Review Article
Austin J Dermatolog. 2014;1(2): 1006.
Facial Dermal Melanocytosis
Shinichi Watanabe*
Department of Dermatology, Teikyo University School of Medicine, Japan
*Corresponding author: Shinichi Watanabe, Department of Dermatology, Teikyo University School of Medicine, 11-1. Kaga-2, Itabashi, Tokyo 173-8605, Japan
Received: March 29, 2014; Accepted: April 28, 2014; Published: April 30, 2014
Abstract
From the standpoint of age of onset, there is overlap between classical nevus of Ota and Hori’s or Sun’s nevus. The distribution of pigmentation is identical between nevus of Ota and Hori’s nevi, although mostly unilateral in nevus of Ota. The histology of Hori’s and Sun’s nevi is identical to nevus of Ota. These late-onset dermal melanocytoses appearing on the face can be treated by Q-switched lasers, as is the case with nevus of Ota. Therefore, these dermal melanocytoses are included in the same disorder, which we propose calling facial dermal melanocytosis (FDM). They are more common than infantile onset cases and are frequently observed in Asian countries. In our study of patients who complained of acquired hypermelanosis appearing on the face, 12.2% were diagnosed as FDM. If “dark rings under the eyes” is included in this category, the incidence of FDM is very high. Adult onset FDM is frequently and persistently confused with the other commonly acquired hypermelanosis, suchas melasma, ephelides, and solar lentigines. Misdiagnosis induces malpractice, because FDM can be treated easily by Q–switched lasers. Therefore, FDM signify differential diagnosis from the other acquired hypermelanosis.
Keywords: Facial; Melanocytosis
Abbreviations
FDM: Facial Dermal Melanocytosis
Introduction
Disorders of melanin pigmentation can be divided on morphological grounds into two types. The first is hypermelanosis, where there is an increased amount of melanin in the skin. The second type is hypomelanosis, where there is a lack of pigment in the skin. Furthermore, hypermelanosis can be divided on histological grounds into epidermal hypermelanosis, dermal hypermelanosis, and mixed epidermal and dermal hypermelanosis. Histological features of dermal hypermelanosis include pigment incontinence with accumulation of melanophages and increased melanin in dermal melanocytes. The dermal hypermelanois due to the presence of melanin–producing dendritic melanocytes that lie in the dermis is named dermal melanocytosis, which includes nevus of Ota, nevus of Ito, Mongolian spots.
Pigmentary disorders appearing on the face, even if they are benign, frequently cause cosmetic and psychological problems to many people, especially women and can lead to the appearance of increased facial aging. These are perceived by some to be an inevitable outward sign of the aging process. However, it is felt by others to be an event that should be delayed or prevented if possible. These facial pigmentations include solar lentigines, pigmented seborrheic keratoses, melasma, nevus of Ota, and facial hypermelanosis fromother causes.
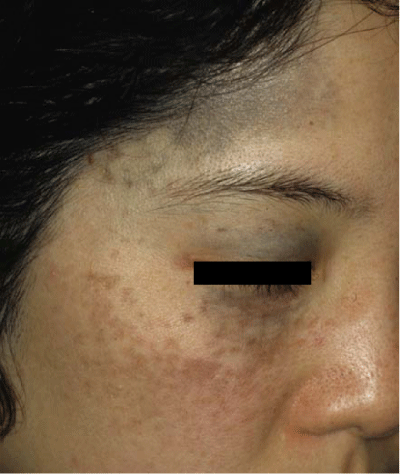
Figure 1: Typical case of nevus of Ota.
Dermal melanocytosis is usually localized, especially common among Asians, and mostly developmental or heritable in origin. Clinically, it shares bluish–grey coloration. When a sufficient number of melanin–containing cells are present in the dermis, various clinical forms are reported, depending on their onset and distribution. While most dermal melanocytosis are congenital or have an onset in early childhood, there is a group that is clearly acquired, with an onset in adult life. Mongolian spots typically disappear in childhood; other dermal melanocytosis persist for life. In this article, dermal melanocytosis appearing on the face, named facial dermal melanocytosis (FDM) [1], has been reviewed.
History of facial dermal melanocytosis (FDM)
Nevus of Ota
Representative of dermal melanocytosis appearing on the face is nevus of Ota (Figure 1). In Japan, bluish–gray hyper pigmentation on the side of the face has been well known for a long time and was considered as Mongolian spots appearing on the face. Mongolian spots, however, are seen most commonly in the sacral region, although they may occur on any portion of the body, and they usually are noted at birth and disappear within a few years. In 1939, therefore, Professor Ota characterized these cases of aberrant Mongolian spots located on the face and involving the eye, and descriptively named the disorder Naevus fusco–caeruleus ophthalmomaxillaris [2,3]. Since then, this pigmentary disorder, which is common in Asians but rare in Caucasians, has been widely known as nevus of Ota. In 1956, Fitzpatrick [4] renamed the syndrome oculodermal melanocytosis. However, ocular involvement is not always associated with such patients, especially in the Japanese cases.
Symmetrical type of nevus of Ota
In 1939, Professor Ota’s pupil Tanino classified his original 26 cases into four types [5]: (1) mild, including two subtypes: (a) orbital, and (b) zygomatic; (2) moderate; (3) intensive; and (4) bilateral. 5–8% of patients demonstrate bilateral pigmentation [6–8]. In 1965, Hidano classified bilateral type of nevus of Ota into two types [8]: symmetric and asymmetric. The asymmetric type is usually moderate to severe, and the extent or severity of pigmentation is different between the right and left side of the face. However, the symmetrical type is different from classical nevus of Ota. Characteristic features of the symmetrical type were summarized by Hidano as follows: symmetric distribution; mild and brown–dominant small spots scattered on lateral sites of the forehead, upper and lower eyelids, and malar area (Figure 2); no mucosal pigmentation; rare and slight ocular pigmentation; late onset (at ages 10˜30); a marked female preponderance; and some family history. Hidano noted that this type of nevus of Ota appeared after 20 years of age in 1⁄3 of the patients and was frequently misdiagnosed as ephelides. Hidano proposed, therefore, that it is a new clinical entity with slight differences from classical nevus of Ota.
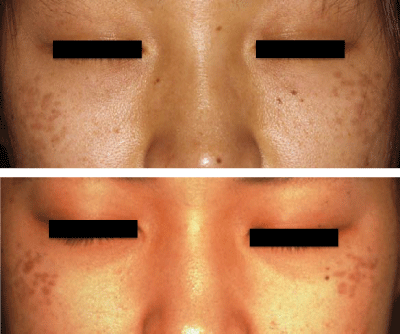
Figure 2: Patients with symmetrical type of nevus of Ota named by Hidano. This pigmentation on the cheeks appeared in puberty and has been misdiagnosed as ephelides. Clinical manifestation forms as discrete macules or speckled pigmentation.
Acquired, bilateral nevus of Ota–like macules (Hori’s nevus)
In 1984, Hori et al reported that 22 of blue–brown macules of the face occurred on both sides of the forehead, temple, eyelids, malar area, alae of the nose, and root of the nose in middle-aged Japanese women [9]. The age of onset ranged from 19 to 69. Pigmented macules consist of blue–brown and/or slate–gray small patches (Figure 3). No patientshad ocular or mucosal pigmentation. The differential diagnosis includes nevus of Ota, Riel’s melanoses, and melasma. However, the same conditions had already been described in Japanese literature in 1982 as bilateral nevus of Ota by Ogino [10] and as symmetrical nevusof Ota by Harada and Niizuma [11] who noted that 1/4 of the cases had been misdiagnosed as Riehl’s melanoses, and were also described as a symmetrical variety of bilateral nevus of Ota in English literature in 1983 by Hidano [12].
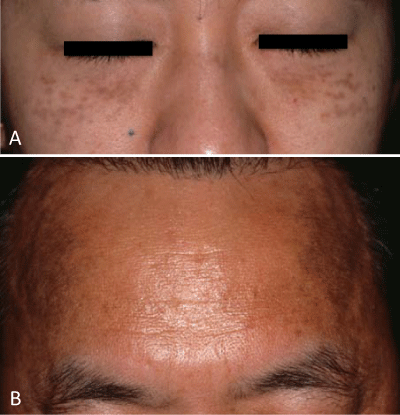
Figure 3: Patients with acquired, bilateral nevus of Ota-like macules (Hori's nevus). A: Pigmentation on the infraorbital area appears as confluent macules, but pigmentaion on the cheeks forms discrete macules, in the same manner as Sun's nevus or symmetrical type of nevus of Ota. B: Symmetrical dark brown pigmentation on the temples is observed in this patient. Differential diagnosis is difficult, but the pigmentation is not uniform in color and the border is not clear, which differentiates it from melasma.
Nevus fusco–caeruleus zygomaticus (Sun’s speckled nevus)
In 1987, Sun et al reported the nevus presenting as a bilateral speckled discoloration of the skin of the face principally in the zygomatic region [13]. The condition usually does not become apparent until the second decade of life, and is much more common in females. No association with any other abnormalities was found. There was a positive family history in 18% of the cases. There was a much higher incidence in the general population in Taiwan. This nevus is very similar to the symmetrical type of nevus of Ota proposed by Hidano in the view of clinical manifestations and family history. The difference is age of onset. In their study, however, 40% of the patients developed the condition before reaching 20 years of age, and 5.5% developed before their 10th birthday. There is a considerable overlap of age of onset between Nevus fusco–caeruleus zygomaticus and symmetrical type of nevus of Ota. A slight difference in the sex ratio and age of onset between these diseases may depend on the difference between clinic–based or community–based studies.
Infraorbital ring–shaped melanosis (dark rings under the eyes)
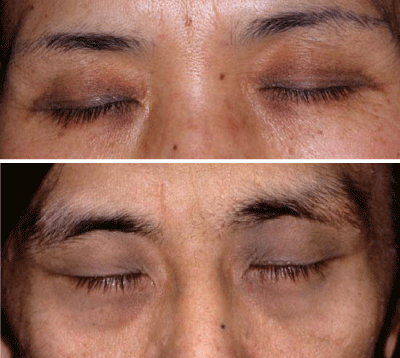
The so called “dark rings under the eyes”, an expression used by many ordinary people, indicates pigment macules under the eyes which are prominent and appear as a condition of general fatigue, especially with regards to insufficient sleep. Similar fluctuation of color tone is frequently noticed by attentive patients with nevus of Ota or their parents [14,15] during or before menstruation, after insufficient sleep, and⁄or when the patients are tired or sick. Some patients with unilateral nevus of Ota complain of homogeneous pigment macules on the infra orbital area on the opposite side of the face after significant improvement of the unilateral nevus by Q–switched ruby laser (QSRL). After careful examination of patients with unilateral nevus of Ota, we observed a different degree of homogeneous pigment macule on the infra orbital area of the opposite side in the same patients, which was usually not mentioned by patients. Therefore, we performed a skin biopsy of the pigmented macule on the infra orbital area taken from the 12 patients who complained of dark rings under the eyes. Histological, all 12 patients indicated dermal melanocytosis, which was confirmed by the Masson–Fontana silver stain and staining against S100 [16]. In addition, the above pigmented macule under the eye can be successfully treated with QSRL (Figure 4) in the same way as conventional nevus of Ota [17]. We speculate that a so–called dark ring under the eyes in the Japanese population is a kind of dermal melanocytosis which can be successfully treated by QSRL. We would like to propose, therefore, the term, “infra orbital ring–shaped melanosis” to describe the dark rings under the eyes caused by dermal melanocytosis, as suggested by the reviewer of our paper [16]. There remains one question: why does the darkness of the lesion caused by dermal melanocytosis change day by day, depending on the status of the host? We suspect that thickening of the dermis, mainly caused by edema, leads to an enhanced incidence of diffused light reflection from the pigments, which then results in increased darkness of the skin.
Figure 4: Patient who complained of dark rings under the eyes before and after Q-switched ruby laser treatment. A: Before laser treatment, B: After 3 laser treatments. After laser treatment, infraorbital ring-shaped melanosis has effectively disappeared.
Peiorbital ring–shaped melanosis (Panda–like nevus of Ota)
We have seen patients with homogenous pigment macules on bilateral periorbital area (Figure 5). These patients indicated dermal melanocytosis confirmed by histological examination. In addition, there are two papers [18,19] which described similar cases to ours. Therefore, we would like to propose the name, “periorbital ringshaped melanosis (Panda–like nevus of Ota)” for homogenous pigment macules on the bilateral periorbital area caused by dermal melanocytosis. This condition has been frequently observed among Indians. Therefore peiorbital ring–shaped melanosis may be common in Indians, although histological confirmation is required.
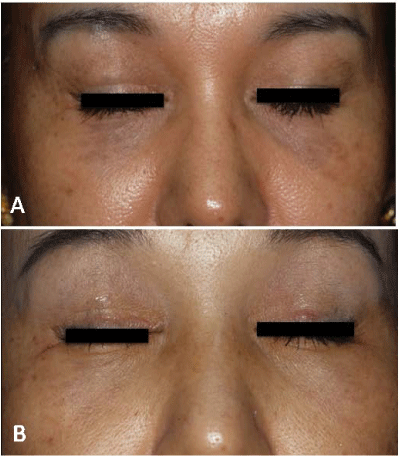
Figure 5: Homogeneous pigment macules on bilateral periorbital area (periorbital ring-shaped melanosis). Dermal melanocytes are confirmed by histological examination.
Classification of FDM
Nevus of Ota shares bluish–grey coloration. The blue skin color results from a decreased diffuse reflectance in the longer wavelength red region of the visible spectrum as compared to the surrounding normal skin. Melanocytes scattered in the upper dermis give a brownish–blue tint while those confirmed to the lower dermis appear more uniformly blue. Therefore, melanocytes located just beneath the epidermis give a brownish tint and may be misdiagnosed as brown birthmarks such as café–au–lait macule. Therefore, we would like to propose the name, “Café–au–lait macules–like nevus of Ota” for a demarcated brownish macule in patients with nevus of Ota (Figure 6).
Figure 6: Brownish macule in a patient with nevus of Ota, which is frequently misdiagnosed as a café-au-lait macule.
In the viewpoint of age of onset, there is overlap between classical nevus of Ota and Hori’s or Sun’s nevus. The distribution of pigmentation is identical between nevus of Ota and Hori’s nevi, although mostly unilateral in nevus of Ota. The histology of Hori’s and Sun’s nevi is identical to nevus of Ota. The late–onset facial dermal melanocytosis can be treated by Q–switched lasers [20], as is the case with nevus of Ota, although Hori’s or Sun’s nevus usually show quicker responses to laser treatment because the number of dermal melanocytes is less in Hori’s nevus than in classical nevus of Ota. Therefore, Hori’s nevus, Sun’s nevus, symmetrical type of nevus of Ota, and the symmetrical variety of nevus of Ota are included in the same disorder and classified as shown in Table 1.
- Classical Nevus of Ota
- Café-au-lait macules-like Nevus of Ota
- Ephelides-like Nevus of Ota
- Symmetrical type of nevus of Ota (Hidano)
- Naevus fusco-caeruleus zygomaticus (Sun's speckled naevus )
- Acquired, bilateral nevus of Ota-like macules(Hori's nevus)
- Peiorbital ring-shaped melanosis (Panda-like nevus of Ota)
- Infraorbital ring-shaped melanosis(Dark rings under the eyes)
Table 1: Facial Dermal Melanocytosis (FDM).
Differentiation
There are many differential diagnosis of FDM, especially in acquired cases with adult onset such as Hori’s nevus or Sun’s speckled naevus from the other adult onset pigmentary disorders appearing on the face. This is because they show a variety of clinical features in color, distribution, size, and onset.
Cafe–au–lait macule
A demarcated brownish macule in patients with nevus of Ota is frequently misdiagnosed as a café–au–lait macule (Figure 6). Differentiation is based on the age of onset; the café–au–lait macule is usually present at birth, however, nevus of Ota is not usually present at birth, although more than half appear within one year after birth. The border of nevus of Ota is less clear and the color of nevus is usually darker than that of café–au–lait macule.
Ephelides
Brownish spots in patients with nevus of Ota are frequently misdiagnosed as ephelides (Figure 2). Ephelides are tan–tobrown pigmented macules of smaller size which appear during early childhood and are commonly dispersed over the face. Their appearance varies seasonally, being darker and more confluent in the summer and fainter in the winter. Ephelides, as described in the standard textbook [21], are very rare in Japan and probably in Asia as a whole. However, the symmetrical type of nevus of Ota or Sun’s nevus commonly appears in and after puberty, mainly on the zygomatic area without seasonal changes.
Melasma
Melasma is classified into epidermal, dermal, and mixed types by Wood’s lamp examination. Recent histopathological examinations [22,23], however, denied the presence of dermal type melasma. Most cases of dermal type of melasma, therefore, are considered to be Hori’s nevus, Riel’s melanoses or some incontinentia pigmenti histologica, which show good response to Q–switched laser treatment. In fact, a case of Hori’s nevus and a case of widespread vitiligo have been presented as melasma in commercial leaflets published by some laser companies.
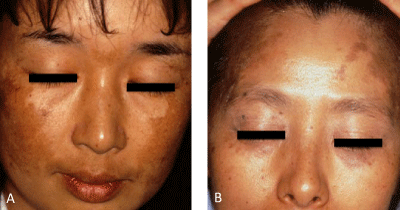
Bilateral pigmented macules in patients with adult onset such as Hori’s nevus are frequently misdiagnosed as melasma. Melasma appears only on sun–exposed areas, for example post inflammatory pigmentation after sun exposure. In melasma, therefore, the periorbital area is never involved (Figure 7A), and alae of the nose or root of the nose alone are very rare, although pigment distribution is mostly symmetrical and similar to that of Hori’s nevus. Melasma is usually well–demarcated and uniform in color (Figure 7A), but rarely mottled. In Hori’s nevus, however, the border is less clear, the color contains a blue or purple–brown tint (Figure 3, Figure 7B), and pigmentation is sometimes speckled. Melasma is exacerbated by sun exposure and lightened by long–term sun protection, while Hori’s nevus is rarely influenced by sun exposure. The treatment required of each condition is very different; Q–switched lasers are the only choice for the treatment of adult onset dermal melanocytosis, while topical hydroquinone is one of the best choices for the treatment of melasma. Therefore, accurate diagnosis is the key to success in the treatment ofthese pigmented lesions.
Figure 7: Comparison of melasma (Figure 7A) with acquired, bilateral nevus of Ota-like macules (Hori's nevus) (Figure 7B). A: The periorbital area is not involved, and the pigmentation is well-demarcated and uniform in color. B: This discoloration, especially brown pigmentation on the temples is frequently misdiagnosed as melasma, but is different from melasma because of periorbital involvement and the brownish to purple tint, which can be observed on the infraorbital area in this patient (infraorbital ring-shaped melanosis).
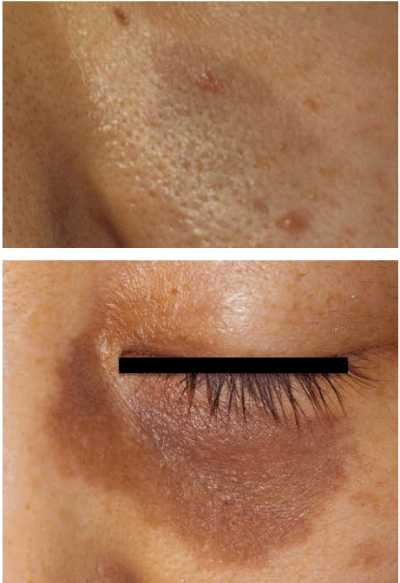
Solar lentigines
Solar lentigines are usually macular lesions with a uniform shade of brown and have an irregular edge, although the size and color are variable. The late–onset FDM shows symmetrical distribution, but solar lentigines are not symmetrical and appear not only on the cheek, but also widely on the sun–exposed areas. The border of FDM is less clear and the color of FDM contains a blue or purple–brown tint. Elderly patients with FDM, however, can be associated with solar lentigines.
Melanocytic tumor
Melanocytic tumors such as congenital nevomelanocytic nevi, common acquired nevomelanocytic nevi, and blue nevi are tumors of nevomelanocytes or blue nevus cells. They are dark pigmented papulo–nodular lesions and are usually elevated. However, FDM is flat pigmented macules with a smooth surface, and have no papulonodular or palpable lesions.
Prevalence of patients with FDM among acquired melanoses appearing on the face
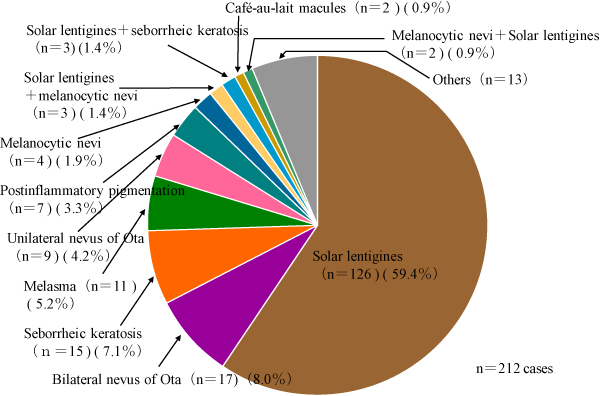
We analyzed patients complaining of pigmented lesions on the face who came to the Department of Dermatology, Teikyo University School of Medicine from November 1998 to April 2000 [24]. We made a diagnosis of these patients based on the clinical and, if necessary, pathological observations. The diagnoses of 212 patients complaining of acquired melanoses appearing on the face were solar lentigo 126 (59.4%), bilateral nevus of Ota 17 (8.0%), seborrheic keratosis 15 (7.1%), melasma 11 (5.2%), unilateral nevus of Ota 9 (4.2%), etc (Figure 8). Our study showed there were a relatively small numberof patients with melasma among those cases. This may be related to the timing of the observation period, which includes only one summer season, since melasma is usually obvious in summer season. In addition, our survey revealed FDM was not rare and accounted for 12.2% of the patients who complained of acquired melanoses on the face.
Figure 8: Diagnosis of patients complaining of acquired melanoses appearing on the face. The diagnoses of 212 patients complaining of acquired melanoses were solar lentigines 126 (59.4%), bilateral nevus of Ota including Hori's nevus 17 (8.0%), seborrheic keratosis 15 (7.1%), melasma 11 (5.2%), Unilateral nevus of Ota 9 (4.2%), postinflammatory pigmentation 7 (3.3%), solar lentigo + nevus cell nevus 5 (2.4%), nevus cell nevus 4 (1.9%), solar lentigines + seborrheic keratosis 3 (1.4%), and café-au-lait macules 2 (0.9%).
Treatment
Selective photothermolysis using the Q–switched lasers with nanosecond pulse–width is a safe and effective method for lightening or eliminating dermal melanocytosis in all patients without any permanent side effects (Figure 4), although transient post inflammatory pigmentation with a peak at one month after laser treatment is sometimes observed, but spontaneously fades gradually over 3 to 4 months. Hypo pigmentation is sometimes reported in patients who received numerous sessions of lasertreatment. This may be due to the short interval of the treatment, since epidermal melanocytes in the post inflammatory pigmentation are activated by the treatment and contain a lot of melanin. They are, therefore, sensitive to laser light and easily destroyed by additionallaser treatment, resulting in permanent hypo pigmentation. It isimportant, therefore, to avoid laser treatment when the target lesions show post inflammatory pigmentation. The efficacy rate by lasertreatment increased with the number of treatments, and usually reached a level of 100% at five or more treatments. The number of treatments depends on the number of dermal melanocytes: darker lesions need more treatments. Pigmentation on the periorbital areas is less sensitive to laser treatment than on the cheek or forehead due to reduced back scattering of laser light in the area located on the soft tissue than on the hard tissue such as bone. However, periorbital pigmentation can be treated by Q–switched lasers.
Conclusion
FDM is not always congenital, but almost always acquired. It appears at any age. Adult–onset cases appear usually as bilateral, light blue–brown pigmentation and become more confluent and grey. They are more common than infantile onset cases and are frequently observed in Asian countries, such as Japan, Korea, and China. A population–based study described the overall incidence of FDM to be 0.8% in Taiwan, with a marked preponderance in women. In our study of patients who complain of acquired melanoses appearing on the face, 12.2% were diagnosed as FDM [24]. If “dark rings under the eyes” is included in this category, the incidence of facial dermal melanocytosis is very high.
Adult onset FDM is frequently and persistently confused with the other common acquired melanoses, such as melasma, ephelides, andsolar lentigines. Therefore, FDM, which is a curable pigmentation by Q–switched lasers, signifies differential diagnosis from the other acquired melanoses.
References
- Watanabe S. Facial dermal melanocytosis: Nevus of Ota and its related dermal melanocytoses. In: Asian skin and skin diseases, special book of the 22nd World Congress of Dermatology. Seoul: Medrang Inc. 2011; 283-291.
- Ota M, Tanino H. Nevus fusco-coeruleus ophthalmomaxillaris and its relationship to pigmentary changes in the eye. Jikeikai Med J. 1939; 63: 1243-1244.
- Ota M. Naevus fusco-caeruleus ophthalmomaxillaris. Jpn J Dermatol. 1939; 46: 369-399.
- Fitzpatrick TB, Kitamura H, Kukita A, Zeller R. Ocular and dermal melanocytosis. AMA Arch Ophthalmol. 1956; 56: 830-832.
- Tanino H. Über eine in Japan häufig vorkommende Nävusform: Naevus fusco-caeruleus ophthalmo-maxillaris Ota: I. Beobachtung über Lokalisation, Verfärbung, Anordnung und histologische Veränderung. Jap J Dermatol Urol. 1939; 46: 107-111.
- Yoshida K. Nevus fusco-caeruleus ophthalmomaxillaris of Ota. Tohoku J Exp Med. 1952; 55: 34-43.
- Inoue K. Nevus of Ota. Hifu Rinshoh. 1968; 10: 122-136.
- Hidano A, Kajima H. Bilateral nevus of Ota. Hifu Rinshoh. 1965; 7: 72-81.
- Hori Y, Kawashima M, Oohara K, Kukita A . Acquired, bilateral nevus of Ota-like macules. J Am Acad Dermatol. 1984; 10: 961-964.
- Ogino A: Bilateral nevus of Ota diagnosed falsely as pigmented contact dermatitis. Rinshoh hifu. 1982; 36: 875-878.
- Harada S, Niizuma T. Symmetrical nevus of Ota. Hifubyo Shinryo. 1982; 4: 727-730.
- Hidano A, Kaneko k. Symmetrical variety of bilateral nevus of Ota. Kukita A, Seiji M, editors. In: Proceedings of the 16th International Congress of Dermatology: Tokyo: University of Tokyo Press. 1983; 683.
- Sun CC, Lü YC, Lee EF, Nakagawa H. Naevus fusco-caeruleus zygomaticus. Br J Dermatol. 1987; 117: 545-553.
- Hidano A, Kajima H, Ikeda S, Mizutani H, Miyasato H, Niimura M. Natural history of nevus of Ota. Arch Dermatol. 1967; 95: 187-195.
- Mori H, Furuya H, Watanabe S. Statistical study of 280 patients with nevus of Ota. Jpn J Dermatol. 1999; 109: 1603-1607.
- Watanabe S, Nakai K, Ohnishi T. Condition known as "dark rings under the eyes" in the Japanese population is a kind of dermal melanocytosis which can be successfully treated by Q-switched ruby laser. Dermatol Surg. 2006; 32: 785-789.
- Watanabe S, Takahashi H. Treatment of nevus of Ota with the Q-switched ruby laser. N Engl J Med. 1994; 331: 1745-1750.
- Kolde G, Schmollack KP, Sterry W. [Periorbital hyperpigmentation. Bilateral nevus of Ota]. Hautarzt. 2001; 52: 460-463.
- Turnbull JR, Assaf Ch, Zouboulis C, Tebbe B. Bilateral naevus of Ota: a rare manifestation in a Caucasian. J Eur Acad Dermatol Venereol. 2004; 18: 353-355.
- Watanabe S. Basics of laser application to dermatology. Arch Dermatol Res. 2008; 300 Suppl 1: S21-30.
- Anstey AV. Disorders of skin colour. 8th edn. In: Rook's Textbook of Dermatology. Wiley-Blackwell. 2010; 58.10-58.11.
- Sanchez NP, Pathak MA, Sato S, Fitzpatrick TB, Sanchez JL, Mihm MC Jr. Melasma: a clinical, light microscopic, ultrastructural, and immunofluorescence study. J Am Acad Dermatol. 1981; 4: 698-710.
- Kang WH, Yoon KH, Lee ES, Kim J, Lee KB, Yim H, et al. Melasma: histopathological characteristics in 56 Korean patients. Br J Dermatol. 2002; 146: 228-237.
- Watanabe S. Study of the patients complaining of melasma or ephelides, Nihon Kohshohin Kagaku Kaishi. 2000; 24: 287-295.