
Mini Review
J Fam Med. 2015;2(2): 1023.
The Widening Role of Family Medicine in Cardiovascular Risk Control Improvement
Mirjana Rumboldt* and Dragomir Petric
Department of Family Medicine, Split University School of Medicine, Croatia
*Corresponding author: Mirjana Rumboldt, Split University School of Medicine, Department of Family Medicine, Croatia
Received: March 25, 2015; Accepted: March 27, 2015; Published: March 30, 2015
Abstract
Although theoretically very effective and apparently quite straightforward, cardiovascular prevention in practice leaves much to be desired. Several reasons, including psychological, ethical, conceptual, and operative issues are involved resulting in the current situation, where lifestyle changes are mostly ignored, overdiagnosis and overtreatment are expanding, so that drug therapy is often prescribed with no good reason, and performed in an episodic or on/ off pattern. In this essay analyzed are the reasons for these aberrations and suggested are some intuitive solutions and opportunities, best fitted to family medicine.
Keywords: Cardiovascular disease; Prevention; Family medicine
Introduction
The expanding knowledge about etiology, prevention, and management of cardiovascular diseases has pawed the way to radical reduction in the prevalence of these disorders [1]. Indeed, several years ago the global community was seemingly approaching the eradication of atherosclerosis, the leading cause of cardiovascular morbidity and mortality. Unfortunately, the reality did not meet the expectations: the decrease in coronary heart disease in developed countries is nowadays stagnant at best [2], and probably increasing [3], while escalating in developing and transitional countries [4]. This glum picture is often attributed to unavailability or delay in application of modern invasive procedures and new medications, particularly in the case of heart attack or stroke. Although this segment of management should not be neglected (e.g. quick and reliable diagnosis, prompt treatment initiation in family practice, faster transportation, better organization and distribution of adequately staffed and well equipped interventional units), the bulk of the problem lies at the other end of the clinical spectrum – in unsatisfactory prevention. Indeed, according to the EURASPIRE III results the prevalence of obesity among coronary patients in Europe has increased in the last decade from 25% to 38%, and that of diabetes from 17.4% to 28%, while smoking and hypertension are keeping the same level, about 20 and 60%, respectively [5].
Which are the obstacles on the path of effective CHD prophylaxis, particularly primary prevention, i.e. adequate protection of apparently healthy, relatively young people against adverse cardiovascular events? In the following paragraphs analyzed are some of the most prominent issues from the family physician’s standpoint, partly skewed due to our view from Croatia, a transitional, post communist country.
Low perception of deferred risk
Most patients will request urgent medical attention for acute, painful, but minor chest conditions, such as intercostal neuralgia or a similar musculoskeletal disorder. On the other hand, chronic conditions, such as arterial hypertension or dyslipidemia, are much less alarming, often do not hurt at all, and their management, especially primary prevention consisting of adequate nutrition, avoidance of weight gain, exercise and/or smoking cessation is mostly ignored or performed from time to time at best. The reasons for this divide are probably psychological [6]: notwithstanding often good theoretical knowledge of the problem, practical execution leaves much to be desired because human perception of deferred risk is considerably inferior to the appreciation of imminent danger. For this reason people unwillingly apply seatbelts, and put them on more for the fear of being fined than for the statistically tiny, but individually immense risk in the case of a car crash. More than twenty years ago we have shown in a field investigation that declaratively appropriate and cost-effective measures in the management of arterial hypertension are seldom operatively implemented in daily practice [6]. Within the medical profession, as among patients and population at large there is a vast gap between words and deeds.
Ethical issues
From the middle of the past century the human rights movement is rapidly expanding, which is good and quite understandable after incredible crimes against human dignity have been committed, not only during World War II but previously and subsequently alike [7]. Patient autonomy should be respected whenever possible, and the traditional, paternalistic doctor-patient relationship replaced by a kind of negotiating, mutually agreeable partnership, with informed consent as one of its cornerstones. It seems however that modern society is moving towards the other extreme: while striving for human rights, the dues are almost neglected. Although these components of moral judgment should stay in balance – more rights beget more obligations – the ethics of rights is overruling the ethics of responsibilities [7]. It is increasingly overlooked that individual rights are limited by the rights of the neighbors and the community at large, so that current moral judgment is focusing more closely on individual than on collective interest. Personal responsibility for careless and hazardous life-style is left out in the cold, but in the case of misfortune instead of silent suffering the health problem is suddenly and vociferously socialized, requesting costly treatment at the expense of solidarity. These inconsistencies in ethics should be corrected if adequate and coherent attitudes towards health care in the community are contemplated.
Cardinal role of risk factors
A number of large investigations, from the Framingham cohort to the recent INTERHEART case-control study [4,8], have clearly demonstrated that CHD is uncommon without concurrent or antecedent exposure to one or more major risk factors. With the clustering of these factors the probability of CHD complications increases exponentially [4,9] (Figure 1). Unfortunately, these plain and simple notions, explaining over 90% of the global coronary risk [9], often go unknown or ignored. A straightforward evaluation of cumulative individual risk, emanating from these studies, is widely disseminated (charts, calculators etc.) and easily accessible to family practitioners, sometimes even overestimating the risk [10]. Although it is scientifically sound to investigate additional, novel risk factors, improvement in population levels of several “conventional” risk factors remains the main goal of scientific elucidation and practical enforcement [4].
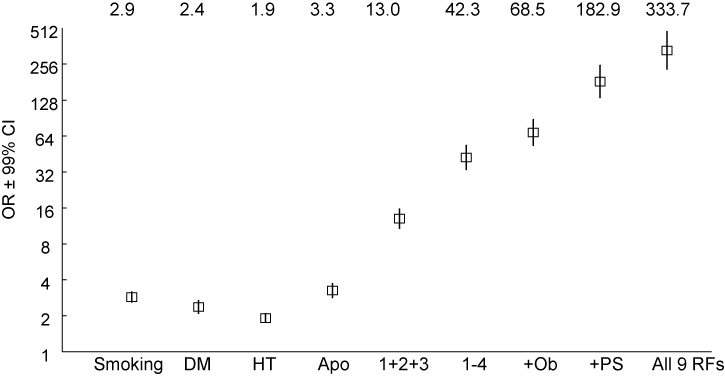
Figure 1: Exponential increase in the probability of acute myocardial
infarction with the aggregation of conventional risk factors (odds ratios and
99% confidence intervals on a logarithmic scale, according to [9]); the classic
6 - smoking, diabetes mellitus (DM), arterial hypertension (HT), dyslipidemia
(Apo for apolipoprotein G: A1 ratio), their combinations (1+2+3; 1-4), obesity
(Ob), psychosocial stress (P/S), and lack of 3 protective (exercise, fruits/
vegetables consumption, moderate alcohol ingestion) factors. According to
[4] and [9].
Desirable risk factor levels are rare
This notion is true for all the evaluated populations, rich and poor, developed, transitional or developing [9-14]. For example, in an analysis of the NHANES-3 data, Vasan et al. [11] have shown that less than 1% of men aged 35-74 years were non smokers, having systolic blood pressure =120 mm Hg, diastolic blood pressure =80 mm Hg, LDL cholesterol =2.6 mmol/l, HDL cholesterol =1.5 mmol/l, and fasting glucose level =6 mmol/l or 2-hour postprandial glucose level =7.8 mmol/l. The same was true for women aged 55-74 years [11]. Stamler et al. [12] have demonstrated years ago that age-adjusted risk of CHD mortality was 77-92% lower among women and men with no major risk factors in relation to the rest of the cohort. Even all-cause mortality rates ranged 40-58% less for those with no major risk factors compared with the rest, and estimated life expectancy gain ranged from 5.8 to 9.5 years [12]. In a Croatian sample of 5,840 persons aged 18-65 years, it was found that 31.1% of the male examinees had BMI =30, that 31.9% had blood pressure >140/90 mm Hg, and that the 75th percentiles of serum cholesterol and triglyceride levels were the high 6.6 and 2.6 mmol/l, respectively [13]!
Early detection of “risky” individuals is paramount
The child is recycling the genetic (inner) and micro social (outer) characteristics of man. Due to clustering of risk factors among the offspring of people suffering from premature atherosclerotic events, such ‘stigmatized’ individuals should be screened, detected and evaluated already in childhood or in school age - the yield is high and the number of persons to be assessed is low; the cost of intervention is almost negligible, and the life-style interventions (e.g. dietary habits, exercise and/or antismoking programs) may have a durable and decisive impact on prognosis. Indeed, marked differences between children of people with premature CHD (offspring aged14.2 ±4.8, parents 39.9±4.2 years) and control pupils (aged 14.2±0.6 years) were demonstrated [14] (Table 1). The probability of adverse prognosis was even higher if additional risk factors coexisted. For example, the prevalence of arterial hypertension among these high-risk children was 46.4%, and that of smoking even higher, 51.3% [14]. The message is straightforward:
Parameter
Control pupils (n=139)
Pupils with parents having AMI <45 years
History only (n= 97)
Additional risk factors (n= 50)
Relative weight (%)*
99.5±11.2
103.8±15.2�
110.1±16.7‡
Plasma cholesterol��� (mmol/l)
4.4±0.6
5.2±1.1�
5.4±1.2‡
Systolic blood pressure
(mm Hg)
114.3±8.5
116.6±15.3�
122.9±17.0‡
Diastolic blod pressure����� (mm Hg)
73.6±7.3
74.3±12.7�
79.7±13.3‡
*Body mass in kg as % of ideal weight for age/gender; �P<0.05; ‡p<0.001 vs. controls.
Table 1: A comparison of control and „risky” pupils in Split, Croatia (according to [14]).
- The incidence of early atherosclerotic complications at young age is low (<5% of CHD patients), an the prevalence of those patients’ offspring among their peers is even lower (<1%);
- Some conventional risk factors (e.g. smoking, obesity) are detectable at a glance, while others (e.g. hyperlipoproteinemia, hypertension) are confidently and cheaply identified in those, selected individuals;
- Simple measures, such as dietary advice or smoking cessation programs, and rare, specific interventions (e.g. statins in familial hypercholesterolemia) substantially improve the cardiovascular prognosis in such persons.
General measures are underestimated and largely ignored
The effectiveness of well structured counseling on life-style modifications is ascertained beyond any reasonable doubt [15]. However, just a minor portion of persons at increased risk quit smoking, decrease body mass and salt intake, adopt a ‘Mediterranean’ diet or engage in adequate exercise for any longer period of time [15]. There are several formal reasons for this hiatus, some of which pertain to still fluid diagnostic criteria (e.g. for the metabolic syndrome) or overlapping guidelines (e.g. misunderstandings about global cardiovascular risk assessment between the Framingham and SCORE tables, although the former is obviously related to morbidity, and the latter to mortality). However, fundamental are socio-economic and cultural barriers [15,16] which may be overcome with early start of gentle and persistent education about healthy life-style, extending from family to school, and involving the whole community. Additional effects may be obtained through legislation and law enforcement (e.g. higher smoking taxation and/or banning).
Drug therapy is hastily prescribed in primary prevention
Potent drugs are too often prescribed on the ground of a single laboratory result or blood pressure reading. Such interventions are frequently superfluous because of false positive findings (e.g. biological variation, laboratory flaw, white coat hypertension) or could be postponed while waiting for the effects of well performed life-style modifications. Moreover, wide implementation of pharmacotherapy, ‘overprescribing’, in primary prevention is charged with several issues:
- Individual prognosis in a low-risk population is only marginally improved by the use of highly effective modern drugs (e.g. statins, ACE inhibitors): several hundreds of low-risk individuals must be treated for years to benefit just a few;
- The expected side-effects, e.g. angioedema with ACE inhibitors, or diabetes mellitus, myopathy and hepatotoxicity with statins, although rare (incidence of these adverse effects is well below 0.1%) become alarming when legions of apparently healthy individuals are exposed to the intervention;
- The probability of adequate intake for such medication is inversely proportional to subjective ailments, motivation, and the number of people exposed. Non-compliance becomes the rule rather than an exception, particularly if the subjects are not informed and motivated well enough;
- This kind of endeavor is potentially extremely expensive, and could absorb up to 25-50% of all the funds affordable to health service [17]. Pharmacoeconomic analyses are invaluable in solving these issues but other variables must be kept in mind as well, including political feasibility and social acceptability [17,18]. For instance, what about proposals for wide prescription of statins to children over 8 years of age if their LDL cholesterol is above 4.9 mmol/l (or just > 4.1 mmol/l in the case of positive family history or two additional risk factors) [19]?
Only well tolerated, highly effective medications should be prescribed in primary prevention. Which kind of evidence is good enough in this respect? Sometimes, because of extremely high cost of large randomized clinical trials, under time constraint, and based upon logically plausible presumptions, instead of “hard” endpoints (e.g. death, stroke, acute myocardial infarction) investigated are “softer” goals (‘surrogate end-points’, e.g. amelioration of a clinical sign or a laboratory result). Although attractive, such studies are often misleading [20]. It is self-evident that results of unconvincing clinical trials should not be implemented in practice. However, even the messages of large, well designed, randomized clinical trials with hard end-points (mostly hospital-based, on very sick in-patients) should not be literally extrapolated to family practice (mostly ambulatory, less sick, out-patients) since the opposite extremes of the same spectrum are at stake. Then, again, the treatment may become worse than the disease itself, as argued earlier.
Pharmacotherapy is underused in secondary CHD prevention
At variance with primary prevention, where pharmacotherapy is often overprescribed, in secondary prevention, i.e. for individuals exposed to substantially higher risk, protective drugs are quantitatively and qualitatively underprescribed. The reasons are again manifold, from differing opinions and attitudes in various countries and even regions, to neglect of convincing scientific evidence, sometimes due to fear of possible adverse effects, which are in this case quite acceptable due to favorable risk/benefit ratio [21]. It is not kept in mind that the level of therapeutic gain differs between the available interventions because of unequal intrinsic efficacy and dissimilar patient characteristics. This concept is best illustrated with the number of patients who need to be treated in order to prevent one event (NNT). Suppose that a small country may afford about 8 million € to give simvastatin, in a daily dose of 20 mg to 25,000 people at elevated CHD risk. If such treatment is offered to very high risk individuals (e.g. 4S study criteria) saved could be some 190 lives per year; if the treatment is offered to medium risk individuals (e.g. HPS study criteria), saved could be about 90 persons, and if the treatment is offered to lower risk individuals (e.g. WOSCOPS or ASCOTLLA criteria) with the same investment avoided could be just some 60 deaths [17]. Many coronary patients may need a complicated drug regimen, of variable therapeutic gain (Table 2), consisting possibly of aspirin (acetysalicylic acid), a β-adrenergic blocker, a statin, an ACE inhibitor, a diuretic, an aldosterone antagonist (e.g. eplerenone), a nitrate, some digoxin, a fish-oil formulation, and other ingredients [22]. Compare for instance the cost-benefit ratios for an ACE inhibitor and a fish-oil product in heart failure (Figure 2) [22]. Hence, individual selection of the most appropriate regimen in terms of efficacy, tolerability and cost is compelling; keeping in mind that overtreatment usually leads not only to noncompliance but to omission of vital interventions in favor of marginal ones!
Intervention
Fatal and nonfatal complications prevented
Mortality decrease
Deaths prevented
NNT/ 1 year
Beta-blockers
42
21
48
Smoking cessation
61
15
67
Statins
37
7
143
Acetylsalicylic acid
19
7
143
ω-3 fatty acids
<6
<3
>330
Table 2: What may be achieved treating 1,000 coronary patients for one year? (after ref. [22]).
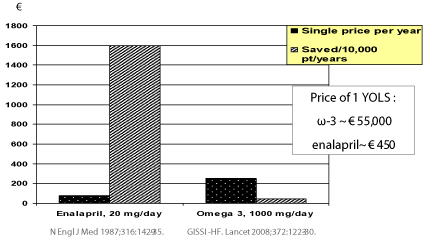
Figure 2: Comparison of two interventions in the management of heart
failure: the efficacy of ω-3 fatty acids is more than 30 times inferior to enalapril
and its cost in terms of years of live saved (YOLS) is over 120 times higher
(according to [22]).
The central role of family medicine
Organizational, financial and political pitfalls have been intentionally skipped in this essay for the sake of brevity. Still, in order to improve the population levels of coronary risk, instead of sophisticated technology, invasive procedures and expensive medications, a lot of education, human understanding, persuasion, and common sense are desperately needed. It can be delivered only in a personalized, family practice. For instance, hypertension, smoking or weight gain, embody many behavioral components that are not easily addressed by formal medical therapy alone. On the other hand the issues of over diagnosis and overtreatment (too much medicine) are increasingly important [22]. It seems that low risk patients are often overtreated at the expense of the high risk minority [23]. Family medicine has a unique opportunity for behavioral modification at the individual and public health level, using peculiar opportunities of empathy, role modeling, and personal skills in communication and education.
It should be remembered that the very first specialization (residency) in family medicine was introduced in Croatia half a century ago [23] and that in this country were the world leaders in the discipline. Instead of treating diseases, family medicine helps sick individuals and enhances the quality of life; instead of depersonalized, industrialized service it offers human understanding, instead of high technology for the benefit of few it delivers efficient care to many, and instead of fee for service it ensures comprehensive care. After identifying the level of coronary risk, family physician must give pertinent, evidence-based information to the patient (or to a small group), answer questions and give some time for data interpretation by the patient, and, after a while to schedule a discussion about his/ her views, problems, and steps to be undertaken. Unidirectional interventions, even well designed and intensive, are short-lived if not enhanced by continuous support [24,25]. Such a task takes a lot of time, dedication and conviction to be effective. The actual family physician must therefore be adequately remunerated for and unloaded of huge capitation (we presume not more than 1,500 persons under care in Croatia) and cumbersome administration, reserving some two hours per day for preventive and educational purposes. Intrinsic to family medicine are certain attitudes that are not readily taught at medical schools: the need to compromise, humility, tolerance and acceptance of different values [26]. The most important teaching method is a good role model (decorum, i.e. the appearance and behavior that manifest inner virtue; e.g. a persuasive physician in the field of preventive cardiology must not be an authoritative, obese smoker).
Preventive programs should be cost-effective as well. However, humanism is about quality and not quantity. It is hardly defined and measured in a quantitative manner. Fine qualitative, followed by quantitative, research has to be done to convince the politicians that investment in family practice is advantageous [24,26]. In this perspective we foresee the solution for the actually stagnant or worsening circumstances in preventive cardiology.
Finally, some additional, relevant problems emerging in everyday practice should be mentioned, which a competent family physician must answer individually, on the spot [27]:
- At which level a risk factor becomes a disease (e.g. millimeters of mercury for blood pressure or millimoles per liter for cholesterol, glucose or uric acid)?
- Which are the pros and cons of diagnostic labeling a freshly discovered, endangered but apparently healthy, symptomless person, assigning her/him a sick role (e.g. hypertension, hyperlipidemia)?
- How to improve compliance? Should the patient be scared, encouraged or something else?
- When it is appropriate to refer a patient for a specialist consultation?
- How to overcome the apparent conflict between general measures (which as a rule are ignored) and drug therapy (which is accepted and even requested, mostly for episodic, on/off and ineffective treatment)?
- When to start deprescribing and/or how to control overprescribing?
References
- Guzman-Castillo M, Ahmed R, Hawkins N, Scholes S, Wilkinson E, Lucy J, et al. The contribution of primary prevention medication and dietary change in coronary mortality reduction in England between 2000 and 2007: a modeling study. BMJ Open 2015; 5: e006070.
- Ford ES, Capewell S. Coronary heart disease mortality among young adults in the U.S. from 1980 through 2002: concealed leveling of mortality rates. J Am Coll Cardiol. 2007; 50: 2128-2132.
- Greenland P, Lloyd-Jones D. Time to end the mixed--and often incorrect--messages about prevention and treatment of atherosclerotic cardiovascular disease. J Am Coll Cardiol. 2007; 50: 2133-2135.
- McGorrian C, Yusuf S, Islam S, Jung H, Rangarajan S, Avezum A, et al. Estimating modifiable coronary heart disease risk in multiple regions of the world: the INTERHEART Modifiable Risk Score. Eur Heart J. 2011; 32: 581-589.
- Kotseva K, Wood D, De Backer G, De Bacquer D, Pyörälä K, Keil U; EUROASPIRE Study Group . Cardiovascular prevention guidelines in daily practice: a comparison of EUROASPIRE I, II, and III surveys in eight European countries. Lancet. 2009; 373: 929-940.
- Rumboldt Z, Jurisić M, Bagatin J, Kuzmanić A, Mirić D, Obad M, et al. [Analysis of operative research in Split: how shall we promote the treatment of arterial hypertension?]. Lijec Vjesn. 1986; 108: 117-122.
- Jonsen AJ. A short history of medical ethics. New York, Oxford: Oxford University Press, 2000: 95-97.
- Chow CK, Islam S, Bautista L, Rumboldt Z, Yusufali A, Xie C, et al. Parental history and myocardial infarction risk across the world: the INTERHEART Study. J Am Coll Cardiol. 2011; 57: 619-627.
- Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet. 2004; 364: 937-952.
- DeFilippis AP, Young R, Carrubba CJ, McEvoy JW, Budoff MJ, Blumenthal RS, et al. An analysis of calibration and discrimination among multiple cardiovascular risk scores in a modern multiethnic cohort. Ann Intern Med. 2015; 162: 266-275.
- Vasan RS, Sullivan LM, Wilson PW, Sempos CT, Sundström J, Kannel WB, et al. Relative importance of borderline and elevated levels of coronary heart disease risk factors. Ann Intern Med. 2005; 142: 393-402.
- Stamler J, Stamler R, Neaton JD, Wentworth D, Daviglus ML, Garside D, et al. Low risk-factor profile and long-term cardiovascular and noncardiovascular mortality and life expectancy: findings for 5 large cohorts of young adult and middle-aged men and women. JAMA. 1999; 282: 2012-2018.
- Turek S, Rudan I, Smolej-Naracic N, Szirovicza L, Cubrilo-Turek M, Žerjavic-Hrabak V, et al. A large cross-sectional study of health attitudes, knowledge, behaviour and risks in the post-war Croatian population (the First Croatian Health Project). Coll Antropol 2001; 25: 77-96.
- Rumboldt M, Rumboldt Z, Pesenti S. Premature parental heart attack is heralding elevated risk in their offspring. Coll Antropol. 2003; 27: 221-228.
- Bergovec M, Reiner Z, Milicić D, Vrazić H. Differences in risk factors for coronary heart disease in patients from continental and Mediterranean regions of Croatia. Wien Klin Wochenschr. 2008; 120: 684-692.
- Serour M, Alqhenaei H, Al-Saqabi S, Mustafa AR, Ben-Nakhi A. Cultural factors and patients' adherence to lifestyle measures. Br J Gen Pract. 2007; 57: 291-295.
- Rumboldt Z, Rumboldt M. Pharmacoeconomics of the statin drugs. Period Biol 2002;104:107-12.
- Pletcher MJ, Lazar L, Bibbins-Domingo K, Moran A, Rodondi N, Coxson P, et al. Comparing impact and cost-effectiveness of primary prevention strategies for lipid-lowering. Ann Intern Med. 2009; 150: 243-254.
- de Ferranti S, Ludwig DS. Storm over statins--the controversy surrounding pharmacologic treatment of children. N Engl J Med. 2008; 359: 1309-1312.
- Gøtzsche P. Deadly medicine and organized crime. How big pharma has corrupted healthcare. London, New York: Radcliffe, 2013.
- Xu W, Goldberg SI, Shubina M, Turchin A. Optimal systolic blood pressure target, time to intensification, and time to follow-up in treatment of hypertension: population based retrospective cohort study. BMJ. 2015; 350: h158.
- Rumboldt Z. [Beware of therapeutic and/or diagnostic enthusiasm]. Lijec Vjesn. 2012; 134: 246-247.
- Rumboldt M, Petric D. Academic cooperation in family medicine: a viewpoint from Split. Acta Med Acad. 2014; 43: 69-75.
- Glavas D, Rumboldt M, Rumboldt Z. Smoking cessation with nicotine replacement therapy among health care workers: randomized double-blind study. Croat Med J. 2003; 44: 219-224.
- Pinjuh Markota N, Rumboldt M, Rumboldt Z. Emphasized warning reduces salt intake: a randomized controlled trial. J Am Soc Hypertens. 2015; 9: 214-220.
- Švab I. The challenged values of family medicine. Eur J Gen Pract 2009 ; 27:1-2.
- Rumboldt M, Kuzmanic M, Petric D, Rumboldt Z. Unsatisfactory cardiovascular risk control – opportunities for family medicine. Zdrav Var 2011; 50: 75-81.