
Research Article
Austin Emerg Med. 2016; 2(8): 1043.
Trauma Stories: The Effect of Eliciting a Semi Structured Narrative of Events on the Mood of Trauma Patients
Sodhi S¹*, Reeves K2,3, Charles S4, Goldberg A2,4 and Jones N3
¹Cooper University Hospital, Cooper One Plaza, Camden, NJ, 08103, USA
²Temple University School of Medicine, 3500 N Broad St, Philadelphia, PA 19140, USA
³Center for Bioethics, Urban Health and Policy, Temple University School of Medicine, 3500 N Broad St, Philadelphia, PA 19140, USA
4Temple University Hospital, 3401 N Broad Street, Philadelphia, PA, 19130, USA
*Corresponding author: Sarab Sodhi, Kelemen 152, Cooper University Hospital, Cooper One Plaza, Camden, NJ, 08103, USA
Received: August 12, 2016; Accepted: September 22, 2016; Published: September 23, 2016
Abstract
Objective: To determine the influence of telling one’s trauma story on a victim of violent trauma‘s mood.
Background: Interpersonal violent trauma is an unfortunate reality in modern America. Numerous approaches aimed at reducing the rates of violence are underway, with many focusing on the role of psychological and emotional interventions on victims’ health and recidivism. The connection between psychological and physical health is well established, with an individual’s positive mood correlated to his or her better health outcomes. This study submits new data to this scholarship by addressing the question of whether trauma victims’ mood can be improved through the act of telling stories about one’s trauma.
Method: This study involved pre- and post- semi-structured interview administration of POMS mood scales.
Level of Evidence: Pilot level IV therapeutic.
Results: Of the 22 participants, none had a worsening of mood, and almost a third (31%) showed a statistically significant overall increase in mood after telling their trauma story. Decreasing levels of felt tension and anxiety and increased levels of vigor and activity were the most significant areas of change.
Conclusion: Talking about trauma, within the limitations of this study, appears to be safe and even beneficial. The benefits appear to be much greater in patients with a more disturbed mood, suggesting a possible target group for the intervention for maximum effectiveness and efficiency.
Keywords: Trauma; Narrative medicine; Mood; Violent trauma
Introduction
Being the victim of a violent trauma has been shown to have a significant negative clinical impact on a patient’s health. For patients with trauma, returning to previous function is often challenging, impacted by mental health disturbances, PTSD, drug and alcohol use [1]. Urban trauma patients were found to develop PTSD symptoms (by the PC-PTSD tool) at a rate of 42% significantly higher than their cohort of urban, low income, non-trauma exposed peers (PTSD symptom rate of 22-32%), a worrisome trend when considering the personal and societal cost of PTSD [2]. Further, 60% of those who tested positive on the PC-PTSD tool agreed with the survey question that they thought it would be helpful for them to talk to someone, indicating that ways to address the mental health aspect of trauma, including addressing mood, could be of great benefit to both the patient and the health care system.
A recent meta-analysis identified 9 clinical studies on the influence of mood on disease processes and found a significant correlation of mood with mortality for a variety of disease states- from asthma to terminal cancer - adjusting for disease severity [3]. Conversely, poor mood, as measured by the HADS (Hospital Anxiety and Depression Scale), has been shown to be highly correlated with increased pain sensation [4] and increased mortality in heart failure patients [5]. This body of research suggests that the impact of mood on clinical outcomes is significant.
Research on how narratives impact mood is beginning to be done. A small study in the mid-1980s found that patient driven written narratives administered upon admission led to 6-month decreased physician follow up, a change the authors define as being a positive impact on qualitative health measures [6]. A study on PTSD patients specifically found that writing about the trauma experience did improve the mood of these PTSD patients [7], however participation in this study required a dedicated visit separate from their follow up care and specialized resources and training for the person running the session.
The question this pilot study looked to answer was if in an urban hospital setting, at the point of visit for follow-up care, talking to a patient about their trauma improved their mood. Our hypothesis was that talking about the trauma would improve mood.4. Methods
Participants were recruited from the waiting room of a trauma clinic at a Level 1 Trauma Center. After having the project and the process explained, interested subjects completed the consent form, which indicated that the study consisted of the completion of 2 moodscales and a short interview. Prior to their physician visit participants completed a POMS mood scale form - a well-validated measurement of mood [8]. Subjects were then interviewed in the patient rooms using a semi-structured interview guide (Appendix I) conducted by a social science methods trained medical student. Subjects were alone during the interview except for 1 occasion where the subject was required to be accompanied by a prison guard. The interview guide included questions about the trauma event itself, the experience of getting to the hospital, memories of the experiences in the emergency department and hospital, about perceptions of care by the medical team, and a set of general questions about perceptions of violence in their community. Immediately after the interview, each participant then completed a second POMS mood scale. All interviews were recorded and anonymized, but remained linked to the mood scales. Temple University’s IRB approved this study.
The POMS Short Form Mood scale was our primary analytical tool for relating narrative to mood. The POMS short form scale is a measurement tool that uses 37 descriptors with options to choose a numerical value that best represents the degree to which that descriptor is consistent with the subject’s mood. Then the collection of responses is used to determine the degree of psychological distress [9]. The POMS Short Form shows good internal consistency, test–retest reliability, and convergent validity with its long form compatriot suggesting that the short form is an equally valid tool that requires less time [10-14].
Results
Demographics
Twenty-six subjects were recruited, 24 men and 2 women, with an average age of 29.1 (range 17-47), and an average length of education of 12 years (ranging from sixth grade to college). The majority of our participants had experience with the criminal justice system, with 73% having a history of arrest and 65% with incarceration. While residences and locations of trauma span the city, our participants and their traumas are concentrated in North Philadelphia (Table 1). 4 subjects’ mood scales could not be properly scored and are thus excluded from this analysis.
Average Age
29.11
Gender
Male
21
Female
1
Geographic Area Lived
North Philly
14
NE Philly
5
West Philly
4
Boxborough
1
Camden
1
Germantown
1
Geographic Location of Trauma
North Philly
23
NE Philly
1
Delaware
1
Kensington
1
Average Years of Education
12
Arrests
73%
Jail
65%
Table 1: Demographics.
Mood scales
The POMS mood scales are scored on 7 subsets: anger-hostility, confusion-bewilderment, depression-dejection, fatigue inertia, tension-anxiety, vigor-activity and total mood disturbance. Upon submission of completed mood scales, the POMS program calculates pre- and post- interview mood disturbance. Reporting at a 95% confidence interval, the average mood was determined to be within normal limits, per the parameters of the scales.
Mood changes with talking about trauma
Thirty-one percent (7/22) of participants surveyed experienced a statistically significant positive change in at least one subset of mood after telling the story of their trauma, the hospital experience, and the aftermath of the trauma, with 2 participants experiencing positive change in both a mood-subset and in total mood (Table 2). No participants had post-interview mood scores indicating/reflecting negative changes in mood.
POMS Subset with Change
# of changes
Total Mood
2*
Anger-Hostility
1
Confusion-Bewilderment
0
Depression-Dejection
1*
Fatigue-Inertia
1*
Tension-Anxiety
2
Vigor Activity
2
Total Changes
9
Total Patients with Changes
7
Subsets annotated with a * had multiple changes in the same subject. One subject had significant changes in both total mood and depression dejection, while another had changes in total mood and fatigue inertia.
Table 2: Significant Changes in Mood by Subset.
Analysis
The 31% of participants who experienced a positive change in mood shares some distinct mood characteristics compared to those participants who demonstrated no mood change. Of note, the preinterview mood scores of those violent trauma patients who would go on to have positive mood changes post-interview were significantly more disturbed initially than those patients with no mood change. A comparison of the pre and post intervention mood scores of the responding cohort, showed a decrease in the negative components of mood and an increase in vigor-activity- the positive mood component (Figure 1). Illustrates the details of the comparison of those who showed a significant change in mood with the “non-responders”.
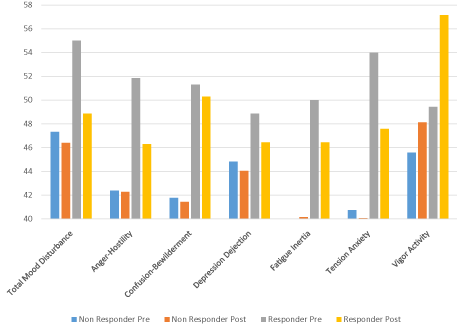
Figure 1: Mood Changes with conversation in Responding and non
responding victims of violent trauma.
Discussion
This study is a proof of concept study with 22 subjects, and while only a third of our participants showed a positive mood change post-interview, the differences between this subset and the other two-thirds of participants is significant, and suggests that if upheld upon expanded study there are valuable clinical implications for a narrative intervention. Specifically, the greater negative mood reported pre-interview by the subjects who had positive mood change suggests that a relatively simple and straightforward means for screening for trauma victims to participate in a targeted intervention involving narrative and storytelling may be possible. If patients reporting for trauma follow-up care score above a certain threshold for negative mood, a 15 to 30 minute interview-based intervention may significantly better their mood. The small power of the study renders it vulnerable to statistical misinterpretation, and the single site looked at also suggests that this data could have only regional validity. The immediate assessment of the intervention also means that long-term assessment of the value of the intervention remains unknown, however a collaborative longitudinal long-term project is in the design phase.
Nevertheless, this study of victims of interpersonal trauma suggests that for a subset of these patients, those with a more disturbed mood, a 10-15 minute conversation with an engaged listener could have a statistically significant change in mood. If this trend holds up on further examination, this could be a clinically effective, cost effective intervention on a high-risk group of patients at risk for significant long term problems of high morbidity and mortality.
Conclusion
This pilot study addresses mood in trauma patients, and offers a simple, inexpensive and minimally labor intensive way of addressing it. Given the extent to which violent trauma patients endure poor clinical outcomes, and the correlations of poor mood with increased mortality, this study suggests a simple and inexpensive intervention that could have a significant impact on the mood of a specific subset of trauma patients. While a larger study would be needed to confirm this trend, beginning to devote more resources to counseling trauma patients, even by non-psychiatric and non-counseling staff, could cause a significant change in the moods of trauma patients and potentially significant health care savings.
Appendix I: Trauma Stories Questionnaire
- Let’s start at the beginning – tell me what happened that brought you to the ER for the visit you’re following up on today?
- Is this the first time you’ve been a victim of a violent crime?
- If yes, was it what you thought it would be like?
- Can you walk me through what happened at the hospital?
- What would you want trauma doctors (med students) to know/learn about what their trauma patients feel in the ER experience?
- Do you think your trauma has changed how family/friends/ loved ones interact with you?
- Has anyone in your house now or growing up been violently injured?
- How has your trauma changed you? Physically/ Emotionally?
- Has your experience changed how you think about violence (in general)?
- Do you think there are differences in how your community sees violence as opposed to people who live in Rittenhouse Square (or other dissimilar part of Philadelphia)?
References
- Michaels AJ, Michaels CE, Smith JS, Moon CH, Peterson C, Long WB. Outcome from Injury: General Health, Work Status, and Satisfaction 12 Months after Trauma. Journal of Trauma-Injury Infection & Critical Care. 2000; 48: 841-850.
- Reese C, Pederson T, Avila S JK, Nagy K, Dennis A, Wiley D, et al. Screening for traumatic stress among survivors of urban trauma. Journal of Acute Care Surgery. 2012; 73: 462-467.
- Frisina PG, Borod JC, Lepore SJ. A Meta-Analysis of the Effects of Written Emotional Disclosure on the Health Outcomes of Clinical Populations. The Journal of Nervous and Mental Disease. 2004; 192: 629-634.
- Tang NK, Salkovskis PM, Hodges A, Wright KJ, Hanna M, Hester J. Effects of mood on pain responses and pain tolerance: an experimental study in chronic back pain patients. Pain. 2008; 138: 392-401.
- Murberg TA, Bru E, Svebak S, Tveteras R, Aarsland T. Depressed Mood and Subjective Health Symptoms as Predictors of Mortality in Patients with Congestive Health Failure: A Two-Years Follow-Up Study. The International Journal of Psychiatry in Medicine. 1999; 29: 311-326.
- Pennebaker JW, Beall SK. Confronting a traumatic event: Toward an understanding of inhibition and disease. Journal of Abnormal Psychology. 1986; 95: 274-281.
- Smyth JM, Hockemeyer JR, Tulloch H. Expressive writing and post-traumatic stress disorder: Effects on trauma symptoms, mood states, and cortisol reactivity. British Journal of Health Psychology. 2008; 13: 85-93.
- Nyenhuis DL, Yamamoto C, Luchetta T, Terrien A, Parmentier A. Adult and geriatric normative data and validation of the profile of mood states. Journal of Clinical Psychology. 1999; 55: 79-86.
- Curran SL, Andrykowski MA, Studts JL. Short Form of the Profile of Mood States (POMS-SF): Psychometric information. Psychological Assessment. Mar 1995; 7: 80-83.
- Shacham S. A Shortened Version of the Profile of Mood States. Journal of Personality Assessment. 1983; 47: 305-306.
- Norman E. Post-traumatic stress disorder in an urban trauma population. Applied Nursing Research. 1991; 4: 171-176.
- Tsay. Predictors of coping efficacy, negative moods and post-traumatic stress syndrome following major trauma. International Journal of Nursing Practice. 2011; 7: 74-83.
- Trauma Informed Care Project. Trauma Informed Care Project [Online]. 2015.
- National Center for Trauma Informed Care. National Association of State Mental Health Program Directors [Online]. 2015.