
Case Report
Austin J Dent. 2016; 3(4): 1043.
Dentin Hypersensitivity Related to Apical Fenestration
Gonzalez R¹, Zeng Q², Nissan R², Yesilsoy C¹ and Yang MB¹*
¹Department of Endodontology, Temple University, USA
²Department of Operative Dentistry and Endodontics, Sun Yat-sen, University, China
*Corresponding author: Maobin Yang, Department of Endodontology, Kornberg School of Dentistry, Temple University, 3223 North Broad Street, Philadelphia, PA 19140, USA
Received: July 20, 2016; Accepted: August 31, 2016; Published: September 02, 2016
Abstract
Dentinal hypersensitivity is a common clinical symptom which is caused by multiple factors. Apical anatomic abnormality including apical fenestration could contribute to dentin exposure, thus may lead to tooth sensation. The purpose of the present case report was to describe a case with initial diagnosis of “dentinal hypersensitivity” caused by apical fenestration and confirmed by cone beam computed tomography, suggesting that apical anatomical morphology should be considered after excluding all other obvious possible etiologies in patients with dentinal hypersensitivity.
Keywords: Dentinal hypersensitivity; Apical fenestration; Cone beam computed tomography
Introduction
Dentinal hypersensitivity (DH) is a pulp related painful condition when dentin is exposed to various stimuli that cause activation of nerve fibers. American Association of Endodontists (AAE) defines DH as “A short, exaggerated, sharp painful response elicited when exposed dentin is subjected to thermal, mechanical or chemical stimuli” [1] (AAE Glossary of Endodontic Terms). Clinically, Tooth hypersensitivity, or more precisely dentinal hypersensitivity is described as an exaggerated response to non-noxious sensory stimuli [2]. The prevalence of DH in the adult population has been reported ranging from 4-74% depending on the types of study designs that vary from patient questionnaires to clinical examinations [3-6].
The exposure of dentinal tubules can be caused by multiple predisposing factors, including: 1) Cemento-enamel junction anatomic profiles with a gap between enamel and cementum that transmit temperature and induce dentin sensation. 2) Tooth wear, abrasion, erosion, attrition, or other mechanical etiologies cause the loss of enamel or cementum structures and exposure of dentin [7]. 3) Loss of periodontal attachment due to the gingival recession or periodontal disease may result in the exposure of root surface, which is the most common etiology of exposed radicular dentin [5,8]. In addition, thin alveolar cortex, fenestration of alveolar bone, trauma, orthodontic therapy or periodontal surgery can contribute to the loss of periodontal attachment and denudation of the root [7]. 4) Even in an intact tooth, nerve fibers can be sensitized to stimuli in the presence of inflammatory mediators [9].
The etiology of DH is multifactorial. To date, the majority of studies support the hydrodynamic theory that stimuli cause a rapid movement of fluid in the dentinal tubules, which mechanically distorts the nerve fibers at the pulp-dentin junction, and activates neuronal fibers located in or near the dentinal tubules [10]. The density and size of dentinal tubules are also the contributing factors and have positive correlation with the pain responses induced from exposed dentin surfaces [11].
A fenestration is defined as “window-like opening or defect in the alveolar plate of bone”, which frequently exposes a portion of the root and usually locates on the facial aspect of the alveolar process [12]. Apical fenestration of a root is usually asymptomatic, but it can become symptomatic after the root canal treatment when the obturation materials are overfilled [12,13]. The diagnosis of apical fenestration can be challenging. In some cases, it may be misdiagnosed as persistent apical periodontitis [14]. Here we report a challenging diagnostic case of a tooth with temperature hypersensitivity. A correct diagnosis and appropriate treatment plan were achieved by using a combination of clinical exam, radiography and cone beam computed tomography (CBCT).
Case Presentation
A 50-year-old female was referred to the Department of Endodontology at Kornberg School of Dentistry, Temple University. The patient reported sharp pain from the maxillary left area provoked by cold liquids during the past one year and a half. Routine oral hygiene instructions, root scaling and root planning were performed 6 months ago, and there was no improvement concerning her chief complaint. Medical History was non-contributory for diagnosis.
Intraoral examination revealed adequate oral mucosal appearance and normal gingival condition. Tooth #11 had a wear-off on the cusp and was absent of any restorations or caries. It had a slightly increased response to cold test compared with the control teeth (#10, #13), but was not lingering. Tooth #12 was devoid of any restorations, caries or attrition, and the cold test showed more intense response than #11 but still not lingering. A probing depth of 4.5mm was found in the mesial-palatal area of #12, and the patient felt very sensitive upon probing in this area. Both #11 and #12 had a normal response to palpation and percussion. Other teeth from this same quadrant were normal in the examination (Figure 1).
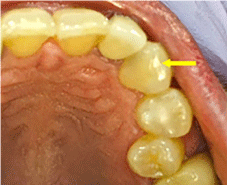
Figure 1: Occlusal view of left maxillary anterior teeth. Teeth #11 had a
slightly wear-off on the cusp (yellow arrow). Tooth #12 was absent of any
restoration, caries or attrition. Other teeth from the same quadrant were
normal.
Radiographic evaluation showed that #11 had a wear-off cusp, with a curved root apex. A mesial cervical concave on the mesial of tooth #12 was concurrent with the 4.5 mm pocket detected during probing evaluation. No other abnormal radiographic signs were detected on these teeth or adjacent teeth (Figure 2A and B).
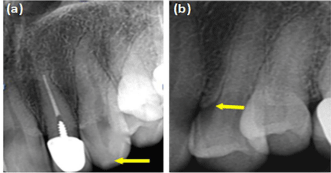
Figure 2: (a) Periapical radiograph of tooth #11. It showed the wear-off of
cusp (yellow arrow), with a curved root apex; (b) Periapical radiograph of
tooth #12. A concavity was seen on the mesial cervical of tooth #12 (yellow
arrow).
A periodontal consultation was obtained by a periodontist. Trauma from occlusion was diagnosed for tooth #12. Based on the results of the clinical and radiographic examinations, the diagnosis of #12 was: reversible pulpitis and dentin hypersensitivity, possibly due to the traumatic occlusion and cervical recession. The occlusal adjustment was made on tooth #12 and desensitizing paste Sensodyne was prescribed. At the three-week follow-up visit, the patient reported a little improvement on symptoms. Both #11 and #12 were still sensitive upon cold test and there was no improvement of sensitivity when probed in the mesial pocket of tooth #12.
To understand the extent of bone loss on the mesial of tooth #12, CBCT was prescribed for this area. The frontal CBCT image on maxillary left quadrant revealed an adequate crown anatomy on #12 with a well demarcated concavity mesially on the cervical area (Figure 3A), which was also seen at the palatal view of tooth #12 (Figure 3B). The root showed an adequate shape (Figure 3C).
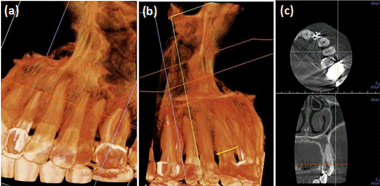
Figure 3: (a) CBCT anterior view of tooth #12. Mesial concavity of #12 was
detected; (b) CBCT palatal view of #12. Mesial cervical bone loss on tooth
#12 was present; (c) CBCT axial view at cervical level of tooth #12. It showed
adequate circumferential contour.
Combining the above CBCT images with clinical examination, we reached the final diagnosis of dentin hypersensitivity for tooth #12 with reversible pulpitis due to the exposed dentin on mesial cervical area. Since there was no improvement of symptom after adjustment of occlusion and application of Synsodyne for 3 weeks, the elective root canal treatment for #12 was proposed.
Patient consent was obtained. Under local anesthesia, rubber dam placement and cavity access were performed. Two canals were located in #12. Working length was determined using an apex locator and confirmed with a periapical radiograph. The two canals were instrumented with Endo Sequence rotary files (Brasseler USA) up to a size of 35/.04 taper, and irrigated with 2.5% sodium hypochloride (NaOCl) followed with 17% EDTA. Each canal was dried and obturated with vertical condensation technique (Figure 4). And the resin restoration was performed.
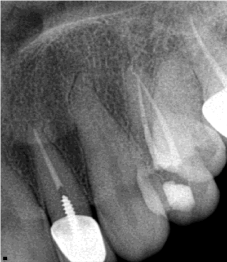
Figure 4: Postoperative apical radiography of tooth #12.
After two weeks, the patient reported less pain when she drank cold but the symptom was not completely resolved. Cold test indicated that tooth #12 had a negative response to cold, but tooth #11 was still slightly sensitive to cold without lingering pain. To further explore the etiology of the hypersensitivity, we checked #11 on CBCT from different angles of views and found that the frontal image of CBCT showed tooth #11 had a root dilaceration and a decrease of bone density at the apical third (Figure 5A). A fenestration of buccal cortical bone was present at the apical of the root from the saggital section view (Figure 5B), which was confirmed by an axial view (Figure 5C). A cold test was repeated by placing a cold cotton pellet on the buccal gingiva around the apical third of the root, and the patient reported intense response. A diagnosis was concluded tooth #11 with reversible pulpitis due to the root fenestration at the buccal bone.
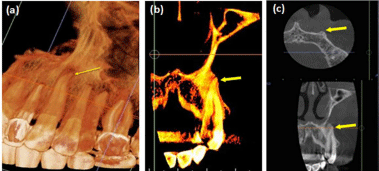
Figure 5: a) CBCT frontal view of tooth #11. Root dilaceration and a
decrease of bone density at the apical third were seen; (b) CBCT sagittal
view of tooth #11. A fenestration was present at the apical third of the root; (c)
CBCT axial view of #11 at the level of the apical third. Little cortical bone was
covering the tip of the root.
After communication with the patient, elective root canal treatment was proposed. After achieving the consent, elective root canal treatment was initiated on tooth #11, following the same procedures for tooth #12, but two-visit treatment was performed instead of one-visit, and Ca(OH)2 was used as an intracanal medicament. One week after the first visit, the patient reported that the symptom disappeared and no more pain occurred upon cold in this area. We proceeded to complete the obturation for tooth #11. Considering the fenestration of apex and vital pulp status, the root canal was instrumented and obturated 2mm short from the apex (Figure 6A).
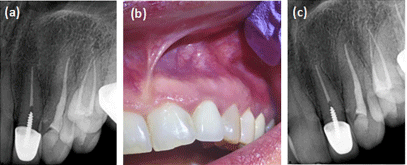
Figure 6: (a) Postoperative apical radiography of tooth #11; (b) Buccal view
of area of #11 and #12 in one-year follow-up. Normal mucosa and gingival
tissue were showed. (c) Apical radiography of tooth #11 and #12 in one-year
follow-up. Normal periapical tissue was seen.
On a two-week follow-up, the patient showed no sensitivity to cold test on teeth #11 and #12. One year after root canal treatment, the patient remained free of symptoms. Intraoral exam showed normal mucosa and gingival tissue around tooth #11 and #12 (Figure 6B). All remaining teeth present normal to cold tests. Normal periapical tissue was seen from apical radiography (Figure 6C).
Discussion
Etiology of DH can be complicated and multifactorial. Loss of enamel, cementum, gingival recession and loss of attachment are the common causes of DH [15]. DH has been reported frequently occurring on occlusal and incisal surfaces which are affected by all types of tooth wear (attrition, erosion and abrasion) [8]. Gingival recession, periodontal disease and periodontal treatment can lead to the exposure of radicular dentin [16]; Occlusal trauma is also considered to be a latent factor for root hypersensitivity since it may destruct the supporting tissue around the tooth to exposure of the root surface dentin or cause periodontal defect, leading to the sensitization of the nerve fibers in dental pulp and peridontium
Proper diagnosis of dentinal hypersensitivity might be a challenge. Vitality tests are extremely valuable in identifying pulp conditions of the offending teeth. Cold test in particular is an essential diagnostic tool for determining the vitality of pulp, and is considered the relative accurate method compared to electrical pulp test and other testing [17]. Common agents used for cold tests include ice, refrigerant sprays, Endoice and CO2 snow [18]. In the present case, tooth #12 was diagnosed for the sensitivity based on periodontal reasons: 1) a 4.5mm pocket on the mesial palatal region; 2) intense sensitivity to cold; 3) trauma from occlusion diagnosed by periodontist, which can be considered as the etiology of tooth sensation; 4) periapical radiography and CBCT detected mesial bone loss due to occlusal trauma. After occlusion adjustment and application of Sensodyne for three weeks, a little improvement to the sensitivity was reported. With this clinical information along with the fact that the response to cold test was more intense on tooth #12, the root canal treatment was performed on tooth #12 first. A follow-up report showed that sensitivity was improved but still remained on tooth #11. The following clinical examination confirmed that the anatomical factor of an apical fenestration contributed to the hypersensitivity of tooth #11. Although apical fenestrations are usually asymptomatic, this case suggested it may cause tooth hypersensitivity via directly transporting temperature to the pulp tissue near the fenestration site.
Apical fenestration is a condition characterized by progressive resorption of alveolar bone around one or more teeth, leaving the apex of teeth covered with only mucosa. The frequency of apical fenestration is between 7.5 to 20% [14]. The overall prevalence of root fenestration was higher in the maxilla (5.37% of teeth) than in the mandible (1.00% of teeth). Apical fenestrations occur most frequently in maxillary first premolars (10.46%), followed by maxillary lateral incisors (7.80%) and maxillary canines (7.58%). It was also reported that root fenestration appeared significantly more often on the labial/ buccal side (99.98%) than the palatal/lingual side (0.02%) [18]. The possible causes of apical fenestration relate to anatomical factors, including root prominence, tooth/jaw ratio, tooth malposition, agerelated changes of the alveolar bone. Orthodontic tooth movement as well as occlusal dysfunction, such as heavy occlusal force, may be contributory to the development of fenestration [14,20]. Apical fenestration can be a result of trauma as well, which has been reported in some cases involving primary teeth [21,22].
Fenestration is usually symptom-free, although some case reports demonstrated that fenestration might give rise to pain after a root canal treatment was done inappropriately [12,14]. The correlation between hypersensitivity and the presence of a fenestration has not yet been reported. In the present case, the bony fenestration resulted in part of the root only covered with mucosa, leaving it unprotected. Temperature changes in oral cavity may cause gradual change in the pulp, compromising its ability to sustain and adapt to temperature variations. Elective root canal treatment is recommended for this type of dentin hypersensitivity. It is important to note that root canals should not be overfilled based on the previous reports [13,14].
Apical radiography is not sufficient for the assessment of bone structures due to the limitation of the two-dimensional images, possible image distortion and blurring of anatomic structures. CBCT provides considerably superior diagnostic results than the conventionally intraoral radiograph due to the three-dimensional presentation of anatomic structures such as anatomical variances of root canals, root fractures, periapical pathologies [14,19,23]. In the present case, CBCT was significantly helpful to diagnose the fenestration defect.
Further research is needed to investigate the correlation between the presence of apical fenestration and potential damages to the neurovascular change of the pulp, in order to understand why some apical fenestration become symptomatic while other cases remain asymptomatic.
Conclusion
Dentinal hypersensitivity can be caused by common factors such as gingival recession, tooth wear and occlusal trauma. This case suggests that dentists should also consider the possibility of apical anatomic structure when examining patients with dentin hypersensitivity, especially when common etiologies fail to explain the symptom. Elective root canal treatment is an optional approach to treat this type of hypersensitivity. Follow-up should be performed to assure no pain arising after root canal treatment. Further research needs to be done to study the possibility of tooth nerve damage in correlation with the existence of root apical fenestration.
References
- AAE. Glossary of endodontic terms 2007.
- Bartold PM. Dentinal hypersensitivity: a review. Aust Dent J. 2006; 51: 212- 218.
- Rees JS. The prevalence of dentine hypersensitivity in general dental practice in the UK. J Clin Periodontol. 2000; 27: 860-865.
- Wang Y, Que K, Lin L, Hu D, Li X. The prevalence of dentine hypersensitivity in the general population in China. J Oral Rehabil. 2012; 39: 812-820.
- Naidu GM, Chaitanya RK, Sirisha NR, Sree SY, Raj Kumar CK, Satti NR. Prevalence of Dentin Hypersensitivity and Related Factors Among Adult Patients Visiting a Dental School in Andhra Pradesh, Southern India. J Clin Diagnostic Res. 2014; 8:48-51.
- Orchardson R, Collins WJ. Clinical features of hypersensitive teeth. Br Dent J. 1987; 162: 253-256.
- West NX, Lussi A, Seong J, Hellwig E. Dentin hypersensitivity: Pain mechanisms and aetiology of exposed cervical dentin. Clin Oral Investig. 2013; 17: 9-19.
- Olley RC, Moazzez R, Bartlett D. The relationship between incisal/occlusal wear, dentine hypersensitivity and time after the last acid exposure in vivo. J Dent. 2015; 43: 248-252.
- Närhi M, Kontturi-Närhi V, Hirvonen T, Ngassapa D. Neurophysiological mechanisms of dentin hypersensitivity. Proc Finn Dent Soc. 1991; 88: 15-22.
- Brännström M, Johnson G. Movements of the dentine and pulp liquids on application of thermal stimuli. An in vitro study. Acta Odontol Scand. 1970; 28: 59-70.
- Garberoglio R, Brännström M. Scanning electron microscopic investigation of human dentinal tubules. Arch Oral Biol. 1976; 21: 355-362.
- Pasqualini D, Scotti N, Ambrogio P, Alovisi M, Berutti E. Atypical facial pain related to apical fenestration and overfilling. Int Endod J. 2012; 45: 670-677.
- Boucher Y, Sobel M, Sauveur G. Persistent pain related to root canal filling and apical fenestration: a case report. J Endod. 2000; 26: 242-244.
- Furusawa M, Hayakawa H, Ida A, Ichinohe T. A Case of Apical Fenestration Misdiagnosed as Persistent Apical Periodontitis. Bull Tokyo Dent Coll. 2012; 53: 23-26.
- Draenert ME, Jakob M, Kunzelmann K-H, Hickel R. The prevalence of tooth hypersensitivity following periodontal therapy with special reference to root scaling. A systematic review of the literature. Am J Dent. 2013; 26: 21-27.
- Gillam DG, Orchardson R. Advances in the treatment of root dentine sensitivity: mechanisms and treatment principles. Endod Top. 2006; 13: 13- 33.
- Villa-Chávez CE, Patio-Marín N, Loyola-Rodríguez JP, Zavala-Alonso NV, Martínez-Castaón GA, Medina-Solís CE. Predictive values of thermal and electrical dental pulp tests: A clinical study. J Endod. 2013; 39: 965-969.
- Chen E, Abbott P V. Evaluation of accuracy, reliability, and repeatability of five dental pulp tests. J Endod. 2011; 37: 1619-1623.
- Pan HY, Yang H, Zhang R, Yang YM, Wang H, Hu T, et al. Use of cone-beam computed tomography to evaluate the prevalence of root fenestration in a Chinese subpopulation. Int Endod J. 2014; 47: 10-19.
- Nimigean VR, Nimigean V. Combined mucosal and alveolar fenestration: A clinical report and literature review. Rom J Morphol Embryol. 2013; 54: 437- 441.
- Triches TC, Paula LK, Bolan M, others. Apical fenestration and ectopic eruption--effects from trauma to primary tooth: a clinical case report. Dent Traumatol. 2011; 27: 74-76.
- Edney MB. Interesting presentation of a retained upper deciduous incisor with apical fenestration. Br Dent J. 2000; 188: 369-370.
- Braun X, Ritter L, Jervøe-Storm PM, Frentzen M. Diagnostic accuracy of CBCT for periodontal lesions. Clin Oral Investig. 2014; 18: 1229-1236.