Case Report
Austin J Dermatolog. 2014;1(1): 1005.
Scalp Haematoma – An Unusual Clinical Presentation of a Desmoplastic Neurotropic Melanoma
CLeitner1, VBisbiroulas1, VPapaefthymiou1, A Hall2, ELadoyanni1*
1Department of Dermatology, the Dudley Group Hospitals NHS Foundation Trust, UK
2Department of Radiology, Russells Hall Hospital, UK
*Corresponding author: Evmorfia Ladoyanni, The Dudley Group Hospitals NHS Foundation Trust, Department of Dermatology, Corbett Hospital, Vicarage Road, Stourbridge, DY8 4JB, United Kingdom,
Received: February 27, 2014; Accepted: April 16, 2014; Published: April 18, 2014
Abstract
Initial assessment of patients with unwitnessed head injuries is heavily reliant on an accurate patient history of preceding trauma. Initial management often follows blindly strict hospital protocols.
This is illustrated by the case of a 90 year old, demented man who developed a haematoma–like lesion on the scalp to the site of an unwitnessed head trauma. The haematoma was confirmed by a CT but instead of slow reabsorption of the bleed, an ulcerated, nodular lesion developed rapidly. On representation 6 months later, a skin biopsy diagnosed a desmoplastic neurotropic melanoma which was at that stage already metastasised.
Thinking outside the box when assessing patients with soft tissue masses at sites of presumed unwitnessed head trauma is vital and awareness of the limitations of diagnostic tools is essential for every clinician who potentially faces this situation, also dermatologists. Planned follow–ups reserved for this small patient cohort only could be life–saving.
Keywords: Desmoplastic neurotropic melanoma, Haematoma, Computer tomography, Soft tissue tumour
Abbreviations
CT–Computed Tomography; DNM – Desmoplastic Neurotropic Melanoma
Case Presentation
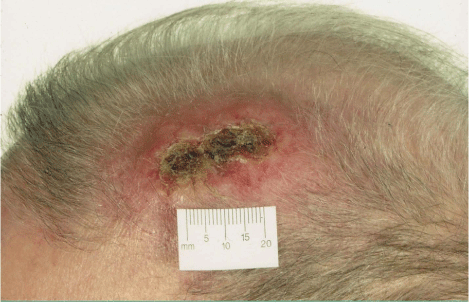
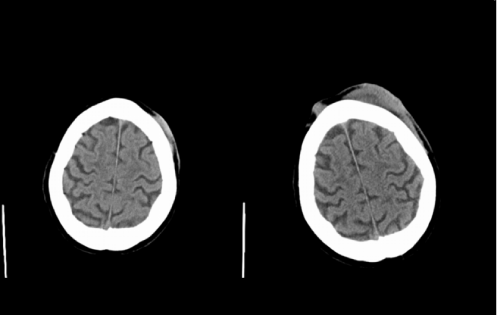
A 90–year–old man with known dementia and hypertension presented to the dermatology clinic with an ulcerated lesion on his left scalp (Figure 1). His daughter gave a history of an un witnessed trauma to this area caused by a metal bar six months prior which had caused bruising only. At the time of this presumed head trauma he had been admitted with acute confusion and a computed tomography (CT) scan of his head had ruled out an intracranial hemorrhage. It had however shown a small subcutaneous soft tissue swelling in the left fronto–parietal scalp that had been diagnosed as haematoma in correlation with the history (Figure 2a). The bruise did not resolve, and started enlarging suddenly and rapidly within 5 weeks prior to presentation to the dermatology department. Clinically, a 6x5cm indurate erythematous plaque with central ulceration was apparent on the left frontal scalp (Figure 1). No palpable regional lymphadenopathy was present. An incision skin biopsy revealed a desmoplastic neurotropic melanoma (DNM) of 5.23 mm thickness. The lesion was widely excised but metastases to scalp, lungs, cervical, and mediastinal lymph nodes developed subsequently and the patient passed away within six months of diagnosis. Comparison of the initial CT head with the staging CT six months later (Figure 2b), showed that the “haematoma” in the left fronto–parietal scalp had significantly increased in size and a new nodule in the right frontal scalp had appeared.
Figure 1: 6x5cm indurated erythematous plaque over left frontal scalp with a centralised, ulcerated area measuring 3x1cm.
Figure 2: Subcutaneous soft tissue mass in the left fronto-parietal scalp (2a) 6 months later: Increase in this mass and formation of a new nodule in the right frontal scalp (2b)
DNM is a subtype of desmoplastic melanoma, exhibiting prominent neurotropism. It presents commonly as inconspicuous, painless, firm, erythematous and amelanotic lesion on chronically sun–exposed skin [1] that can develop within a few months to several years [2]. In the head and neck area, cranial nerve involvement, nerve palsies, and tumor extension to the brain have been reported [2]. Clinical diagnosis can be difficult due to lack of characteristic features. Histologically, DNM should be considered for any scarlike spindle cell proliferation seen in chronically sun–exposed skin of elderly patients. Almost all DNMs demonstrate positive immune histochemistry to S–100, but are negative to HMB–45, Melan A, Mart–1, MITF, and tyrosinase. Wide local excision is treatment ofchoice [3]. Median tumor thickness and invasion have been reported to be greater at time of diagnosis and local recurrence rate higher when compared to other cutaneous melanomas [2]. Neurotropism, ulceration and tumor thickness have been associated with shorter recurrence time [3].
Literature on the appearance of melanoma and melanoma metastases on plain CT is limited. Probably, because this method of imaging is not specific enough for a conclusive diagnosis of soft tissue masses [4]. In general, malignant soft tissue tumors on CT are characterized by ill–defined, irregular borders with blurring of surrounding fat planes, and invasion of other structures. Necrosis and haemorrhage can cause in homogeneity in their appearance and challenges are imposed on radiologists when trying to distinguish malignant from benign lesions, especially in areas with limited surrounding fat to delineate tissue planes. Distinguishing between haematoma and soft tissue tumor on CT can be difficult, and a history of trauma provides normally an important clue on interpretation. Unfortunately in this case it was misleading. Haematoma during the acute phase displays increased attenuation on CT that may allow for a specific diagnosis. However, it evolves rapidly to a nonspecific appearance with iso or hypodensity. Conversely, tumors with internal haemorrhage can mimic haematoma [5]. Our patient's CT images are six months apart, and one would expect a decrease in size of the haematoma secondary to resorption. Instead, growth of the lesion suggested neoplasia. The loss of occasional hyperdensity on the second scan might be due to a resolving intra–tumoralhaemorrhage.
Conclusion
Management of head injuries is often protocol–driven and the diagnosis heavily reliant on an accurate history. Initial assessment of soft tissue changes on the scalp and reassessment of non–resolving clinical cutaneous signs in patients with an unwitnessed preceding head trauma requires lateral thinking. Clinicians need to be aware that a CT is not reliable in diagnosing soft tissue changes [4]. If there is a high suspicion of underlying cutaneous malignancy, a skin biopsy to a site of previous trauma has the best diagnostic yield and should be considered early. A planned follow–up of patients with an uncertain and un witnessed history of preceding trauma accompanied by soft tissue changes to the scalp could be potentially life–saving. In this case a review at four weeks would have been adequate to assess if the bruise had resolved.
Acknowledgement
We would like to thank Dr. Eduardo Calonje, Consultant and Director of Histopathology, St. John's Institute of Dermatology, St. Thomas Hospital, London for making the histological diagnosis.
References
- Quinn MJ, Crotty KA, Thompson JF, Coates AS, O'Brien CJ, McCarthy WH. Desmoplastic and desmoplastic neurotropic melanoma: experience with 280 patients. Cancer 1998; 83: 1128-1135.
- Carlson JA, Dickersin GR, Sober AJ, Barnhill RL. Desmoplastic neurotropic melanoma. A clinicopathologic analysis of 28 cases. Cancer 1995; 75: 478-494.
- Chen JY, Hruby G, Scolyer RA, Murali R, Hong A, Fitzgerald P et al. Desmoplastic neurotropic melanoma: a clinicopathalogic analysis of 128 cases. Cancer 2008; 113: pp. 2770-2778.
- Beaman FD, Kransdorf MJ, Andrews TR, Murphey MD, Arcara LK, Keeling JH. Superficial Soft-Tissue Masses: Analysis, Diagnosis, and Differential Considerations. Radio Graphics 2007; 27: 509-523.
- Weekes RG, McLeod RA, Reiman HM, Pritchard DJ. CT of soft tissue neoplasms. AJR Am J Roentgenol.1985; 144: 355-360.