Abstract
Background: While underserved pregnant women smoke for many of the same reasons as smokers in general, there are other factors contributing to higher smoking prevalence. Health interventions require an understanding of the problem if they are to be appropriately targeted and effective.
Aims: To assess barriers, facilitators and motivators of participants from the New England SCRIPT smoking cessation study who were trying to or recently quit smoking during pregnancy.
Methods: Pregnant participants recruited from prenatal clinics were randomized into one of three groups comparing the effectiveness of smoking cessation interventions differing in complexity and cost. Responses from motivational interviewing calls of 227 women were coded and tallied as a percent of respondents. Smokers were queried about perceptions of health risks, pros and cons, and benefits of quitting. Recent quitters were asked why they quit; benefits since quitting; difficulties/urges anticipated; and plans for not smoking.
Results: Health concerns of mothers and infants were cited as a benefit to quitting. Barriers to quitting included stress reduction, weight issues, and social acceptance. Unique facilitators and/or benefits included self-talk, prayer, selfwill and weight gain.
Discussion: Some of these findings mirrored previous research. However, participants who quit smoking during pregnancy did not mention weight concerns as a barrier to maintenance, and reported new and useful facilitators.
Conclusions: Data collected during this MI counseling study supports and expands other qualitative literature of smoking cessation processes among pregnant women, and may help inform the development of new interventions to appropriately support this population.
Keywords: Pregnant women; Smoking; Cessation; Motivation interviewing
Abbreviations
NE: New England; Q & W: Quit and Win; MI: Motivation Interviewing
Introduction
Smoking during pregnancy poses a significant health risk to both women and their unborn infants [1-3]. Moreover, smoking cessation reduces the deleterious effects to the fetus, the infant, and, may benefit a woman’s long-term health [4]. Pregnancy, therefore, provides an ideal opportunity to promote smoking cessation for women and their family, given that many women are motivated to protect the health of their fetus and/or have developed an aversion to smoking [5-8]. Yet despite significant progress in developing effective smoking cessation interventions, not all women are motivated to quit smoking during and after pregnancy [9-12]. In the U.S., the prevalence among pregnant women has been reported to be 10.7% although smoking rates remain disproportionately high among underserved pregnant women [13]. The highest prenatal smoking prevalence has been reported to be among those who are aged 20–24 years, (17.6%), American Indian/Alaskan Native (26.0%), <12 years of education (17.4%), and have Medicaid coverage during pregnancy, [13] which may represent a disadvantaged subgroup of pregnant smokers who are less likely to quit smoking during pregnancy [14].
To develop targeted interventions to achieve sustained smoking cessation during and after pregnancy, a comprehensive understanding of the scope of the problems they face is needed. Although qualitative studies have been conducted exploring potential barriers, many of the studies have been small, have been based on purposive samples, or examined select barriers [15,16]. Recently, Fleming et al. conducted a qualitative systematic review synthesizing findings from 38 studies that examined barriers and facilitators to smoking cessation experienced by women during and after pregnancy [17]. They highlighted the preponderance of barriers over facilitators for disadvantaged pregnant smokers to help assist with development of policy and practice [17]. Qualitative studies have increased our understanding of barriers to quitting faced by underserved pregnant women. However, additional research is needed to further expand our understanding of this complex, challenging and changing issues. To better understand barriers preventing this subgroup of pregnant smokers to quit smoking, we were interested in examining the thoughts and concerns expressed about smoking and cessation as part of information collected during motivational interviewing (MI) counseling during the randomized clinical trial, the New England Smoking Cessation/Reduction in Pregnancy Trial (NE SCRIPT). The objectives of this study were to: 1) identify barriers, facilitators, and motivators of pregnant women who were still smoking during pregnancy and 2) identify barriers, facilitators, and motivators of pregnant women who quit smoking before of during pregnancy based on information obtained during MI counseling sessions.
Methods
The MI counseling sessions were part of the randomized clinical trial, the New England Smoking Cessation/ Reduction in Pregnancy Trial (N.E. SCRIPT) with the primary aim of comparing the effectiveness of three smoking cessation interventions. A total of 8,526 pregnant women attending prenatal clinics were screened for smoking status at their first or second visit from 22 urban prenatal care clinics in Rhode Island, Connecticut, and Massachusetts. Patients were invited by clinic staff to participate even if they had no intention to quit smoking. Of those screened, 1,858 smokers (21.8%) were identified, 1,341 (72.2%) smokers initially agreed to participate, 517 smokers refused and 276 could not be contacted. To be eligible, a pregnant woman had to have had at least one puff of a cigarette within the past 7 days Sixty-three adolescents were also excluded from these analyses as we focused on adults. Furthermore, the adolescents represented a very small group for this study and may have very different views on smoking cessation compared to their adult counterparts. The final group consisted of 1002 pregnant smokers (54%) (Figure 1).
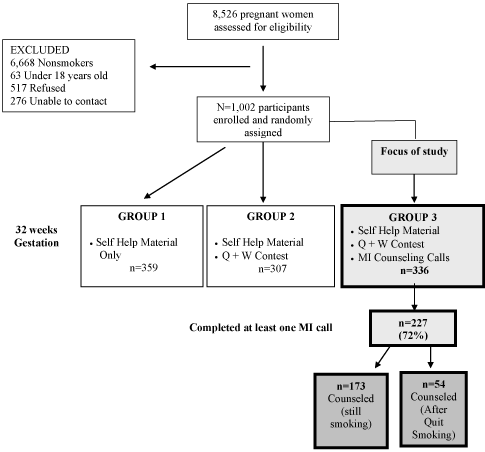
Figure 1: Recruitment and Retention Rates.
All participants completed a written Informed Consent Form prior to randomization to one of three experimental groups. Group 1 received self-help materials (a Quit Kit including A Pregnant Woman’s Guide to Quit Smoking); [18] Group 2 received the Quit Kit and was enrolled in a “Quit and Win” (Q&W) lottery program; [19] and Group 3 received the Quit Kit, the Q&W program, and up to three MI telephone calls. This report focuses on women who were randomly assigned to Group 3 (n=227) and completed at least one motivational interview telephone call. The study protocol was approved by the Memorial Hospital of Rhode Island Institutional Review Board.
MI interviewing
Motivational interviewing is defined as a “directive, patientcentered counseling style for eliciting behavior change by helping clients explore and resolve ambivalence” [20]. The goal of MI techniques is to help patients move through the stages of readiness to change in dealing with unhealthy behavior [21]. MI techniques include; giving advice, decreasing desirability, expressing empathy, reflective listening, and providing feedback and active helping [22]. The objectives of MI calls were to discuss women’s smoking habits, enhance their perception of maternal/fetal risks, determine their readiness to change, encourage participants to use the intervention materials and to provide support for personal decision-making.
MI training procedures
Counselors were trained in MI techniques in a two-day (16 hour) training program by a credentialed MI counseling specialist. Detailed information on MI training, procedures, and quality control has previously been described [23]. During the initial interview, the MI counselor introduced herself to the participant and spent time building rapport before progressing to the assessment of her smoking status as well as by discussing the pros and cons of smoking and readiness to make changes. The MI counselor next offered advice regarding the benefits of quitting and then went on to assist the participant with goal setting tailored to her readiness, and finally arranged a follow-up appointment to discuss smoking at the next phone call.
Six strategies were used starting with asking open-ended questions, listening reflectively, affirming the participant, summarizing to link together materials that had been previously discussed and eliciting self-motivational statements by using probing questions and clarifying statements. Notes taken during the motivational interview calls used a structured form from which the MI counselors prompted participants. For women who were still smoking, they were queried regarding their perception of health risks of smoking, health risks of second hand smoke, pros and cons of smoking, benefits of quitting and concerns about quitting. For women who self-reported to have quit smoking, they were queried as to reasons why the participant quit smoking, benefits or changes noticed since quitting, difficulties or urges anticipated and plans for not smoking after delivery. Counselors used a structured form to document an attempted or completed call, including the extent to which the core MI intervention components were followed. Notes from the first call made while women were in the process of quitting smoking and the first call made after quitting were included in these analyses.
Analysis
The comments noted and recorded by the MI counselor were entered into a database. All responses were coded initially by one investigator (NH) with no apriori coding structure in mind, such that a response from a given participant might have met the criteria for more than one code. Following development of the coding structure, a second investigator (PMR) reviewed it and made recommendations for changes when needed. Finally, all four authors independently reviewed the coding structure and met to discuss and finalize the coding structure as a group whereby decisions were made and finalized regarding collapsing and combining similar topics into a single category. Searches for alternative interpretations were conducted as part of the analysis process before final decisions were made about reporting findings. Totals were counted for all responses that met specified criteria. Each total was divided by the total number of participants that gave any response to the given question. The totals and percentages are presented. Calculations and analyses were performed using Microsoft Excel 2010 and SAS 9.4 (SAS Institute, Inc, Cary, NC).
Results
Of the 336 participants assigned to receive MI calls, 227 women completed at least one MI call prior to her due date including 54 who were no longer smoking and 173 who were still smoking.
Demographic characteristics of those included in our sample vs. those excluded are presented in Table 1, with no significant differences noted between those included and those excluded.
No Calls or Called After Delivery
n=109
Final Sample
n=227
N
%
N
%
Race/Ethnicity
Non-Hispanic White
76
69.7
135
59.5
Non-Hispanic Black
14
12.8
45
19.8
Hispanic
18
14.9
41
18.6
Other
1
0.9
6
2.6
Age Group
18-20
27
24.8
34
15.0
21-25
38
34.9
87
38.3
26-30
22
20.2
55
24.2
31 and over
22
20.2
51
22.5
Highest Grade Completed
< 8th
3
2.8
14
6.2
9-11th
38
34.9
69
30.5
> 12th grade
69
62.4
143
63.3
Smoking Status at Baseline Survey
Quitter
18
16.5
49
21.6
Smoker
91
83.5
178
78.4
Statement that Best Describes Smoking at Baseline
You smoke now about the same as before you became pregnant
11
10.1
22
9.7
You smoke now, but you cut down the number of cigarettes you smoke after you became pregnant
79
72.3
151
66.5
You stopped smoking after you became pregnant.
18
16.5
47
20.7
You stopped smoking before you became pregnant
0
0
2
1.0
You smoke more now than before you became pregnant.
1
1.0
5
2.2
Seriously thinking about quitting smoking completely during this pregnancy
Yes
86
92.5
174
92.1
No
7
7.5
15
7.9
Cigarette Smokers Living in the Same House
No
32
29.4
83
36.7
Yes
77
70.6
143
63.3
Cigarette Smokers Are Family Members and Friends (Not Counting Those in the Same Household)
No
7
6.4
18
7.9
Yes
102
93.6
209
92.1
Support from Family, Friends and Co-Workers if Decided to Quit
A Lot
85
81.1
181
79.7
Some
12
11.2
19
8.4
A Little
4
3.7
12
5.3
None
3
2.8
13
5.7
*Received One or More Call; All calls were before the participant’s due date.
*None of these differences are statistically significantly different.
Table 1: Demographics Characteristics of Women Who Received MI calls* vs Women Who Did Not Receive Any MI Calls**.
Of those who received MI calls, the majority (59.5%) were non- Hispanic White, over one-third (38.3%) were between the ages of 21-25 years, and the majority (63.3%) had high school education. Most participating women (63.3%) reported living in the same house as other smokers and almost all (92.1%) were exposed to cigarette smoke from other smokers outside of the household. Of interest was that 79.7% reported that they would be well supported to quit. For both groups of women, the majority were current smokers at baseline, had cut down on the number of cigarettes smoked after they became pregnant, and lived with a current smoker.
Table 2 presents responses of pregnant women who were still smoking.
Health Risks of Smoking
Health Risks of Second Hand Smoke
Pros of smoking
Cons of smoking
Benefits to Gain from Quitting
Worries about Quitting
Mom
N=65
n (%)
N=51
n (%)
N=54
n (%)
N=49
n (%)
N=45
n (%)
N=56
n (%)
Lung disease or asthma
(not cancer)
27 (42)
General health (bad for health); worse than smoking; just as harmful as smoking
42 (82)
Relaxes/ makes you feel better/ substitute for medication
25 (46)
Smells terrible/ hair and clothes smell/ burns eyes
30 (61)
Healthier /feel better/ low risk for cancer/ low risk for heart disease
26 (58)
No worries
31 (55)
Cancer
31 (48)
Lung disease-asthma, bronchitis, emphysema (excluding cancer)
5 (10)
Reduces stress
20 (37)
Breathing problems/ chest pains/ coughing/ voice changes, asthma
15 (31)
Save money
18 (40)
Weight gain/ appetite increase
14 (25)
General health
19 (26)
Prematurity/ pregnancy problems
1 (2)
Not good/ habit/ mind game [addictive]
14 (26)
Expensive
13 (27)
Improved taste buds/ fresher breath/ clearer skin/ whiter teeth
9 (20)
Mood swings & dealing with stress
7 (13)
Prematurity
7 (9)
None
1 (2)
Provides company/ fights boredom
8 (15)
General health
16 (33)
Better breathing,
no coughing6 (13)
Dealing with triggers/ urges/ cravings
6 (11)
Other heart health
4 (6)
Nothing
7 (13)
Bad breath/ taste
11 (22)
Environmental improvement/ house smells better
5 (11)
Finding a replacement for cigarettes
3 (5)
Pregnancy problems
4 (5)
Reduced hunger/eat less
4 (7)
Stains nails & teeth/ skin wrinkles
11 (22)
Better role model for baby/ improved social relationship.
5 (11)
Taste
2 (4)
Second hand smoke, air quality
8 (16)
Exercise more/ more easily/ more energy
5 (11)
Helps digestion
1 (2)
Feel sick
8 (16)
Will gain more weight /better appetite
1 (2)
Social acceptance
1 (2)
Causes cancer
3 (6)
Addiction
1 (2)
Prematurity/ premature labor
2 (4)
Controls appetite
1 (2)
Depression
1 (2)
Baby
N=38
n (%)
N=5
n (%)
N=8
n (%)
N=12
n (%)
Low birth weight
22 (58)
Later (infant or child) illness
3 (60)
Health risks of unborn baby
7 (88)
Healthier baby/ baby benefits
11 (92)
General child/ illness
12 (32)
Low birth weight
1 (13)
No second hand smoke
2 (17)
Birth defects
5 (13)
Low birth weight
1 (20)
SIDS
1 (13)
Development
2 (5)
General health
1 (20)
SIDS
2 (5)
Table 2: Responsesa of motivational interviewing intervention calls of pregnant women who were still smoking regarding health risks of smoking and secondhand smoke (ETS), pros and cons of smoking, and benefits and worries about quitting.
Health risks of smoking among women who were still smoking
Sixty-five participants responded to questions regarding the health risks of smoking which included both risks to the mother and to the fetus. The most frequently cited health risks included: lung disease (42%), cancer (48%), though other issues including general health, heart health, prematurity and pregnancy problems were also mentioned. Fetus/infant health risks mentioned most frequently were low birth weight (58%) and general child illness (32 %).
Health risks of second hand smoke (or environmental tobacco smoke-ETS)
Risks of ETS exposure were reported by 51 participants who were still smoking. General health (82%) and lung (10%) diseases were mentioned by the majority of participants. Prematurity, pregnancy problems, and later infant or child illness were also mentioned.
Pros (positive aspects) of smoking
In a discussion of pros and cons of smoking among women still smoking, 54 participants reported good things about smoking. Fortysix percent mentioned relaxation (and/or a substitute for medication) and 37% cited stress reduction. Other participants (15%) mentioned that smoking provides company.
Cons (negative aspects) of smoking
Cons of smoking reported by 49 participants who were still smoking included health conditions as well as other more practical aspects of smoking. These included a terrible smell on clothing and hair (61%), breathing problems or chest pains (31%), general health concerns (33%), cancer (6%), and prematurity (4%). The expense of cigarettes was also reported by 27% of respondents. Other practical negative aspects of smoking mentioned included bad breath and stained nails and teeth, physical feelings of sickness (e.g. nausea), lack of appetite and depression.
Benefits of quitting
Benefits of quitting were reported by 45 participants who were still smoking. Better health (lower risk of cancer and heart disease-58%), saving money (40%), better breathing (13%) and personal factors (improved taste, fresher breath, and better skin- 20%) were mentioned. Other benefits included better household environment, being a better role model for the baby, increased energy and exercise, and a better appetite or better weight gain.
Worries about quitting
Fifty-six women still smoking mentioned their concerns about quitting. These included: weight gain (25%), mood swings and stress (13%), dealing with urges (11%,) and finding a replacement for cigarettes (5%).
Table 3 presents responses for women who had quit smoking shortly before or during pregnancy.
Reasons Why Quit
Benefits / changes you noticed since you quit
Difficulties / urges you anticipate
Plans for not smoking after birth
Mom
N=32
n (%)
N=42
n (%)
N=33
n (%)
N=25
n (%)
Health, non-respiratory illness/hospitalization
13 (41)
No more asthma / improved breathing / chest doesn’t hurt
15 (36)
None – too sick to think of urges
13 (39)
Will remain smoke free
13 (52)
Pregnancy / would feel guilty
12 (38)
Save money
9 (21)
Eats to curb urges
5 (15)
Will use study materials/reading /
chew gum5 (20)
Asthma / breathing problems
6 (19)
Hungrier / better appetite / weight gain / reflux improvement
10 (24)
Keeps busy to get rid of urges / stay away from triggers
5 (15)
Will use prayer / self will/ will try, but not sure
3(12)
Nausea
5(16)
No changed noticed as yet
8 (19)
Social gatherings with others smoking / friends who smoke / 2nd hand smoke at work
2 (6)
Don’t want to think too far into the future/no plan
3 (12)
Smell / taste
5 (16)
Healthier skin / feel healthier
7 (17)
Having a bad moment / stressful argument / tragedy, mood swings, grouchiness
3 (9)
Will keep busy to remain smoke free
1 (4)
Save Money
2 (6)
Better taste / food tastes better / better sense of smell
5 (12)
Self-talks to get rid of urges / talks with buddy
1 (3)
Will allow nobody to smoke in home
2 (8)
Health of children in home / ETS
4 (13)
More energy / not tired anymore
6 (14)
Family members smoking
1 (3)
Request of family / boyfriend / husband
3 (9)
No more depression / no cravings / no edginess / nervousness sensitive to smoke
4 (10)
Strong urges in the morning / craving / not smoking
2 (6)
Not enjoying it / bad habit
2 (6)
No longer embarrassed by smell of clothes & hair / teeth whiter
3 (7)
Environmental/ dirty in house
1 (3)
Environmental / house smells better
4 (10)
Baby
N=23
n (%)
Health / development of baby
23 (100)
Table 3: Motivational interviewing phone call responsesa of pregnant women who had quit smoking shortly before or during their pregnancy regarding reasons for quitting, benefits and difficulties in quitting, and plans to stay quit postpartum.
Reasons for quitting smoking among those not currently smoking
Of the 54 participants who reported quitting, only 32 gave specific reasons why they quit. Forty-one percent cited non-respiratory or general health reasons and fourteen (38%) quit due to the pregnancy or associated guilt. Nineteen percent mentioned asthma or other breathing problems. Other reasons why women reported to have quit included the feelings of nausea and bad smell or taste, saving money, the health of children in the home, ETS exposure of others, the request of a boyfriend, husband or other family member, no longer enjoyed smoking, and the environment in the home.
Benefits or changes noticed since quitting
Forty-two participants noticed benefits or changes. Better respiratory function (36%) and saving money (21%) was mentioned. Additionally, better appetite, weight gain and reflux improvements were noted by 24%. Other positive changes noted included better skin, improvement in tasting food, more energy, fewer psychological barriers (depression, cravings, edginess), and no longer embarrassed by the cigarette smell on clothes and hair.
Difficulties/Urges anticipated
Expected difficulties in staying quit were reported by 33 participants. Solutions mentioned regarding urges included eating (15%), keeping busy (15%), and self-talks (3%). Specific moments of difficulty mentioned included social gatherings with friends who smoke stressful moments or mood swings, family members smoking, and strong urges in the morning. However, the highest proportion (39%), stated that they were too sick to think of urges to smoke.
Plans for not smoking after delivery of the baby
Specific plans were reported by 25 participants with 52% reporting that they plan to remain smoke free. Using the study materials to remain smoke free was planned by 20% and use of prayer or “selfwill” to try to stay smoke free was reported by 12%. Keeping busy and allowing no one to smoke in the home were also reported. Several women did not have any plans, as they did not want to think too far into the future.
Discussion
Participants from the NE SCRIPT project provided valuable and informative insights into the motivators, barriers, and facilitators of underserved pregnant women who were trying to quit smoking or had recently been successful in quitting during their MI counseling calls. The approach used to examine barriers and facilitators of smoking cessation among pregnant women was unique in that the information was obtained during MI counseling sessions rather than using traditional qualitative methods. Although a number of our findings are consistent with previous qualitative research, [17] several of our findings may be unique to this population.
A number of the factors identified in this study as barriers or facilitators to quitting smoking during and after pregnancy were also reported by Flemming et al. [17] These factors can be divided into several categories that include: psychological factors (stress and mood management, perceived mental health benefits, enjoyment, weight gain avoidance, behavioral habit, and addiction); individual factors (personal appearance, risks to mother’s health, environment, living conditions); social factors (social support, prevalence and acceptability of smoking in the individual’s environment, relationship with significant others), and changing connection with the infant during and after pregnancy (health risks to fetus and infant, ETS exposure).
Potential health risks to the fetus were reported as a motivator to quit smoking, which is consistent with other studies [5,24]. Yet previous studies reported that women were motivated to quit only temporarily (only during pregnancy); factors (i.e., unborn infant health factors) that motivated women during pregnancy were no longer relevant postpartum as suggested by the high postpartum relapse rates (45% resuming smoking within 3 months postpartum) [10,14]. In fact, estimates are that 50% to 70% of women who stop smoking during pregnancy return to smoking regularly within 6 to 12 months postpartum [25-27].
While some studies report that quitting in pregnancy was perceived as a temporary change in smoking status, [28,29] our findings suggest that some women strive to remain ex-smokers stating that they wanted to bring up their children in a smoke-free environment.
In contrast to previous findings, [17] which reported that health risks perceptions operated as a barrier, we found that both quitters and women who continued to smoke reported that they were concerned about both their own health as well as the health of their infant(s) as motivators to quit smoking. Additionally, we found that the perceived health risks of smoking matched the benefits to be gained from quitting although others were discordant (partners, family, and friends who smoke).
Although some women noted that family and friends encouraged their quitting, others cited family and friends as barriers to quitting [17]. Fleming et al., suggested that among pregnant women, barriers and facilitators are not “fixed and mutually exclusive categories; instead they are factors with a latent capacity to help or hinder smoking cessation” [30]. As suggested by Ingall et al, [16] “women are greatly influenced by partners and friends who smoke and attempting to quit can be costly to these relationships.” As our participants described, barriers included social gatherings with others smoking as well as family members and friends who smoke. In contrast, other women reported pressures from family members contributed to their quitting smoking which has also been documented by pregnant women from other studies [31,32]. In addition, setting a good example for children (i.e., being a positive role model) has previously been reported among pregnant women, as well as among SCRIPT participants.
The benefits of smoking previously documented by pregnant women and the general population, which included relief of tension, coping, and perception of relaxation, were also mentioned by SCRIPT participants. Other barriers associated with smoking that were cited included physiological factors (i.e., nausea, smell and taste). Plesch et al. [33] also described these smoking related changes in a study of 209 pregnant smokers. Of those participants, 53% reported that cigarettes tasted different, 29% stated that after becoming pregnant cigarettes tasted badly, and 30% reported that they tasted stronger or bitter. Also, of 62% who stated that cigarettes smelled different, 39% reported that the smell was worse, and 20% stated that it made them sick [33]. Aversion of smoking is quite common among women who are pregnant, and is consistent with our findings.
Weight concern, another strong motivating factor in the decision to quit smoking during pregnancy, was noted by 25% of SCRIPT participants [34,35]. Weight concern has also been shown to be associated with relapse after pregnancy. Of interest was that in the present study, women who had quit smoking during pregnancy did not mention weight as a potential barrier to staying quit, rather a number of women cited a better appetite and weight gain as a benefit to quitting.
The NE SCRIPT educational material were cited as a facilitator of smoking abstinence postpartum, which was similar to another study [11] that demonstrated effectiveness of education material. Several other factors cited in our study included saving money since quitting; belief of lowering the risk for specific health conditions (i.e., cancer and heart disease) by quitting, ability to gain weight, and the use of self-talk, prayer and self-will to help with quitting and remaining quit.
In considering these findings, several limitations need to be addressed. First, the sample of participants were based on recruitment for a smoking cessation intervention project, which may be subject to “healthy volunteer” bias. However, given that this program was offered to all pregnant smokers regardless of their interest and/or readiness to quit smoking, these findings are likely generalizable to other underserved pregnant women. Also, MI does not present a traditional qualitative data collection technique, which accounts for limitations in the probing and notes taken by counselors. The study intervention tailored the MI counseling to readiness to change so counseling and questions were detailed and tailored for each participant, but were not necessarily consistently applied across the total sample. However, treatment fidelity practices were implemented with all counselors receiving not only an initial training but also posttraining competency assessments, ongoing fidelity checks as well as ongoing support and corrective feedback. Also, adolescent smokers, who were few in this study and were not included in these analyses, should be addressed separately, as the adolescent perspective is potentially very different from that of an adult.
Despite these limitations, this study sample provided insight into potential motivators, barriers, and facilitators among a predominantly group of low-income pregnant women during their processes of quitting and staying smoke free, which were identified prospectively. While these concepts are not novel, the relative emphasis of each response category may lend some quantitative estimate to the prevalence of these thoughts.
Conclusion
Many of the barriers and facilitators identified during MI counseling are common among all pregnant women who smoke. However, we did find that certain thoughts, concerns and motivators of low-income pregnant women as expressed in the MI setting were unique to this underserved subgroup of pregnant smokers which requires further investigation. Our results may help to inform specific topics to include in MI counseling sessions and development of public health materials, such as training for providers, and written, video, web, text or other media for patients to help pregnant women to quit and remain smoke free during after their pregnancy. Additionally, these findings may help inform future research to develop and test new interventions that address the complex and challenging issues of underserved pregnant women’s lives.
Acknowledgments
We especially acknowledge the contributions and leadership of the Principal Investigator, Thomas Lasater, whose tenacity made the New England SCRIPT study possible. The authors also thank all participants of the New England SCRIPT study as well as the Counselors who conducted the Motivational Interviewing for this project.
Funding
This work was supported by funding from NIH #HL57457.
References
- CDC. The health consequences of involuntary exposure to tobacco smoke: a report of the surgeon general. Atlanta, GA: Centers for Disease Control and Prevention. 2006.
- Fiore MC, Jaen CR, Baker TB, Bailey WC, Benowitz NL et. al. Treating Tobacco Use and Dependence: 2008 Update, Clinical Practice Guideline. Rockville, MD: US Department of Health & Human Services 2008.
- Jaakola J, & Gissler, M. Maternal smoking in pregnancy, fetal development, and childhood asthma. Am J Public Health. 2004; 94: 136-140.
- Smoking Cessation During Pregnancy. A Clinician's Guide to Helping Pregnant Women Quit Smoking. 2011 self-instructional guide and tool kit. American College of Obstetricians and Gynecologists, 2011.
- Edwards N & Sims-Jones N. Smoking and smoking relapse during pregnancy and postpartum: results of a qualitative study Birth. 1998; 25: 94-100.
- McBride CM, Emmons KM, & Lipkus IM. Understanding the potential of teachable moments: the case of smoking cessation. Health Educ Res. 2003; 18: 156-170.
- Orleans CT, Johnson RW, Barker DC, Kaufman NJ, & Marx JF. Helping pregnant smokers quit: meeting the challenge in the next decade. West J Med. 2001; 174; 276-281.
- Pletsch PK, & Kratz AT. Why do women stop smoking during pregnancy? Cigarettes taste and smell bad. Health Care Women Int. 2004; 25: 671-679.
- Melvin CL, Dolan-Mullen P, Windsor RA, Whiteside HP, Jr., & Goldenberg RL. Recommended cessation counselling for pregnant women who smoke: a review of the evidence. Tob Control. 2000; 9: III80-84.
- Lumley J, Chamberlain C, Dowswell T, Oliver S, Oakley L, & Watson L. Interventions for promoting smoking cessation during pregnancy. Cochrane Database Syst Rev. 2009 CD001055.
- Brandon TH, Simmons VN, Meade CD, Quinn GP, Lopez Khoury EN, Sutton SK, et al. Self-help booklets for preventing postpartum smoking relapse: a randomized trial. Am J Public Health. 2012; 102: 2109-2115.
- Windsor RA, Woodby LL, Miller TM, Hardin JM, Crawford MA, & DiClemente CC. Effectiveness of Agency for Health Care Policy and Research clinical practice guideline and patient education methods for pregnant smokers in medicaid maternity care. Am J Obstet Gynecol. 2000; 182: 68-75.
- Tong VT, Dietz PM, Morrow B, D'Angelo DV, Farr SL, Rockhill KM, et al. Trends in smoking before, during, and after pregnancy--Pregnancy Risk Assessment Monitoring System, United States, 40 sites, 2000-2010. MMWR Surveill Summ. 2013; 62: 1-19.
- Wen K, Miller S, Roussi,P, Belton T, Baman J, Kilby L, et al. A content analysis of self-reported barriers and facilitators to preventing postpartum smoking relapse among a sample of current and former smokers in an underserved population. Health Educ Res. 2015; 30: 140-151.
- Gamble J, Grant J, & Tsourtos G. Missed opportunities: A qualitative exploration of the experiences of smoking cessation interventions among socially disadvantaged pregnant women. Women Birth. 2015; 28: 8-15.
- Ingall G, & Cropley M. Exploring the barriers of quitting smoking during pregnancy: a systematic review of qualitative studies. Women Birth. 2010; 23: 45-52.
- Flemming K, McCaughan D, Angus K, & Graham H. Qualitative systemic review: barriers and facilitators to smoking cessation experienced by women in pregnancy and following childbirth. J Adv Nurs. 2015; 71: 1210-1226.
- Windsor R. A pregnant woman's guide to quit smoking, 5th edition. Washington, DC: Society for Public Health Education. 1985.
- Cahill, K., & Perera, R. Quit and Win contests for smoking cessation. Cochrane Database Syst Rev. 2008; 10: CD004986.
- Hettema JE & Hendricks PS. Motivational interviewing for smoking cessation: a meta-analytic review. J Consult Clin Psychol. 2010; 78: 868-884.
- Prochaska JO, DiClemente CC & Norcross JC. In search of how people change. Applications to addictive behaviors. Am Psychol. 1992; 47: 1102-1114.
- Miller W & Rollnick S. Motivational Interviewing. Helping People Change (Third ed.): The Guilford Press. 2012.
- Parker D, Windsor R, Roberts M, Hecht J, Hardy N, Strolla L et al. Feasibility, cost and cost-effectiveness of a telephone-based motivational intervention for underserved pregnant smokers. Nicotine Tob Res. 2007; 9: 1043-1051.
- Schneider S, Huy C, Schutz J & Diehl K. Smoking cessation during pregnancy: a systematic literature review. Drug Alcohol Rev. 2010; 29; 81-90.
- McBrid CM & Pirie PL. Postpartum smoking relapse. Addict Behav. 1990; 15: 165-168.
- Mullen PD, Richardson MA, Quinn VP & Ershoff DH. Postpartum return to smoking: who is at risk and when. Am J Health Promot. 1997; 11: 323-330.
- Polanska K, Hanke W & Sobala W. Smoking relapse one year after delivery among women who quit smoking during pregnancy. Int J Occup Med Environ Health. 2005; 18: 159-165.
- Abrahamsson A, Springett J, Karlsson L & Ottosson, T. Making sense of the challenge of smoking cessation during pregnancy: a phenomenographic approach. Health Educ Res. 2005 20: 367-378.
- Kennison LH. Smoking and pregnancy: reconciling incompatibilities. Holist Nurs Pract. 2009; 23: 32-38.
- Fleming K, Graham H, Morag H, Fox D & Sowden A. Smoking in pregnancy: a systemic review of qualitative research of women who commence pregnancy as smokers. J Adv Nurs. 2013; 69: 1023-1036.
- Hiscock R, Judge K, & Bauld L. Social inequalities in quitting smoking: what factors mediate the relationship between socioeconomic position and smoking cessation? J Public Health (Oxf). 2011; 33: 39-47.
- Nasman P & Ortendahl M. Perceived consequences among pregnant and non-pregnant women of continuing or ceasing to smoke. Int J Gynaecol Obstet. 2007; 99: 117-121.
- Pletsch PK, Pollak KI, Peterson BL, Park J, Oncken CA, Swamy K et al. Olfactory and gustatory sensory changes to tobacco smoke in pregnant smokers. Res Nurs Health. 2008; 31: 31-41.
- Berg CJ, Park ER, Chang Y & Rigotti NA. Is concern about post-cessation weight gain a barrier to smoking cessation among pregnant women? Nicotine Tob Res. 2008; 10: 1159-1163.
- Levine MD, Marcus MD, Kalarchian MA, Weissfeld L, & Qin L. Weight concerns affect motivation to remain abstinent from smoking postpartum. Ann Behav Med. 2006; 32: 147-153.
