
Case Report
Austin Emerg Med. 2016; 2(7): 1036.
Off-Pump Coronary Artery Bypass Complicated with Third Nerve Palsy: A Case Report
Nasiri B1, Tloee M1, Taban Sadeghi M1*, Sabzi F2 and Naseri Alavi SA3
1Cardiovascular Research Center, Tabriz University of Medical Sciences, Tabriz, Iran
2Kermanshah University of Medical Sciences, Kermanshah, Iran
3Department of Neurosurgery, Tabriz University of Medical Sciences, Tabriz, Iran
*Corresponding author: Mohammadreza Taban Sadeghi, Cardiovascular Research Center, Tabriz University of Medical Sciences, Tabriz, Iran
Received: June 28, 2016; Accepted: August 08, 2016; Published: August 10, 2016
Abstract
Pituitary apoplexy is a clinical syndrome caused by an acute ischemic or hemorrhagic vascular accident involving a pituitary adenoma or an adjacent pituitary gland. We report an exceedingly rare case of unknown pituitary adenoma that after three-vessel off-pump coronary artery bypass grafting (OPCAB) complicated by hemorrhage. The patient showed hyponatremia, fever, lethargy after surgery. CABG with cardiopulmonary bypass (CPB) is not recommended for patients with neurologic problems such as previous stroke or tumor, however OPCAB also may complicated by pituitary hemorrhage. This case report is the second to describe pituitary hemorrhage after OPCAB. The patient referred for surgery in a neurosurgery center and underwent transesphenoidal resection of adenoma. The sign and symptom of the occulomotor nerve palsy recovered partially in 6th month of follow-up.
Keywords: Coronary artery bypass; Third Nerve Palsy; Pituitary Adenoma
Introduction
Pressure affects on subarachnoid plexus or increasing cerebrospinal fluid production followed by displacement of third nerve and optic nerve. It can make specific sign and symptom such as eye’s field defect, eye’s glob muscles plegia, anisocoria, changing the level of consciousness from delirium to coma, change in mental status, and focal neurologic deficit [1]. Disruption of the hypothalamicpituitary- adrenal axis’s way in adenoma necrosis caused primary hypopitutarisem and secondary adrenal deficiency [2]. Pituitary damage cannot disable function of Aldosterone-secreting cells of the adrenal cortex because its function depends on the renin–angiotensin system and potassium levels of stimulation; however, cortisol is produced in the zone fasciculate by the hypothalamus-pituitaryadrenal axis, that the disruption of this way causes post operative hypocortisolism and subsequent hyponatremia [3]. Coronary artery bypass graft surgery (CABG) is one of the main therapies of patients suffering from coronary artery disease (CAD). There are two methods for performing CABG: Off pump CABG and on pump CABG [4]. In on-pump CABG the heart will stop during the surgery. Cardiopulmonary bypass (CPB) machine supply the body’s blood. While the heart is stopped the surgeon operates the graft procedure. After the grafting procedure complete, the patient is removed from the machine. In off-pump CABG, the surgeon sewing the vessel on the pumping heart. Off pump CABG is a newer procedure to On-pump CABG and doesn’t need to use the CPB machine. This case report is the second to describe pituitary hemorrhage after OPCAB. The patient referred for surgery in a neurosurgery center and underwent transesphenoidal resection of adenoma. The sign and symptom of the occulomotor nerve palsy recovered partially in 6th month of followup.
Case Presentation
A 66-year-old male with diabetes and acute coronary syndrome was referred to our hospital for emergency CABG Preoperative carotid Doppler sonography of both carotid arteries revealed no significant stenosis of both carotid arteries. Physical examination at admission did not reveal any neurological deficit, including visual loss and cranial nerve palsy. The patient scheduled for OPCAB. Anesthesia protocol included a combination, of fentanyl and pancronium bromide supplemented with isoflurane, to permit early extubation. OPCAB was performed through a medial sternotomy incision. Conduits for CABG, including the left internal mammary artery (LIMA) and saphenous vein were harvested in the standard fashion. The right pleural space was opened routinely to allow displacement of the heart to facilitate exposure of the circumflex artery. Revascularization of the left anterior descending artery (LAD) with the LIMA was typically performed first, followed by revascularization of LCX and the right coronary artery (RCA). We used an optimal combination of pharmacological and mechanical methods to reduce the coronary artery movement. Intravenous heparin (1 mg/kg) infused to maintain an activated clotting time (ACT) between 200 and 300 seconds. The distal coronary anastomosis was performed using a running 7-0 monofilament proline suture. Proximal anastomosis to aorta was made on a punch aortotomy after applying a side clamp to the ascending aorta. Visualization of the anastomosis was enhanced with the use of humidified carbon dioxide blower. The systolic arterial pressure was maintained at 80–150 mmHg during the surgery. After finishing of procedures, heparin was neutralized by administration of protamine sulfate. The patient was admitted to the ICU after surgery. The effects of anesthetic drugs were reversed two hours after the surgery in ICU. The patient weaned in 4th hours of surgery. The patient was oriented, but complained of severe headaches and inability in abduction of right eye, right-sided ptosis and diplopia. The patient did have not history of loss of consciousness, or seizure. There was a previous history of hypertension and diabetes mellitus. Neurologic Examination revealed complete ptosis of the right eye and the right pupil was fixed and exhibits no reaction to light. Visual acuity and visual field were normal. The others cranial nerves i.e. four, five and six were functionally normal, and there was no evidence of sensory or motor weakness. The postoperative hemodynamic and respiratory functions were normal. A diagnosis of ischemic or hemorrhagic stroke or subarachnoid hemorrhage with involvement of right third nerve was suspected. Cranial magnetic resonance revealed a large suprasellar mass with bleeding (Figure 1). The finding was typical of pituitary apoplexy. Ischemic or hemorrhagic stroke, intracranial aneurysm, or any space occupied legion was not observed. The patient referred for surgical resection of the pituitary gland 10 days after the OPCAB. The resected tissue contains adenoma necrosis with intra tumoral hemorrhage (Figure 2). The patient exhibited partial recovery with remaining mild right eye ptosis and impaired light reflex and eye movement after the resection. Two year follow-up revealed no recurrence of the pituitary adenoma or establishment of new neurologic sign or symptom.
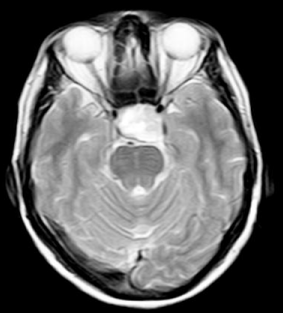
Figure 1: Magnetic resonance images demonstrated the suprasellar
extension of macro adenoma with bleeding (arrows).

Figure 2: Pathological exam demonstrated the macro adenoma necrosis with
bleeding.
Discussion
No more case of pituitary adenoma bleeding after OPCAB cardiac surgery has been reported so far and all remaining 11 cases of apoplexy were reported with on pump CABG [5]. Our case is a rare case report of pituitary adenoma apoplexy that occurred after OPCAB. The frequency of apoplexy after CPB is related to its effect on body organ system. CPB with its side effect on coagulation system may be associated with more neurologic complication than the operation which performed by OPCAB. Pituitary adenomas have an incidence of %10 between intracranial neoplasm with an overall annual incidence of 16 per million per year [6]. The prevalence of occult adenomas is unknown, but symptomatic adenoma has an incidence up to 9 per 10,000. Adenoma may slowly enlarge over years and can lead to morbidity by compressing effect on neighboring structures, such as cranial nerve or pituitary hormone over secretion. Patients may have headaches, visual defects, and cranial nerve palsy from the compressive effects on Para-cellular structures [7]. Much of these adenomas are silent and may be present itself due to trauma, surgery or spontaneously and became hemorrhagic. However, pituitary adenoma apoplexy is a benign syndrome. In other hand an extension of bleeding may be associated with life-treating such as coma. Spontaneously adenoma hemorrhage is a rare phenomenon, but the wide variety of medical interventions with anticoagulation therapy may be associated with this syndrome [8]. CPB associated with two major risk factors for adenoma apoplexy i.e. anticoagulation with heparin and fluctuation of blood pressure. Non-pulsatile high and low blood pressure CPB may associate with capillary bleeding due to adenoma or ischemia consequently. Adenoma ischemia further may complicated by hyper coagulation of CPB. Most reported cases of adenoma apoplexy occur in on-pump surgery, but occurrence of this syndrome in OPCAB is reported in one cases [9]. Off-pump CABG needs to maintain ACT in a lower range than CPB, so lower dose of heparin can be used. In a study, the patients with known pituitary adenoma underwent CABGs. Three of these patients affected by pituitary hemorrhage after on-pump CABG, but one of those who underwent one-vessel OPCAB did not exhibit apoplexy after the surgery. They recommended OPCAB for patients with known pituitary adenoma who require CABG. In our case, the initial ACT was 250s, which was a standard ACT (200–300) for OPCAB, but the excessive fluctuation of blood pressure during heart positioning for obtuse marginal grafting may cause ischemia and consequently bleeding in the pituitary adenoma in this special case.
Conclusion
We suggest that pituitary apoplexy should be included in the differential diagnosis of the patient’s presenting with isolated third cranial nerve palsy and that prompt neurosurgical decompression should be considered in order to preserve third cranial nerve function in these patients.
References
- Savage EB, Gugino L, Starr PA, Black PM, Cohn LH, Aranki SF. Pituitary apoplexy following cardiopulmonary bypass: considerations for a staged cardiac and neurosurgical procedure. Eur J Cardiothorac Surg. 1994; 8: 333- 336.
- Chen Z, Murray AW, Quinlan JJ. Pituitary apoplexy as unilateral third cranial nerve palsy after coronary artery bypass surgery. Anesth Analg. 2004; 98: 46-48.
- Liberale G, Bruninx G, Vanderkelen B, Dubois E, Vandueren E, Verhelst G. Pituitary apoplexy after aortic abdominal aneurysm surgery: a case report. Acta Chir Belg. 2006; 106: 77-80.
- Yousuf-ul Islam M , Ahmed MU , Shahzeb Khan M , Imran Bawany F , Asadullah Khan A, Hussham Arshad M. On Pump Coronary Artery Bypass Graft Surgery Versus Off Pump Coronary Artery Bypass Graft Surgery: A Review. Global Journal of Health Science. 2014; 6: 186-193.
- Levy E, Korach A Merin G, Feinsod M, Glenville B. Pituitary apoplexy and CABG: should we change our strategy? Ann Thorac Surg. 2007; 84: 1388- 1390.
- Cardoso ER, Peterson EW. Pituitary apoplexy: a review. Neurosurgery. 1984; 14: 363-373.
- Francois J, Neetens A. Oculomotor paralyses and tumors of the pituitary gland. Confin Neurol. 1968; 30: 239-252.
- Kim JP, Park BJ, Kim SB, Lim YJ. Pituitary apoplexy due to pituitary adenoma infarction. J Korean Neurosurg Soc. 2008; 43: 246-249.
- Tomohiro Mizuno. Pituitary apoplexy with third cranial nerve palsy after off-pump coronary artery bypass grafting. Interactive CardioVascular and Thoracic Surgery. 2011; 13: 240-242.