
Case Report
Austin J Dent. 2017; 4(7): 1091.
Raising the Self Esteem with the Oral Rehabilitation of a Child with Incontinentia Pigmenti Syndrome
França DCC, Pereira TDS, Hall KB, Nagata ME, Pessan JP and Ávila de Aguiar SMHC*
Department of Pediatric Dentistry and Public Health, Aracatuba Dental School, UNESP Univ Estadual Paulista, Brazil
*Corresponding author: Ávila de Aguiar SMHC, Department of Pediatric Dentistry and Public Health, Aracatuba Dental School, UNESP Univ Estadual Paulista, Araçatuba, São Paulo, Brazil
Received: August 24, 2017; Accepted: October 06, 2017; Published: October 30, 2017
Abstract
Incontinentia pigmenti (IP) is a rare X-linked dominant syndrome that mainly affects the skin, eyes, hair, central nervous system and teeth. Although dermatologic manifestations are among the most important aspects for the diagnosis of the syndrome, oral involvement characterized by hypodontia, conoid teeth and delayed eruption are also important for the diagnosis and patient aesthetic rehabilitation. These abnormalities may cause feeding problems influencing the patient quality of life. This study reported a case of a 10-year-old girl with cutaneous manifestations and hypodontia. The child´s main complaint was related to her smile. The treatment plan was the tooth restoration (conoid) and installation of the space maintainers. This case enhances the importance of integrated dental treatment, which combines pediatric dentistry, orthodontics and conventional prosthesis. In addition, hypodontia is frequently found in incontinentia pigmenti, and dentists should be aware of this condition in order to help with the diagnosis.
Keywords: Incontinentia pigmenti, child, Pigmentation disorders, Oligodontia
Introduction
Incontinentia pigmenti (IP) syndrome is a rare X-linked dominant genodermatosis which mainly affects women and is usually lethal for males when in the mother’s utero [1]. Synonyms of IP type 2 are: Bloch-Sulzberger syndrome, Bloch-Siemens syndrome, familial incontinentia pigmenti (pigment incontinence). The incidence of the disorder is 1 case per 40,000 populations. The name of the disease reflects morphological changes of the skin seen under a microscope system [2]. The disease is systemic and involves tissues of ectodermic and mesodermic origin including coetaneous tissue, teeth, eyes and the central nervous system (CNS), amongst other organs. In 80% of the cases other defects are seen in the form of dental, skeletal, nail anomalies, microcephaly, seizures, psychomotor retardation, strabismus, opitc nerve atrophy, retinal detachment, cataracts, etc, [3].
Cutaneous manifestations of IP are divided into the following four stages, although not all stages may be present in some cases: stage 1-erythema, vesicles and blisters appearing in a typically linear pattern; stage 2-papulae, verrucous lesions and hyperkeratosis; stage 3-hyperpigmentation; stage 4-hypopigmentation and cutaneous atrophy. In all of these stages, the cutaneous lesions tend to follow the lines of Blaschko [4].
The blistering stage of the lesion needs to be differentiated from Herpes simplex and Bullous Impetigo. The lesions are linear and in clusters in classical Incontenentia Pigmenti. Warty phase needs to be differentiated from linear epidermal birthmarks or warts. Hyperpigmentary stage needs to be differentiated from moles and other causes of hyperpigmentation. Hyperpigmentation of Incontenentia Pigmenti is classically in whorls [3].
Following dermatologic alterations, dental manifestations are the most frequent, which are observed in 80% of patients and usually affect both the primary and permanent dentitions [4,5]. The most frequent alteration is hypodontia (up to 43% of patients), followed by pegged or conically crowned teeth (30% of patients). Other dental features were also reported as delayed eruption, partial anodontia, hypomineralization and gothic palate [6]. All these manifestations are important because they persist throughout the patient’s life, thus requiring an adequate dental treatment plan when the diagnosis of the disease to oral rehabilitation is made by a multidisciplinary team [4].
The majority of dental anomalies in IP patients could be successfully corrected. Some of these anomalies may greatly influence the quality of life causing psychological and feeding problems [7]. This article reports a case of a 10-year-old girl with cutaneous manifestations and hypodontia. The diagnosis of incontinentia pigmenti in this patient was based on the description of vesiculobullous lesion at birth followed by hyperpigmented lesion overlapping the previous area of the vesicobullous lesion.
Case Presentation
A 10-year-old girl was brought by her mother to the Department of Pediatric Dentistry because the girl was complaining that her teeth were “thin and ugly”.
Her mother was 33 years old at the child’s birth, and although pregnancy was not planned, the prenatal care was made. During pregnancy, there were no reports of illnesses, injuries, needs of radiographs and use of drugs. Before the birth of the patient, four miscarriages were reported.
The child’s birth was in the hospital (caesarian) without the presence of complicating factors such as: child-birth too fast or slow, cyanosis, bleeding, poor sucking or the need to stay in an incubator.
In the neonatal period, three days after birth, there were pigmented vesiculobullous eruptions on the trunk and limbs. At the age of five she had severe allergy and was diagnosed with dust, smoke, heat and animal allergy. At the time, the mother did not make the use of drugs. In respect to family history and past health of the patient, there was no report of any disease or changes beyond those described above.
In physical examination, the presence of scars related to the vesiculobullous rash mainly on lower limbs, sparse eyebrows and prominent lips could be seen. Other findings commonly associated with the syndrome were not observed (Figure 1).
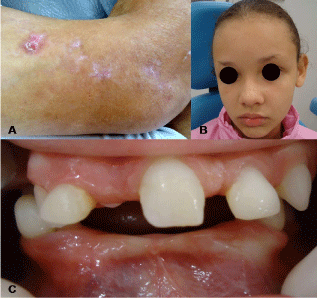
Figure 1: Scars on lower limbs (A), Sparse eyebrows (B), Intraoral Aspects
(C).
On clinical intraoral examination, hypodontia, conoid teeth and delayed tooth eruption were observed (Figure 1). Radiographically, there are no changes or bone lesions and it could be notice the absence of all premolars, permanent maxillary left central and lateral incisors, all permanent mandibular central and lateral incisors, all second permanent molars, all third molars (Figure 2).
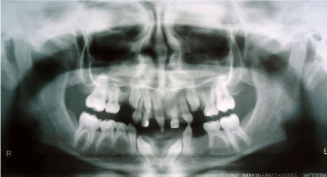
Figure 2: Orthopantomographic radiograph confirming the absence of
deciduous and permanent teeth, and characterizing radicular and coronal
changes.
The treatment plan was carried out on panoramic radiography, restoration of the permanent maxillary right central incisor (conoid), impression of both arches for making space maintainers (Figure 3), installation, maintenance, and periodic replacement of the space maintainers. Regular maintenance of space maintainers was also carried out monitoring tooth eruption, growth and development of the patient. She returned for dental examination every 3 months. In 1 year of follow-up dental care, there have been no extensive caries and fair periodontal health was confirmed. Currently, the oral health and the clinical aspect of the patient is highly satisfactory, as it can be observed in Figure 4.
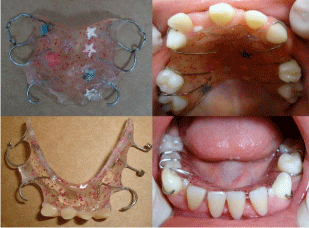
Figure 3: Maxillary space maintainer and mandibular functional space
maintainer.
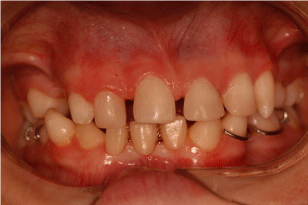
Figure 4: Current clinical aspects of the patient.
Discussion
The syndrome involves organs and tissues whose embryonic origin is ectodermal and mesodermal. Manifestations may be cutaneous or extracutaneous, being more in the former [8]. In the majority of cases, these abnormalities present themselves in the first few weeks of life [9].
Nuclear factor kappa B (NF-KB) regulates the expression of various genes, including cytokines and adhesion of molecules. Activation of NF-KB also confers protection against apoptosis induced by tumor necrosis factor (TNF). The NF-KB essential modulator (NEMO) gene is indispensable in the process of NF-KB activation. Recently, the cause of IP was attributed to a mutation that inactivates the NEMO gene located at chromosome X (q28) [10,11].
The clinical manifestations of IP vary widely even in the same family, ranging from subtle cutaneous and dental changes to severe and incapacitating ophthalmologic and neurologic manifestations. The latter is the most serious clinical manifestations of IP. In this case, the patient showed no ophthalmologic manifestations, although a retinal related symptom is not the most frequent ophthalmologic alteration, ranging in reports from 18% to more than 33% of patients. The prognosis for children who do not develop these manifestations is good, but continuous ophthalmologic follow-up is recommended [12].
The management of the skin and systemic abnormalities in incontinentia pigmenti is based on symptomatology alone. Support and corrective measures may be used whenever possible [13]. Although dermatologic manifestations are among the most important aspects for the diagnosis of the syndrome, they are less damaging to the patient.
Oral involvement is also important and may exhibit any of a triad consisting of hypodontia, conical teeth and delayed eruption [4,5,14]. Since the patient did not present more damaging manifestations, her most severe complication was related to aesthetics and dental anomalies. In a clinical study of 20 patients with IP, hypodontia and conical teeth were the most prevalent dental anomalies [5], as observed in the present case report. For these reasons, after stabilization of growth and development, through a multidisciplinary approach, orthodontic corrections, placement of dental implants and prosthetic rehabilitation will be held.
Radiographic examination revealed the absence of various permanent tooth germs, which in the future will lead to problems in masticatory and occlusal function if not treated adequately, and probably psychosocial problems due to a compromised esthetic appearance. The patient also presented hypodontia of deciduous teeth and conoid teeth, aspects that agree with the clinical findings of the syndrome. The mother reported that child´s main complaint was related to her smile and this was already affecting her self-esteem. The treatment plan was the restoration of the permanent maxillary right central incisor (conoid), and making space maintainers, installation, maintenance, and periodic replacement of space maintainers.
IP patients should be reviewed regularly and gain access to specialist dental care [6,15], for this reason the girl was referred for integrated dental treatment combining pediatric dentistry and orthodontics, with less concern regarding the disease but more emphasis given on the treatment of hypodontia. Hypodontia is a frequent finding in incontinentia pigmenti, and dentists should be aware of this condition in order to help with the diagnosis and in the guidance of patients and their families.
Acknowledgement
All authors have made substantive contribution to this study and/or manuscript, and all have reviewed the final paper prior to its submission.
References
- Nso Roca AP, Baquero-Artigao F, García-Miguel MJ, Guerrero Vázquez J, Guerrero Fernández J, Vicente Cuevas M, et al. Incontinentia pigmenti. Initial and long-term characteristics. An Pediatr (Barc). 2008; 68: 9-12.
- Buinauskiene J, Buinauskaite E, Valiukeviciene S. Incontinentia pigmenti (Bloch-Sulzberger syndrome) in neonates. Medicina (Kaunas). 2005; 41: 496-499.
- Mane S. Incontinentia pigmenti. Indian Pediatr. 2006; 43: 1103-1104.
- Kitakawa D, Fontes PC, Magalhães FA, Almeida JD, Cabral LA. Incontinentia pigmenti presenting as hypodontia in a 3-year-old girl: a case report. J Med Case Rep. 2009; 3: 116.
- Poziomczyk CS, Bonamigo RR, Santa Maria FD, Zen PR, Kiszewski AE. Clinical study of 20 patients with incontinentia pigmenti. Int J Dermatol. 2016; 55: 87-93.
- Minic S, Novotny GE, Trpinac D, Obradovic M. Clinical features of incontinentia pigmenti with emphasis on oral and dental abnormalities. Clin Oral Investig. 2006; 10: 343-347.
- Minić S, Trpinac D, Gabriel H, Gencik M, Obradović M. Dental and oral anomalies in incontinentia pigmenti: a systematic review. Clin Oral Investig. 2013; 17: 1-8.
- Montes CM, Maize JC, Guerry-Force ML. Incontinentia pigmenti with painful subungual tumors: a two-generation study. J Am Acad Dermatol. 2004; 50: 45-52.
- Buinauskaite E, Buinauskiene J, Kucinskiene V, Strazdiene D, Valiukeviciene S. Incontinentia pigmenti in a male infant with Klinefelter syndrome: a case report and review of the literature. Pediatr Dermatol. 2010; 27: 492-495.
- Nogueira A, Lisboa C, Eloy C, Mota A, Azevedo F. Vesicular rash in a newborn. Incontinentia pigmenti. Indian J Dermatol Venereol Leprol. 2009; 75: 330.
- Thakur S, Puri RD, Kohli S, Saxena R, Verma IC. Utility of molecular studies in incontinentia pigmenti patients. Indian J Med Res. 2011; 133: 442-445.
- Kim BJ, Shin HS, Won CH, Lee JH, Kim KH, Kim MN, et al. Incontinentia pigmenti: clinical observation of 40 Korean cases. J Korean Med Sci. 2006; 21: 474-477.
- Pacheco TR, Levy M, Collyer JC, de Parra NP, Parra CA, Garay M, et al. Incontinentia pigmenti in male patients. J Am Acad Dermatol. 2006; 55: 251- 255.
- Russell DL, Finn SB. Incontinentia pigmenti (Bloch-Sulzberger syndrome): a case report with emphasis on dental manifestations. J Dent Child. 1967; 34: 494-500.
- Cho SY, Lee CK, Drummond BK. Surviving male with incontinentia pigmenti: a case report. Int J Paediatr Dent. 2004; 14: 69-72.