Abstract
The hospitalization of smokers is an additional motivation to cessation, as it poses forced abstinence.Studies including outpatients that attended a cessation clinic reveals differences in self-reported and biochemically verified abstinence in 7-11% of subjects. Determination of carbon monoxide in exhaled air and saliva continine are reliable biomarkers for measuring smoking status.
Objectives: To assess the accuracy of self-reported smoking cessation using biomarkers verification among hospitalized patients, and receipt of smoking cessation interventions during hospital admission. Materials and Methods: A prospective study was conducted in medical clinic in a University Hospital from January to May 2013; we obtained data from admitted smokers who reported abstinence since admission. We perform interview, exhaled carbon monoxide and cotinine saliva measurement.
Results: 40 patients, 22 women, mean age was 54.2 years ± SD 2.5. Eleven had strong nicotine dependence. By exhaled carbon monoxide and saliva cotinine, abstinence was found in 82.5% and 72.5% respectively. 55% of the patients received cessation advice, 35% were referred to tobacco cessation clinic.
Conclusion: Self-reported smoking abstinence in hospitalized patients had false positives. Inaccuracy self-reported abstinence in hospitalized smokers was higher than that reported in outpatients. There are more false positives in admitted patients than in outpatients. Almost half o hospitalized smokers do not receive adequate intervention for smoking cessation
Keywords: Cessation; Hospitalization; Self-report; Biomarkers abstinence
Introduction
Smoking is the leading cause of preventable disease and death worldwide [1,2]. About a third of the world's population smokes. In 2003 the World Health Organization developed the Framework Convention for Tobacco Control the Convenio Marco de la Organization Mundial de la Salud para el Control del Tobacco (CMCT), the first treaty of global public health, as a package of strategic measures to achieve tobacco control globally [2,3]. To ratify the treaty, Uruguay has implemented different legal, social, political, economic, health care and educational cessation evidence based strategies.
Hospitalization of a smoker is an additional motivation for cessation and determines forced abstinence in most of the cases, however not all inpatient refer their true smoking status at the time of admission, and routine cessation intervention is not a standardized practice in hospitals. There are few national studies that establish the reliability of self-reported smoking abstinence. One study reported up to 11% false self-reports of abstinence when collated with measurement of carbon monoxide (CO) in expired air, attending outpatient unit cessation [4]. International studies found between 3% and 6% false negatives in outpatients, also cross-checked with exhaled CO [5-7].
There are different biomarkers to assess smoking status, measurement of CO in exhaled air or the determination of nicotine and cotinine in plasma, saliva, urine and hair; among others [4,5].
Determination of carbon monoxide in exhaled air and saliva cotinine are reliable biomarkers to measure the consumption of tobacco. They are non-invasive, inexpensive and easy to implement [8-10].
CO has a half-life of 2 to 5 hours and its levels in exhaled air normalize after 48 to 72hrs after last cigarette. Smokers tend to have concentrations of exhaled CO above 8 to 10 parts per million (ppm), that is why these values smoking status, with a saernes tiatikveitny aosf s 9ta0n%d a[6rd,1 c1u].t -Aolffth poouignht tiot desifftaebrlsi sinh international literature, Erhan et al. in a prospective analytical study that included 322 patients, 243 smokers and 55 non-smokers, found that the cut-off point for the exhaled CO with greater sensitivity and specificity to classify smoking status was 6.5ppm In addition, there are both individual and environmental factors that can alter the level of exhaled CO and therefore the cut-off point. Individual variables include smoking rate, puff depth physical activity and ventilatory capacity of individuals, conditions such as asthma or chronic obstructive pulmonary disease (COPD). The contribution of environmental exposures such as combustion fuel vehicles, among others should be considered, however non-smokers have CO values below 6ppm [12-15].
Cotinine is a product of nicotine metabolism in the liver; the latter is the major psychoactive component of tobacco smoke. The measurement of salivary cotinine can detect tobacco consumption in the last two to four days. It has high sensitivity and specificity for detecting consumption in 97 and 99 % respectively. In non-smokers saliva cotinine levels are below 10ng /ml [6].
The aim of this study was to assess the reliability of self-reported smoking abstinence in smokers admitted using two biomarkers: salivary cotinine and carbon monoxide in exhaled air. A secondary objective was to determine how often hospitalized patients receive cessation intervention.
Materials and Methods
Design and Population
We conducted a prospective, analytical study. The population were patients admitted to an Internal Medicine Clinic at a University hospital, Clinics Hospital, Facultad de Medicina, and Universidad de la República. All patients admitted consecutively from 1st March to 31st May 2013 who reported being current smokers and had quit since hospital admission were included as a convenience sample. Patients who refused to participate were excluded.
Procedure and variables measured
Daily surveys were performed to identify patients who met the inclusion criteria. Once the patient was eligible, underwent an interview and measurements after at least 4 days in hospital to avoid misclassification of smoking status due to biomarkers clearance halflife.
Variables obtained by the interview were: basic demographics, age of onset of smoking, smoking rate, type of tobacco consumption, previous quit attempts, date and approximate time of the last cigarette. Fagerstrom Test for Nicotine Dependence (FTND) was performed [16]. Receipt of cessation intervention was assessed in the interview.
Co in exhaled air measurement was performed with Pico Smokerlizer® portable monitor, using as a cutoff point = 6ppm; and measurement of saliva cotinine through Nic Alert® sticks, using a cutoff point of = 11ng/mL (semi quantitative method, chromatographic).
Health care teams were unaware of secondary objective to avoid information bias.
Statistical analysis
Basic statistics were used to report quantitative and categorized variables Correlation between self-reported abstinence and values of biomarkers was analysed. Self-reported sensitivity was calculated, taking as reference both exhaled CO and salivary cotinine at the mentions cut off levels. SPSS version 19 package was used.
Ethical aspects
The study obtained the approval of the Institutional Ethics Committee. Patients signed informed consent.
Results
40 patients were included, 22 were women, with a mean age 54.2 ± SD 2.5 years. Nicotine dependence according to FTND was high in 11 cases, moderate in 16 cases and mild in 13 cases. Population characteristics are shown in Table 1. By exhaled CO and salivary cotinine abstinence was found in 82.5% and 72.5% respectively (Figure 1).
Characteristics
SEX
53.5% Women
45% Men
AGE
54.2±2.5
20-80
AGE of ONSET
16.5±1.3 Years
8-50 Years
CIG/DAY average
23
PREV QUIT ATTEMPTS
55% Patients
FAGERSTROM LOW
37.50%
FAGERSTROM MODERATE
35%
FAGERSTROM HIGH
20%
Table 1: Population characteristics.
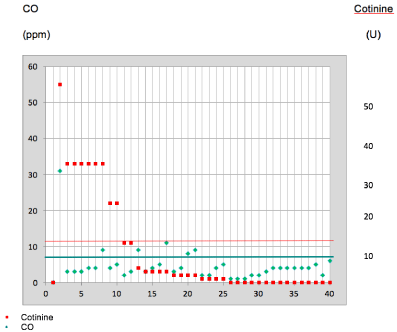
Figure 1: CO and continine level.
Using biochemical verification to assess no smoking status, selfreported abstinence showed a 74% sensibility.
Patients received some form of cessation intervention in 55% of cases, of these 62.5% received brief counselling, 35% were referred to the tobacco cessation unit, 20% were asked about second hand smoke exposure and 50% was informed about the health damages related to smoking. Health care providers who provided these interventions were nurses in 35% of cases, physician in 72.5%, 12.5% students, and some patients received information from more than one member of the health team (Figure 2 and Figure 3).
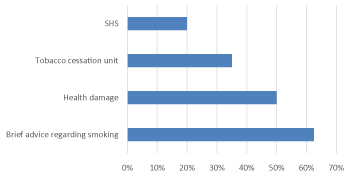
Figure 2: Intervention during the hospitalization. SHS: Second Hand Smoke.
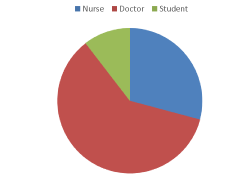
Figure 3: Health care providers who gave advice.
Discussion
According to our study, self-reported smoking abstinence in hospitalized patients has false positives. Using biochemical verification by exhaled CO and salivary cotinine abstinence was found in 82.5% and 72.5% respectively. Using these methods to assess non-smoking status, self-report abstinence had shown a sensitivity of 74%.
These results are consistent with the findings in outpatient setting in a smoking cessation clinic. Parodi et al, reported positive biomarkers indicating current smoking in 11% patient’s selfreporting abstinence [4].
However Barruco and colleagues reported only 3% false negative, concluding that the reliability of self-reporting abstinence in patients attending cessation units is high and therefore the measurement of CO exhaled should not be performed routinely, but it could be useful, as a motivator [5,17]. In our study, this rate is 18.5% and 17.5% for CO and cotinine respectively. One possible explanation for this high inaccuracy in self report may be the fear of being stigmatized if they reveal their true smoking status during hospitalization. In an outpatient cessation program, frequent and sustained contact between patients and providers, create the appropriate climate to disclose the true status, even if patient has failed to achieve complete cessation [17]. The smoking of the patients because of the lack of time or knowledge. We do not link false negatives to second-hand smoke even though the CO can be modified by environmental conditions, generally does not rise more than 10ppm and our patients had greater than this value levels [5,18].
Even though the use of biomarkers helps assess smoking status and intervene appropriately, availability and cost prevent them to be widely used, outside the research field.
As for the secondary objective only 55% of inpatients received any form of cessation intervention, 35% were referred to the cessation programme of the institution. This means that about half of hospitalized smokers do not receive adequate intervention for cessation, missing a window of opportunity, attachable moment were smokers may be more motivated to quit, fact is that about 45% did not provide information or brief counselling.
Our study has weaknesses such as a small simple size, from single health centre where patients belong to a low social economic status, which might not be representative of smokers in general. However, it has strengths, as using to different biomarkers to assess smoking status.
Conclusion
In our study the reliability of self-report in hospitalized patients is lower than that reported in the literature. Nearly half of the patients did not receive advice for cessation. Both aspects should be considered and targeted with systematic evidence based intervention by the healthcare providers. Need to further train health care providers on cessation skills should be considered.
References
- World Health Organization. WHO Report on the Global Tobacco Epidemic. 2013.
- Organizacion Mundial de la Salud. Tobacco Fact Sheet N 339 [Internet]. 2012.
- World Health Organization. WHO report on the global tobacco epidemic: 2008—the MPOWER package. 2008.
- Parodi C, Llambi L, Barros M, Esteves E. Medicion de monoxido de carbono en la unidad de cesaicon de tabaquismo: lecciones aorendidas. Arch Med Interna. 2013; 35: 33–37.
- Barrueco M, Jimenez Ruiz C, Palomo L, Torrecilla M, Romero P, Riesco J. Veracidad de la respuesta de los fumadores sobre su abstinencia en las consultas de deshabituacion tabaquca. Arch Bronoconeumologia. 2005; 41: 135–140.
- Benowitz NL, Peyton J, Ahijevych K, Hall S, LeHouezec J, Hansson A, et al. Biochemical verification of tobacco use and cessation. Nicotine Tob Res. 2002; 4: 149–159.
- Rigotti NA, Clair C, Stead LF, General M, Hospital MG. Interventions for smoking cessation in hospitalised patients. Cochrane Database Syst Rev. 2015; 1–73.
- Deveci S, Deveci F, Açik Y, Ozan A. The measurment of exhaled carbon monoxide in healthy smokers and non-smokers. Respir Med. 2004; 98: 551–556.
- Zabert G, Bartolome Berra F, Videla A, Zabert I. Factores que afectan las mediciones de monoxido de carbono en el aire exhalado como biomarcador del consumo de tabaco. Prev Tab. 2012; 14: 11–18.
- Perez Trulen A, Herrero Labraga I, Clemente Jimenez M, Marton Tunidor R. Marcadores biologicos para la determinacion de exposicion de los fumadores. In: Fagerström KO, Jimenez Ruiz C, editors. Tratado de tabaquismo. Madrid: aula medica. Formacion en salud; 2004; 299–314.
- King Ba, Dube SR, Tynan Ma. Secondhand smoke exposure in cars among middle and high school students--United States, 2000-2009. Pediatrics [Internet]. 2012; 129: 446–452.
- Jiménez-Ruiz CA, Fagerström KO. TRATADO DE TABAQUISMO. 3rd ed. Madrid: aula medica. Formacion en salud; 2011.
- Sayazu K, Sekizawa K, Okinaga S, Yamaya M, Ohrui T, Sasaki. Incresed carbon monoxide in exhaled air of asthmatic patients. Am J Resp Crit Care Med. 1997; 156: 1140–1143.
- Chatkin G, Chatkin J, Aued G, Petersen G, Jeremias, ET, Thiesen F. Evaluation of the exhaled carbon monoxide levels in smokers with COPD. J Bras Pneumol. 2010; 36: 332–338.
- Sato S, Nishmura K, Koyam H, Tsukino M, Oga T, Hajiro T. Optimal cutoff level of breath carbon monoxide for assesing smoking status in patients with asthma and COPD. Chest. 2003; 124: 1749–1754.
- Fagerström KO. Measuring degree of physical dependence to tobacco smoking with reference to individualization of treatment. Addict behav. 1978; 3: 235–241.
- Velicer W, Prochasaka J, Rossi J, Snow M. Assesing otcome in smoking cessation studies. Psychol Bul. 1992; 11: 23–41.
- Eriksen M, Mackay J, Ross H. EL ATLAS DLE TABACO. 4th ed. Atlanta, Georgia: American Cancer Society; 2012.
