
Original Manuscript
Ann Depress Anxiety. 2023; 10(1): 1116.
Prevalence of Anxiety and Depression Symptoms in Patients Diagnosed with Atopic Dermatitis in Mexico: A Cross-Sectional Study
Macias-Weinmann A*; Chávez-Ruiz AK; González-Díaz SN; Canseco-Villareal JI; Noyola-Pérez A
Regional Center of Allergy and Clinical Immunology, Hospital Universitario “Dr. José Eleuterio González”, México
Corresponding author: Macias-Weinmann A Regional Center of Allergy and Clinical Immunology at the Hospital Universitario “Dr. José Eleuterio González”, Madero y Gonzalitos S/N, Mitras Centro, 64460, Monterrey, Nuevo León, Mexico. Tel: +52 (81)8346-2515 Email: amaciasweinmann@gmail.com
Received: February 28, 2023 Accepted: March 31, 2023 Published: April 07, 2023
Abstract
Introduction: Atopic Dermatitis (AD) is one of the most common inflammatory skin diseases affecting individuals of all ages. It is proposed that intense pruritus, sleep cycle disturbances, stigmatization, and social isolation due to the visual nature of the disease, along with the poor quality of life and the presence of neuroinflammation, contribute to the development of anxiety and depression. According to recent systematic reviews and meta-analyses evaluating the relationship between AD, anxiety, and depression, there is a higher likelihood of developing depression during the disease, predominantly in children and both disorders in adults. However, no Mexican studies have determined the prevalence of anxiety and depression symptoms in children, adolescents, and adults diagnosed with AD.
Objective: To determine the prevalence of anxiety and depression symptoms in patients diagnosed with AD.
Material and Methods: This is an observational, cross-sectional, and comparative study. We included forty-eight patients who met the inclusion criteria and applied two self-administered screening questionnaires for anxiety and depression symptoms.
Results: A prevalence rate of depression symptoms of 4.5% and 16.7% were found in children and adolescents, respectively, and 27.3% and 16.6% for anxiety symptoms, respectively. On the other hand, in the group of adults, the presence of clinically significant symptoms of anxiety and depression was present at 40% and 45%, respectively.
Conclusion: It is crucial that allergists evaluate the psycho-emotional sphere in patients with AD with the available screening tools with the aim to identify and refer in a timely manner.
Keywords: Atopic dermatitis; Anxiety; Depression; Allergic disorder; Mental health
Abbreviations: AD: Atopic Dermatitis; DALYs: Disability-Adjusted Life Years (DALYs); SCAS: Spence Children’s Anxiety Scale; CDI: Kovacs Depression Inventory; BDI II: Beck Depression Inventory-Second Edition; BAI: Beck Anxiety Inventory, DSM-IV: Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; DSM-V: Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition; SCORAD: SCORing Atopic Dermatitis
Introduction
Atopic Dermatitis (AD) is a prevalent and complex inflammatory skin disease that affects individuals of all ages, with a reported prevalence of up to 20% of children and 10% of adults in high-income countries [1,2]. The disease is characterized by eczematous lesions, intense pruritus, and a chronic or relapsing course [3,4]. Furthermore, AD imposes the highest disability-adjusted life years (DALYs) burden compared to other dermatoses and is associated with numerous atopic and non-atopic comorbidities, such as asthma and allergic rhinitis, food allergy, and mental health disorders [2,5].
Anxiety and depression are leading causes of global disability and have been associated with AD. Recent systematic reviews and meta-analyses have examined the correlation between anxiety, depression, and AD and have found that patients with AD have a greater likelihood of presenting with depression predominantly in childhood and both disorders in adulthood. Furthermore, research has consistently discovered a positive association between anxiety in adults and children with AD, with higher mean scores for anxiety assessment tools [6]. However, no Mexican studies have established the prevalence of anxiety and depression symptoms in children, adolescents, and adults diagnosed with AD.
The effect of AD on patients' lives is substantial, as it restricts interpersonal relationships, negatively influences self-worth, and results in rejection and stigmatization. Therefore, the aim of this research is to determine the prevalence of anxiety and depression symptoms in Mexican patients diagnosed with AD and establish the correlation between the results obtained from the anxiety and depression scales and the different variables examined in the population. Our findings will assist in identifying the percentage of individuals in the Mexican population who may be at risk of developing mental health disorders because of their illness and in supporting the development of targeted interventions to improve the mental health of individuals with AD. Incorporating patient burden and comorbidities into the evaluation and management of patients with AD is critical to improving therapeutic decision-making and achieving superior patient outcomes.
Material and Methods
We conducted an observational, cross-sectional, and comparative study at the Regional Center of Allergy and Clinical Immunology at the Hospital Universitario "Dr. José Eleuterio González" in Monterrey, Nuevo León, Mexico, from November 5, 2021, to November 1, 2022. The study protocol was approved by the Research Ethics Committee and Ethics Committee of the Hospital Universitario "Dr. José Eleuterio González".
We included all patients over seven years old of both genders who were diagnosed with AD. Participants were verbally informed about the study's objective, and their queries were addressed to ensure their understanding. They were also given written assent and consent as appropriate. The study used two self-applicable physical screening questionnaires for anxiety and depression symptoms. Children and adolescents aged 7-17 years were administered the Spence Children's Anxiety Scale (SCAS) and the Kovacs Depression Inventory (CDI), while adults aged ≥8 years were given the Beck Depression Inventory-Second Edition (BDI-II) and the Beck Anxiety Inventory (BAI). The questionnaires took approximately 15 minutes to complete.
During the single study visit, we collected sociodemographic variables such as age, gender, and education and clinical variables such as the presence of concomitant atopic diseases, duration of symptoms, and severity of atopic dermatitis.
Overview of Assessment Tools used for Anxiety and Depression
Our study utilized various validated tools to assess anxiety and depression symptoms in both adults and children. The Beck Anxiety Inventory (BAI) is a popular tool used to measure anxiety symptoms in individuals and evaluate their severity based on various behavioral and symptomatic factors. It consists of four main factors, namely subjective, neurophysiological, autonomic, and panic, and has been validated across different settings and populations. The inventory includes 21 items evaluated on a 4-point scale, and a global score range of 0 to 63 points. A score of 16 points or more is considered clinically significant for anxiety, with scores ranging from 0-5 indicating minimal anxiety, 6-15 indicating mild anxiety, 16-30 indicating moderate anxiety, and 31-63 indicating severe anxiety [7]. The Beck Depression Inventory-Second Edition (BDI-II) is a commonly used tool to diagnose depression symptoms in adults. It evaluates the presence of depression symptoms, including both DSM-IV and DSM-V criteria and cognitive symptoms, through 21 items rated on a scale of 0 to 3. The BDI-II has strong psychometric properties and provides cutoff points for different levels of depression severity: 0-13 for minimum range, 14-19 for mild depression, 20-28 for moderate depression, and 29-63 for severe depression [8].
For assessing the severity of depressive symptoms in children and adolescents aged 7-17 years, we used the Kovacs Children's Depression Inventory (CDI). The CDI consists of 27 items scored on a 3-option scale, with a total score range of 0 to 54 points. The cutoff point that defines the presence of depressive symptoms is 19. This scale covers both expressions of classic depressive symptoms (such as crying, sadness, hopelessness, reduced motivation, difficulty sleeping, and feeling worthless) and manifestations of depression in two contexts: school and family (such as having no friends, feeling like a burden, worse and performance in school). [9]
The SCAS consists of 44 items scored on a 4-option scale that evaluates anxiety symptoms in children and adolescents. The evaluation is based on whether the level of anxiety is higher than that of other children and adolescents in their age and gender group and the severity of these symptoms. The scores are added and compared with the appropriate age and gender T-score. A T-score of less than 60 is classified as "normal and a T-score of 60 or higher suggests the presence of elevated anxiety that may require further investigation and confirmation through clinical evaluation [10].
Statistical Plan Analysis
Descriptive statistics reported frequencies and percentages for categorical variables. Measures of central tendency and dispersion (mean/median; standard deviation/interquartile range) were reported for quantitative variables after assessing the distribution of the variables using the Kolmogorov-Smirnov test. Categorical variables were compared using Pearson's chi-square test. For quantitative variables, independent groups were compared using the t-test or Mann-Whitney U- test. P<0.05 and a confidence interval of 95% were considered statistically significant. The statistical package SPSS version 25 was used. A minimum sample of 48 participants was required and calculated with a finite population sample formula.
Results
Patient Characteristics
We recruited 48 patients with AD, including 22 children, six adolescents, and 20 adults. The mean age of the participants was 17.1±9.8 years, with the third grade being the predominant level of education in children and the second grade of high school in adolescents. On the other hand, most adults (65%) had completed their undergraduate degree (Table 1). Only four patients had a medical record of anxiety/depression, one adolescent and three adults.
Children
Adolescents
Adults
Total
(n = 22)
(n = 6)
(n = 20)
(n = 48)
Age* (years)
9 ± 1.8
15.1 ± 1.8
26.6 ± 7.9
17.1 ± 9.8
Female gender n(%)
16 (72.7)
3 (50)
16 (80)
35 (72.9)
Current school year
1º elementary school
1 (4.5)
2º elementary school
5 (22.7)
3º elementary school
6 (27.3)
4º elementary school
3 (13.6)
5º elementary school
2 (9.1)
6º elementary school
5 (22.7)
1º junior high year
1 (16.7)
2º junior high year
1 (16.7)
3º junior high year
1 (16.7)
1º high school year
1 (16.7)
2º high school year
2 (33.3)
Highest level of education
Completed elementary school
0 (0)
Completed junior high
1 (5)
Completed high school
6 (30)
Bachelor’s degree
13 (65)
Note: *mean ± SD; +Measured with SCORAD (SCORing Atopic Dermatitis); NA: Not Applicable
Table 1: Demographic characteristics of patients.
Atopic History
The average length of time for which AD persisted was 118.2 months, and most patients in all three generational groups exhibited a mild form of the disease, with rates of 59.1%, 66.7%, and 60%, respectively. Only two patients (4.3%) presented with isolated AD, as most patients had at least one concurrent allergic disease (Table 2).
Children
Adolescents
Adults
Total
(n = 22)
(n = 6)
(n = 20)
(n = 48)
Time of evolution of atopic
72.3 ± 29.2
120 ± 25.1
168.2 ±
118.2 ±
Dermatitis in months.
Severity of atopic dermatitis+ n(%)
124.2
93.5
Mild
13 (59.1)
4 (66.7)
12 (60)
29 (60.4)
Moderate
8 (36.4)
2 (33.3)
3 (15)
13 (27.1)
Severe
1 (4.5)
0 (0)
5 (25)
6 (12.5)
Concomitant atopic diseases with AD n(%)
1 disease11 (50)
2 (33.3)
8 (40)
21 (43.7)
2 diseases
9 (40.9)
3 (50)
10 (50)
22 (45.8)
3 diseases
2 (9.1)
0 (0)
1 (5)
3 (6.2)
None
0 (0)
1 (16.7)
1 (5)
2 (4.3)
Note: *mean ± SD; +Measured with SCORAD (“SCORing Atopic Dermatitis”); AD: Atopic Dermatitis.
Table 2: Atopic History.
Approximately, 37.5% of the evaluated population had allergic rhinitis as the sole concomitant atopic disease, the most prevalent in all three generational groups.
This was followed by the combination of allergic rhinitis with allergic asthma and conjunctivitis, present in 29.1% and 14.5%, respectively. Three subjects in the study had four allergic diseases at the time of evaluation (AD and three other concomitant diseases) (Figure 1).
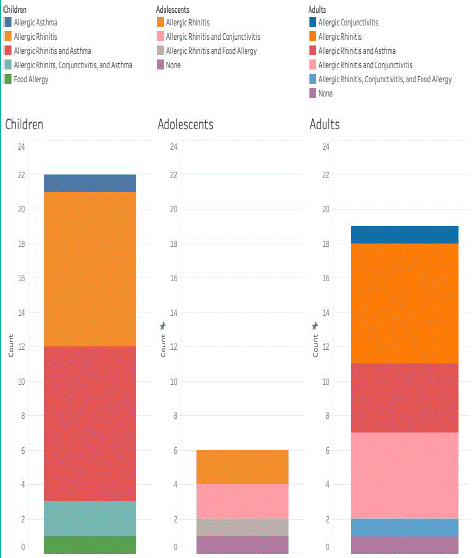
Figure 1: Allergic diseases concomitant to atopic dermatitis.
Symptoms of Anxiety and Depression in Children and Adolescents with Atopic Dermatitis
The presence of depressive symptoms was found in 2 patients, one in the children's group and another in the adolescents' group. Likewise, the presence of anxiety symptoms was reported in 6 children and one adolescent.
When evaluating the anxiety subgroups reported by the SCAS, the predominant traits in the children's group were separation anxiety and fear of physical injury, present in 45.5% of the sample. On the other hand, in the adolescents' group, the subgroups mentioned above were present in 50% of the sample and the subset of generalized anxiety (Table 3).
Children
Adolescents
(n = 22)
(n = 6)
Abandonment anxiety
10 (45.5)
3 (50)
Social phobia
6 (27.3)
1 (16.7)
Obssesive compulsive
3 (13.6)
3 (50)
Panic/Agoraphobia
6 (27.3)
1 (16.7)
Fear of physical injury
10 (45.5)
3 (50)
Generalized anxiety
8 (36.4)
3 (50)
Note: Data presented in n (%). SCAS ("Spence Children's Anxiety Scale").
Table 3: Anxiety subgroups in children and adolescents with the SCAS scale.
Number of concurrent atopic diseases
Anxiety symptoms
Present
Absent
p-value
None
0 (0)
1 (8.3)
One disease
2 25)
6 (50)
0.29
Two diseases
6 (75)
4 (33.3)
Three diseases
0 (0)
1 (8.3)
Number of concurrent atopic diseases
Depression symptoms
Present
Absent
p-value
None
1 (11.1)
0 (0)
One disease
3 (33.3)
5 (45.5)
0.508
Two diseases
5 (55.6)
5 (45.5)
Three diseases
0 (0)
1 (9.1)
Note: Calculated using Pearson’s chi-squared test.
Table 4: Relationship between anxiety and depression symptoms with the number of atopic diseases in adults with atopic dermatitis.
A chi-square test was conducted to evaluate the association between the presence of anxiety and the number of atopic diseases in groups of children and adolescents. In the group of children, having only one allergic disease had a protective effect for the presence of anxiety symptoms, with a p value of 0.052. No differences were found in the group of adolescents.
Symptoms of Anxiety and Depression in Adults with Atopic Dermatitis
Furthermore, we evaluated the presence of anxiety and depression symptoms in the adult population with the Beck scales. Patients with moderate and severe symptoms were considered to have clinically significant anxiety. On the other hand, clinically significant depression was assessed based on mild symptoms, as there are no established criteria to determine the score that demonstrates when it is clinically relevant. Out of the total sample, 40% exhibited significant clinical symptoms of anxiety. Regarding the severity of anxiety symptoms, 15% had minimal symptoms, 45% had mild symptoms, 25% had moderate symptoms, and 15% had severe symptoms. Similarly, 45% of the participants showed significant clinical symptoms of depression. In terms of the severity of depression symptoms, 55% had minimal symptoms, 20% had mild symptoms, 15% had moderate symptoms, and 10% had severe symptoms. These results suggest a high prevalence of anxiety and depression symptoms among adults with AD.
Within the depression symptoms, sleep pattern disorders had the highest score, followed by difficulty concentrating and energy loss. On the other hand, the lowest score was pessimism, followed by sadness and feelings of punishment. On the other hand, in the anxiety symptoms, the highest scores were obtained in the third factor (subjective symptoms of anxiety), followed by the first factor (panic).
Proportions of patients with anxiety and depression symptoms were compared to evaluate the presence of an association with age, gender, and number of atopic diseases. No statistically significant associations were found.
Symptoms of Anxiety and Depression by Age Group
A comparison was made of the proportions of anxiety and depression symptoms among patients with AD by age group. Statistically significant differences were found between the children and adults regarding depression symptoms (p=0.007), but not among adolescents. Moreover, no differences were found between groups in the presence of anxiety symptoms (p= 0.48).
The severity of Atopic Dermatitis and the Presence of Anxiety and Depression Symptoms
The presence of anxiety and depression symptoms was compared among the severity classifications of AD, which was measured using the SCORAD tool. No relationship was found between the presence of anxiety (p=.757) or depression (p= .221) and the severity of the atopic condition.
Duration of Atopic Dermatitis and the Presence of Anxiety and Depression Symptoms Additionally, the duration of AD was compared between patients with and without anxiety and depression symptoms. No statistically significant differences were found for anxiety in children (p=.427), adolescents (p=.350) or adults (p=.596) nor for depression on children (p=.991), adolescents (p=.350) or adults (p=.818).
Discussion
In this comparative survey study, 48 patients over the age of 7 with a diagnosis of dermatitis were recruited and interviewed and assessed using tools appropriate to their age group, to evaluate the prevalence of symptoms of anxiety and depression. We found a prevalence rate of depression of 4.5% and 16.7% for children and adolescents, respectively, as well as 27.3% and 16.6% for anxiety, respectively. The above findings are consistent with those reported in the general population, with anxiety being more prevalent than depression. In addition, significant clinical symptoms of anxiety and depression were present in the adult group, 40% and 45%, respectively.
Multiple comparisons were made between the presence and absence of the above conditions concerning the number of concurrent atopic diseases and the time and severity of AD, but no significant statistical differences were found. Other allergic disorders often accompany classic AD, and when not adequately controlled, it can substantially impact the mental health and quality of life of patients. Psychological problems such as anxiety and depression are considered more of a result than a cause of skin disorders, as AD is recognized as a chronic stress factor with implications for personal life. However, when patients have adequate control of their disease, as in most of our sample, it is difficult to find such statistical associations, but their relevance becomes tangible in clinical practice. In addition, the comparison between the presence and absence of depressive and anxiety symptoms is unfair due to the imbalance of the groups. Still, since the study's main objective was to determine the prevalence of these conditions in patients with AD, the intentional balance was not sought between their presence and absence.
Pinto L. et al. [11] determined an association between anxiety, depression, and AD in a prospective cross-sectional design in 31 adult patients in 2014. However, the instrument they used was the Hospital Anxiety and Depression Scale (HADS), which has a different sensitivity than the instrument used in this study (BDI-II), as reported by Le Fleur [12] in 2011. This would explain the discrepancy between the two populations.
This study has some limitations. Although an active attempt was made to balance the groups to obtain a better comparison, a convenience sampling at the Regional Center for Allergy and Clinical Immunology resulted in an imbalance between the groups. In addition, no single instrument is sensitive enough to evaluate the presence of symptoms of anxiety and depression in all three age groups, so using different tools limits the analysis. On the other hand, this study represents a milestone since, as far as our knowledge goes, it is the first of its kind in the Mexican population, which gives it strength.
Future research should focus on creating instruments that precisely measure the presence of anxiety and depression symptoms in patients with atopic diseases, as this population is one where a biological condition can result in psychological burden.
Additionally, it is essential to consider the overall severity of all atopic diseases, not just their presence, which could be a determinant in presenting symptoms of anxiety and depression.
Conclusion
In conclusion, this study suggests that patients diagnosed with AD have a prevalence of anxiety and depression symptoms like those reported in the general population. Despite not finding a higher prevalence in this group of patients, as some studies describe, we know that AD generates a significant burden on the patient and is one of the leading causes of DALYs lost. In addition, multiple atopic comorbidities can be found simultaneously and contribute even more to developing these symptoms. Therefore, it is crucial for allergists treating patients with this chronic skin condition to analyze these psychological and emotional aspects during the clinical course of the disease with the different screening tools available. The aim is to identify, refer and treat in a timely manner, along with a multidisciplinary team, patients with AD who are at risk of developing these mental health disorders.
References
- Langan SM, Irvine AD, Weidinger S. Atopic dermatitis. Lancet. 2020; 396: 345–60.
- Urban K, Chu S, Giesey RL, Mehrmal S, Uppal P, et al. The global, regional, and national burden of atopic dermatitis in 195 countries and territories: An ecological study from the Global Burden of Disease Study 2017. JAAD Int. 2021; 2: 12–8.
- Silverberg JI. Comorbidities and the impact of atopic dermatitis. Ann Allergy Asthma Immunol. 2019; 123: 144–51.
- Herrera-Sánchez DA, Hernández-Ojeda M, Vivas-Rosales IJ. Estudio epidemiológico sobre dermatitis atópica en México. Rev Alerg Mex. 2019; 66: 192–204.
- Laughter MR, Maymone MBC, Mashayekhi S, Arents BWM, Karimkhani C, et al. The global burden of atopic dermatitis: lessons from the Global Burden of Disease Study 1990-2017. Br J Dermatol. 2021; 184: 304–9.
- Rønnstad ATM, Halling-Overgaard A-S, Hamann CR, Skov L, Egeberg A, et al. Association of atopic dermatitis with depression, anxiety, and suicidal ideation in children and adults: A systematic review and meta-analysis. J Am Acad Dermatol. 2018; 79: 448-456.
- Guillén Díaz-Barriga C, González-Celis Rangel AL. Propiedades psicométricas del Inventario de Ansiedad de Beck en adultos asmáticos mexicanos. Psic y Sal. 2018; 29: 5–16.
- González DA, Reséndiz A, Reyes-Lagunes I. Adaptation of the BDI-II in Mexico. Salud Ment (Mex). 2015; 38: 237–44.
- The Spence Children’s Anxiety Scale. The Spence Children’s Anxiety Scale. 2021.
- Rivera CL, Bernal G, Rosselló J. The Children Depression Inventory (CDI) and the Beck Depression Inventory (BDI): Their validity as screening measures for major depression in a group of Puerto Rican adolescents. Int J Clin Health Psychol. 2005; 5: 485–98.
- Ferreira-Pinto L, Leite C, Delgado L, Moreira A, Lourinho I, et al. Evaluating an anxiety scale and Personality traits in Atopic Dermatitis and its relation with severity markers [dissertation]. 2014.
- Le-Fleur CC. Comparing the BDI-II and the HADS (HADS-D) as a screening tool for depression amongst HIV infected individuals attending a public health clinic [dissertation]. 2011.