
Case Report
Austin J Dent. 2017; 4(3): 1075.
Aggressive Periodontitis - A Comprehensive Treatment Approach
Bapure S¹*, Triveni MG², Mehta DS², Vinod V³ and Khyati C²
¹Department of Periodontology & Implantology, College of Dental Science, India
²Department of Periodontics, Bapuji Dental College & Hospital, India
³Department of Prosthodontics and Implantology, College of Dental Science, India
*Corresponding author: Sunil Bapure, Department of Periodontology & Implantology, College of Dental Science, Amargadh-364210, Gujarat State, India
Received: March 09, 2017; Accepted: April 19, 2017; Published: May 10, 2017
Abstract
Destructive periodontal disease affecting the connective tissue attachment & alveolar bone supporting the teeth have long been considered the principal cause for tooth loss. Aggressive periodontitis is a multifactorial disease consisting of a heterogenous group of infectious disease characterized by the complex host microbial interaction in the periodontium. Genetic, immunologic and environmental/behavioral risk factors are also involved. Aggressive periodontitis (AgP), as the name implies, is a type of periodontitis, where there is rapid destruction of periodontal ligament and alveolar bone which occurs in otherwise systemically healthy individuals generally of a younger age group, but patients may be older. Pathogenic bacteria in the dental plaque, especially Aggregatibacter Actinomycetemcomitans (AA) and Porphyromonas Gingival is having an indispensable role in the etiopathogenetic of an aggravated host response. A long-term stability of periodontal health can be achieved following comprehensive non-surgical, surgical periodontal therapy and systemic antimicrobial therapy.
The present report describes a case of Aggressive periodontitis treated successfully through a comprehensive dental approach.
Keywords: Aggressive periodontitis; Aggregatibacter actinomycetemcomitans; Comprehensive; Multifactorial
Abbreviations
AgP: Aggressive Periodontitis; GagP: Generalized Aggressive Periodontitis; AA: Aggregatibacter Actinomycetemcomitans
Introduction
Aggressive Periodontitis (AgP) is usually presented in early phase of life implies that etiologic agents have been capable of causing clinically detectable levels of disease over a relatively short time. The existence of specific forms of AgP has also been recognized based on specific clinical and laboratory features. Generalized Aggressive Periodontitis (GAgP) being one among its form is characterized by “generalized interproximal attachment loss affecting at least three permanent teeth other than the first molars and incisors” rapid attachment loss, bone destruction and familial aggregation [1].
According to Lang, et al. 1999; Tonetti & Mombelli 1999; the distinguishing features of GAgP include predilection for people under 30 years of age, but patients may be older, generalized inter proximal attachment loss affecting at least 3 permanent teeth other than the first molars and incisors, attachment loss occurring in pronounced episodic periods of destruction. The disease is frequently associated with the presence of periodontal pathogens, neutrophil function abnormalities, genetic factors including a poor serum antibody response to infecting agents and environmental/behavioral risk factors [2,3].
According to Shah, 1993 GAgP has been frequently associated with the detection of Porphyromonas gingivalis, Bacteroides forsythus and Aggregatibacter Actinomycetemcomitans, contrast to Aggregatibacter Actinomycetemcomitans, which is facultatively anaerobic, P. gingivalis and B. forsythus are fastidious strict anaerobes. P. gingivalis is known to produce potent enzymes and a relationship between the clinical outcome of therapy and bacterial counts has also been documented for P. gingivalis with non-responding lesions often containing this organism in elevated proportions.
Case Presentation
A 27-year-old Caucasian female patient reported to the Department of Periodontology, Bapuji Dental College & Hospital, Davangere with the chief complaint of bleeding gums since four to five months. On eliciting the familial history, it was revealed that the patient’s elder sister had similar complaint and was treated for the same. On intra-oral examination, an edentulous upper anterior region revealed clinically missing teeth that included 14, 13, 12, 11, 21, 22, 23, 24 (Figure 1) which were extracted previously due to increased mobility as told by the patient and periodontal condition illustrating severe generalized horizontal bone loss as revealed in the previous OPG (Figure 2). The preliminary examination of dentulous sites revealed, generalized enlarged reddish pink gingiva with thickened and rolled margins. The consistency of the gingiva was firm and nodular. Generalized deep probing pocket depths (PD) of 5-6 mm in the maxillary and 8-9 m min the mandibular arches, with 60% sulcus bleeding index (SBI) was recorded. Suppuration was noted. The patient was systemically healthy and was not under any medications. The blood investigations were in the normal range and based on the clinical and laboratory findings ruling out Trauma from Occlusion, a provisional diagnosis of generalized aggressive periodontitis was made (Chart 1).
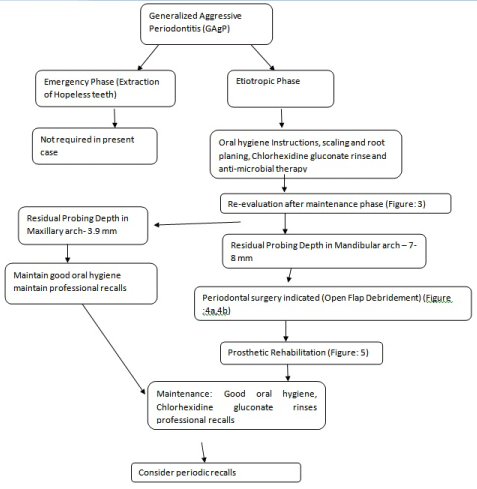
chart 1: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
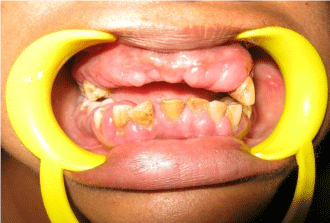
Figure 1: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
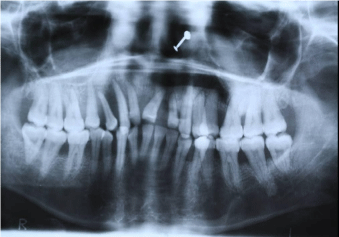
Figure 2: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
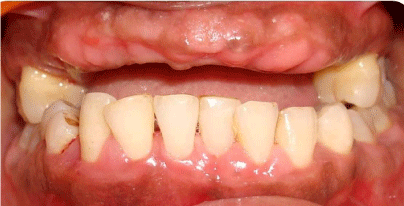
Figure 3: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
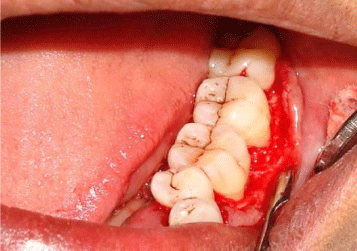
Figure 4a: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
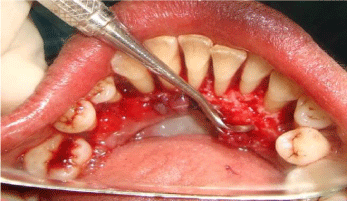
Figure 4b: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
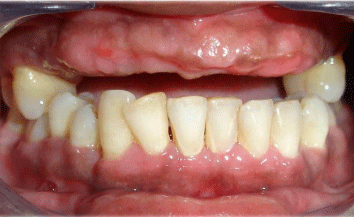
Figure 5: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
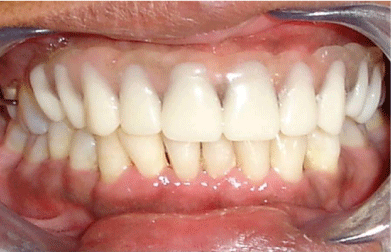
Figure 6: Overall survival, autologous stem cell transplant (ASCT) versus no ASCT (p=0.12).
Treatment protocol
Owing to the considerable amount of bone loss relative to the young age of the patient, the overall treatment concepts and goals in patients with aggressive periodontitis warrants a well-thoughtthrough treatment plan and an often more aggressive treatment approach, in order to halt further periodontal destruction and regain as much periodontal attachment as possible. The ultimate goal of treatment is to create a clinical condition that is conducive to retaining maximum teeth possible for as long as possible and following a radical extraction protocol by not retaining the teeth with hopeless prognosis that can affect the outcome of the treatment. The treatment protocol followed as follows:
Discussion
Aggressive periodontitis (AgP) which is a complex disease comprises a group of rare, often severe, rapidly progressive forms of periodontitis often characterized by an early age of clinical manifestation and a distinctive tendency for cases to aggregate in families. The variability in the age of onset of aggressive periodontitis may be associated with the type and severity of etiologic factors. Aggressive Periodontitis has a Multifactorial etiology. Insofar the young age of onset is an indication of a significant contribution of host factors and perhaps of other nonplaque-related etiology as Baer has contemplated that the amount of periodontal destruction usually is not commensurate with the amount of local factors observed, similar observation was seen in the present case. An important feature of aggressive periodontitis is that the subjects are healthy and not inflicted with a debilitating systemic disease that affects their general health and predisposes to periodontal destruction and the sex predilection of occurrence of AgP in females (3:1), and its tendency to clusters within family.
Likewise, in this case as well, the patient who was a systemically healthy female with occurrence of similar condition in her sister as reported lead towards the diagnosis of AgP and based on the extent of destruction it was concluded to GAgP.
Given the rapid progression of the disease and the high degree of difficulty in gaining control of the disease, early diagnosis and treatment of aggressive periodontitis should be preferred and however, the general practitioner does play an essential role in the early detection of patients who potentially have aggressive periodontitis like in our case the practioner who referred the patient played an important role by already extracting the teeth with hopeless prognosis thus helping us in improving the prognosis of treatment outcome.
Successful treatment of GAgP is considered to be dependent not only on early diagnosis but also on therapy which is directed towards elimination/suppression of the infecting microorganism and also to provide an environment conducive to long-term maintenance. The stable treatment results can be obtained by ensuring patient education and patient compliance with the aim of altering modifiable risk factors.
Long-term elimination of aggressive periodontitis has not been possible with conventional debridement alone. Antibiotic used as an adjunct to debridement has been known to aid in the treatment outcome. One should first mechanically reduce the subgingival bacterial load, which might otherwise inhibit or degrade the antimicrobial agent. Disrupting the structured bacterial aggregates that can protect the bacteria from the agent the patient was prescribed medication which comprised of Amoxicillin (500 mg) TID and Metronidazole (400 mg) as the synergistic effect of metronidazole and amoxicillin on A. actinomycetemcomitans has been documented [4] with their efficacy and effectiveness proven in the treatment of GAgP as the tetracycline failure was seen in A.A suppression [5].
The effect of root planning alone on generalized aggressive periodontitis is much better documented [6], and likewise a statistically significant reduction in clinical probing depth was seen in the maxillary arch which was reduced to 3.9 mm after phase one therapy and residual probing depth of 7-8 mm was seen in the mandibular arch. Phase I therapy showed drastic reduction in SBI to as low as 10%. Leaving residual pockets of 6 mm is a risk factor for the progression of periodontal disease after active treatment [7]. Residual deep pockets are niches in the mouth where considerable numbers of pathogenic bacteria can remain, even after initial phase of treatment [8]. Thus, Pocket Reduction procedure (Open Flap Debridement) was considered for the residual pockets in the mandibular arch as it results in greater PPD reduction and clinical attachment gain [9].
After the successful reduction in pocket depth after the required therapy, another level on which age impacts treatment in aggressive periodontitis is the prosthetic rehabilitation [8] and the patient was given all the treatment options suitable which included a removable, fixed prosthesis. Owing to the less survival rate of implant supported prosthesis in aggressive periodontitis patients, the patient was advised a fixed prosthesis and was given the same. Since the patient was young and had already undergone multiple extractions, the patient was bound to have an effect on her general and psychological well-being, self-esteem and daily social life. However, successful comprehensive treatment comprising of the periodontal and prosthetic rehabilitation aided in improving the Oral Health Related Quality Of Life of the patient doing which Engendering feelings of ease and confidence in his or her abilities, a skilled periodontist is capable of allaying patient’s fears and render the dental encounter to be a pleasant and painless one.
Conclusion
There exists an essential variance between a diagnosis and a classification, whereby a diagnosis is known to be the clinician’s best conjecture, leading on to a treatment plan, whereas a classification does not allow such flexibility [10]. Thus, elucidating the clinical, laboratory, radiographic and the underlying aetiologies associated the diagnosis was given which is classified as GAgP.
A successful outcome in the treatment of GAgP can be achieved with a prompt diagnosis and customized periodontal treatment for individual patients. Although, various advanced diagnostic and treatment modalities have emerged in the management of aggressive periodontitis, it is extremely important that a patient with GAgP be carefully monitored to provide early treatment when necessary due to an increased susceptibility to periodontal diseases in later stages of life. Our approach in management of this case was successful, as the treatment addressed key factors such as early diagnosis, elimination of periodontal pathogens by non-surgical and surgical periodontal therapy and the approach aimed at stability of the affected site through comprehensive rehabilitation.
Thus, by following a comprehensive treatment protocol with adequately desired patient compliance, we were able to improve and retain the present status of the periodontium as well as prosthetically rehabilitate and improve the oral health related quality of life of the patient.
References
- Lang NP, Bartold PM, Cullinan M, Jeffcoat M, Mombelli A, Murakami S, et al. Consensus Report: Aggressive periodontitis. Ann Periodontol. 1999; 4: 53.
- [No authors listed]. Parameter on aggressive periodontitis. American Academy of Periodontology. J Periodontol. 2000; 71: 867-869.
- Tonetti MS, Mombelli A. Early-onset periodontitis. Ann Periodontol. 1999; 4: 39-53.
- Van Winkelhoff AJ, Tijhof CJ, de Graff J. Microbiological and clinical results of metronidazole plus amoxicillin therapy in Actinobacillus actinomycetemcomitans-associated periodontitis. J Periodontol. 1992; 63: 52-57.
- Pavicic MJ, van Winkelhoff AJ, de Graff J. Synergistic effects between amoxicillin, metronidazole, and the hydroxymetabolite of metronidazole against Actinobacillus actinomycetemcomitans. Antimicrob Agents Chemother. 1991; 35: 961-966.
- Hughes FJ, Syed M, Koshy B, Marinho V, Bostanci N, McKay IJ, et al. Prognostic factors in the treatment of generalized aggressive periodontitis: I. Clinical features and initial outcome. J Clin Periodontol. 2006; 33: 663-670.
- Matuliene G, Pjetursson BE, Salvi GE, Schmidlin K, Bragger U, Zwahlen M, et al. Influence of residual pockets on progression of periodontitis and tooth loss: results after 11 years of maintenance. J Clin Periodontol. 2008; 35: 685- 695.
- Teughels W, Dhondt R, Dekeyser C, Quirynen M. Treatment of aggressive periodontitis. Periodontol 2000. 2014; 65: 107-133.
- Heitz-Mayfield LJ, Trombelli L, Heitz F, Needleman I, Moles D. A systematic review of the effect of surgical debridement vs non-surgical debridement for the treatment of chronic periodontitis. J Clin Periodontol. 2002; 29: 92-102.
- Armitage GC, Cullinan MP. Comparison of the clinical features of chronic and aggressive periodontitis. Periodontol 2000. 2010; 53: 12-27.