
Case Presentation
Austin Emerg Med. 2016; 2(9): 1048.
Spinal Hydatid Disease with Neurologic Complications: A Report of Two Cases and Review of Literatures
Meshkini A1, Bazzazi AM2, Mirzaei F1, Javanshir N3 and Naseri Alavi SA1*
¹Department of Neurosurgery, Faculty of Medicine, Tabriz University of Medical Sciences, Tabriz, Iran
²Department of Neurosurgery, Tabriz Aalinasab Hospital, Tabriz, Iran
³Department of Microbiology, Faculty of Medicine, Tabriz University of Medical Sciences, Tabriz, Iran
*Corresponding author: Seyed Ahmad Naseri Alavi, Department of Neurosurgery, Faculty of Medicine, Tabriz University of Medical Sciences, Tabriz, Iran
Received: December 17, 2016; Accepted: December 29, 2016; Published: December 30, 2016
Abstract
We present two patients with spinal hydatid disease who presented with its consequent neurologic complications. The first was a 32-year-old female with sudden urinary retention, paraparesis, low back pain and decreased libido. Magnetic resonance imaging revealed a solitary mixed lobulated mass in the right paravertebral region at T6-T7 level. She underwent surgical decompression and appropriate chemotherapy. Although the symptoms were relieved, she came back after 56 months with recurrence of the disease. The second case was a 12-year-old boy presented with weakness in the lower limb and upper motor deficit. On magnetic resonance images, there was a solitary anteriorly located intramedullary mass at T1-T2. During surgical excision, an intradural extramedullary cystic mass was found. Surgical excision and decompression was performed and oral albendazole was administered. The symptoms resolved and the patient was stable within three years follow-up.
Keywords: Hydatid Cyst; Thoracic Spine; Case Report; Neurologic Complication
Introduction
Hydatid disease (cystic echinococcosis, hydatidosis), which is caused by two larval forms of Echinococcus, E. granulosus and less commonly E. multilocularis [1], is one of the most prevalent helminthic infections all over the world and is endemic in Iran and in its neighbor countries [2,3]. Bone involvement is not a very common finding in hydatid disease (0.5 to 4%), with spinal involvement in about half of these cases [4-6]. However, spinal hydatid disease is always in the list of differential diagnoses in patients with paraparesis, paralysis and pain in the spinal region in endemic areas [7]. Spinal involvement can be morphologically classified into five types: 1) primary intramedullary hydatid cysts; 2) intradural extramedullary hydatid cysts; 3) extradural intraspinal hydatid cysts; 4) vertebral hydatidosis; and 5) paravertebral hydatidosis [8]. Operative procedures are the method of choice, especially in symptomatic patients with the cord compression; usually accompanied with adjuvant chemotherapy [9]. Despite this aggressive approach, the recurrence rate is still discouragingly high [10]. The authors report histopathologically confirmed spinal hydatid disease in two cases presented with neurological complications.
Case Presentation
Case 1
The first case with spinal hydatid disease was a 32 year-old married female who presented with sudden urinary retention to the department of emergency at Imam Reza Teaching Centre, Tabriz, Iran. She had experienced off and on but increasing paraparesis and pain in her lumbar region, as well as a progressive impairment of libido for the last 3 months before development of urinary retention. In physical examination, muscle strength of both lower extremities was decreased; 3/5 and 2/5 at proximal and distal part of the left lower limb, and 2/5 and 1/5 at proximal and distal part of the right lower limb, respectively. Deep tendon reflexes (DTRs) were increased at both sides of the lower limb (4+), while the Babinski’s reflex was normal. Muscle wasting was prominent in the lower extremities. Clonus was detected in the right side. The patient was investigated with routine hematologic investigations including blood counts, and underwent abdominal ultrasonographic examination with inconclusive findings. Plain radiographs of the spine in anteroposterior (AP) and lateral views revealed presence of a mass at the level of thoracic spine. On these plain radiographs, there was a well-defined osteolytic cavitatory area without periosteal reaction or sclerosis. A computerized tomography (CT) scan showed presence of a massive destructive effect on the posterior ring and right pedicle of the T6 vertebrae, along with osteolysis in its transverse process and adjacent ribs (Figure 1). Magnetic resonance (MR) images presented a solitary mixed lobulated space occupying lesion in the right paravertebral region at T6-T7 level, suggesting of hydatid cyst. The patient was administered oral albendazole (400mg TDS) and the mass was excised surgically. A laminectomy was performed through the posterior approach for decompression. A histopathologic confirmation of the diagnosis was obtained. The antihelminthic therapy was continued for 1 year. Follow-up program including regular neurologic assessment plus imaging investigations was carried out every 4 weeks. The patient was lost to follow-up after 12 months postoperation. Within this period, no abnormal finding was documented; however after 56 months from the first operation, the patient was admitted again for recurrence of the disease. The chief complaint for new admission was a progressive paraparesis in the lower limbs developed within 1.5 months. The patient was not able to walk before being seen at our department. The main finding on new CT scan and MRI was presence of a cystic mass in the right neuroforamen at level of T4-T5 with a right paravertebral and epidural component (Figure 2). The lesion was hyposignal on T1W and hypersignal on T2W images. After excision, the histopathological examination confirmed recurrence of the disease.
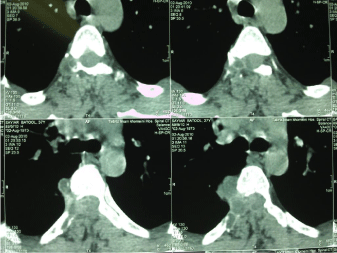
Figure 1: A computerized tomography (CT) scan showed presence of a massive destructive effect on the posterior ring and right pedicle of the T6 vertebrae, along
with osteolysis in its transverse process and adjacent ribs.
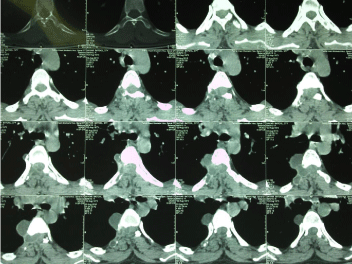
Figure 2: The main finding on new CT scan and MRI was presence of a cystic mass in the right neuroforamen at level of T4-T5 with a right paravertebral and
epidural component.
Case 2
The second case was a 12 year-old boy referred to the department of emergency at Imam Reza Teaching Centre, Tabriz, Iran with weakness in his lower limb as the chief complaint. In physical examination, upper motor deficit and paraparesis in both lower limbs were apparent. Routine hematologic investigations including blood counts were all within normal ranges. Abdominal sonography was along with normal findings. Plain X-ray radiography in the cervicothoracic region showed a deformity in the cervicothoracic junction. On MR images, there was a solitary anteriorly located intramedullary mass at T1-T2. During surgical excision, however, an intradural extramedullary cystic mass was found anterior to the spinal cord with accompanying arachnoiditis. A laminectomy was performed through the posterior approach for decompression. Histopathological examination confirmed the diagnosis of hydatid cyst. The patient received oral albendazole (400mg TDS for one year) and regular follow-up was planned including neurologic assessment plus imaging investigations was carried out every 4 weeks. After 3 years, neurological problems resolved completely.
Discussion
We report here two cases with spinal hydatid disease, one an adult woman and the other a young boy. Although hydatid disease of the spine has been claimed to be a rare entity [11-15], it is not an uncommon cause of spinal cord compression in endemic countries [16], such as Iran. For the female case, a sudden urinary retention, progressing paraparesis and weakness in the lower limb and pain in the lumbar region were the main complaints. For the boy with spinal hydatid disease, upper motor deficit and paraparesis in the lower limbs were the presenting complaints. In a case-series by Altinörs et al. [17], the clinical presentation of spinal hydatidosis (n=458) was variable, including paraparesis (62%) or paraplegia (26%), back pain or radicular pain (55%), numbness or sensitivity loss (36%) and sphincter disturbance (30%). Lakhdar et al. [18] report 3 patients including 2 children (1 boy, 1 girl) and 1 adult who presented with progressive paraparesis attributed to a histologically proven intradural hydatid cyst. Kahilogullari et al. [19] reported a patient presented with back pain, paraparesis, and weakness. An intradural extramedullary cystic lesion was identified with MR imaging and was shown to be a hydatid cyst by histopathologic examination after surgical removal. Celik et al. [20] reported a 34-year-old male patient with back and low back pain, progressive weakness and numbness in both lower extremities, and spastic paraplegia. MR images revealed a lobulated cystic lesion with extradural intraspinal localization in the thoracic region, consisted with diagnosis of hydatid cyst. Manifestations of spinal hydatid disease are believed to be related to compression of the cysts on other structures [21]. As a result, the disease presents itself with radiculopathy, myelopathy and/or local pain due to development of bony destructive lesions, pathological fracture and resulted cord compression [22]. The site of involvement in vertebral hydatidosis is commonly the thoracic vertebrae [23-25].The thoracic spine was involved in 50% of the cases with spinal hydatid disease in two previous reports [9,26]. Twenty patients with spinal hydatidosis were studied by Herrera et al. The thoracic and lumbar regions were affected equally in 35% of the patients [5]. Location of the disease in our two cases also followed this pattern; i.e. at T6-T7 level for the female patient and at T1-T2 for the boy. The abdominal ultrasound examinations were accompanied with normal findings in our two cases. We performed this examination to rule out visceral hydatid disease; because it is claimed that hydatid disease usually affects the soft tissues first and bones are involved later. This was not true in our cases, in accordance with a previous report on 4 cases with spinal hydatid disease [27]. In the female patient, computerized tomography (CT) scan showed presence of a massive destructive effect on the posterior ring and right pedicle of the T6 vertebrae, along with osteolysis in its transverse process and adjacent ribs. Involvement of contiguous ribs and paravertebral masses are suggestive of hydatid disease in previous report [28]. In both cases in the present study, report of MR imaging was consistent with the final diagnosis after histopathological confirmation. It is well-accepted that MR imaging is superior to CT for detection and diagnosis of hydatid cyst in the spine, and to assess its neurological consequences in the region [29]. These cysts demonstrate characteristic appearance on MR images. While on T1W images viable cysts contain a low intensity fluid surrounded by an iso- to mildly hyperintense wall, on T2W images they appear as a low-intensity rim surrounding the high signal cyst content. So T2W images indicate the viability of cysts, while a decrease in the intensity of the signal of the content and an increase of the signal of the cyst walls indicate a dying cyst [1]. Although MR imaging was accurate in diagnosis of hydatid cysts in our cases, location of cyst in the second case was a little different in MR image and during operation. On MR image, the cyst was reported to be an intramedullary mass, while it was found to be located intradural and extramedullary after excision. The intradural and extramedullary involvement, like our second case, is extremely rare in the literature [30-35]. The exact mechanism for the intradural extramedullary involvement is not yet clear. This may occur through vertebral portal venous anastomosis, through the neural foramen, or through hematic dissemination primarily; or after dural tearing during surgery or during an aggressive invasion of spinal space [1,16,18]. Both patients in our report were operated and posterior laminectomy was performed for decompression.
In addition, antihelminthic chemotherapy (albendazole) was administered for at least 1 year after operation. These approaches improved the symptoms; however, recurrence occurred in the first case after about 5 years. Although albendazole drug therapy appears to be effective for treatment of patients with primary solitary hydatid disease in the spine [36], it is not generally effective without surgical interventions [37]. Even in cases who receive both surgical and systemic interventions, recurrence is still a big problem to that extent that some regard hydatidosis as a malignant condition [38]. Invasive diffuse spread within the bone and canal, as well as spillage of fluid caused by cyst rupture has been proposed as underlying etiologies for high rate of recurrence in these patients [27]. Due to high recurrence rate, strict follow-up is recommended after primary treatment [12].
References
- Kaen A, Lagares A, Perez-Nuez A, Rivas JJ, Ramos A, Lobato RD. Intradural extramedullary spinal hydatidosis: case report. Neurocirugia (Astur). 2009; 20: 282-287.
- Altintas N. Past to present: echinococcosis in Turkey. Acta Trop. 2003; 85: 105-112.
- Shahnazi M, Hejazi H, Salehi M, Andalib AR. Molecular characterization of human and animal Echinococcus granulosus isolates in Isfahan, Iran. Acta Trop. 2011; 117: 47-50.
- Ozdemir HM, Ogün TC, Tasbas B. A lasting solution is hard to achieve in primary hydatid disease of the spine: long-term results and an overview. Spine. 2004; 29: 932-937.
- Herrera A, Martínez AA, Rodríguez J. Spinal hydatidosis. Spine. 2005; 30: 2439-2444.
- Fares Y, Khazim R, El Zaatari MM, Haddad GF, Barnes PR. Spinal hydatid disease and its neurological complications. Scand J Infect Dis. 2003; 35: 394-396.
- Ndondo AP, Fieggen G, Wilmshurst JM. Hydatid disease of the spine in South African children. J Child Neurol. 2003; 18: 343-346.
- Braithwaite PA, Lees RF. Vertebral hydatid disease: radiological assessment. Radiology. 1981; 140: 763-766.
- García-Vicua R, Carvajal I, Ortiz-García A, López-Robledillo JC, Laffón A, Sabando P. Primary solitary Echinococcosis in cervical spine. Postsurgical successful outcome after long-term albendazole treatment. Spine. 2000; 25: 520-523.
- Turtas S, Viale ES, Pau A. Long-term results of surgery for hydatid disease of the spine. Surg Neurol. 1980; 13: 468-470.
- Abbassioun K, Amirjamshidi A. Diagnosis and management of hydatid cyst of the central nervous system: Part 2: Hydatid cysts of the skull, orbit, and spine. Neurosurg Q. 2001; 11: 10–16.
- Turgut AT, Altin L, Topçu S, Kiliçoğlu B, Aliinok T, Kaptanoğlu E, et al. Unusual imaging characteristics of complicated hydatid disease. Eur J Radiol. 2007; 63: 84-93.
- Secer HI, Anik I, Celik E, Daneyemez MK, Gonul E. Spinal hydatid cyst mimicking arachnoid cyst on magnetic resonance imaging. J Spinal Cord Med. 2008; 31: 106-108.
- Basak M, Ozel A, Yildirim O, Erturk M. Relapsing hydatid disease involving the vertebral body and paravertebral soft tissues. Acta Radiol. 2002; 43: 192-193.
- Schnepper GD, Johnson WD. Recurrent spinal hydatidosis in North America. Case report and review of the literature. Neurosurg Focus. 2004; 17: E8.
- Sapkas GS, Machinis TG, Chloros GD, Fountas KN, Themistocleous GS, Vrettakos G. Spinal hydatid disease, a rare but existent pathological entity: case report and review of the literature. South Med J. 2006; 99: 178-183.
- Altinörs N, Bavbek M, Caner HH, Erdogan B. Central nervous system hydatidosis in Turkey: a cooperative study and literature survey analysis of 458 cases. J Neurosurg. 2000; 93: 1-8.
- Lakhdar F, Arkha Y, Rifi L, Derraz S, El Ouahabi A, El Khamlichi A. Spinal intradural extramedullary hydatidosis: report of three cases. Neurosurgery. 2009; 65: 372-376.
- Kahilogullari G, Tuna H, Aydin Z, Colpan E, Egemen N. Primary intradural extramedullary hydatid cyst. Am J Med Sci. 2005; 329: 202-204.
- Celik C, Sasmaz MF, Oktay F, Ucan H, Kaptanoglu E. Paraplegia associated with spinal hydatid cyst: a case report. Spine. 2010; 35: E356-358.
- Bhake A, Agrawal A. Hydatid disease of the spine. J Neurosci Rural Pract. 2010; 1: 61-62.
- Joshi N, Hernandez-Martinez A, Seijas-Vazquez R. Primary sacral hydatid cyst. A case report. Acta Orthop Belg. 2007; 73: 674-677.
- Song X, Liu D, Wen H. Diagnostic pitfalls of spinal echinococcosis. J Spinal Disord Tech. 2007; 20: 180-185.
- Patel D, Shukla D. Back bugged: A case of sacral hydatid cyst. J Neurosci Rural Prac. 2010; 1: 43-45.
- Shukla SK, Sharma V, Singh K, Trivedi A. Primary lumbosacral intradural hydatid cyst in a child. J Neurosci Rural Pract. 2010; 1: 109-111.
- Islekel S, Ersahin Y, Zileli M, Oktar N, Oner K, Ovül I, et al. Spinal hydatid disease. Spinal Cord. 1998; 36: 166-170.
- Prabhakar MM, Acharya AJ, Modi DR, Jadav B. Spinal hydatid disease: a case series. J Spinal Cord Med. 2005; 28: 426-431.
- Claudon M, Bracard S, Plenat F, Regent D, Bernadac P, Picard L. Spinal involvement in alveolar echinococcosis: assessment of two cases. Radiology. 1987; 162: 571-572.
- Pedrosa I, Saíz A, Arrazola J, Ferreirós J, Pedrosa CS. Hydatid disease: radiologic and pathologic features and complications. Radiographics. 2000; 20: 795-817.
- Akhan O, Dinçer A, Saatçi I, Gülekon N, Besim A. Spinal intradural hydatid cyst in a child. Br J Radiol. 1991; 64: 465-466.
- Berk C, Ciftçi E, Erdoğan A. MRI in primary intraspinal extradural hydatid disease: case report. Neuroradiology. 1998; 40: 390-392.
- Islekel S, Zileli M, Ersahin Y. Intradural spinal hydatid cysts. Eur Spine J. 1998; 7: 162-164.
- Lam KS, Faraj A, Mulholland RC, Finch RG. Medical decompression of vertebral hydatidosis. Spine. 1997; 22: 2050-2055.
- Onbas O, Kantarci M, Alper F, Sekmenli N, Okur A. Spinal widespread intradural extramedullary hydatidosis. Neuroradiology. 2004; 46: 310-312.
- Pau A, Simonetti G, Tortori-Donati P, Turtas S, Viale GL. Computed tomography and magnetic resonance imaging in spinal hydatidosis. Surg Neurol. 1987; 27: 365-369.
- Kotil K, Tari R, Savas Y. Medical treatment of primary extradural solitary lumbar hydatid disease. J Clin Neurosci. 2010; 17: 793-795.
- Govender TS, Aslam M, Parbhoo A, Corr P. Hydatid disease of the spine. A long-term follow-up after surgical treatment. Clin Orthop Relat Res. 2000; 378: 143-147.
- El-On J, Ben-Noun L, Galitza Z, Ohana N. Case report: clinical and serological evaluation of echinococcosis of the spine. Trans R Soc Trop Med Hyg. 2003; 97: 567-569.