
Case Report
Austin J Endocrinol Diabetes. 2016; 3(3): 1046.
Severe Growth Failure in a Prepubertal Boy: What is Behind the Scene?
Ljiljana Saranac¹*, Zlatko Djuric¹, Zorica Stojsic², Ana Milenovic¹ and Dragoljub Lazarevic¹
¹Pediatric Clinic, University of Nis, Serbia
²Institute of Pathology, University of Belgrade, Serbia
*Corresponding author: Ljiljana Saranac, Pediatric Clinic, Faculty of Medicine Nis, University of Nis, Nis, Serbia
Received: July 14, 2016; Accepted: August 08, 2016; Published: August 10, 2016
Abstract
Background: When examining a short child, the pediatrician-endocrinologist must be aware of the vast number of causative issues and the complex origin of growth disorders.
Case Report: A prepubertal boy aged 12.75 years was referred for an endocrinological assessment because of severe growth retardation. His height of 119.5 cm was -4.8 SD for his Chronological Age (CA), his Height Age (HA) corresponded to 6.5 years, and his Body Mass (BM) of 21.4 kg was 0.6 kg below his ideal weight-for-height. The boy also presented very poor verbal skills and learning and hearing problems. He did not have any abdominal complaints, pain, nausea or abnormal stools; however, his appetite was poor.
Results: Upper endoscopy revealed diffuse macro nodular changes in the distal duodenum. Because of this very unusual endoscopic picture, various polyposis syndromes and enteropathies were considered. However, the pathohistology of the small bowel biopsies revealed the real nature of the disease: the presence of Giardia lamblia trophozoites in the mucosa. Multihormonal acquired pituitary dysfunction was suspected and confirmed.
Conclusion: We reported an unusual case of severe growth failure accompanied by poor cognitive, verbal and hearing skills caused by longterm giardiasis that probably began during a critical period for growth and development.
Keywords: Giardia; Polyposis; Growth
Introduction
Height is the most prominent human phenotypic characteristic, and short stature produces significant anxiety in children and their families. When examining a short child, the pediatricianendocrinologist must be aware of the vast number of causative issues and the complex origin of growth disorders. In this era of wide genetic use in diagnosis of short stature, we should not forget a clinical picture of old phenotypes, that could mimic different pathological conditions.
Case Report
A prepubertal boy aged 12.75 years was referred for an endocrinological assessment because of severe growth retardation. His height of 119.5 cm was -4.8 SD for his Chronological Age (CA), his Height Age (HA) corresponded to 6.5 years, and his Body Mass (BM) of 21.4 kg was 0.6 kg below his ideal weight-for-height. His BMI was 14.98 kg/m2 (-1.88 SD). The boy’s stature was proportionally short, without any dysmorphic features. In addition to growth failure, the main reason for the referral was an extremely low serum iron level (Table 1). There were no signs of puberty, and the boy’s Bone Age (BA) was estimated at 8.5 years. The boy also presented very poor verbal skills and learning and hearing problems. He did not have any abdominal complaints, pain, nausea or abnormal stools; however, his appetite was poor. His family history was positive for short stature; the boy had an extremely short grandmother and short parents, and his two-year-younger sister was also pathologically short (-4 SD for CA).
Patient’s values
Rang
Haemopoethic and biochemical parameters
RBC T/l
4.6
3.1 – 5.8
WBC G/l
10.7
4.0 – 10.0
Hemoglobin (g/l)
68
110 – 180
Hematocrit
0.24
0.31 – 0.59
PLT G/l
320
130 – 400
Serum Iron (µmol/l)
2.1
8.95 – 21.48
TIBC µmol/l
71.7
44.8 – 71.6
UIBC µmol/l
69.6
26.8 – 53.7
Total proteins (g/l)
77.5
60 – 80 g/l
Triglycerids (mmol/l)
0.5
0.30 – 1.63
Cholesterol (mmol/l)
3.48
1.81 – 5.44
Hormonal status parameters
fT4 (pmol/l)
7.01
7.0 – 16.0
TSH (mIU/l)
1.07
0.4 – 4.60
FSH (U/l)
2.4
1.0 – 7.5
LH (U/l)
2.9
1.0 – 7.5
PRL (mU/l)
111
150 -500
IGF1 (ng/ml)
64
183 – 850
Table 1: Haemopoethic, biochemical and hormonal status parameters.
We focused our investigation on excluding possible endocrine and non-endocrine causes of short stature. The boy’s thyroid hormone status (TSH and fT4 levels at the lower cut-off values) suggested central hypothyroidism or attenuation of the thyroid hormone axis. A very low Insulin Growth Factor 1 (IGF1) level was confirmed, and the boy’s PRL level, which was unusually low for a stressed prepubertal child, indicated poor somatomammotropic function. The patient’s gonadotropin levels corresponded to prepubertal values (Table 1).
Dynamic tests of somatotropic function showed a suboptimal response. The peak value of GH (growth hormone) in insulin hypoglicaemia test was 13.7 mU/ml at 30th minute, and the peak of the clonidine test also showed an insufficient GH response (12.0 mU/ml at 60th minute; Table 2). Cortisol response in insulin hypoglicaemia test was normal.
Time (min)
0
15th
30th
60th
90th
120th
Insuline test
Glicaemia(mmol/l)
5.0
3.18
4.12
2.26
3.77
4.65
STH (mU/l)
0.115
0.390
13.7
5.558
9.566
5.142
Clonidine test
STH (mU/l)
0.294
-
0.747
12.0
8.923
4.742
Table 2: Insulin and clonidine test of Somatotropic (STH) function.
The diagnosis of partial Growth Hormone Deficiency (GHD) was established. The cut off value for diagnosis of GHD is less than 20mU/l (Consensus guidelines of Growth Hormone Research Society for the diagnosis and treatment of GH deficiency) [1]. Contrary to our expectations, no congenital pituitary abnormalities were found; pituitary MRI revealed a completely normal pituitary gland size and structure.
Celiac disease was excluded by normal serum IgA and IgA tissue Transglutaminase antibodies (tTG Abs) according to European Society for Pediatric Gastroenterology, Hepatology and Nutrition criteria [2]. Cystic fibrosis was ruled out by two negative sweat chloride tests performed on two separate days. Stool bacterial culture and ova and parasite tests were negative.
Upper endoscopy revealed diffuse macronodular changes in the distal duodenum (Figure 1). Because of this very unusual endoscopic picture, various polyposis syndromes and enteropathies were considered, as well as benigne lymphonodular hyperplasia (Herman’s syndrome) [3]. However, the pathohistology of the small bowel biopsies revealed the real nature of the disease: the presence of Giardia lamblia trophozoites in the mucosa, chronic mucosal inflammation with eosinophilia and reactive lymphoid follicles (responsible for the macronodularity of the mucosal surface on endoscopy).
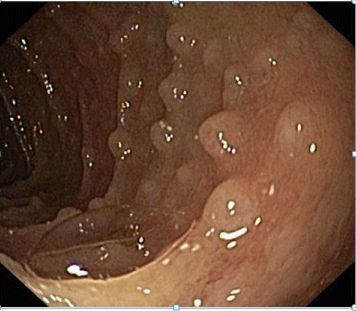
Figure 1: Endoscopic appearance of distal duodenum with diffuse mucosal
macronodularity.
Informed consent to report this case was obtained.
Discussion
Giardiasis is the most common water born parasitic infection of the human intestine with highest prevalence in developing countries. Chronic, neglected giardiasis without gastrointestinal complaints is an unusual cause of growth retardation. Extra-intestinal manifestations, failure to thrive and cognitive deficiencies have been reported as longterm sequelae of Giardia infections [4-7]. In our patient, documented partial GH deficiency was acquired as consequence of chronic small bowel inflammation and malabsorption and central hypothyroidism, all of which suggest pituitary dysfunction. Poor cognitive and verbal skills and partial hearing loss could also be attributed to giardiasis in such circumstances. Deficiencies of micronutrients (e.g., iodine, iron and zinc) that are essential for thyroid hormone synthesis play important roles in neuronal development and metabolic activity, neuronal arborization, myelinization and the emergence of brain networks [8-10]. Malabsorption and consequent malnutrition caused by giardiasis have been shown to affect anthropometric measures [9,10]. The clue of diagnosis was the peculiar appearance of distal duodenum mucosa and pathohistological investigation.
Although Giardia is a non-invasive parasite, post-giardiasis chronic inflammatory syndrome is likely to include immunologic components. Giardia infection tends to be self-limiting in individuals with competent immune systems. In contrast, immunodeficient patients are prone to invasive and systemic forms of the disease [11].
Herein we present an unusual case of severe growth failure overwhelming body mass deficiency and mimicking complex endocrine disorder. The case is very intriguing and instructive and emphasizes specificity of neglected Giardiasis with consequences on growth and development, without abdominal complaints. Peculiar endoscopic picture is shown and pituitary dysfunction is documented.
Conclusion
We reported an unusual case of severe growth failure accompanied by poor cognitive, verbal and hearing skills caused by long-term giardiasis that probably began during infancy, a critical period for growth and development. Multihormonal acquired pituitary dysfunction was suspected and confirmed.
Acknowledgment
Supported by a grant from the Ministry of Science of Republic of Serbia No 31060.
References
- GH Research Society. Consensus guidelines for the diagnosis and treatment of growth hormone (GH) deficiency in childhood and adolescence: Summary Statement of the GH Research Society. GH Research Society. J Clin Endocrinol Metab. 2000; 85: 3990-3993.
- Hysby S, Koletzko S, Karponay-Szabo IR, Mearin ML, Phillips A, Shamir R, et al. European society for pediatric gastrenterology, hepatology and nutrition guidelines for the diagnosis of coeliac disease. J Pediatr Gastroenterol Nutr. 2012; 54: 136-160.
- Albuquerque A. Nodular lymphoid hyperplasia in the gastrointestinal tract of adult patients. World J Gastroinest Endosc 2014; 6: 534-540.
- Halliez M, Buret AG. Extra-intestinal and long term consequences of Giardia duodenalis infections. World J Gastroenterol. 2003; 19: 8974-8985.
- Solaymani Mohammadi S, Singer SM. Giardia duodenalis: The double edged sword of immune responses in Giardiasis. Exp Parasitol. 2010; 126: 292-297.
- Tsourdi E, Heidrich F, Winzer M, Rollig C, Kirsch C, Meinel J et al. An exotic cause of exudative enteropathy. Am J Case Rep. 2014; 15: 226-229.
- Gardner TB, Hill DR. Treatment of giardiasis. Clinical Microbiology Reviews. 2001; 14: 114-128.
- Saranac L, Zivanovic S, Bjelakovic B, Stamenovic H, Novak M, Kamenov B. Why is the thyroid so prone to autoimmune disease? Horm Res Pediatr. 2011; 75: 157-165.
- Farthing M, Mata L, Urutia J, Kronmal R. Natural history of Giardia infection of infants and children in rural Guatemala and its impact of physical growth. Am J Clin Nutr. 1986; 43: 395-405.
- Berkman D, Lescano A, Gilman R, Lopez S, Black M. Effects of stunting, diarrhoeal disease, and parasitic infection during infancy on cognition in late childhood: a follow-up study. Lancet. 2002; 359: 564-571
- LoGalbo P, Sampson H, Buckley R. Symptomatic giardiasis in three patients with X-linked agammaglobulinaemia. J Pediatr. 1982; 101: 78-80.