
Case Report
Austin J Dent. 2016; 3(4): 1044.
Parotid Gland Tuberculosis: A Clinical Rarity
Rahman T*, Ahmed SS, Hashmi GS and Zainab S
Department of Oral and Maxillofacial Surgery, Aligarh Muslim University, India
*Corresponding author: Tabishur Rahman, Department of Oral and Maxillofacial Surgery, Dr. Ziauddin Ahmed Dental College and Hospital, Aligarh Muslim University, Aligarh, Uttar Pradesh, India
Received: July 16, 2016; Accepted: September 10, 2016; Published: September 12, 2016
Abstract
We describe a case of Parotid gland tuberculosis which is a rarely encountered clinical entity. The condition is often misdiagnosed as a neoplasm or other inflammatory diseases of salivary gland and leads to unnecessary surgery. The paper highlights the importance of considering this condition in the differential diagnosis especially in the countries where tuberculosis is endemic.
Keywords: Parotid; Tuberculosis; Infection; Swelling
Introduction
Tuberculosis of the parotid gland is a rare clinical entity which causes some difficulties in diagnosis because of the similarities in presentation to that of a neoplasm. Extrathoracic tuberculosis is seen in approximately 20% of overall active tuberculosis [1]. However, parotid gland involvement is a clinical rarity, even in countries in which tuberculosis is endemic [2].
Case Presentation
A 15-year-old female presented with an enlarging asymptomatic mass in the left parotid region of one year duration with accompanied history of fever. The medical history was non-revealing for any systemic disease. Physical examination revealed a mobile, non-tender mass of 5X5 cm occupying the superficial lobe of the left parotid gland extending from mandibular angle to ear lobe with no overlying skin changes. There was no sinus or discharge from swelling (Figure 1). Cervical lymphadenopathy was noticed on involved side. Facial nerve function was normal. The complete blood count, erythrocyte sedimentation rate, other biochemical investigations and chest X-ray were normal. Monteux test was positive and sputum smear examination was negative for acid fast bacilli (AFB). Ultrasonography (USG) of the parotid region showed enlarged left parotid gland with hypo echoic rounded solid mass like lesions within the architecture of the gland without any calcification and cystic degeneration (Figure 2). USG guided fine needle aspiration cytology of the swelling showed granulomatous epithelioid cell clusters, macrophages and caseation necrosis, suggestive of tubercular parotid lymphadenitis (Figure 3). AFB smear prepared from fine needle aspiration cytology (FNAC) sample positively confirmed our diagnosis of tubercular parotitis. The patient was treated with four drugs (Isoniazid, Rifampicin, Ethambutol and Pyrazinamide) anti-TB regimen for 2 months, followed by two drugs (Isoniazid, Rifampicin) for 4 months and showed a complete resolution of swelling.
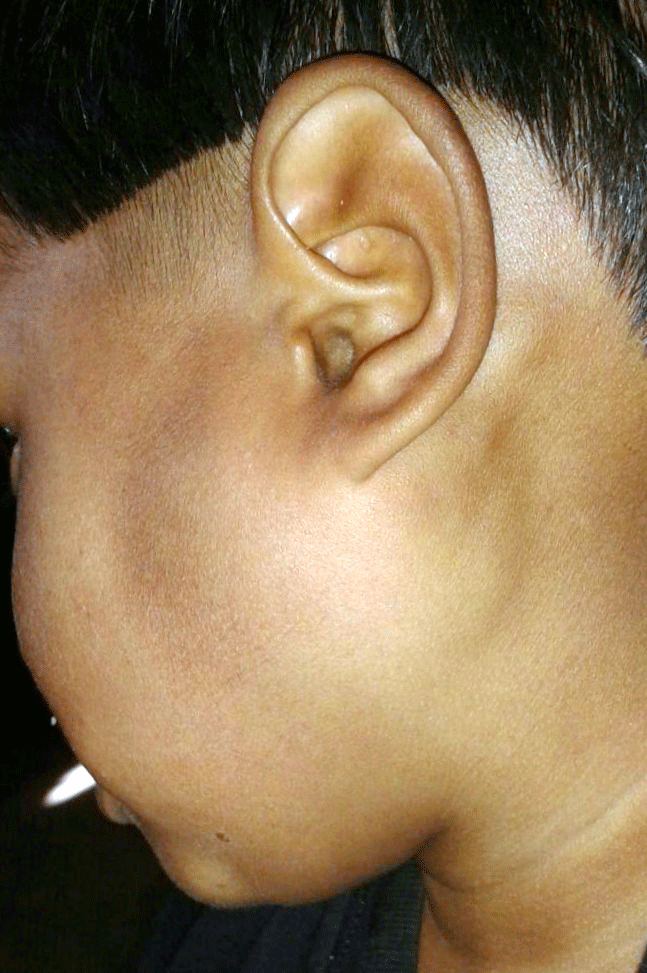
Figure 1: Swelling in the left parotid region.
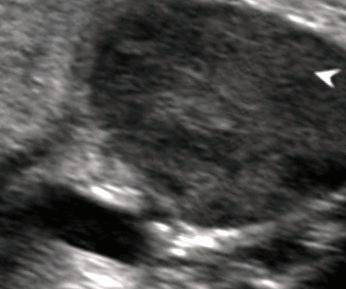
Figure 2: USG of the parotid region showing enlarged parotid gland with
hypo echoic rounded solid lesions within the architecture of the right parotid
gland with absence of calcification and cystic degeneration.
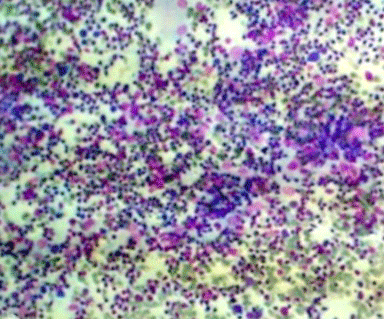
Figure 3: FNAC showing epithelioid cell granuloma with macrophages
(Magnification 10 X).
Discussion
Apart from being endemic in many developing countries the incidence of tuberculosis is increasing in developed countries in recent years due to factors such as the development of resistant strains and co-infection with HIV [3]. Although it commonly involves the lungs, extra pulmonary forms account for approximately 20% of overall active tuberculosis, but the salivary glands are rarely infected [4]. Parotid gland involvement may occur either primarily when the mycobacterium ascends into the salivary gland via its duct from a focus of mycobacterial infection in the oral cavity or secondarily through hematogeneous or lymphatic spread from a primary lung focus [5,6]. The latter mode is more common but in our case chest X-ray was normal excluding the pulmonary tuberculosis as the primary source. When AFB is negative from Stenson’s duct Figure 1: Swelling in the left parotid region. secretion or saliva it is very difficult to differentiate clinically from a neoplasm or other inflammatory diseases of salivary gland like mumps, sarcoidosis, actinomycosis etc. USG of the parotid swelling plays a major role in the diagnosis of parotid tuberculosis. Ultrasound differentiates benign from malignant neoplasms and demonstrates whether a lesion is intraglandular orperiglandular in location [7]. Sonographically parotid tuberculosis can be of two types: parenchymal and periparotid type. The parenchymal type appears as a diffusely enlarged, comparatively hypoechoic gland, with or without focal intraparotid nearly anechoic zones as seen in the present case. The latter appears as hypoechoic nodules located in the peripheral zone of the hyperechoic parotid gland, consistent with enlarged periglandular lymph nodes [8]. The correlation in findings of USG-guided FNAC with postoperative histological findings shows an overall accuracy of 86-89% [9]. The mainstay of treatment is antitubercular chemotherapy for at least six months.
Conclusion
Although rare, tuberculosis should be considered in the differential diagnosis of any patient presenting with a swelling in the parotid gland to avoid unnecessary surgery.
References
- Lee IK, Liu JW. Tuberculous parotitis: case report and literature review. Ann Otol Rhinol Laryngol. 2005; 114: 547-551.
- Aygenc E, Albayrak L, Ensari S. Tuberculous parotitis. Inf Dis Clin Prac. 2002; 11: 555-557.
- Erkan AN, Cakmak O, Kayaselcuk F, Koksal F, Ozluoglu L. Bilateral parotid gland tuberculosis. Eur Arch Otorhinolaryngol. 2006; 263: 487-489.
- Holmes S, Gleeson MJ, Cawson RA. Mycobacterial disease of the parotid gland. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000; 90: 292-298.
- Hamdan AL, Hadi U, Shabb N. Tuberculous parotitis: a forgotten entity. Otolaryngol Head Neck Surg. 2002; 126: 581-582.
- Rajendra Takhar, Motilal Bunkar, Vinod Jangid, Anil Saxena. Bilateral parotid gland tuberculosis: A rare Occurrence. EJCDT. 2015; 64: 653-656.
- Howlett DC. High resolution ultrasound assessment of the parotid gland. Br J Radiol. 2003; 76: 271-277.
- Kushwaha RAS, Kant S, Verma SK, Sanjay, Mehra S. Isolated metacarpal bone tuberculosis: A case report. Lung India. 2008; 25: 17-19.
- Chou YH, Tiu CM, Liu CY, Hong TM, Lin CZ, Chiou HJ, et al. Tuberculosis of the parotid gland: Sonographic manifestations and sonographically guided aspiration. J. Ultrasound Med. 2004; 23: 1275-1281.