
Research Article
Austin J Dent. 2015;2(2): 1019.
Surface and Mechanical Properties of Different Dental Composites
Dalia A Abuelenain¹, Ensanya A Abou Neel1,3,4*and Ayman Al-Dharrab²
¹Department of Operative Dentistry, King Abdulaziz University, Saudi Arabia
²Department of Oral and Maxillofacial Prosthodontics,King Abdulaziz University Jeddah, Saudi Arabia
³Department of Dentistry, Tanta University, Egypt
4Division of Biomaterials and Tissue Engineering, London
*Corresponding author: Ensanya A Abou Neel,Department of Operative Dentistry, King Abdulaziz University, Saudi Arabia
Received: March 18, 2015; Accepted: April 27, 2015; Published: May 05, 2015
Abstract
Due to the unlimited revolution in dental composites technology, a wide variety of materials are available in the market. Materials’ selection is therefore a challenge and requires proper analysis of material properties. This study investigated the compressive, flexure, hardness and surface roughness of six commercially available dental composites (Filtek Z250 and 350 XT and P90, Tetric-N-Ceram and Tetric-N-Ceram Bulk Fill and IPS Impress Direct). The results showed that the highest strength and modulus (compressive and flexure) was observed for Filtek Z250 and 350XT. All tested composites showed bottom/ top hardness ratios above the minimum acceptable level (0.8) and surface roughness below the minimum acceptable level (0.2m) except Filtek P90. Accordingly, for high stress bearing applications, the materials of choice would be Filtek Z250 and Z350 XT. For low stress-bearing applications, IPS Empress and Tetric N-Ceram would be materials of choice. With P90 composites, high plaque accumulations would be expected.
Keywords: Dental composites; Compressive and flexure strength; Vicker hardness; Hardness ratio and surface roughness
Introduction
In recent years, dental composite restorations became the most popular anterior and posterior esthetic resin filling material. This was attributed to the excellent esthetic, near ideal mechanical properties, ease of handling and the rapid progress with enamel and dentin bonding technology that increases the longevity of restorations [1-3]. A wide variety of dental composite filling materials are commercially available in the market. Some of these products are recommended for use in areas bearing high occlusal loads; others are recommended for better esthetic or easy handling/less application time or less polymerization shrinkage. These products vary in composition, initiator/activator system, filler type, loading, and particle size. It has been proved that these variations dramatically influence the composite properties [1,4-7] e.g., degree of resin conversion [8,9]. Accordingly, they put a burden on dental practitioners when selecting a material that fulfills the practical and clinical needs.
Previous work by Gajewski et al. [8] showed that different polymers would have different degree of conversion, reaction kinetics and physical and mechanical properties. Surface hardness would also vary with the degree of conversion [10-12]. Bottom/top hardness ratio was used as an indicator of bottom/top degree of conversion [5]. Due to the unlimited revolution in dental composites technology, a wide variety of materials are available in the market. Investigating the materials’ properties and performance should continue to help dental practitioners select the optimum composite material with the highest possible tolerance to the harsh oral environment.
The aim of the present study was to investigate the compressive and flexure properties as well as surface hardness, hardness ratio (as an indication of bottom to top conversion ratio) and roughness of six different commercially available dental composites having different organic matrix, filler loading and filler types, under the same curing and testing conditions.
The null hypothesis was that, there is no difference in mechanical properties, surface hardness, bottom/top hardness ratio and roughness between different commercially available composite when subjected to the same curing and testing conditions.
Materials and Methods
Six different commercially available composites materials were used throughout this study. Details of the studied composite are presented in Table 1. To standardize the procedures, all samples were cured using the same protocol with a light-emitting diode curing unit (3M ESPE Elipar, Germany) with a 10 mm diameter tip. The light intensity of 1800 mW/cm2 as measured with a specific radiometer (LITEX 682 Dentamirica, USA) was used for light curing. The intensity of the light was checked between samples.
Product Name/Code
Type
Manufacturer
Monomers
Fillers
Filtek Z250/Z250
Universal hybrid
3M/ESPE
Bis-GMA, UDMA Bis-EMA
Zirconia/ Silica
Filtek Z350 XT/Z350
Nano-filled
3M/ESPE
Bis-GMA, UDMA TEGDMA, PEGDMA, Bis-EMA
20 nm nanosilica fillers,
5.00–20.00 nm agglomerates zirconia/silica particles,
0.60–1.40 um clusters particle size
Filtek P90/P90
Micro-Hybrid/ Silorane based composite
3M/ESPE
silorane
Quartz particles, yttrium fluoride
Tetric N-Ceram
Bulk Fill/NCB
Hybrid
Ivoclar Vivadent
Dimethacrylates
Barrium glass, ytterbium trifluoride, mixed oxides
Tetric N-Ceram/NC
Nano-hybrid
Ivoclar Vivadent
Dimethacrylates TEGDMA
Barrium glass, ytterbium trifluoride, mixed oxides and copolymers
Table 1: Products information for tested dental composites. Bis-GMA, bisphenol A diglycidyl methacrylate; Bis-EMA, ethoxylated bisphenol A glycol dimethacrylate; UDMA, urethane dimethacrylate; TEGDMA, triethylene glycol dimethacrylate; PEGDMA, polyethylene glycol dimethacrylate; silorane represents a mixture that is made of both siloxane and oxirane structural moieties.
Compression test
Thirty six specimens were prepared (n=6 for each composite), using a cylindrical split Teflon mold with 8 mm height and 4 mm diameter according to ISO 4049 specification for polymer-based restorations [13]. Composite were packed into the Teflon mold in 4 increments of 2mm each. Each increment was cured for 40 seconds. The bottom increment was pressed into the mold against a glass slab covered with a celluloid strip. Once the top increment was applied, its surface was covered by a celluloid strip and then a glass slab to provide a flat, smooth surface and to extrude the excess material. The glass slabs and strips were then removed; the excess material was removed with a sharp scalpel. Specimens were then stored in deionized water at 37°C for 24 hours before testing.
The dimensions of each specimen were measured with micrometer accurate to 0.01mm. The specimens were subjected to a compression test at a crosshead speed of 0.25mm/min and 50kN load using the Instron testing machine (Instron 5969, USA). The compressive strength (MPa), modulus (GPa) and strain at break (%) were measured using the Bluehill 3 software.
Three-point bending test
Thirty six specimens were prepared (n=6 for each composition), by backing composite into a rectangular split Teflon mold (2x2x25mm3) according to ISO 4049 specification for polymer-based restorations [13]. A celluloid strip was placed on the top and bottom surface of each specimen; and the mold was sandwiched between two glass slides and tightened at both ends using paper clamps. This was to obtain flat and smooth surfaces of each specimen and also allow for extrusion of excess materials. Each specimen was then subjected to 4 overlapping 20 seconds curing cycles from each side. The cured specimen was then removed from the mold; excess materials were removed with a sharp scalpel. The cured specimens were then stored for 24 hours in de-ionized water at 37°C±1 prior to testing.
The dimension of each specimen was determined with a micrometer accurate to 0.01 mm prior to the three-point bending test. This test was carried out using the Instron testing machine (Instron 5944, USA) with a span of 20 mm at a crosshead speed of 0.25mm/ min and 2 KN load. The flexure strength (MPa), modulus (GPa) and strain at break (%) were measured using Bluehill 3 software.
Vickers micro-hardness number and hardness ratio
Thirty specimens were prepared (n=5 for each composition), using cylindrical metal molds of 2 mm height and 5 mm diameter. Composite were packed into the mold and covered with celluloid strips and compressed with glass slide to render the surface flat as discussed above. The composite were cured from the top surface only for 40 seconds. Samples were stored dry at room temperature for 7 days prior to testing. Vickers hardness numbers were determined using a micro-hardness tester (Micromet 6040, Buehler, USA) under a load of 100 g and dwell time of 10 seconds. Three readings were recorded for each surface (top and bottom); the hardness number was presented as the average of these six readings.
To calculate the hardness ratio, the following equation was used:
Where VHNbottom and VHNtop are the Vicker hardness number of the bottom and top surface respectively.
Surface roughness
Surface roughness of all tested dental composites was measured (n=5) with a surface scanning interferometry (ContourGT, Bruker, USA) that was calibrated according to the manufacturer’s instructions. Vision64 software (Bruker, USA) was used to analyze the obtained data. Ra, the arithmetic mean of the absolute values of the collected roughness data points.
Statistical analysis
Results were subjected to one way ANOVA and Tuky’s post hoc test to delineate areas of significance (p<0.05) using SPSS.16 software.
Results
Compression test
Figure 1a shows the stress-strain curves of all tested composites. The stress-strain curves were characterized by the presence of toein region followed by an elastic region. Each composite was broken under compression once the applied stress become equals to its elastic limits indicating the brittle behavior of all tested composites.
Regarding the compressive strength (MPa), Filtek Z250 showed the highest compressive strength. However, there was no significant difference in the mean compressive strength of Filtek Z250 and Tetric-N-Ceram or Filtek Z350 XT (p>0.05). There was a significant difference between Filtek Z250 and other tested composites. So, the compressive strength followed this order: Filtek Z250>Tetric-NCeram> Filtek Z350 XT>IPS Empress Direct>Tetric-N-Ceram Bulk Fill>Filtek P90 – Table 2.
Material/Code
Compressive strength (MPa)
Mean ± SD
Compressive Modulus (GPa)
Mean ± SD
Flexure strength (MPa)
Mean ± SD
Flexure Modulus (MPa)
Mean ± SD
Top VHN
Mean ± SD
Bottom VHN
Mean ± SD
Hardness Ratio
Mean ± SD
Surface Roughness
(Ra, nm)
Filtek Z250/Z250
318±37.9
9.3±1.3
138.2±23.5
12.4±2.4
77.7±0.8
77.5±1.6
0.99±0.01
27.4±4.3
Filtek Z350 XT/Z350
291.7±23.6
8.5±0.7
127.5±13.8
11.6±1.4
77.1±2
69.7±2.4
0.91±0.03
114.0±18.0
Filtek P90/P90
252.5±51.0
6.2±0.6
99.1±16.7
9.1±1.2
51.3±3.4
46.3±3
0.90±0.04
324.7±63.4
Tetric N-Ceram
Bulk Fill/NCB
260.0±31.9
7.3±0.8
95.1±8.1
8.3±0.3
43.3±2.8
39.6±4
0.89±0.08
89.5±14.0
Tetric N-Ceram/NC
308.6±29.3
6.2±0.5
82.9±15.6
8.9±0.5
34.6±3.1
30.7±4.6
0.89±0.08
88.9±24.2
IPS Empress Direct/IPS
272.0±32.9
5.3±0.9
98.6±7.6
6.8±0.5
30.5±1.2
27.7±1.8
0.91±0.06
81.2±19.5
Table 2: Compressive, flexure properties, Vicker Hardness Number (VHN) of the top and bottom surface, hardness ratio and surface roughness of tested dental composites.
Regarding the compressive modulus (GPa), Filtek Z250 showed the highest modulus. The compressive modulus of Filtek Z250 was significantly (p<0.05) higher than other tested composites except Filtek Z350 XT. There was no significant difference in the modulus value between Tetric N-Ceram and Filtek P90. The modulus followed this order: Filtek Z250>Filtek Z350 XT>Tetric-N-Ceram Bulk Fill>Tetric-N-Ceram=Filtek P90>IPS Empress Direct – Table 2.
Regarding the strain at break (%), it followed the following order: IPS Empress Direct (10±1)=Tetric N-Ceram (10±1)>Filtek P90 (9±1)>Tetric N-Ceram Bulk Fill (8±1)>Filtek Z250 (6±0.2)>Filtek Z350 XT (5±0.5).
Three-point bending test
Figure 1b showed the stress-strain curves of tested composites under the three-point bending test. The stress-strain curves showed the brittle behavior of tested composites.
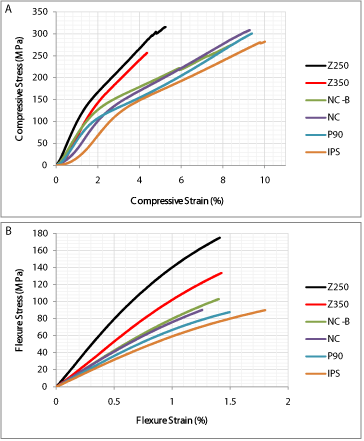
Figure 1: Stress-strain curves of the tested dental composites under (a)
compression and (b) three-point bending test.
Regarding the flexure strength (MPa), Filtek Z250 showed the highest flexure strength; its strength was significantly (p<0.05) higher than other tested composites except Filtek Z350 XT. The flexure strength followed the following order: Filtek Z250>Filtek Z350 XT>Filtek P90>IPS Empress Direct>Tetric-N-Ceram Bulk Fill>Tetric-N-Ceram – Table 2.
Regarding the flexure modulus (GPa), Filtek Z250 showed the highest flexure strength; its strength was significantly (p<0.05) higher than other tested composites except Filtek Z350 XT. The flexure modulus followed the following order: Filtek Z250>Filtek Z350 XT>Filtek P90>Tetric-N-Ceram>Tetric-N-Ceram Bulk Fill>IPS Empress Direct– Table 2.
Regarding the strain at break (%), it followed this order: IPS Empress Direct (2 ±0.1)>Filtek Z250 XT (1.3 ±0.3)>Filtek Z250 (1±0.1)=Filtek P90 (1±0.2)=Tetric-N-Ceram (1±0.2)=Tetric-NCeram Bulk Fill (1±0.1).
Vickers micro-hardness number and degree of conversion
The average VHN as measured from both the top and bottom surface followed this order: Filtek Z250>Filtek Z350 XT>FiltekP90>Tetric-N-Ceram Bulk Fill>Tetric-N-Ceram>IPS Empress Direct– Table 2. Again, Filtek Z250 showed significantly (p<0.05) higher hardness than other tested composites except Filtek Z350 XT.
The hardness ratio followed this order: Filtek Z250>IPS Empress Direct>Filtek P90>Filtek Z350 XT>Tetric-N-Ceram>Tetric-NCeram Bulk Fill– Table 2. Again, Filtek Z250 showed significantly (P<0.05) higher hardness ratio than other tested composites. Generally the hardness ratios of all tested composites are above the minimal acceptable level (0.8) as indicated in literatures.
Surface roughness
The average Ra values as measured from five different readings for each composite followed this order: FiltekP90>Filtek Z350 XT>Tetric-N-Ceram Bulk Fill>Tetric-N-Ceram>IPS Empress Direct>Filtek Z250–Table 2. P90 showed the highest significant surface roughness, Z250 however has the lowest significant surface roughness.
Discussion
Long-term performance of dental composites is determined by their physical and mechanical properties. This study aimed to investigate the compressive and flexure properties, which are important indicators of fracture resistance of brittle materials [14], of commercially available six dental composites. Surface properties such as hardness (i.e. resistance to micro-indentation, wear and abrasion [7,14] and roughness were also measured. The hardness ratio may indicate the bottom/top degree of monomer conversion [5,9]. Surface roughness of dental composites has an important effect on the initial adhesion and retention of dental plaques [15,16]. A subsequent risk of dental caries and periodontal diseases would be expected with rough surfaces [17-21]. Surface roughness also affects the color [22], gloss [23] and staining susceptibility [24] of dental composites.
The composites used in this study vary in resin matrix and filler type/loading/particle size. Filtek Z250, Z350 XT and P90 are supplied by the same manufacturer (3M Company). Both Filtek Z250 and Z350 XT vary mostly in the filler particle size; Filtek Z350 XT has nanosized filler particles and nanoclusters. Filtek P90, however, has different resin matrix (silorane-based), filler type, loading and size which render this material a highly different from both Filtek Z250 and Z350 XT. The other three composites, Tetric N-Ceram, Tetric N-Ceram Bulk and IPS Empress are supplied by Ivoclar Vivadent; they have a slight variation in filler loading.
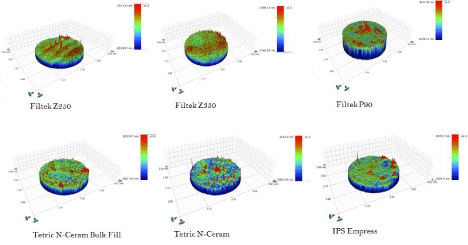
Figure 2: Surface roughness of the tested dental composites.
As the results indicated, the micro-hybrid Filtek Z250 has the highest mechanical properties (in term of compressive and flexure strength and modulus), surface hardness, highest degree of conversion (as indicated by hardness ratio) but the lowest surface roughness than other tested formulations. Similar performance was observed for the nano-filled Filtek Z350 XT composite except that Filtek Z350 XT has significantly lower hardness ratio than Filtek Z250. The similarity in behavior of Filtek Z250 and Filtek Z350 XT could be related to the similarity in resin matrix, filler type and loading. The presence of nanofillers and nanoclusters in Filtek Z350 XT composites could affect the light reflection and hence the degree of conversion. A significant reduction in mechanical properties, hardness, and hardness ratio was observed for Filtek P90 that was provided by the same company as Filtek Z250 and Filtek Z350 XT. This was expected due to the variation in resin matrix, filler type, loading and size. This finding was in agreement with other studies [7].
Regarding hybrid composites (Tetric-N-Ceram Bulk fill), and Nano-hybrid IPS Empress, they have lower mechanical properties than Filtek Z250 and Z350 XT. Nano-hybrid Tetric N-Ceram composites, however, have comparable compressive strength to Filtek Z250 and Z350 XT. It has been also evident that the nanohybrid Tetric N-Ceram has higher compressive and flexure properties than the micro-hybrid Tetric N-Ceram Bulk Fill. This finding was in agreement with other study [25] and it could be attributed to the higher filler loading and nano-filler dimensions in Tetric N-Ceram. Accordingly, the use of the bulk fill composite in load-bearing areas and as a core material would be questionable. The lowest compressive and flexure moduli but the highest strain% at break was detected for IPS Empress indicating its greatest flexibility and hence resistance to permanent shape changes before fracture.
Surface hardness was measured after 7 days of curing to allow time for post-cure conversion [26]. The bottom/top hardness ratio in this study was obtained from 2 mm thick samples. As observed in a previous study, the bottom/top hardness ratio of 0.8 corresponds to a 0.9 bottom/top degree of conversion [5]. As seen from this study, all tested composites have bottom/top hardness ratio of more than 0.8 (i.e., above the minimum required level specified in literatures, indicating a bottom/top degree of conversion of more than 0 [5]. The highest hardness ratio was observed for Filtek Z250. More interestingly, the bulk fill composite, Tetric N-Ceram Bulk Fill, has similar hardness ratio to its incremental fill Tetric N-Ceram composites indicating that there is no concern about the degree of conversion with this bulk fill material.
Although, similar protocol was used for samples preparation, the highest surface roughness was observed for Filtek P90. This could be attributed to the presence of silorane-based matrix which has different viscosity to other tested methacrylate-based composites [27]. Generally, surface roughness values obtained for all tested composites are far below the maximum level for bacterial accumulation [28] except for Filtek P90 indicating the high risk of recurrent decay with Filtek P90.
Conclusion
Variations in resin matrix and filler technology influenced the mechanical and physical behavior of different composite materials. Selection of dental composites can be undertaken with high precision when the material properties are well established. Based on the finding from this study, for high stress bearing applications, the materials of choice would be Filtek Z250 and Z350 XT. With low stress-bearing applications when a high resiliency and flexibility are required, e.g., cervical and abfraction lesions, IPS Empress and Tetric N-Ceram could be the material of choice. All tested composites showed hardness ratio above the minimum required level (0.8) and surface roughness below the minimum required level (0.2 μm) except Filtek P90.
Acknowledgment
This project was funded by the Deanship of Scientific Research (DSR), King Abdulaziz University, Jeddah, under grant no (3-165-35- RG). The authors therefore acknowledge with thanks DSR technical and financial support. The authors would also like to acknowledge the “Advanced Technology Dental Research Laboratory” at King Abdulaziz University, Faculty of Dentistry.
References
- Cramer NB, Stansbury JW, Bowman CN. Recent advances and developments in composite dental restorative materials. J Dent Res. 2011; 90: 402-416.
- Ferracane JL. Resin composite state of the art. Dent Mater. 2011; 27: 29-38.
- Kim KL, Namgung C, Cho BH. The effect of clinical performance on the survival estimates of direct restorations. Restor Dent Endod. 2013; 38: 11-20.
- Arcis RW, Lopez-Macipe A, Toledano M, Osorio E, Rodriguez-Clemente R, Murtra J, et al. Mechanical properties of visible light-cured resins reinforced with hydroxyapatite for dental restoration. Dent Mater. 2002; 18: 49-57.
- Bouschlicher MR, Rueggeberg FA, Wilson BM. Correlation of bottom-to-top surface microhardness and conversion ratios for a variety of resin composite compositions. Oper Dent. 2004: 29: 698-704.
- Jayanthi N, Vinod V. Comparative evaluation of compressive strength and flexural strength of conventional core materials with nanohybrid composite resin core material an in vitro study. J Indian Prosthodont Soc. 2013; 13: 281-289.
- Porto IC, de Aguiar FH, Brandt WC, Liporoni PC. Mechanical and physical properties of silorane and methacrylate-based composites. J Dent. 2013; 41: 732-739.
- Gajewski VE, Pfeifer CS, Froes-Salgado NR, Boaro LC, Braga RR. Monomers used in resin composites: degree of conversion, mechanical properties and water sorption/solubility. Braz Dent J. 2012; 23: 508-514.
- Poggio C, Lombardini M, Gaviati S, Chiesa M. Evaluation of Vickers hardness and depth of cure of six composite resins photo-activated with different polymerization modes. J Conserv Dent. 2012; 15: 237-241.
- Sabatini C. Comparative study of surface microhardness of methacrylate-based composite resins polymerized with light-emitting diodes and halogen. Eur J Dent. 2013; 7: 327-335.
- Ferracane JL. Correlation between hardness and degree of conversion during the setting reaction of unfilled dental restorative resins. Dent Mater. 1985; 1: 11-14.
- Santos GB, Medeiros IS, Fellows CE, Muench A, Braga RR. Composite depth of cure obtained with QTH and LED units assessed by microhardness and micro-Raman spectroscopy. Oper Dent. 2007; 32: 79-83.
- ISO 4049: 2000. Polymer-based filling, restorative and luting materials Geneva, Switzerland: International Organization for Standardization.
- Sakaguchi R L. Craig's Restorative Dental Materials 13 ed Philadelphia: ELSEVIER MOSBY. 2012.
- Ionescu A, Wutscher E, Brambilla E, Schneider-Feyrer S, Giessibl FJ, Hahnel S. Influence of surface properties of resin-based composites on in vitro Streptococcus mutans biofilm development. Eur J Oral Sci. 2012; 120: 458-465.
- Mei L, Busscher HJ, van der Mei HC, Ren Y. Influence of surface roughness on streptococcal adhesion forces to composite resins. Dent Mater. 2011; 27: 770-778.
- Einwag J, Ulrich A, Gehring F. [In-vitro plaque accumulation on different filling materials]. Oralprophylaxe. 1990; 12: 22-25.
- Quirynen M, Bollen CM. The influence of surface roughness and surface-free energy on supra- and subgingival plaque formation in man. A review of the literature. J Clin Periodontol. 1995; 22: 1-14.
- Quirynen M, Bollen CM, Papaioannou W, Van Eldere J, van Steenberghe D. The influence of titanium abutment surface roughness on plaque accumulation and gingivitis: short-term observations. Int J Oral Maxillofac Implants. 1996; 11: 169-178.
- Quirynen M, Marechal M, Busscher HJ, Weerkamp AH, Darius PL, van Steenberghe D. The influence of surface free energy and surface roughness on early plaque formation. An in vivo study in man. J Clin Periodontol. 1990; 17: 138-144.
- Gedik R, Hurmuzlu F, Coskun A, Bektas OO, Ozdemir AK. Surface roughness of new microhybrid resin-based composites. J Am Dent Assoc. 2005; 136: 1106-1112.
- Ghinea R, Ugarte-Alvan L, Yebra A, Pecho OE, Paravina RD, Perez Mdel M. Influence of surface roughness on the color of dental-resin composites. J Zhejiang Univ Sci B. 2011; 12: 552-562.
- Ohara N, Koizumi H, Matsumoto Y, Nakayama D, Ogino T, Matsumura H. Surface roughness and gloss of indirect composites etched with acidulated phosphate fluoride solution. Acta Odontol Scand. 2009; 67: 313-320.
- Berger SB, Palialol AR, Cavalli V, Giannini M. Surface roughness and staining susceptibility of composite resins after finishing and polishing. J Esthet Restor Dent. 2011; 23: 34-43.
- Leprince JG, Palin WM, Vanacker J, Sabbagh J, Devaux J, Leloup G. Physico-mechanical characteristics of commercially available bulk-fill composites. J Dent. 2014; 42: 993-1000.
- Abou Neel EA, Palmer G, Knowles JC, Salih V, Young AM. Chemical, modulus and cell attachment studies of reactive calcium phosphate filler - containing fast photo-curing, surface – degrading, polymeric bone adhesives. Acta Biomaterialia. 2010; 6: 2695-2703.
- Pereira R, Aguiar FHB, Oliveira BBMN, Ambrosano GMB, Lima DANL, Baron GMM, et al. Evaluation of surface roughness of resin-based composites submitted to different light activation protocols and bleaching agents Journal of Research in Dentistry. 2013; 1: 309-315.
- Bollen CM PW, Van Eldere J, Schepers E, Quirynen M, van Steenberghe D. The influence of abutment surface roughness on plaque accumulation and peri-implant mucositis. Clin Oral Implants Res. 1996; 7: 201–211.