
Clinical Image
Austin J Emergency & Crit Care Med. 2019; 5(1): 1068.
To Look for a Needle in the Haystack: An Uncommon Cause of Endocarditis
Berlot G1*, Tomasini A1, Roman-Ponuz E1, Bussani R2
¹Department of Anesthesia and Intensive Care, University of Trieste, Italy
²Department of Pathological Anatomy, University of Trieste, Italy
*Corresponding author: Giorgio Berlot, Department of Anesthesia and Intensive Care, Cattinara Hospital, Strada di Fiume 447, University of Trieste, Italy
Received: November 25, 2019; Accepted: December 28, 2019; Published: December 31, 2019
Clinical Image
A 39/year/old man with a long-term history of iv. drug abuse was admitted to our ICU in coma. At the brain CT-scan, multiple bilateral hypodensities were present and a Trans-Esophageal Echocardiography (TEE) demonstrated a massive endocarditis involving the tricuspid, the aortic and the mitral valves. He died 3 days later due to the occurrence of a multiple organ failure. At the autopsy, septic embolus’s were found in all organs; the examination of the heart not only confirmed the TEE findings (Figure 1) but a 15mm-long distal part of a needle was retrieved from the right side of the interventricular septum causing an abscess penetrating in the left ventricle which caused the left-sided endocarditis (Figure 2). The admission imaging were reviewed by physicians other than those involved in the initial evaluation and unaware of the correct diagnosis but again the foreign body was not identified likely due its small size.
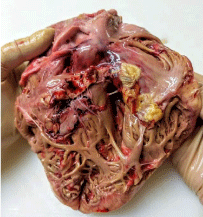
Figure 1: Massive tricuspidal end ocarditis and septal penetrating abscess.
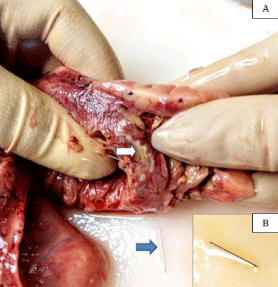
Figure 2: Panel A: Interventricular abscess and necrotic area (white arrow)
where the needle (blue arrow) (B) was located. Panel B: The retrieved needle.