
Research Article
J Fam Med. 2015;2(2): 1022.
Association of Vitamin D and Homocysteine Level in Angiographically Proven Coronary Heart Disease Patients
Neeraj Kumar Singh1, Wahid Ali1*, S M Natu1, Rishi Sethi2 and Pratibha Singh2
1Department of Pathology, King George’s Medical University, UP, Lucknow
2Department of Cardiology, King George’s Medical University, UP, Lucknow
*Corresponding author: Wahid Ali, Department of Pathology, King George’s Medical University, UP, Lucknow
Received: January 22, 2015; Accepted: March 24, 2015; Published: March 25, 2015
Abstract
Introduction: Coronary heart disease (CHD) is the result of the accumulation of atheromatous plaques within the walls of the arteries. Many well established risk factors have been associated with CHD however, Vitamin D deficiency has traditionally been linked with poor bone health. Results from several studies indicate that low levels of vitamin D may be linked to a higher risk of ischemic heart disease. Elevated levels of homocysteine emerge as independent risk factor for cardiovascular diseases.
Aims/Objective: To study the association of vessel wall blockade, in CHD subjects, with the level of circulating vitamin D and homocysteine levels and to establish the relationship between vitamin D and homocysteine with degree of vessel wall blockade.
Materials and Methods: The samples (non fasting venous blood) were collected from the Department of Cardiology, King George’s Medical University, Lucknow. Samples were separated on the site within an hour of venipuncture and stored at -20oC. Further the samples were estimated for vitamin D and homocysteine levels in the subjects.
Result/ Conclusion: Homocysteine level was significantly (p=0.0001) higher among the cases compared with the controls. However, the vitamin D level was significantly lower among the cases than controls. Our study results conclude that the measurement of homocysteine and vitamin D levels might prove to be a useful marker in early detection of CHD.
Keywords: Vitamin D; Homocysteine; Angiographically; Heart Disease
Introduction
Coronary heart disease (CHD) is the leading cause of death world-wide. CHD is a major cause of death for both sexes: the World Health Organization estimates that 3.8 million men and 3.4 million women around the world die from CHD each year [1]. According to the World Health Organization (WHO), almost 23.6 million deaths will be attributed to cardiovascular diseases (CVD), mainly stroke and heart diseases by the year 2030. Emerging risk factors, particularly inflammatory markers and markers of atherosclerotic burden, might identify those who are actually at high risk and might benefit from more aggressive risk reduction. More than 100 emerging risk factors have been proposed till date for their potential to improve global risk assessment [2].
The significance of any association between cardiovascular disease and circulating homocysteine concentration is attracting considerable attention these days. The normal activities of the transsulfuration and remethylation pathways maintain intracellular homocysteine levels within a narrow range, and the controlled release of Homocysteine into blood results in blood measurements that provide an accurate index of homocysteine status. In the circulation, homocysteine is rapidly oxidized and very little homocysteine remains in the reduced form.
The majority of homocysteine forms a disulfide bridge with protein, and some reacts either with itself to produce homocysteine or with cysteine to form the mixed disulfide cysteine-homocysteine. The link between high level of serum homocysteine and atherosclerotic diseases has been suspected since 1969 [3]. Wald et al. evaluated 20 prospective studies and concluded that lowering homocysteine concentrations by 3μmol/L decreased the risk of ischemic heart disease by 16% and stroke by 24% [4]. Nutritional factors have also been shown to play a major role in the etiology and management of CHD.
Vitamin D has been shown to have several biological effects on the heart in animal studies. It plays a role in cardiac cell contraction, proliferation, maturation, protein expression, and collagen expression.
The VDR was first identified in cultured cardiac cells by Sampson et al [5], and in rat normal hearts by Walters et al [6]. Baksi et al showed increased contractility in response to increasing concentration of the extracellular calcium bath in atria from rats maintained on a vitamin D–deficient diet [7]. These results suggest that vitamin D might play a role in maintenance of vascular tone and cardiac output.
Historical Background
Coronary Heart Disease has emerged as a leading cause of death among the population of new civilized world especially in the western countries, but in the recent past due to changes in the lifestyle of Indian population there is noted a rise in several risk factors among the population living in major cities causing the rise in fatality due to coronary heart disease.
In our study, we are studying the correlation of homocysteine and Vitamin D levels among a small subgroup of the patients diagnosed as Coronary Heart Disease recently diagnosed in our institution to establish an association between the two factors, whether they have protective effect or are the risk factors, for Coronary Heart Disease.
Homocysteine and its Correlation with Coronary Heart Disease
Homocysteine is an amino acid formed from the metabolism of methionine, an essential amino acid derived from dietary protein. Although Homocysteine was first isolated by Butz and du Vigneaud in 1932 [10] it was not until 1964 that Gibson et al [11] reported that patients with homocystinuria had vascular anomalies and arterial thrombosis.
In 1969, McCully et al [12] has put the theory of arteriosclerosis based on the findings of arterial changes in an infant suffering from homocystinuria due to cystathionine β-synthase (CBS) deficiency (an inborn error involving the trans-sulfuration pathway), Wilcken DE et al in 1976 [13] studied the pathogenesis of coronary artery disease as a possible role for methionine metabolism. Methionine metabolism was investigated in 25 patients having age below 50 years who were angiographically proven as having Coronary Heart Disease and in 22 control patients among them 17 had normal coronary arteries at angiography whereas 5 were healthy volunteers. The result of this study showed a reduced ability to metabolize homocysteine in patients with premature coronary heart disease.
In 1984 by Brattstrom et al [14], established the raised homocysteine level as a possible risk factor for cerebrovascular disease.
Clarke R et al [15] in 1991, studied the Design of clinical trials to test the homocysteine hypothesis of vascular disease, that was a randomized, blinded intervention study with folic acid or placebo treatment of patients with vascular disease to determine whether Homocysteine-lowering therapy reduces cardiovascular risk and improves outcome.
Graham IM et al [16] in 1997 have shown that patients with premature cardiovascular disease show Hyperhomocysteinemia is an independent risk factor for cardiovascular disease. Zhang D, Jiang X, Fang P, et al [17] worked over how Hyperhomocysteinemia promotes inflammatory monocyte generation and accelerates atherosclerosis in transgenic cystathionine beta-synthase-deficient mice in 2009. Merchant et al (2003) [18] studied sera of 46,036 men with age between 40–75 years, showed that B-vitamin intake causes 21% lower rate of peripheral arterial disease for every 400 Ìmol/L increase in intake.
Vitamin D and its Correlation with Coronary Heart Disease
In the 1980s and 1990s several observations on the relation between vitamin D and CHD suggested that vitamin D could explain differences in mortality from ischemic heart disease (IHD). The National Health and Nutritional Examination Surveys (NHANES) conducted between 1988 and 2004 showed that individuals with vitamin D deficiency had a higher risk of reporting incidences of heart failure (HF) and MI than those individuals with higher intake of vitamin D [19].
In 1981, Scragg drew on ecological studies of variation in Cardiovascular disease, by season, latitude and altitude and published a hypothesis that sunlight and vitamin D may protect against cardiovascular disease [20].
Thomas J. Wang et al 2008, studied 1739 Framingham Offspring Study participants (mean age 59 years; 55% women; all white) without prior cardiovascular disease. Vitamin D status was assessed by measuring 25-dihydroxyvitamin D (25-OH D) levels. Conclusion of the study was, Vitamin D deficiency is associated with incident cardiovascular disease [21].
Liu et al 2011 examined 548 heart failure patients and found that after a mean follow-up of 18-month lower baseline 25-hydroxyvitamin D [25(OH)D] plasma concentrations were associated with significantly increased risk of all-cause mortality, even after adjustment for various confounders [22].
A more recent study in 2012 of Zahra Dana Siadat et al [23] measured 25 (OH) D serum levels in 57 patients that were diagnosed with coronary artery disease upon coronary angiography and 62 individuals in the control group who were matched for age and sex with the patients and examined the association between serum 25 (OH) D and coronary artery disease with regard to cardiovascular risk factors. Results of the study concluded were that, low levels of 25 (OH) D are associated with prevalent coronary artery disease independent of cardiovascular risk factors.
Aims and Objective
The aim of the study is to analyze the association of circulating vitamin D and homocysteine levels in angiographically proven CHD patients, with an objective to access the serum 25, OH vitamin D and Homocysteine level in angiographically proven cases of coronary heart disease.
Furthermore to establish the association of serum Homocysteine and vitamin D level with the severity of vessel wall blockade.
Subjects
Our study evaluated participants who had angiographically proven coronary heart disease. This is a case control study with subjects having clinically established CHD and admitted at the Cardiology Department King George’s Medical University.
Our study consisted of 100 angiographically proven subjects with CHD where as subjects having CHD with a previous history of diabetes, active tuberculosis, thyroid disorders, ovarian malignancy and pregnant and lactating females were excluded.
However subjects with no previous history of CHD where kept as control.
Study duration was from August 2013 to August 2014.
CLINICAL HISTORY is taken with the special emphasis on the following points
- Age
- Sex
- Occupation
- History of smoking
- Dietary History
- History of level of physical activity during routine days of life
- Family History
- History of Diabetes
- History of Hypertension
- Psychosocial environment of work place and family
- History of Alcohol intake
PHYSICAL EXAMINATION: all the subjects examined physically
- Height
For measurement of BMI
- Weight
- Blood Pressure
- Pulse rate
PRIMARY EVALUATION
- Electrocardiography
- Treadmill exercise
All angiographically proven subjects showing variable degree of cardiac vessel blockage were categorized as CASES and rest of the subjects as well as some subjects from the healthy population were categorized as CONTROL and both of the groups were evaluated further by biochemical examination and follow up.
Biochemical Parameters of Study
Sera of the study groups, cases as well as control were sampled for further biochemical analysis of-
- Lipid profile
- Serum Homocysteine levels
- Serum Vitamin D levels
Serum Homocysteine was estimated from the kit supplied by Autopure Homocysteine kit from Accurex Biomedical Pvt. Ltd [24- 32].
Serum vitamin D was measured from the kit supplied by Diametra routine 25-OH Vitamin D analysis [33-36].
Statical Analysis
The results are presented in Mean ± SD and percentages.
The unpaired t-test was used to compare the age, lipid levels, homocysteine and vitamin D levels between cases and controls.
The one way analysis of variance was used to compare the lipid levels, homocysteine and vitamin D levels among different vessels type followed by Tukey’s post-hoc comparison tests.
The Pearson correlation coefficient was calculated to find the correlation among the study parameters.
The p-value<0.05 was considered significant. All the analysis was carried out by using SPSS 16.0 version (Chicago, Inc., USA).
Results
The mean age of the case and control subjects was 53.04±8.98 and 55.45±5.90 respectively.
The difference in the mean age of cases and controls was found to be statistically insignificant (p>0.05). More than one third of the cases (41.7%) and 25% of controls were between 50-60 years.
However, 39.3% of cases and 75% of controls were below 50 years of age.
Majority of the cases (85.7%) and controls (90%) were males. However, the difference was statistically insignificant (p>0.05).
The height, weight and BMI were similar (p>0.05) between cases and control Comparison of lipid levels between cases and controls. The TC was almost similar (p>0.05) in both cases (128.04±38.04) and controls (126.19±34.66).
Similarly, TG was also insignificantly (p>0.05) higher among the cases (132.01±53.71) than controls (112.82±48.37).
LDL was significantly (p=0.01) higher among the cases (74.30±23.64) compared with controls (60.01±12.03). There was no significant (p>0.05) difference in HDL, VLDL, TC/HDL and LDL/HDL.
The homocysteine was significantly (p=0.0001) higher among the cases (9.86±5.98) compared with controls (3.33±1.95). However, the vitamin D level was significantly (p=0.008) lower among the cases (50.50±38.79) than controls (75.13±24.52).
The percentage of double vessel (53.6%) was higher than single (33.3%) and triple vessel (13.1%).
TC was insignificantly (p>0.05) higher in triple (134.90±43.63) vessel cases than single (130.63±38.90) and double (124.75±36.62). There was no significant (p>0.05) difference in TG, HDL, LDL, VLDL, TC/HDL and LDL/HDL among the angiographic findings.
+The vitamin D level was significantly (p=0.03) different among the different vessels.
The post hoc comparison test revealed that the vitamin level was significantly (p=0.04) higher among single vessel (47.05±33.33) than triple vessel (41.24±34.34).
There was no significant (p>0.05) difference in the level of Homocysteine among the vessels.
Discussion
India is undergoing a rapid health transition with rising burden of coronary heart disease (CHD) [37].
According to the World Health Report 2002, cardiovascular diseases (CVD) will be the largest cause of death and disability in India by 2020 [38].
Based on data from the Framingham trial nearly 50% of males and 30% of females over the age of 40 will develop coronary artery disease.
In our study the mean age of the cases and controls was 53.04±8.98 and 55.45±5.90 respectively (Figure 1).
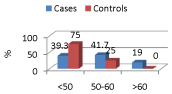
Figure 1: Age distribution of cases and controls.
The most earlier and recent studies maximum cases fall into the age between 50 and 60 years. Though the control group had a comparable age and that the 39.3% of the cases also fall into the category of below 50 years of age this may be due to the lesser activity level in the control group as well.
In our study majority of the cases (85.7%) and controls (90%) were males (Figure 2).
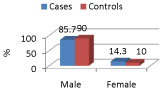
Figure 2: Gender distribution of cases and controls.
Basically the etiology of CHD involves multiple factors contributing to the pathogenesis. Our study has shown that there is more percentage of male to female cases due to CHD which is mainly contributed to the some very unhealthy habits that are more socially acceptable for man than for a woman like smoking, taking excess alcohol, preferring red meat in diet to fruits, etc. Moreover females in India are lesser aware to the risk factors responsible for CHD.
The moderate physical activity was observed among 45.2% of cases and in 35% of controls. However, 31% of cases and 40% of controls had vigorous physical activity. 23.8% of cases and 25% of controls were in mild physical activity (Figure 3).
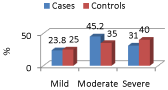
Figure 3: Distribution of cases and controls according to physical activity.
Though our study had no statistical significance still looking at the control group having all the serum as well as BMI and other physical parameters of the study under the normal ranges, most of the control group subjects had vigorous physical activity.
The TC was almost similar (p>0.05) in both cases (128.04±38.04) and controls (126.19±34.66). Similarly, TG was also insignificantly (p>0.05) higher among the cases (132.01±53.71) than controls (112.82±48.37). LDL was significantly (p=0.01) higher among the cases (74.30±23.64) compared with controls (60.01±20.67) (Figure 4).
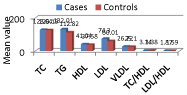
Figure 4: Comparison of Lipid levels between cases and controls.
In middle-aged and elderly white men, a high level of fasting triglycerides is a strong risk factor of IHD independent of other major risk factors, including HDL cholesterol similar to our study in Indian set up.
In our study the Homocysteine level was significantly (p=0.0001) higher among the cases (9.86±5.98) compare with controls (3.33±1.95).
However, the vitamin D level was significantly (p=0.008) lower among the cases (50.50±38.79) than controls (75.13±24.52) (Table 1 & Figure 5).
Cases (n=84)
Controls (n=20)
p-value1
Homocysteine
9.86±5.98
3.33±1.95
0.0001*
Vitamin D
50.50±38.79
75.13±24.52
0.008*
Table 1: Comparison of Homocysteine and Vitamin D levels between cases and controls.
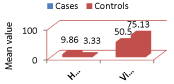
Figure 5: Comparison of Homocysteine and Vitamin D levels between cases
and controls.
Our study findings go in concordance with the most recent studies concluding that raised homocysteine levels and lowered vitamin D levels both are the risk factors involved in the pathogenesis of CHD.
In our study the percentage of double vessel (53.6%) was higher than single (33.3%) and triple vessel (13.1%) (Figure 6).
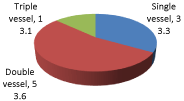
Figure 6: Distribution of patients according to angiographic findings among
the cases.
Current study shows that cases have a high frequency of single vessel disease; the most common anatomical location for the significant was the anterior wall particularly in LAD territory.
Though the levels of TC and TG are high in our cases there is no significant difference (p>0.05) among the angiographic findings (Figure7).
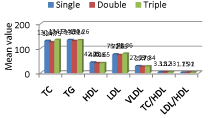
Figure 7: Lipid levels according to angiographic findings.
In our study may be because of lipid lowering agents used in the treatment might have caused some altered levels of lipids in the study group.
The vitamin D level was significantly (p=0.03) different among the different vessels.
The post hoc comparison test revealed that the vitamin level was significantly (p=0.04) higher among single vessel (47.05±33.33) than triple vessel (41.24±34.34).
There was no significant (p>0.05) difference in the level of Homocysteine among the vessels (Table 2 and Figure 8).
Lipid levels
Vessels
p-value1
Single
Double
Triple
Homocysteine
9.90±5.84
9.92±5.89
10.11±6.20
0.17
Vit. D
47.05±33.33a
43.34±31.34
41.24±34.34 a
0.03*
Table 2: Homocysteine and Vitamin D levels according to angiographic findings.
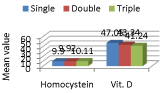
Figure 8: Homocysteine and Vit. D levels according to angiographic findings.
Conclusion
Finally, we conclude that measurement of serum homocysteine and vitamin D might prove to be a useful maker in early detection of CHD.
1ANOVA test, *Significant, ap=0.04 (Post hoc comparison test)
Indian patients with angiographically documented CAD frequently have vitamin D deficiency.
Patients with lower 25(OH) D levels had higher prevalence of double- or triple-vessel CAD and diffuse CAD.
Endothelial dysfunction as assessed by brachial artery FMD (flow mediated dilation) was also more frequently observed in those with low 25(OH) D levels.
This goes in conjunction with our study which concludes the vitamin D level was significantly (p=0.03) different among the different vessels.
References
- Mack, J. and Mensah, G. (2004) Atlas of Heart Disease and Stroke, Geneva: WHO.
- Brotman DJ, Walker E, Lauer MS, O'Brien RG. In search of fewer independent risk factors. Arch Intern Med. 2005; 165: 138-145.
- McCully KS. Vascular pathology of homocysteinemia: implications for the pathogenesis of arteriosclerosis. Am J Pathol. 1969; 56: 111-128.
- Wald DS, Law M, Morris JK. Homocysteine and cardiovascular disease: evidence on causality from a meta-analysis. BMJ. 2002; 325: 1202.
- Walters MR, Wicker DC, Riggle PC. 1, 25-Dihydroxyvitamin D3 receptors identified in the rat heart. J Mol Cell Cardiol. 1986; 18: 67-72.
- BAKSI SN, HUGHES MJ: Deficiency in dietary vitaminD, not calcium, alters noradrenergic responsiveness in rat atria in vitro. J Mol Cell Cardiol. 1986; 18: 653–656.
- Weishaar RE, Simpson RU. The involvement of the endocrine system in regulating cardiovascular function: emphasis on vitamin D3. Endocr Rev. 1989; 10: 351-365.
- Zittermann A, Schleithoff SS, Tenderich G, Berthold HK, Körfer R, Stehle P. Low vitamin D status: a contributing factor in the pathogenesis of congestive heart failure? J Am Coll Cardiol. 2003; 41: 105-112.
- Weishaar RE, Kim SN, Saunders DE, Simpson RU. Involvement of vitamin D3 with cardiovascular function. III. Effects on physical and morphological properties. Am J Physiol. 1990; 258: E134-142.
- Butz LW, du Vigneaud V. The formation of a homologue of cystine by the decompensation of methionine with sulphuric acid. J Biol; Chem 1932; 99:135–142
- GIBSON JB, CARSON NA, NEILL DW. PATHOLOGICAL FINDINGS IN HOMOCYSTINURIA. J Clin Pathol. 1964; 17: 427-437.
- McCully KS. Vascular pathology of homocysteinemia: implications for the pathogenesis of arteriosclerosis. Am J Pathol. 1969; 56: 111-128.
- Wilcken DE, Wilcken B. The pathogenesis of coronary artery disease. A possible role for methionine metabolism. J Clin Invest. 1976; 57: 1079-1082.
- Brattstrom LE, Hardebo JE, Hultberg BL. Moderate homocysteinemia--a possible risk factor for arteriosclerotic cerebrovascular disease. Stroke. 1984; 15: 1012-1016.
- Clarke R, Daly L, Robinson K, Naughten E, Cahalane S, Fowler B, et al. Hyperhomocysteinemia: an independent risk factor for vascular disease. N Engl J Med. 1991; 324: 1149-1155.
- Graham IM, Daly LE, Refsum HM, Robinson K, Brattström LE, Ueland PM, et al. Plasma homocysteine as a risk factor for vascular disease. The European Concerted Action Project. JAMA. 1997; 277: 1775-1781.
- Zhang D, Jiang X, Fang P, Yan Y, Song J, Gupta S, et al. Hyperhomocysteinemia promotes inflammatory monocyte generation and accelerates atherosclerosis in transgenic cystathionine beta-synthase-deficient mice. Circulation. 2009; 120: 1893-1902.
- Merchant AT, Hu FB, Spiegelman D, Willett WC, Rimm EB, Ascherio A. The use of B vitamin supplements and peripheral arterial disease risk in men are inversely related. J Nutr 2003; 133:2863–2867.
- Judd SE & Tangpricha V. Vitamin D deficiency and risk for cardiovascular disease. The American Journal of the Medical Sciences 2009; 338: 40-44.
- Scragg R, Jackson R, Holdaway IM, Lim T, Beaglehole R. Myocardial infarction is inversely associated with plasma 25-hydroxyvitamin D3 levels: a community-based study. Int J Epidemiol. 1990; 19: 559-563.
- Wang TJ, Pencina MJ, Booth SL, Jacques PF, Ingelsson E, Lanier K, et al. Vitamin D deficiency and risk of cardiovascular disease. Circulation. 2008; 117: 503-511.
- Liu LC, Voors AA, van Veldhuisen DJ, van der Veer E, Belonje AM, Szymanski MK, et al. Vitamin D status and outcomes in heart failure patients. Eur J Heart Fail. 2011; 13: 619-625.
- Siadat ZD, Kiani K, Sadeghi M, Shariat AS, Farajzadegan Z, Kheirmand M. Association of vitamin D deficiency and coronary artery disease with cardiovascular risk factors. J Res Med Sci. 2012; 17: 1052-1055.
- Eikelboom JW, Lonn E, Genest J Jr, Hankey G, Yusuf S. Homocyst(e)ine and cardiovascular disease: a critical review of the epidemiologic evidence. Ann Intern Med. 1999; 131: 363-375.
- Scott J, Weir D. Homocysteine and cardiovascular disease. QJM. 1996; 89: 561-563.
- Nygård O, Nordrehaug JE, Refsum H, Ueland PM, Farstad M, Vollset SE. Plasma homocysteine levels and mortality in patients with coronary artery disease. N Engl J Med. 1997; 337: 230-236.
- Seshadri, S., et al., N.Engl. j.Med. 2002; 346: 477-483.
- McLean RR, Jacques PF, Selhub J, Tucker KL, Samelson EJ, Broe KE, et al. Homocysteine as a predictive factor for hip fracture in older persons. N Engl J Med. 2004; 350: 2042-2049.
- Refsum, H., Clinical Laboratory News. May 2002: 2-14.
- Guttormsen AB, Schneede J, Fiskerstrand T, Ueland PM, Refsum HM. Plasma concentrations of homocysteine and other aminothiol compounds are related to food intake in healthy human subjects. J Nutr. 1994; 124: 1934-1941.
- Vilaseca MA, Moyano D, Ferrer I, Artuch R. Total homocysteine in pediatric patients.Clin Chem. 1997; 43: 690-692.
- Faure-Delanef L, Quéré I, Chassé JF, Guerassimenko O, Lesaulnier M, Bellet H, et al. Methylenetetrahydrofolate reductase thermolabile variant and human longevity. Am J Hum Genet. 1997; 60: 999-1001.
- Holick MF1 . Vitamin D status: measurement, interpretation, and clinical application.Ann Epidemiol. 2009; 19: 73-78.
- Morris HA. Vitamin D: a hormone for all seasons--how much is enough? Clin Biochem Rev. 2005; 26: 21-32.
- Zerwekh JE. Blood biomarkers of vitamin D status. Am J Clin Nutr. 2008; 87: 1087S-91S.
- Moyad MA. Vitamin D: a rapid review. Dermatol Nurs. 2009; 21: 25-30, 55.
- Srinath Reddy K, Shah B, Varghese C, Ramadoss A. Responding to the threat of chronic diseases in India.Lancet. 2005; 366: 1744-1749.
- World Health Organization. The World Health Report 2002. Geneva, Switzerland: WHO, 2002.