
Special Article - Periodontal Diseases
Austin J Dent.2017; 4(6): 1088.
Ossifying Fibroma of Maxilla
Saravanan Rethinam¹, Deepshika Saravanan¹, Kavitha Muthu¹* and Preethi Sambandam²
¹Department of Oral Surgery, RVS Dental College and Hospital, India
²Department of Periodontics, RVS Dental College and Hospital, India
*Corresponding author: Kavitha Muthu, Department of Oral Pathology, RVS Dental College and Hospital, Coimbatore 641402, Tamil Nadu, India
Received: June 23, 2017; Accepted: July 11, 2017; Published: August 30, 2017
Abstract
Peripheral Ossifying Fibroma is a solitary growth over the gingiva that arises from the periodontal ligament. The common site of occurrence is the interdental papilla of the maxillary anterior teeth. This paper documents a case of peripheral ossifying fibroma in the right maxillary posterior region and alveolar ridge in forty-year old female patient. This contradicts the common predilection of lesion with regard to site, as the common occurrence is the anterior maxillary region.
Keywords: Peripheral ossifying fibroma, Epulis, Fibro-osseous lesion, Fibroma
Introduction
Peripheral Ossifying Fibroma (POF) is a non-neoplastic growth which is relatively common. It occurs only on the soft tissue over the alveolar bone and is a reactive lesion [1]. This reactive lesion occurs in response to low–grade irritations such as trauma, plaque, calculus, micro-organisms, masticatory forces, ill-fitting dentures and poor quality restorations. The lesion occurs in any age group predominantly in the second decade of life [2]. Females are commonly affected and anterior maxilla is the most prevalent location of involvement [3]. Almost 60% of the lesions occurred in the maxilla, and in both jaws more than 50% occurred in the incisor-cuspid region [4].
A recent study revealed that the prevalence of peripheral ossifying fibroma is 4% among all reactive gingival lesions with female predilection of third decade. With regard to the anatomic location posterior maxilla contributes only for 7% distribution of all reactive gingival lesions [5].
It occurs exclusively on gingiva, appears as a nodular mass, pedunculated or sessile that usually emanates from interdental papilla. The colour ranges from red to pink with the lesion frequently but not always ulcerated. The teeth are usually unaffected and rarely migration or loosening of adjacent teeth has been noticed. In vast majority of cases, there is no apparent underlying bone involvement, on rare occasions superficial erosion of bone has been noticed. It accounts for 3% of all oral tumors and for 9.6% of all gingival lesions [6].
In the early stages the lesion totally radiolucent. Intermediate stages of lesion exhibit mixed radiolucent and radio opaque densities depending on the amount of the calcified material. Histopathologically, a large number of fibroblast and cementoblast with flat elongated nuclei are present within a network of interlacing collagen fibres. At the later stages the cementoblasts coalesce to present as common islands of bone & calcification.
The definitive diagnosis is based on histological examination with the identification of cellular connective tissue and the focal presence of bone or calcifications [3,7].
Prognosis is good, but some instances of recurrence have been reported regularly in various studies. After elimination of the local etiological factors surgical excision is the treatment of choice. The surgical treatment includes aggressive curettage, localized surgical resection and segmental resection.
The mass should be excised down to the periosteum because recurrence is more likely, if the base of the lesion is allowed to remain. The teeth associated with Peripheral Ossifying fibroma are generally not mobile. Though there have been reports of dental migration secondary to bone loss. Extraction of the neighboring teeth is usually not considered necessary [8].
Case Presentation
A forty year old female patient named Mrs. Chithra presented to Department of Periodontology with the complaint of swelling in the upper right premolar-molar region present for the past three months. The swelling was insidious in onset, was initially small in size and gradually grew to the present size. The swelling was associated with bleeding on brushing and was asymptomatic.
On intraoral examination a pinkish red pedunculated growth extending mesiodistally from fifteen to seventeen was noticed, it was measuring about 2.8x2.5x2.7 cm in the upper right alveolar region (Figure 1). On palpation the growth was fibrous and non tender in consistency and had a papillated surface. The oral hygiene was fair with considerable amount of supra and subgingival calculus, there was a grade- III mobility in 15, 16.
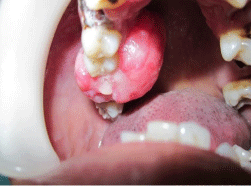
Figure 1: Pre operative view of the lesion.
Radiographic examination revealed horizontal bone loss in 15, 16, 17 regions and mild migration of the teeth. The impression of CT revealed a soft tissue density lesion with areas of calcification arising from the superior alveolus of maxilla on the right side between premolar and molar tooth; medially the lesion caused extrinsic compression over the tongue (Figure 2). Superiorly the lesion was abutting the hard palate on the medial aspect and the posterolateral wall of the maxilla on the lateral aspect, there was thinning of bone noted on the floor of the right maxillary sinus and laterally the lesion was abutting the buccinator muscle.
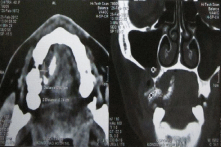
Figure 2: CT image of the lesion.
A provisional diagnosis of epulis was given; Irritation fibroma, pyogenic granuloma and peripheral ossifying fibroma were considered in the differential diagnosis. Patient was advised blood investigation; complete blood count, bleeding time, clotting time, fasting blood glucose and post prandial blood glucose. The hemogram was within normal limits, the treatment plan was phase-I therapy followed by excisional biopsy of the lesion.
The scaling and root planning was performed and patient was scheduled for surgery. The lesion was surgically excised under local anesthesia and the specimen was sent for histopathologic examination (Figure 3,4 and 5). Excised lesion) Mobile teeth were also extracted and sutures were given Figure 6 patient was recalled after a week and the surgical site revealed uneventful healing, the patient was put on a regular maintenance protocol.
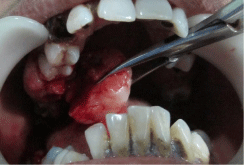
Figure 3: During excision of the lesion.

Figure 4: Excised lesion.
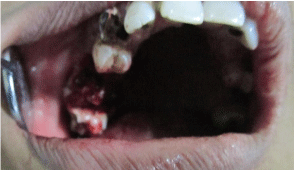
Figure 5: Immediatepost operative view of the excised site.
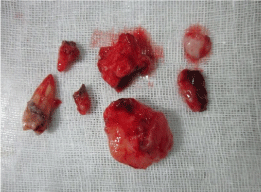
Figure 6: Excised lesion with extracted teeth.
The histopathological examination revealed stratified squamous acanthotic epithelium with elongated retepegs with highly cellular connective tissue with collagen fibres and fibroblast. Stroma revealed myxoidchange with foci of bony trabeculae and osteoid. The high degree of cellularity was in contrast to the findings of irritational fibroma and decreased vascularity was not correlating with pyogenic granuloma. The presence of cellular connective tissue with fibroblast and foci of calcifications confirmed the histologic diagnosis of POF (Figure 7).
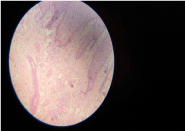
Figure 7: Microscopic appearance of acanthotic epithelium, fibrocellular
connective tissue with areas of calcification.
Discussion
Ossifying fibroma of the jaws is a benign fibro-osseous lesion; its origin is from the periodontal ligament [6]. Peripheral Ossifying Fibroma is a common lesion of the gingiva with various synonyms like epulis, Calcifying Fibroblastic Granuloma, Peripheral Cementifying Fibroma, and Peripheral Fibroma with cementogenesis, Peripheral Cement-ossifying fibroma, Ossifying fibroepithelial polyp and Peripheral fibroma with osteogenesis.
The term POF was coined by Eversole and Rovin [2], it occurs exclusively on the gingiva. It is a relatively common growth of the gingiva and it is considered to be reactive in nature rather than neoplastic [9]. An early POF that presented as ulcerated nodules with little calcification also existed which allowed easy misdiagnosis as pyogenic granuloma [4]. However, Gardner proposed that the highly cellular connective tissue is characteristic of POF that histologic diagnosis can be made based only on that irrespective of the presence of calcification [10].
Commonly POF occurs in the second decade of life [2]. In contrast, it was found in a forty year old female patient in the present case. The common site of occurrence of POF is the anterior maxilla [3], but in this case it was found in the posterior maxillary teeth region which is less prevalent location.POF is a reactive lesion which occurs in response to low grade irritations such as trauma, plaque, calculus and poor quality restorations [11]. This patient had a poor oral hygiene, hence plaque and calculus have been implicated in the etiology of the lesion.
The pathogenesis of POF remains controversial. Chronic irritation of the periosteal and periodontal membrane causes metaplasia of the connective tissue, which initiates the formation of bone or dystrophic calcification [12]. Prasad, et al. [13] observed that POF in some case may initially develop as a pyogenic granuloma that undergoes subsequent fibrous maturation and calcification. In the present case local factors along with hormonal influence due to the patient’s age and sex could be implicated in the etiopathogenesis of the present lesion [14].
The radiographic appearance varies from cystic lesion, mixed density lesion and massive expansile lesions [15]. It is always advisable to go for further investigations like CT with MRI to know the extent of lesion and for treatment planning.
Histologically POF consists of fibrocellular proliferation which consists of large number of fibroblast within this woven bone calcifications are seen. The histologic picture is not unique for POF, it has been considered that the differing pictures are a range of a single lesion in diverse stages of maturation [15]. Immunohistochemistry studies indicate the proliferating cells having myofibroblastic nature along with C68 positive histiocytic components intermingling lymphocytes and plasma cells showing reactive or inflammatory phenomenon [7]. In the present case, histopathological examination revealed acanthoticstratified squamous epithelium with elongated reteridges and underlying connective tissue was composed of densely packed collagen fibres, fibroblasts with mild chronic inflammatory cell infiltration. Areas of ossification in the connective tissue were also evident and the histologic findings correlated with that of POF.
Rarely, abnormally large sized peripheral ossifying fibroma and the lesion associated paraneoplastic syndrome such as osteomlacia can give rise to local and systemic complications [16,17].
Treatment consists of local surgical excision down to the underlying bone for extensive clearing of the base of the lesion. Removal of local factors or irritants is also required. The recurrence rate is about 16-30% [4,16] and the recurrences are believed to be related to lack of inclusion of periosteum or periodontal ligament in the excised specimen. If the defect is large, in recurrent cases and for esthectic reasons, filling the area with reconstructive materials can be considered [18]. The treatment rendered in this case was excision and curettage followed by a regular maintenance protocol. Though these lesions are reactive, some of the ossifying fibromas have been reported with multicentric nature [11,19]. It is sensible to have a regular follow up for these cases since the recurrence rate is relatively high. Regarding this case, the healing was satisfactory and no recurrence has been observed till date.
References
- Moon WJ, Choy SY, Chung EC, Kwon KH, Chae SW. Peripheral ossifying fibroma in the oral cavity CT and MRI findings. Dentomaxillofac Radiol. 2007; 36: 180-182.
- Eversole LR, Rovin S. Reactive lesions of the gingiva. J Oral Pathol. 1972; 1: 30-38.
- Bhaskar SN, Jacoway JR. Peripheral fibroma and peripheral fibroma with calcification: report of 376 cases. J Am Dent Assoc. 1966; 73: 1312-1320.
- Buchner A, Hansen LS. The histomorphologic spectrum of peripheral ossifying fibroma. Oral Surg Oral Med Oral Pathol. 1987; 63: 452-461.
- Hunasgi S, Koneru A, Vanishree M, Manvikar V. Assessment of reactive gingival lesions of oral cavity: A histopathological study. J Oral Maxillofac Pathol. 2017; 21: 180.
- Dahiya P, Kamal R, Saini G, Agarwal S. Peripheral ossifying fibroma. J Nat Sci Biol Med. 2012; 3: 94-96.
- Garcia de Marcos JA, Garcia de Marcos MJ, Arroyo Rodriguez S, Chiarri Rodrigo J, Poblet E. Peripheral Ossifying fibroma of gingiva: A clinical and immunohistochemical study of four cases. J Oral Sci. 2010; 52: 95-99.
- Cuisia ZE, Brannon RB. Peripheral ossifying fibroma--a clinical evaluation of 134 pediatric cases. Pediatr Dent. 2001; 23: 245-248.
- Neville BW, Damm DD, Chi AC,Allen CM. Oral and Maxillofacial Pathology 4th edi. Elsevier Health Sciences; 2015.
- Gardner DG. The peripheral odontogenic fibroma: an attempt at clarification. Oral Surg Oral Med Oral Pathol. 1982; 54: 40-48.
- Kumar SK1, Ram S, Jorgensen MG, Shuler CF, Sedghizadeh PP. Multicentric peripheral ossifying fibroma. J Oral Sci. 2006; 48: 239-243.
- Orkin DA, Amaidas VD. Ossifying fibrous epulis. An abbreviated case report. Oral Surg Oral Med Oral Pathol. 1984; 57: 147-148.
- Prasad S1, Reddy SB, Patil SR, Kalburgi NB, Puranik RS. Peripheral ossifying fibroma and pyogenic granuloma. Are they interrelated? N Y State Dent J. 2008; 74: 50-52.
- Kenney JN1, Kaugars GE, Abbey LM. Comparison between the peripheral ossifying fibroma and peripheral odontogenic fibroma. J Oral Maxillofac Surg. 1989; 47: 378-382.
- Liu Y, Wang H, You M, Yang Z, Miao J, Shimizutani K et al. Ossifying fibromas of the jaw bone: 20 cases. Dentomaxillofac Radiol. 2010; 39: 57-63.
- John RR1, Kandasamy S1, Achuthan N1. Unusually large-sized peripheral ossifying fibroma. Ann Maxillofac Surg. 2016; 6: 300-303.
- Sandoval MA, Palermo MA, Carrillo R, Bundoc R, Carnate JM Jr, Galsim RJ. Successful treatment of tumor- induced osteomalacia after resection of an oral peripheral ossifying fibroma. BMJ Case Rep. 2017.
- González-Serrano J, López-Pintor RM, Sanz-Sánchez I, Paredes VM, Casañas E, de Arriba L, et al. Surgical Treatment of a Peripheral Ossifying Fibroma and Reconstruction with a Porcine Collagen Matrix: A Case Report. Int J Perodontics Restorative Dent. 2017; 37: 443-449.
- Choudary SA, Naik AR1, Naik MS, Anvitha D. Multicentric variant of peripheral ossifying fibroma. Indian J Dent Res. 2014; 25: 220-224.