
Case Report
Austin J Dent.2015;2(1): 1014.
Combined Orthodontics and Orthognathic Surgery for the Correction of Class II Div I Malocclusion – Two Days Post-operative Recovery. Case Report
Prithiviraj Jeyaraman1*, Narendran Kesavaraj2, Priti S. Mulimani1
1Department of Orthodontics, Faculty of Dentistry, Melaka Manipal Medical College, Malaysia
2Consultant Oral and Maxillofacial Surgon, Amsa Dental Clinic, Nandhi Koil Street, Trichy, India
*Corresponding author: Prithiviraj Jeyaraman, Department of Orthodontics, Faculty of Dentistry, Melaka Manipal Medical College, Melaka – 75150, Malaysia
Received: October 09, 2014; Accepted: January 30, 2015; Published: February 02, 2015
Abstract
An adult patient with severe skeletal deformity and Class II Division 1 malocclusion was treated with orthodontic appliances and orthognathic surgery. The combined orthodontic-orthognathic surgical procedure, with proper planning and collaboration of the specialists, resulted in a successful, satisfactory and quick outcome for the patient, by restoring facial aesthetics, occlusal balance and functional efficiency in a relatively short period of time.
Keywords: Orthognathic; Orthodontics; Aesthetics; Surgery; Anterior maxillary Osteotomy
Introduction
Deformities of the jaws result in skeletal and dental malocclusions which often cause dysfunction and distress to the patients and provide a challenging task to the Orthodontist to restore occlusal harmony, muscular balance and optimum function. These deformities at an early age, when the patient is still growing, have the potential to be corrected with growth-modifying appliances. However, in adults, depending upon the case, the jaws may be left in the same position and the underlying skeletal deformity can be camouflaged by dental correction or a combined orthodontic and surgical approach can be adopted, which would correct both the jaws and the occlusion [1]. An inter-disciplinary and planned approach in collaboration with the Oral and Maxillofacial surgeons, in the latter option, provide outcomes which restore aesthetics, function and balance, which go a long way in improving the confidence, psychosocial well-being and prospects of the patient [1]. However, there are also associated risks and complications with this approach, one of them being the trauma of the surgical procedure which the patient has to undergo. The accompanying oedema, pain and loss of function during the immediate post-operative phase often make the patient apprehensive about the whole procedure. Gentle tissue-manipulation and handling of the tissues to minimize surgical trauma on the operating table and frequent flushing with povidone-iodine solution [2] during the surgery are the key in providing an un-eventful and relatively smooth recovery for the patient from this procedure. We present a case, in which, such an approach was adopted while carrying out the orthognathic surgery, which consequently resulted in two days immediate recovery and rapid healing and restoration of function and aesthetics after the surgical procedure in the patient.
Diagnosis and Etiology
A 23 year old female patient, presented with the chief complaint of severely protruding upper front teeth, inability to close the lips and an unsatisfactory smile. The patient was quite concerned about her appearance and desired orthodontic treatment to correct her proclined incisors and improve the smile at the earliest, as she was planning to take up a career inmodelling.
On extra-oral examination, the patient had a class II skeletal pattern with convex profile, decreased lower facial height,a potentially competent lip and lower lip trap with deep mentolabial sulcus. The skeletal convexity was observed to be maxillary. Frontal view of the face showed chin deviation to the right. The lower lip was everted. Incisor visibility at rest was around 4-5 mm and in smile the full length of incisor crowns was seen with no excessive gingival display. (Figures 1-3).
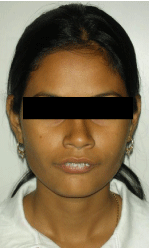
Figure 1: Pre surgical extra oral (Frontal view).
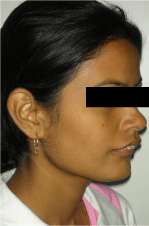
Figure 2: Pre surgical extra oral (Profile).

Figure 3: Post surgical extra oral (Fontal view).
Intra-orally, overjet was around 12 mm, overbite was 100 % with a deep curve of spee. Canines were in Class II relationship and the molars were also in full-cusp Class II on both-sides. Upper and dental midlines were coinciding with each other and the upper midline was matching with the facial midline. A diagnosis of severe skeletal Class II, with dental Angle’s Class II division 1 was made.
Treatment Plan & Objectives
A combined orthodontic and surgical approach was planned to address the severe skeletal Class II. Anterior maxillary osteotomy6 with superior reposition of premaxillary segment was planned to achieve an acceptable facial profile and pleasing appearance. Extraction of upper first premolars was decided to retract the upper incisors. Pre-surgical orthodontics for levelling, aligning and decompensation followed by post-surgical orthodontics for final settling and adjustments were to be carried out, to obtain a Class I occlusion.
Treatment progress
Extraction of 14 and 24 was carried out. A full orthodontic appliance, of 0.022” slot MBT system, Ormco Inspire Ice,was bonded in the upper and lower arches. Second molar bonding was done. Initial 0.016” NiTiarch wires were used for aligning, followed by 0.018” NiTi, 19 X 25” NiTi, and 19 X 25” Stainless Steel arch wires sequentially. In the lower arch initially 0.016” reverse curve NiTi was used to level the arch followed by 0.019 X 0.025”NiTi and 0.019 X 0.025” Stainless Steel wire.
After the pre-surgical objectives were reached, pre-surgical impressions were taken, models poured, mounted on a semiadjustable articulator and model surgery was carried out. Maxillary set-back of 4mmwas executed during the mock surgery and the splint was fabricated.
After preparing the patient, the surgery was carried out and occlusion was sequentially adjusted on the operating table, concomitant to the jaws being repositioned, by using the fabricated splints. The key to the surgical procedurehere was frequent flushing of betadine solution and handling the tissues gently to minimize the surgical trauma as much as possible. Minimizing surgical trauma provides a quick and relatively painless recovery for the patient, with as little post-surgical oedema as possible. Within two days, the patient had made a full and complete recovery and the pre- and post-surgical results could be compared with almost no post-surgical oedema present. Needless to say, the patient was more than satisfied with the outcome and with the relatively trouble-free and fast post-surgical recovery than anticipated.
Within 3 months of the surgery, the post-surgical orthodontic settling and finishing was carried out and the patient was debonded6 months after the surgery. The total duration of the treatmentwas just9 months, including the pre- and post-surgical orthodontics.
Treatment result
The treatment plan worked out as planned and resulted in correction of the severe skeletal Class II deformity of the jaws. The patient had pleasing facial appearance and profile. Lips were competent and lower lip-trap and eversion were eliminated. The incisor exposure, overjet, overbite and curve of spee were restored to normal and a Class I molar, Class I canine, matching midlines and good buccal intercuspationwere obtained. The smile line was consonant and pleasing and overall a satisfactory facial and dental result was achieved.
Discussion
Severe skeletal malocclusions especially Class II, are frequently seen among the Indian population. Most patients refuse to undergo surgical correction of the jaws due to the associated morbidity and risk factors mainly the post-surgicaloedema. They prefer to opt for a camouflage treatment or in some cases due to lack of awareness or financial resources, not get treated at all. By combining Orthodontics and Orthognathic surgery a refined and better treatment alternative can be provided to the patients with skeletal deformities [3,4]. Furthermore, if the surgery is carried out in a manner to minimize post-surgical trauma and oedema, the post-surgical recovery phase for the patient is easier, quicker, painless and less expensive [1,5,6]. The patient can regain full functional ability and get back to work as soon as possible, cutting hospitalization costs and number of days of absence from work. It turns out to be a more personally, socially, psychologically and economically beneficial solution for the patient and their family members (Figures 4,5).
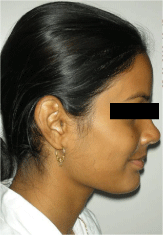
Figure 4: Post surgical extra oral (Profile).
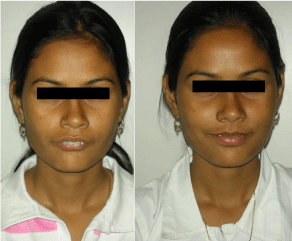
Figure 5: Pre and Post- surgical extra oral frontal view.
In the presented case, the severity of the skeletal malocclusion necessitated the maxillary surgery. Anterior maxillary osteotomy and maxillary superior reposition helped correct the maxillary prominence, reduce the overjet and molar relationship, partially. An intermediate splint used on the operating table during this procedure, acted as a template for guiding the position of the maxilla, facilitated auto-rotation of the mandible to the new maxillary position and allowed the planned intermediate maxillo-mandibular position to be established. By systematic co-ordination between the surgeon and the Orthodontist, the case was planned well since the beginning, and each step charted out in collaboration, which helped reduce the treatment time greatly by avoiding making errors and mistakes during the treatment and having to go back and forth correcting the errors. With the increase in the number of adult patients, such interdisciplinary and professional co-ordination is the need of the day, in being able to offer successful, good quality service to our patients and in maintaining the integrity of our clinical practice.
Conclusion
With the advances in techniques and refinement of surgical and orthodontic procedures, fast and efficient combined orthodonticorthognathic surgery treatment option can be offered to patients with skeletal deformities. Co-ordinated planning between the surgeon and the Orthodontist and due care to handle tissues during the surgical procedure can ensure a quick, painless and hassle-free recovery for the patients, enabling them to resume normal life and work as quick as possible, thus bringing credit to the successful surgeon-orthodontist team and their successful treatment strategy.
References
- Proffit WR, Fields HW, Sarver DM. Contemporary orthodontics. 4th ed. St Louis: Mosby Elsevier; 2007
- Chundamala J, Wright JG . The efficacy and risks of using povidone-iodine irrigation to prevent surgical site infection: an evidence-based review. Can J Surg. 2007; 50: 473-481.
- Arnett GW, Bergman RT . Facial keys to orthodontic diagnosis and treatment planning. Part I. Am J Orthod Dentofacial Orthop. 1993; 103: 299-312.
- Arnett GW, Bergman RT . Facial keys to orthodontic diagnosis and treatment planning--Part II. Am J Orthod Dentofacial Orthop. 1993; 103: 395-411.
- Fonseca RJ, Turvey TA, Marciani RD. Oral and Maxillofacial Surgery: Volume 3. 2nd ed. Elsevier Health Sciences, 2008.
- Epker BN . A modified anterior maxillary ostectomy. J Maxillofac Surg. 1977; 5: 35-38.