large mandibular and maxillary tumors, because they can save the anatomical structures including adjacent teeth, maxillary sinus or inferior alveolar nerve [15,16].
Conclusion
The OKC has been the subject of much debate with respect to its origin, its growth, and treatment modalities. Keratocystic odontogenic tumours are known for their peculiar behavior, varied origin, and unique tendency to recur. Post operative follow up is essential following surgical management due to its high recurrence.
References
- Godhi SS, Kukreja P. Keratocystic odontogenic tumor: a review. J Maxillofac Oral Surg. 2009; 8: 127-131.
- Maurette PE, Jorge J, de Moraes M. Conservative treatment protocol of odontogenic keratocyst: a preliminary study. J Oral Maxillofac Surg. 2006; 64: 379-383.
- Philipsen HP: Keratocystic odontogenic tumor, in Barnes L, Everson JW, Reichart P, Sidransky D (eds): World Health Organization Classification of Tumors: Pathology and Genetics of Head and Neck Tumors. Lyon, IARC Publishing Group, 2005, p 306.
- Stoelinga PJ. Long-term follow-up on keratocysts treated according to a defined protocol. Int J Oral Maxillofac Surg. 2001; 30: 14-25.
- Lund VJ. Odontogenic keratocyst of the maxilla: a case report. Br J Oral Maxillofac Surg. 1985; 23: 210-215.
- Philipsen.H.P On keratocysts in the jaws. Tandleagebladet.1956; 60:963.
- Ide F, Mishima K, Saito I. Solid-cystic tumor variant of odontogenic keratocyst: an aggressive but benign lesion simulating keratoameloblastoma. Virchows Arch. 2003; 442: 501-503.
- Shafer Hine Levy. Cyst and tumors of odontogenic origin. R Rajendran.Shafers textbook of Oral Pathology:Noida, Elsevier Publications 2009; 6: 254-62.
- Brad W Neville, Damm Douglas D, Carl M Allen, Jerry E Bouquot. Odontogenic cysts and Tumors. Oral and Maxillofacial Pathology ,Noida , Saunders ( Elsevier) Publications 2009;3:683-87.
- White SC, Pharoah MJ. Cysts and cyst like lesions of the jaws. In: White SC, editor. Text Book of Oral Radiology. 6th ed. St. Louis: Mosby Elsevier 2009. p. 506-12.
- Giuliani M, Grossi GB, Lajolo C, Bisceglia M, Herb KE. Conservative management of a large odontogenic keratocyst: report of a case and review of the literature. J Oral Maxillofac Surg. 2006; 64: 308-316.
- Shear M, Speight P.Cysts of oral and maxillofacial regions ( 4th edition) Oxford Blackwell Munksgaard 2007:6-58
- Cakur B, Miloglu O, Yolcu U, Göregen M, Gürsan N. Keratocystic odontogenic tumor invading the right maxillary sinus: a case report. J Oral Sci. 2008; 50: 345-349.
- Ortakoğlu K, Süer BT, Sençimen M. A large keratocyst containing a third molar tooth in the maxillary antrum. Turk J Med Sci 2005: 35; 341-346.
- Nakamura N, Mitsuyasu T, Mitsuyasu Y, Taketomi T, Higuchi Y, Ohishi M. Marsupialization for odontogenic keratocysts: long-term follow-up analysis of the effects and changes in growth characteristics. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002; 94: 543-553.
- Jung YS, Lee SH, Park HS. Decompression of large odontogenic keratocysts of the mandible. J Oral Maxillofac Surg. 2005; 63: 267-271.