Abstract
Background: Cultural competent care seems to improve quality of care. Community nurses and otherhealth care professionals should have the knowledge and skills in understanding and dealing with immigrant patients/ clients while caring in the community.Training interventions aimed for health professionals, to meet the diverse needs of patients, have been suggested to be effective in increasing the knowledge and capability of addressing cultural issues. Measuring the effect of a study abroad program is one way to determine its impact on developing nurses’ cultural competence.
Aim: ?he paper aims to present the cultural competence level of community nurses in Cyprus, before and after a cultural competence workshop as an intervention.
Method: A quasi-experimental design was used in this study, participating two groups with pre-test and post-test to investigate culturally competence related factors. Between pre-test and post-test an intervention (a cultural competent training workshop) was held with 92 community nurses from a total of 170 that participated in the larger study. The intervention training was based on the Papadopoulos, Tilki and Taylor Model (PTT).
Results: After intervention 25% of community nurses who participated in the workshop improved their cultural competence level based on the Culturally Competent Tool of the PTT Model.
Conclusions: The findings indicated that this particular training intervention seemed to be effective as it increased nurses’ cultural competence levels.
Keywords: Cultural competence; Cultural awareness; Cultural knowledge; Cultural sensitivity; Cultural competence training intervention
Introduction
The ethnic demography in the Cypriot society is constantly evolving and cultural diversity is increasing. The most recent statistics showed that, in 2011, there were 173.009 foreign citizens comprising of 68 different nationalities living permanently in Cyprus with a total of 2.626 still remaining stateless or unknown [1].
This multiplicity of various nationalities is changing Cyprus into a multicultural country and it is posing new challenges for the health care system. In order to minimize the health disparities related to the cultural backgrounds of patients, health care professionals should improve their cultural competence [2]. This can be defined for example “as the on-going process in which the health care provider continuously strives to achieve the ability to effectively work within the cultural context of the client (individual, family, community)” [3].
Educational and training interventions aimed for health professionals, to meet the diverse needs of patients, have been suggested to be effective in increasing the knowledge and capability of addressing cultural issues [4,5]. Beach et al. [6] conducted a systematic literature review of 34 intervention programs designed to improve the cultural competence of health care providers. According to their literature review cultural competence education does promote and enhance the cultural knowledge, attitudes and skills of health professionals. However, they mentioned that there is a lack of evidence that the cultural competence training would improve patient outcome and they suggested that future research should pay more attention to the effects of cultural competence training from a patient’s point of view [6]. Measurements of effectiveness and a description of the program’s content and format are essential in determining a study’s strength [5].
Culture and Cultural Competence
Health care professionals should have knowledge of the influence of culture in the care processes when encountering immigrant patients/clients. The concept of culture has to be integrated in all aspects of nursing care and there are multiple definitions for culture to consider. Hall [7] gives a broad definition of culture by saying that it is “the study of relationships between elements in a whole way of life”, rather than the practice or a simple description of morals and modes of thinking in societies. Multiculturalism in health care refers to the dissimilarities brought on by patient’s cultural, national and ethnical background as well as the different social reality experienced by the patient. The underlying assumption in this final project was that every individual is culturally unique and it is important to acknowledge that there is as much diversity within the cultural groups as there is between them [8].
Cultural competence is viewed as an on-going process by both Papadopoulos and Campinha-Bacote [9,3], however, the latter emphasizes the requirement of health care providers to see themselves as becoming more culturally competent rather than already being culturally competent. To achieve this level, they must first and foremost be aware of their own attitudes, beliefs and practices on cultural matters. When encountering different views of the culturally diverse patients who do not share the same opinions and values, the health care professional must be prepared and willing to adjust these attitudes and behaviour [10].
The most important tools for health care professionals in multicultural encounters are professional knowledge, understanding, sensitivity and interaction skills. Respecting both the patient and the patient’s values are intertwined in the encounters [11]. When discussing different care options with the patients, the primary starting point is respect for the patient’s cultural beliefs, customs, life, values and following the patient’s own will. Even though the decisions in health care are often made together with the family of the patient, it is still important to stress that the patient’s own will and wishes will be heard. As the number of different cultures encountered is increasing at speed, it is becoming more challenging for a nurse to obtain culture specific knowledge [11].
This poses new challenges to cultural competence education as well. It is important to begin teaching the cultural competency attitudes and skills at the beginning of curricular studies. This should include learning to assess diverse patients´ needs and increase understanding of their problems. Early introduction to cultural issues may help the future health care professionals to become more culturally competent and patient-focused as they start practising their profession [11].
Nowadays, nurses care for culturally diverse patients, thus nursing requires culturally competent practitioners. Academics and/ or nurse educators that are responsible for preparing nurses, who will provide culturally appropriate care, need effective approaches for teaching transcultural nursing. Experiential learning, an important dimension of cultural competence, has been well-recognized as a method for changing attitudes. Study abroad programs can provide nurses with this type of learning [12].
Many nurse educators believe that discussing different cultures with nurses often highlighted important differences; unfortunately, in many instances, this resulted in reinforcing stereotypes. That is, individuals from a specific culture were discussed as homogenous. To date, nursing continues to refine both the importance of and the method for teaching cultural competence. Knowing that diversity exists and being “sensitive” to cultural differences have evolved today into the process of cultural competence [12].
In addition to models, several instruments have been developed that measure one of more of the dimensions considered a part of cultural competence. However, some of these measures may not be useful if educators are seeking a comprehensive measure of cultural competence. In this study the Cultural Competence Assessment Tool (CCA Tool) by Papadopoulos and Lees [13], based on Papadopoulos, Tilki and Taylor model (PTT model), is used. It measures all dimensions of cultural competence. Nurse educators should be aware that some tools may be more appropriate for use or specifically designed for nurses, rather than healthcare providers in general [12- 14].
Papadopoulos, Tilki and Taylor Model (PTT model)
The model refers to the nurse’s capacity to provide effective health care that takes into consideration the patient’s cultural beliefs, behaviours and needs in the nursing process. The model includes four components of cultural competence: 1) cultural awareness, 2) cultural knowledge, 3) cultural sensitivity and 4) cultural practice (Figure 1). Further, the PTT model emphasized the need for nurses to have both culture-specific and culture-generic competence. Culturespecific competence refers to the knowledge and skills that would enable nurses to understand the values and cultural prescriptions that relate to a particular ethnic group and operate within a particular culture. Culture-generic competence is defined as the acquisition of knowledge and skills that are applicable across ethnic groups [15]. Apart from these areas, they also emphasized the need for nurses to promote anti-oppressive and anti-discriminatory practice. To provide this knowledge and skills with structure and to facilitate learning, the following stages were proposed. A conceptual map is provided for each stage as a guideline but can be modified to suit the type and level of nurses.
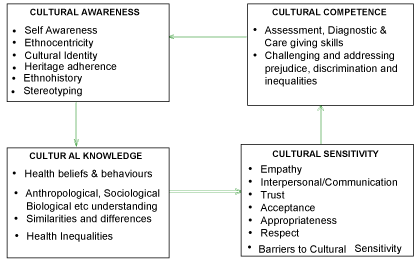
Figure 1: The Papadopoulos, Tilki and Taylor Model for Developing Cultural
Competence [17].
The first stage in the model, cultural awareness, begins with an examination of one’s own personal value base and beliefs. Raising self-awareness crucially contributes towards understanding the nature and construction of cultural identity. At the same time, a person becomes more aware that cultural background is a major factor in shaping one’s values and beliefs and in turn health beliefs and practices. Therefore the ‘cultural awareness’ stage constitutes an essential first stage in the process of achieving cultural competence [16].
The second stage is cultural knowledge which can be gained in a number of ways. Meaningful contact with people from different ethnic groups can enhance knowledge about health beliefs and behaviours and raise understanding of problems faced. This knowledge is required in order to understand the similarities and differences of cultural groups as well as the inequalities in health within and between groups. An important element in achieving cultural sensitivity -the third stage- is how professionals view people in their care. Considering research participants as true partners is an essential component of cultural sensitivity and a crucial element in anti-oppressive practice. The achievement of the fourth stage, that of cultural competence, requires the synthesis and application of previously gained awareness, knowledge and sensitivity. Further, focus is given to practical skills such as assessment of need, clinical diagnosis and other caring skills [16].
Methods
The study was a comparative quantitative one with a pre-test, post-test data collection period. A quasi-experimental design was used in this study with a sample of 170 community nurses (pre-test) and 158 community nurses (post-test). The one day seminar course served as the intervention.
Ethical considerations
Permission to conduct the research was obtained from the Cyprus National Bioethics Committee. The researchers provided participants with an information sheet about the study and a consent form. Anytime they wished they could terminate their participation in the study. Confidentiality was maintained by coding the questionnaires so that responses could not be linked to any individual nurse. Participation in the workshop was voluntary.
The cultural competence assessment tool (CCA Tool)
The self-assessment CCA Tool [13] of Papadopoulos and Lee’s is based on the model of Papadopoulos et al. [17]. It consists of four sections (awareness, knowledge, sensitivity and competent practice), with an equal number of statements in each section with which the participant can either agree or disagree. In addition, visual analogue scales (VAS) are included which allow the participants to self-rate their cultural awareness, knowledge, sensitivity and practice.
The agree/disagree responses to statements were marked by the authors, and a level of cultural competence was assigned depending on which statements were correct. The levels were ‘cultural incompetence’, ‘cultural awareness’, ‘cultural safety’ or ‘cultural competence’. As participants were unable to determine (objectively) their own level of cultural competence on completion of the tool, the VAS provided them with an opportunity to self-assess their competence and provided the researchers with an opportunity to compare personal perceptions of cultural competence with objective scoring. It was anticipated that the participants would achieve a higher level of cultural competence as a result of the intervention [16,18].
The intervention- A training workshop on cultural competence
Randomized sampling of the community nurses was used. Ninety two (n=92) community nurses participated in the workshop attending 7 hours’ workshop at a university setting. The workshop was repeated two days (n=50 the first day and n=42 the second day). One of the authors of the model was the main trainer. Two of this paper authors participated also as trainers.The training consisted of three sessions as described below:
a) Cultural awareness session: The aim of the cultural awareness session was to assist participants in recognizing the need to examine their own cultural values, beliefs and practices in order to reduce the risk of cultural bias, cultural clashes and the imposition of inappropriate or unethical care through ethnocentric assessments. A cultural introduction exercise focused on the culture of the participants, exploring the impact of gender, age, socio-economic and other differences, and socialization in different communities and societies. It highlighted the culture of all peoples who live in Cyprus and the way in which individuals adhered to different aspects of their culture contextually. This was followed by a values clarification exercise emphasizing the values that exist across cultures but that are shaped by time and society.
b) Cultural knowledge session: The cultural knowledge session highlighted the potential for misunderstanding due to ethnocentricity, stereotyping and the impact of the unequal distribution of power.
It then focused on health beliefs and behaviors and the cultural meanings of illness in different minority ethnic groups. Thereafter was devoted to the origin of common stereotypes, examining myths and realities about particular ethnic groups and the impact and access to healthcare. The aim of this session was to explore the origins and impact of stereotyping on individuals and services, to examine stereotypes of common minority ethnic groups in catchment area (such as Sri Lankan, Turkish-Cypriots, Philippino), to consider the truths and myths of different stereotypes and how these impact on health and to reflect on the impact of stereotypes on client care and on both therapeutic and professional working relationships.
c) Cultural sensitivity and cultural practice session: The cultural sensitivity session focused on ways of avoiding insensitivity and establishing trust and rapport in order to facilitate accurate assessment, diagnosis and the delivery of holistic culturally appropriate care. This session dealt with interpersonal relationships with clients whose first language was not Greek, and explored differences in verbal and non-verbal communication. It also included attention to the differing ways in which distress is expressed across cultures and religious groups. This session focused on family responsibility and its role in relation to caring in different cultures, highlighting differences in family structure, function and roles which influence healthcare.
As cultural competence comprises cultural awareness, knowledge and sensitivity, the focus in these sessions was on nursing practice. The session explored the principles of anti-oppressive practice in relation to ethnic minority clients and families, exploring their strengths and challenging racist attitudes and practices. It then explored ways of helping clients overcome fear and mistrust, assessing mental state and working with clients’ explanatory models and coping strategies.
As in all the sessions, participants shared examples of good and bad practice and drew upon their own cultural knowledge, professional practice and perspectives from differing professional disciplines. Where possible, research-based evidence was utilized but much was learned from the cultural knowledge and experience of participants.
Results
Participants’ ages ranged from 26-62 years old. The mean was 37.76 years. Gender was predominately female (91.3%).Most of the community nurses were from health visitors departments (48.9%). The rest were from home nursing departments (21.7%), mental health centres (25%) and from rural centres (4.3%).
The community nurses who participated in the workshop, 64.1% stated that they often come into contact with people of other nationalities, 25% frequently and 10.9 % rarely, and 22.8% stated that they were helped enormously by the workshop, 54.8% considerably, 20.6% slightly and 1.8% not at all.
When the community nurses were asked why there were not interested in learning about other cultures, the following answers were given because they: a) may ‘not be interested’ in other cultures, b) were never taught such a thing, c) didn’t have a colleague from another culture.
When the participants were asked how many of them have friends from other cultures, 7 participants (7.6%) responded positively (over the2days) and the rest gave a negative answer. Some stereotypes they referred to included: “Husband snatchers, low education, thieves, dirty, lazy, aggressive, mafia members, violent, dangerous, not honest, demanding, strange eating habits, responsible for unemployment, they smell, they create ghettos…”
Participants reported that they needed more time to express themselves. Also noteworthy in the discussions was that nobody mentioned that Cypriots were migratory people. Participants also stated that the workshop was a unique experience for them and that it gave them the opportunity to re-evaluate their ‘cultural self’. They reported that through the exercises they saw aspects of themselves - as a reflective experience.
They expressed the need and the desire to participate in similar workshops again to improve their practices in transcultural health and nursing care. All participants acknowledged that many Cypriots may have racist feelings and/or perceptions due to misconceptions and stereotypes. However they agreed that, this should not be possessed by health professionals and this workshop helped the participants to manage or modify believes and perceptions associated with negative feelings toward other cultures. Ultimately this will help in transforming behavior in everyday life.
It is essential to note that community nurses who participated in the workshop had 4.8times more possibilities of improving their cultural competence level, than the community nurses who did not participate in the workshop (Table 1).
WORKSHOP (participation)
Change in cultural competence level
YES
NO
?
%
?
%
YES
22
84,6
70
53,4
NO
4
15,4
61
46,6
p-value
0,03
Odds ratio
4,793
Table 1: Possibility of improving cultural competence level, with the participation in the workshop.
Discussion
There was greater willingness to identify knowledge deficits about particular cultural groups rather than examine beliefs and attitudes towards clients or to reflect on professional practice.
Nurses exposed to a different culture of clients than in their home environment can gain some proficiency in cultural competence through a study abroad program. Even short programs can have the benefit of additional learning. Therefore the measurement of effectiveness over a longer period of time is essential. Influencing other nurses on competence who have not had the opportunity to study abroad might also be a strategy; this would also continue to reinforce the participants’ learning.
While this study did not use qualitative data as a measure of effectiveness, such data, especially regarding nurses evaluation of the program and the course work, can further enhance and improve a program and should be considered.
This type of information may influence outcomes of nurses’ learning and acquisition of proficiency. Using the same country for annual experiences has the benefit of providing the faculty with an opportunity to continually refine their program and the important relationships in the host country.
In order to use reported research findings, nurse educators must continue to be aware of the differences in the definitions of terms such as cultural awareness, sensitivity and competence used in investigations. Clarification is also needed in the literature regarding whether a program is a study abroad program, an exchange program or an immersion program.
Further, in order to promote replication, researchers should include the program’s goals, objectives and strategies on which research on effectiveness is based on their reports.
Principles for effective cultural competence training
1) Compulsory mandates to attend cultural competence training programmes can lead to resistance or at best superficial participation, invoking sensitivities by suggesting that participants’ performance is less than satisfactory. Therefore, it is more effective to adopt a holistic approach, involving participants in decisions about the training programmes, emphasising the benefits for all patients/clients as well as the whole organisation and the community [19].
2) It is necessary to allow adequate time out for health care professionals to disengage from the intensity of their everyday work and to engage in cultural competence learning.
3) It is important to have a clear framework for the delivery of cultural competence training and to recognise that while educational content is essential, the process of learning is equally significant.
4) Although factual knowledge about diverse groups, habits and customs may be more acceptable to participants, training should be moved beyond the delivery of facts to challenging ethnocentric beliefs, practices and unwitting prejudice among staff.
5) Pre- and post-training assessment of cultural competence is highly desirable for three reasons: to provide information about participants’ existing levels of cultural competence, to give an indication of the effectiveness of the training to the trainers, and to provide the participants with a measure of their progress.
6) Training programmes should be evaluated and lessons learned and if possible shared with others.
The application of these principles will lead to effective cultural competence training which will result in better patient/client care for all leading to a culturally competent practice and an increase satisfaction within the community.
Limitations
There are limitations in this study. The sample was not randomly selected. However, the research team decided to proceed with a convenient sample because it was very difficult to locate and approach certain groups of community nurses.
Conclusion
Short-term, financially feasible study programs can produce changes in cultural competence for nurses. This study’s results add to the literature on the effectiveness of such a program. The study also provided support for the specific PTT model and its relevant instrument on cultural competence for health professionals.
A description of the program that was included may assist other nurse educators in planning such an experience. In addition, comparisons of nurses who participate in such an experience and those who have had only the traditional learning for cultural content and competence should be undertaken. Further studies might also address the application of increased cultural competence on nurses’ clinical practice.
Nurses should be informed about the diverse needs of different people in order to understand and contribute to their satisfaction. Culturally competence care is an essential element of the 21st century for those who are responsible for providing health care in transcultural societies. The Community Nurse must respect the different language, values and traditions of a social group, to incorporate the culture of individuals to care and be open to different ways of incorporating the client’s treatment and to possess social skills such as patience, lack of selfishness and rejection, respect, desire for change and learning.
Acknowledgments
The authors greatly appreciate the continuous support, advice and guidance given by Professor (I) Rena Papadopoulos, Middlesex University and deeply thank her for the provision of her tool and model and leading the intervention workshop.
References
- Cyprus Statistical Service. 2012.
- University Research Institute of Urban Environment and Human Resources, UEHR-National Kapodistrian University of Athens Medical School, IOM. Equality in Health: Greek National Report. European Commission. 2006.
- Campinha-Bacote J. The Process of Cultural Competence in the Delivery of Healthcare Services: A Model of Care. Journal of Transcultural Nursing. 2002; 13: 181-183.
- Moffat J and Tung JY. Evaluating the effectiveness of culture brokering training to enhance cultural competence of independent living centre staff. Journal of Vocational Rehabilitation. 2004; 20: 56-59.
- Hunter JL and Krantz S. Constructivism in Cultural Competence Education. Journal of Nursing Education. 2010; 49: 207-213.
- Beach MC, Price EG, Gary TL, Robinson A, Gozu A, Palacio A, et al. Cultural Competency: A Systematic Review of Health Care Provider Educational Interventions. Medical Care. 2005; 43: 356-373.
- Hall S. Cultural Studies: Two paradigms. Media, Culture and Society. 1980; 2; 57-72.
- Giger J, and Davidhizar R. Transcultural Nursing- Assessment and Intervention. 4th ed. St. Luis: Mosby. 2003.
- Papadopoulos I. Transcultural Health and Social Care. Development of Culturally Competent Practitioners. Elsevier. 2006.
- Vanderpool HK. Report of the ASHP Ad Hoc Committee on Ethnic Diversity and Cultural Competence. American Journal of Health-System Pharmacy. 2005; 6: 1924-1930.
- Crosson J, Deng W, Brazeau C, Boyd L, Soto-Greene M. Evaluating the Effect of Cultural Competency Training on Medical Student Attitudes. Family Medicine. 2004; 36: 199-203.
- Ballestas H and Roller MC. The effectiveness of a study abroad program for increasing student’s cultural competence. Journal of Nursing Education and Practice. 2013; 3: 125-133.
- Papadopoulos I. and Lees S. Developing culturally competent researchers. Journal of Advanced Nursing. 2002; 3: 258–264.
- Campinha-Bacote J. Cultural Competency in Healthcare Delivery: Have I Asked Myself the Right Questions? 2012.
- Gerrish K and Papadopoulos I. Transcultural competence: The challenge for nurse education. British Journal of Nursing. 1999; 8: 1453-1457.
- Papadopoulos I, Tilki M, Ayling S. Cultural Competence in Action for CAMHS: The development of a cultural competence assessment tool and a short cultural competence training programme. Contemporary Nurse (Special TCN issue). 2008; 2: 129-140.
- Papadopoulos I, Tilki M, Taylor G. Transcultural Care: A guide for Health Care Professionals. London Quay Books. Wilts. 1998.
- Vasiliou M, Kouta C, Raftopoulos V. The use of the cultural competence assessment tool (CCATool) in community nurses: The pilot study and test-retest reliability. International Journal of Caring Sciences. 2013; 6: 44-52.
- Kandola R and Fullerton J. Diversity in Action: managing the mosaic. London: Institute of Personnel Development. 1998.
