
Research Article
Austin ENT Open Access. 2018; 2(1): 1004.
Secrets in Cricotracheal Resection for Benign Laryngotracheal Stenosis
Mettias ADB¹*, Mosleh M² and Elbestar MF²
¹ENT Lecturer, Fayoum University, Fayoum, Egypt
²ENT Professor, Cairo University, Egypt
*Corresponding author: Bassem A D Mettias, ENT Lecturer, Fayoum University, Fayoum, Egypt, 8 Stanborough Green, Welwyn Garden City, UK
Received: December 19, 2017; Accepted: January 02, 2018; Published: January 09, 2018
Abstract
Background: Benign Laryngotracheal stenosis is a challenging airway disease. Laser and reconstructive surgeries are less successful in severe stenosis. Method: A retrospective evaluation of 29 patients with laryngotracheal stenosis who had segmental resection with end-to-end anastomosis. Patients were Cotton’s grade 3-4 and McCaffrey stage III. The approaches were tracheatracheal, cricotracheal, thyrocricotracheal in 14, 10 and 5 respectively. Patients underwent laryngeal release procedures according to length of resection. Results: 22 patients had successful outcome. 5 patients (17.2%) failed. The success rate was higher (90%) in short segment compared to 68% in long segments. 15 patients didn’t have further intervention while 6 patients did; one had repeat resection and the rest dilatation. 10.3% had postoperative vocal cord paralysis. Conclusion: The tips for successful segmental resection in airway surgery should start with patient selection, surgical approach to the stenosis and tension free anastomosis. Segmental resection has very successful outcome in severe laryngotracheal stenosis for short and long term.
Keywords: Subglottic; Trachea; Stenosis; Ruyesection; AnastomosisIntroduction
The causes of adult laryngeal and upper tracheal stenosis vary between traumatic, idiopathic, chronic inflammatory disease, collagen vascular disease, benign and malignant neoplasms [1]. The most common cause is iatrogenic internal injury [2]. Patients typically present with months to years of exertional dyspnea or cough, which has often been misdiagnosed as asthma. Others are diagnosed in intensive care with failure of weaning of endotracheal tube [3]. An endotracheal cuff pressure greater than 30mm Hg exceeds the mucosal capillary perfusion pressure, causing mucosal ischemia, which may lead to ulceration and chondritis of the tracheal cartilages. These circumferential lesions heal with fibrosis, leading to a progressive tracheal stenosis [4].
In 1994, Myer-Cotton System modified the original Cotton System in 1984. He classified the horizontal stenosis into 4 grades; depending on the percentage of narrowing of the lumen [5]. McCaffrey designed another clinical staging depending on the vertical length and the location of the stenotic segment [6]. Monnier et al. designed another staging system with considering the co-morbidities and glottis involvement that can affect the prognosis [7].
Surgical options for laryngotracheal stenosis are closed or open techniques. In closed operation, dilatation, endoscopic laser ablation or laryngotracheal stents can be used. In the open approach, different procedures are used such as cricoid splitting procedures, Laryngotracheaplasty (LTP), vascularized myo-osseus flap, slide tracheoplasty, tracheal transplantation, Cricotracheal Resection (CTR) [8]. The standard technique used in the curative treatment of laryngotracheal stenosis is the segmental resection and anastomoses, by means of tracheotracheal anastomsis through the Küster operation and cricotracheal resection through the Pearson operation. The Rethi operation is reserved for cases of glottic and subglottic stenosis [9]. During the 1980s and 1990s, it became apparent, notably through the work of Grillo, and Laccourreye, that resection of laryngotracheal stenosis with primary anastomotic reconstruction could achieve decannulation rates up to 97% [10,11].
The advantages of CTR are preservation of the normal framework of the larynx and trachea, may improve postoperative voice abilities and laryngeal function, near normal-mucosalized airway without granulation tissue formation, which is seen after the use of cartilage grafting and longer-term stenting and finally avoidance of donor site morbidity [12].
The potential complications of partial cricoid resection include difficulty with deglutition and aspiration, vocal cord paralysis, suture granulomas, anastomotic dehiscence, and re-stenosis [13].
Material and Methods
This study is a retrospective case series of 9 years experience (Level III evidence). It was done at Kasr Al Ainy hospital of the Cairo University between January 2001 and April 2010. 29 patients were recruited; who presented with chronic airway obstruction due to combined Subglottic (SGS) and tracheal stenosis.
Every patient was evaluated by history of presenting symptoms, cause of stenosis and past medical history for fitness of general anesthesia with emphasizing on diabetes mellitus, pulmonary function. Any previous treatment was evaluated regarding the type of surgery, the duration of postoperative free symptoms.
Full head and neck examination and degree of respiratory distress were done. Every patient had flexible laryngoscopy to assess the mobility of the vocal cords and the diameter of airway according to Cotton classification. Every patient had axial CT neck of 2mm cuts with saggital reconstruction. The vertical length of stenosis from imaging and flexible laryngoscopy was calculated according to McCaffrey criteria.
Patients were selected for CTR according to following criteria
• Length of stenosis < 6cm of subglottic and/or upper tracheal wall.
• Severe stenosis (grade III or IV) as classified by Cotton grading.
Exclusion criteria are stenosis extending to less than 5mm below the true vocal cords, associated gottic and/or supraglottic stenosis, long segment stenosis more than 6cm, associated bilateral vocal cords paralysis or bilateral arytenoid fixation, mild stenosis (Cotton I, II) candidate for laser dilatation or other methods, neoplasia and tracheomalacia.
Direct laryngoscopy under general anesthesia for endoscopic calculation of stenosis according to Cotton was done for all patients either during initial preoperative tracheostomy or before the definitive surgery. 4mm Hopkin rod 0° bronchoscope was used with Photo-documentation (Figure 1).
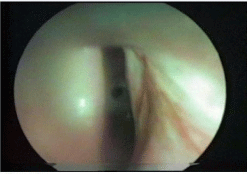
Figure 1: Laryngotracheal stensis below the glottic area.
Operative Tips
The patient was laid in a supine position with head hyperextended. Elliptical skin incision around tracheostomy stoma was done, extending laterally to posterior border of sternomastoid. Subplatysmal flap was elevated superiorly above the hyoid bone and inferiorly to manubrium sterni. Deep investing fascia was dissected and strap muscles were separated without cutting. In revision surgery, the dissection was much difficult due to excessive fibrosis. The thyroid isthmus was divided with transfixation of the lobes.
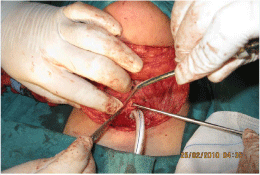
Figure 2: Subperichondrial dissection.
Then dissection around the trachea should be in a subperichondrial plane with no attempts toward identification of recurrent laryngeal nerves (Figure 2). After completion of the anterior dissection, the stenotic segment should be opened longitudinal to assess its extent. Dissection was completed posteriorly by strict adherence to the posterior tracheal wall.
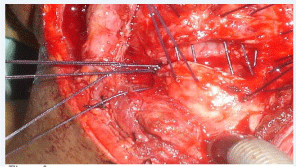
Figure 3: Interrupted inverted sutures.
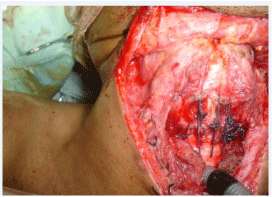
Figure 4: Re-inforcement sutures.
Subperichondrial dissection of the cricoid cartilage was carried out. The stenosis was excised according to the extent of cricoid involvement with blade 15 as follows:
• Rim of anterior arch and posterior lamina were excised if only inferior edge of cricoid cartilage is involved (10 cases, 34.8%).
• Whole anterior arch and rim of posterior lamina (3 cases, 10.3%) if stenosis affected the whole anterior arch.
• Half of posterior lamina below the upper end of cricoid by 5mm in long stenotic segment (2 cases, 6.9%).
After the resection, blunt cervicomediastinal dissection on anterior surface of trachea was carried by finger down to the level of the carina. The lateral dissection was avoided to prevent injury to the vessels at the root of neck and devascularization of trachea. The proximal and distal segments were dissected posteriorly from the esophagus to hold the sutures.
Laryngeal release procedures were performed according to the length of stenotic segment to obtain a tension free anastomosis. In short segment stenosis, suprahyoid was done involving division of myelohoid, geniohyoid and genioglossus medially and stylohyoid muscle laterally. In long stenotic segment (more than 3cm), suprahyoid was followed by infrahyoid release to aid drop of larynx. In infrahyoid release, the sternohyoid and omohyoid ± thyrohyoid muscles were divided near their thyroid cartilage attachment.
The anastomosis was performed by advancing the distal to the proximal segment. This was accomplished by either trachea-tracheal or cricotracheal or thyrocricotracheal. In the first 2 cases, absorbable Vicryl was used but later changer to polydioxanone (PDS 0-0) suture and needle 40. Anastomosis was performed in submucosal inverted pattern where 3 sutures at least were placed to each half 5mm apart. After placing all sutures, the knots were tied simultaneously by the main surgeon and the assistant for each half starting from a posterior to anterior (Figure 3) [3]. Re-enforcement vicryl 0-0 sutures were then placed between anterior tracheal wall (below previous anastomosis) and cricothyroid membrane (Figure 4). Approximation of thyroid lobes and pretracheal muscles was done with vicryl 0-0 sutures. Patients whose preoperative tracheostomy was done less than 2 rings from resection margin or concomitant stomal stenosis, had their tracheostomy position readdressed.
At the end of procedure, neck flexion position was maintained for 1 week by stay suture between chin, skin of upper chest in midline. All patients were followed up 1, 6 and 12 months after surgery. During follow up, clinical improvement in term of stridor, quality of life, voice was assessed. Photo-endoscopic documentation of the speech, mobility of vocal cords, breathing and recurrence of stenosis were also done. The surgery was considered successful if no recurrence of stenosis that cause airway compromise necessitates revision tracheostomy within 12 months. The quality of life regarding voice, breathing was also important indicator. Mild granulation or anastomotic fibrous ring that doesn’t constrict the lumen is classified as successful surgery however they were reported in the complications related to procedure.
Results
29 patients were treated; 20 males and 9 females. The age of patients ranged from 11 to 48 (with a mean of 25.3). There were 2 operating surgeons responsible for the cases. Prolonged intubation was the main etiological factor in most of the patients (86%; 25 patients). The duration of intubation ranged from 4 to 40 days. Blunt external trauma (10.3%) and finally specific granuloma (laryngoscleroma) was the cause in one patient (3.7%). No patients showed raised blood sugar, however one patient had anemia that was corrected before the operation.
Regarding the mobility of vocal cord preoperatively, two patients (6.9%) had unilaterally impaired mobility as a result of missed sublaxation of arytenoids and vocal cord paralysis from blunt trauma. 27 patients presented already with tracheostomy to overcome airway obstruction. The length of resection varied from 1-5 cm with average of 3cm. 10 patients had short stenotic segment (=< 3cm) while 19 had long stenosis (> 3cm). 3 patients were Cotton grade II, 14 were grade III and 12 were grade IV. The mode of anastamosis varied with the length of affected cricoid cartilage. 14 patients had trachea-tracheal repair, 10 underwent cricotracheal and only 5 patients had thyrocricotracheal. 27 patients (93.1%) had cervicomediastinal dissection. 10 patients (34.5%) had suprahyoid release while 16 patients (55.1%) had both supra and infrahyoid laryngeal release. 2 patients had temporary intratracheal stent which was spontaneously extruded during coughing after surgery. Eight patients had concomitant tracheostomy performed during surgery and was later subjected to decannulation trials, while 21 patients (72.4%) recovered without concomitant tracheostomy and were left intubated in the ICU for 2 days before extubation. The patients were monitored for restonsis from 2 up to 36 months (Table 1).
No
Age
Resection Anastomosis
Cervicomediastinal
Dissection
Suprahyoid
Infrahyoid
Segment/cm
Outcome
Complication
S
1
45
Tracheal
Yes
No
No
2.5
Success
1st Surgeon
2
11
Thyrocricotracheal
Yes
No
No
2
Success
3
18
Cricotracheal
Yes
No
No
2.5
Success
4
20
Tracheal
Yes
Yes
Yes
3
Failure
Permanent Stenosis
5
15
Tracheal
No
No
No
1.2
Success
Hoarseness
6
46
Thyrocricotracheal
Yes
Yes
Yes
4.5
Failure
Permanent Stenosis
7
48
Cricotracheal
Yes
No
No
2
Success
8
20
Tracheal
Yes
Yes
No
1.2
Success
Mild stenosis dilated
9
41
Cricotracheal
Yes
No
No
3
Success
10
30
Cricotracheal
Yes
Yes
No
3.5
Success
Rt Palsy, wound infection
11
15
Tracheal
Yes
No
No
1.5
Success
Mild stenosis dilated
12
19
Tracheal
Yes
No
No
3
Success
Granulation dilated twice
13
24
Tracheal
Yes
Yes
Yes
3.5
Success
Granulation dilated once
14
40
Thyrocricotracheal
Yes
Yes
Yes
3.5
Success
15
12
Tracheal
Yes
Yes
Yes
3
Success
Mild stenosis dilated
16
35
Tracheal
Yes
Yes
Yes
4.5
Success
17
33
Cricotracheal
Yes
Yes
Yes
4.5
Success
18
50
Tracheal
Yes
No
No
3
Success
V.c palsy
2nd Surgeon
19
25
Cricotracheal
Yes
Yes
No
4
Success
20
20
Thyrocricotracheal
Yes
Yes
Yes
5
Failure
Esophargeal injury
21
14
Cricotracheal
Yes
Yes
No
4
Failure
bilateral v.c palsy
22
25
Cricotracheal
Yes
No
No
3
Died
Anastomosis rupture (vicryl)
23
18
Thyrocricotracheal
Yes
Yes
No
4
Died
Anastomosis rupture (vicryl)
24
9
Cricotracheal
Yes
No
No
1
Success
25
8
Tracheal
Yes
No
No
3
Success
26
15
Tracheal
Yes
No
No
2
Failure
tracheostomy 1week later
27
45
Tracheal
Yes
No
No
3
Success
28
30
Cricotracheal
Yes
No
No
3
Success
29
14
Tracheal
No
No
No
2
Success
Table 1: Details of recruited patients.
22 patients (76%) had successful decannulation. 5 patients (17.2%) failed with persistent tracheostomy; 4 due to restenosis and one due to vocal cord paralysis. 2 patients (6.8%) died from rupture of the anastomosis at 5th week when Vicryl was used in the anastomosis. The success rate was higher (90%) in short segment compared to 68% in long resected segments (Table 2). 15 patients didn’t have further intervention while 6 patients required. One had repeat resection after 1 month of 1st surgery. One patient required dilatation once; 3 required 2 sessions and only one patient required 3 dilatation sessions. One patient developed small tracheoesophageal fistula that healed spontaneously after 1 week (Table 3).
Item
Short (3 cm)
Long (>3 cm)
Number of patients
10
19
Decannulation
9 (90%)
13 (68%)
Cervicomediastinal dissection
8
19
Suprahyoid release
1
12
Infrahyoid release
0
8
Table 2: Relation of length of stenosis, release procedure, success of surgery.
Resection-Anastomosis
Number patient
Success
Tracheo-tracheal
14
12 (86%)
Cricotracheal
10
8 (80%)
Thyrocricotracheal
5
2 (40%)
Table 3: Relation of extent of resection-anastomosis and success of surgery.
2 patients (6.8%) had postoperative unilateral vocal cord paralysis. One (3.4%) patient had bilateral paralysis immediately mandating tracheostomy. The patient with preoperative bilateral cord immobility was due to fixation of arytenoid from trauma not paralysis. He was discharged with tracheostomy and later decannulated after recovery of vocal cords from trauma (after 6 months). There was one patient with postoperative wound infection with delayed removal of the drain until infection subsided.
Discussion
The fractured cricoid or tracheal cartilage rings have lost aggrecan and collagen I in regions of cartilage ring attenuation or fracture, or both. Only collagen II was preserved in areas of gross cartilage loss [14].
The cricotracheal resection are indicated in severe SGS (grade III or IV) without associated glottic pathology and a margin of at least 4mm of normal airway beneath the vocal folds and above the stenosis. If resection is performed up to the level of the true vocal folds, significant glottic edema should be expected and appropriate airway management should be considered postoperatively (with tracheotomy tube or t-tube). CTR can be used for patients who have persisting stenosis after previous failed attempts for airway reconstruction (LTRs) [12]. Syal et al showed similar report that thyrotracheal anastomosis had significant postoperative morbidity and decreased success rate when compared with cricotracheal anastomosis [15]. From this study, the success has dropped significantly when stenosis was involving higher level in the airway between 86%, 80% and 40% for tracheal, cricotracheal and thyrocricotracheal respectively. The only bias would be the unequal number of recruited patients at each level of stenosis. The length of stenotic segment had negative impact on the success of surgery, being 90% in short segment of less than 3cm compared to 69% in long segment of stenosis.
The recurrent laryngeal nerves enter the larynx just medial to the inferior cornua of the thyroid cartilage [16]. The dissection in sub-perichondrial plane allows safely excision of all fibrosis. In this study, the fibrosis around cricoids and trachea is a usual finding due to either previous attempts of reconstruction or urgent tracheostomy. By following this virgin plane of dissection without any attempt to identify the never, the chance of injury is small (10.3% in current series).
The resection of the anterior portion of cricoid cartilage is performed from the midline of the thyroid cartilage anteriorly, extending posteriorly along the lower border of the cricoid cartilage, leaving an intact posterior cricoid plate [17]. Other authors found it safe to resect below crico-thyoid joint [16]. From current study, we resected up to half posterior lamina (normal height 2-3 cm) but it was crucial to leave a minimum upper 5mm. This would provide a bed for holding the sutures, provide healthy mucosa above anastomosis, and preserve the function of crico-arytenoid joint and the recurrent laryngeal nerves.
The average length of trachea that could be resected was 6.4cm, or up to 58% of total tracheal length when cervical flexion and releasing maneuvers were used [11]. 3.5cm can be safely resected from trachea and reconstructed without the use of releasing maneuvers [10]. The longest stenotic segment in the current study was 5cm.
During the anastomosis, care must be taken when suturing the posterolateral edge of the cricoid ring not to entrap the recurrent laryngeal nerve in the suture line. It is also important to avoid passing the needle through the lumen to avoid suture granuloma.
Most authors recommend interrupted absorbable suture material for the anastomosis; for membranous pars (4-0 polyglactin, Vicryl) and for cartilaginous pars (3-0 polyglactin, Vicryl). The knots of the membranous wall are tied inside, then the knots of the cartilage are tied outside [3-16]. Sutures are placed 3-4 mm apart and 3-4 mm from the edge (membranous wall) or through 1 cartilaginous tracheal ring. The circumference is divided into 4 parts and each quarter is completed separately. The posterior quarters are completed first. The sutures are clipped with a hemostat and each hemostat is sequentially clipped [3]. From 1998, surgeons started to place a running 4-0 Polydioxanone (PDS) to minimize the risk of anatomosis dehiscence [16,17]. In this study, PDS was superior to vicryl as 2 patients died from dehiscence of the later. The use of stay re-enforcement sutures also support the anastomosis.
Segmental resection showed good results in lot of series. Peña reported 91% success rate of 56 cases of subglottic stenosis [18], Rea’s case review of 65 patients with tracheal stenosis showed 95% success [16]. We achieved 76.9% success rate in this study.
In a study on 70 patients by Monnier, he compared the results of a single versus double stages CTR. Double-stage CTR was used for SGS combined with posterior glottic stenosis or fusion of the vocal cords. The rate of decannulation is 98% in primary CTRs, 100% in salvage CTRs after 12 failed LTRs and one failed CTR and 58% in extended CTRs (i.e. when CTRs must be combined with an additional open airway procedure such as posterior cricoid split and costal cartilage graft with a pedicled flap of membranous trachea). Two tracheal rings must be kept intact between the anastomosis and the tracheostomy stoma [19].
Laryngeal release procedures aimed to provide tension free anastomosis, Dedo and Fishman recommended cutting the thyrohyoid membrane; Montgomery cut the suprahyoid muscles and split the inside of the greater cornu of the hyoid bone. Suprahyoid release is better than infrahyoid because important vessels and nerves are not present in the suprahyoid region in addition less the maneuver causes less difficult in deglutition [20]. In cervicomediastinal dissection; the pretracheal plane is opened sharply and a finger is placed in the pretracheal plane down toward the carina. Blunt anterior mobilization with minimal lateral dissection to avoid airway devascularization is used [3].
Approximation of the tracheal ends is helped by simple cervical flexion through a heavy suture is placed through the chin skin and the presternal skin [18].
In this series, we did cervico-mediastinal dissection initially for almost all patients followed suprahyoid release for extra length. We reserved the infrahyoid release for long segment of stenosis. There was no dysphagia reported in the 29 patients. There was no relation between types of laryngeal release procedure and the incidence of restenosis.
Conclusion
Segmental resection is very effective way in the treatment of laryngotracheal stenosis. There is no restriction on the selection of horizontal stenosis; and up to 6cm vertical length of airway can be safely excised. Laryngeal release procedures are adjuvant during the anastomosis. The risk of laryngeal nerve injury is small. Proper assessment and handy surgical approach is important to achieve better voice quality and minimize the recurrence of stenosis.
References
- Goldenberg David, Esclamado Ramon, Flint Paul Cummings Charles w. Surgical management of upper airway stenosis, 4th edn edited by Cummings Charles W, vol 2, Larynx/Trahea/ Bronchus, edited by Flint, chapter ninety three. Elsevier Mosby, Philadelphia Pennsylvania, USA. 2005.
- Rutter Michael J. Update on the management of tracheal stenosis. Current Opinion in Otolaryngology & Head and Neck Surgery. 2002; 10: 440-443.
- Liberman M, Mathisen DJ. Treatment of Idiopathic Laryngotracheal Stenosis. Semin Thorac Cardiovasc Surg. 2009; 21: 278-283.
- Spittle N, McCluskey A. Tracheal stenosis after intubation. BMJ. 2000; 321: 1001-1002.
- Myer CM, O'Connor DM, Cotton RT. A proposed laryngotracheal stenosis grading system based on endotracheal tube sizes. Ann Otol Rhinol Laryngol. 1994; 103: 319-323.
- McCaffrey TV. Classification of laryngotracheal stenosis. Laryngoscope. 1992; 102: 1335.
- Monnier Ph, Ikonomidis C, Jaquet Y, George M. Proposal of a new classification for optimising outcome assessment following partial cricotracheal resections in severe pediatric subglottic stenosis. International Journal of Pediatric Otorhinolaryngology. 2009; 73: 1217–1221.
- Lorenz Robert R. Adult laryngotracheal stenosis: etiology and surgical management. Current Opinion Otolaryngology Head Neck Surgery. 2003; 11: 467–472.
- Amorós JM, Ramos R, Villalonga R, Morera R, Ferrer G, Díaz P, et al. Tracheal and cricotracheal resection for laryngotracheal stenosis: experience in 54 consecutive cases. European Journal of Cardio-thoracic Surgery. 2006; 29: 35-39.
- Laccourreye O, Naudo P, Brasnu D, Jouffre V, Cauchois R, Laccourreye H, et al. Tracheal resection with end-to-end anastomosis for isolated postintubation cervical trachea stenosis: long-term results. Ann Otol Rhinol Laryngol. 1996; 105: 944-948.
- Grillo HC. Circumferential resection and reconstruction of mediastinal and cervical trachea. Ann Surg. 1965; 162: 374-388.
- Walner DL. Techniques for successful laryngotracheal reconstruction in children with severe subglottic stenosis: operative techniques in otolaryngology-head and neck surgery. 2001; 12: 187-195.
- Ward RF, Triglia JM. Airway Growth After Crico-tracheal Resection in a Rabbit Model and Clinical Application to the Treatment of Subglottic Stenosis in Children: Laryngoscope. 2000; 110: 835-844.
- Mankarious LA, Adams AB, Pires VL. Patterns of Cartilage Structural Protein Loss in Human Tracheal Stenosis: Laryngoscope. 2002; 112: 1025-1030.
- Syal R, Tyagi I, Goyal A. Traumatic laryngotracheal stenosis-An alternative surgical technique International Journal of Pediatric Otorhinolaryngology. 2006; 70: 353-357.
- Rea F, Callegaro D, Loy M, Zuin A, Narne S, Gobbi T, et al. Benign tracheal and laryngotracheal stenosis: surgical treatment and results. European Journal of Cardio-thoracic Surgery. 2002; 22: 352-356.
- D'Andrilli A, Ciccone AM, Venuta F, Ibrahim M, Andreetti C, Massullo D, et al. Long-term results of laryngotracheal resection for benign stenosis. European Journal of Cardio-thoracic Surgery. 2008; 33: 440-443.
- Peña J, Cicero R, Marín J, Ramírez M, Cruz S, Navarro F, et al. Laryngotracheal reconstruction in subglottic stenosis: an ancient problem still present. Otolaryngol Head Neck Surg. 2001; 125: 397-400.
- Monnier Ph. Partial cricotracheal resection for pediatric subglottic stenosis: single-stage or double-stage surgery? International Congress Series. 2003; 1240: 777-781.
- Kato I, Iwatake H, Tsutsumi K, Koizuka I, Suzuki H, Nakamura T, et al. End-to-end anastomosis in chronic tracheal stenosis. Auris, Nasus, Larynx. 2003; 30: 69-73.