Abstract
Using a cross-sectional statewide survey, we described specialist attitudes and beliefs about Medicaid patients and characteristics associated with negative beliefs. 804 physician members of the Colorado Medical Society providing adult specialty care in Colorado (1600 eligible) endorsed 14 positive and negative characteristics about Medicaid patients on a Likert Scale from which we created a “favorableattitude outcome.86% of r versus “unfavorableattitude outcome.86% of r attitude outcome.86% of respondents had unfavorable attitudes towards Medicaid patients. In an adjusted model, unfavorable attitudes were associated with physician characteristics of income highly dependent on productivity (versus little/no dependence p=.01; versus some dependence, p=.07), an independent practice (versus employed by large organization, p=.03), and being in a surgical or hospital-based specialty (versus a medical specialty p=.05 and p‹.01, respectively).Given the potential for negative bias to affect access to and quality of care, more research is needed into the contributors to and effects of this bias.
Keywords: Medicaid; Access; Bias; Vulnerable Populations
Abbreviations
ACA: Affordable Care Act; CMS: Colorado Medical Society; OBGYN: Obstetrics/Gynecology
Introduction
Medicaid, the largest United States health coverage provider, insures more than 1 in 5 Americans. In states expanding Medicaid, Medicaid and Children’s Health Insurance Program enrollment increased nearly 39% under the Affordable Care Act (ACA) as of May, 2017 [1]. Colorado is among the trend leaders with only 2 states surpassing its 76% enrollment increase as of May, 2017 [2].
There is currently little understanding of how Medicaid patients are viewed by physicians. Do physicians view this patient population positively and welcome them into their practices? Or do negative beliefs predominate, with potential implications for lowered quality of care and reduced willingness to improve access? In national healthcare debates, a common critique of Medicaid centers around lower practice acceptance of Medicaid patients [3], heightening the relevance of these questions.
The importance of answering these questions is further underscored by a growing body of evidence on bias in health care, mostly with regard to racial bias [4]. These studies showed that many physicians had negative attitudes that favored whites over minority groups [5,6]. Furthermore, these attitudes were reflected in worse interactions with minority patients [7-9], and in some cases may have affected medical decision-making [10-12].
To date, most investigations of physician bias have focused on general attitudes – overall positivity or negativity without regard to underlying beliefs. Such attitudes revealed general propensities to behave more positively or negatively, but did not provide information about specific issues that may be of concern [13]. For example, a belief that a patient group is dangerous would imply different reactions than a belief that the group is lazy, although both are negative. The goal of the current study was to examine specialty physicians’ attitudes and beliefs about Medicaid patients. We further investigated practice and physician characteristics associated with negative attitudes. We focused on specialty rather than primary care because Medicaid patients experienced worse specialty care access compared to Medicare and privately insured patients [14].
Methods
Population surveyed
To obtain a wide sample across the state, we partnered with the Colorado Medical Society (CMS) for physician recruitment. CMS is the largest organization of physicians in Colorado, with over 7,500 members across all specialties and employment settings. After passage of the ACA, CMS identified access to specialty care as a strategic priority, leading to organizational support of this member survey. Physicians were excluded if retired, still in training, primarily in pediatric practice or focused on general medical care including family medicine, general internal medicine or emergency medicine. From the resulting pool of 3,266 adult specialist CMS members for recruitment, 1,800 were randomly selected to receive a solicitation letter with a $2 bill included. Of letter recipients, 200 were subsequently found to be ineligible (e.g., deceased, met exclusion criteria or invalid contact information), leaving 1600 for recruitment. Between April and June of 2014, physicians with email addresses known to CMS (70%) were sent up to 5 electronic requests to participate in the survey through a secure website, followed by a printed survey if no response. Physicians with unknown email address were mailed printed surveys twice (Figure 1). The Colorado Multiple Institutional Review Board approved the study.
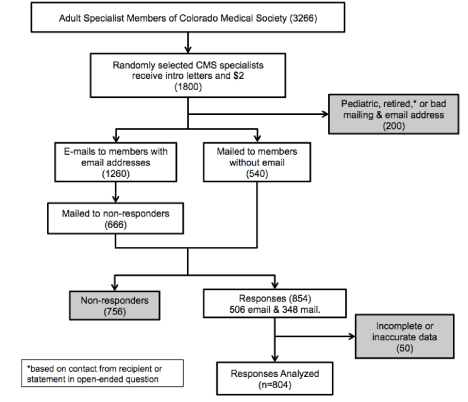
Figure 1: Survey Flowchart among Colorado Adult Medical Specialists, 2014.
From 29 specialties reported by participants,4 categories were grouped for analysis: medical specialties (e.g., endocrinology, cardiology, or neurology), hospital-based specialties (e.g., anesthesia, pathology or radiology), surgical specialties (e.g., general surgery, orthopedic surgery, or neurosurgery) and obstetrics/gynecology (OBGYN). OBGYN was kept separate due to specific patient demographics and large representation among survey respondents.
Survey development and content
In the absence of validated surveys addressing provider attitudes and beliefs about Medicaid patients, our team developed a survey using the Dillman tailored design method [15]. This methodology outlines fundamental research-based guidelines for survey development and implementation to maximize validity, reliability, and response rate. Survey development included multidisciplinary review by physicians of multiple specialties, public health professionals, and CMS leadership. Further survey refinement followed pilot survey response review, including open-ended responses from a group of specialty physicians. These procedures resulted in 14 characteristics (Figure 2) chosen to represent possible views of Medicaid patients, with some positive and some negative characteristics (consensually defined). Using a 5-point Likert-scale ranging from strongly disagree (-2) to strongly agree (+2), participants were asked to indicate whether each of the 14 characteristics described a “typical adult Medicaid patientattitude outcome.86% of r. Immediately following these ratings, a single open-ended question asked participants for additional thoughts regarding any issues addressed in the survey thus far. In a separate section of the survey, participants were asked to report on characteristics of themselves and their practices (9 items, Table 1).
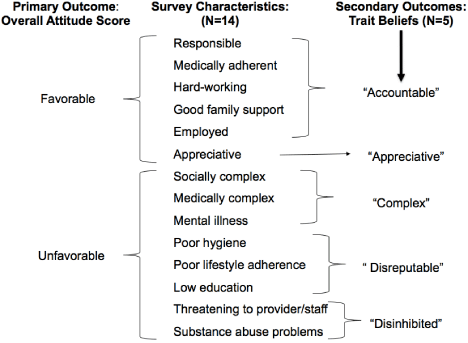
Figure 2: Relationship between 14 Perceived Characteristics for Medicaid Patients, from a Specialist Survey, and Primary and Secondary Analyzed Outcomes,
Colorado, 2014.
Overall Attitude
Characteristics†
Total
N=804
Favorable
n=113
Unfavorable
n=691
p-value*
Years in practice
<10 yrs
10-20 yrs
>20 yrs
155 (19.7)
255 (32.5)
374 (47.7)
23 (20.9)
23 (20.9)
64 (58.2)
132 (19.6)
232 (34.4)
310 (46.0)
0.016
Gender
Male
Female
597 (75.9)
190 (24.1)
81 (73.0)
30 (27.0)
516 (76.3)
160 (23.7)
0.44
Practice Setting
Urban
Suburban
Rural
305 (38.8)
379 (48.1)
103 (13.1)
40 (36.4)
61 (55.5)
9 (8.2)
265 (39.1)
318 (47.0)
94 (13.9)
0.14
Employer
Large organization employee
Independent practice
132 (18.2)
592 (81.7)
28 (27.7)
73 (72.3)
104 (16.7)
519 (83.3)
0.0077
Ownership Interest
Yes
No
579 (72.7)
218 (27.4)
77 (67.5)
37 (32.5)
502 (73.5)
26.5 (181)
0.19
Income Affected by Productivity
Little or no effect
Significant effect
Large or complete
102 (12.8)
183 (23.1)
507 (64.0)
24 (21.2)
22 (19.5)
67 (59.3)
78 (11.5)
161 (23.7)
440 (64.8)
0.015
Specialty Type‡
Hospital-based
Medical
Surgical
OBGYN
152 (19.7)
218 (28.2)
280 (36.2)
122 (28.7)
13 (12.3)
42 (39.6)
35 (33.0)
16 (15.1)
139 (20.9)
176 (26.4)
245 (36.8)
106 (15.9)
0.024
Avg Specialty Salary, by quartile
Bottom quartile
Lower middle quartile
Higher middle quartile
Top quartile
214 (27.7)
168 (21.7)
191 (24.7)
199 (25.7)
34 (32.1)
24 (22.6)
26 (24.5)
22 (20.8)
180 (27.0)
144 (21.6)
165 (24.8)
177 (26.6)
0.55
Medicaid patients in training
Many
Few or none
626 (80.5)
152 (19.5)
88 (78.6)
24 (21.4)
538 (80.8)
128 (19.2)
0.59
Notes: *P-value for chi-square test of proportion of favorable versus unfavorable attitude for each characteristic variable. † Race/ethnicity breakdown not included in analysis due to low number of non-Caucasian groups. ‡ Specialty type groupings were Hospital-based (anesthesiology, pathology, radiology), Medical (allergy/immunology, cardiology, dermatology, endocrinology, gastroenterology, hematology/oncology, infectious disease, nephrology, neurology, psychiatry, pulmonary/critical care, rheumatology, sports medicine), Surgical (colorectal surgery, general surgery, gynecologic oncology, neurosurgery, obstetrics/gynecology, oral/maxillofacial surgery, ophthalmology, orthopedic surgery, otolaryngology, plastic surgery, thoracic surgery, urology, vascular surgery) and OBGYN (obstetrics and gynecology).
Table 1: Adult Specialty Physician Survey Respondent Characteristics and Overall Attitude (%) about Medicaid Patients, Colorado, 2014.
Although the survey did not ask participants for income information, national data [16] were used to impute an average annual salary for each specialty. Each participant was then assigned a salary quartile based on their stated specialty.
Data analysis
The primary outcome was specialists’ overall attitude (general favorability or unfavorability) toward Medicaid patients. An attitude score was created for each participant by averaging his/her agreement with the 8 unfavorable characteristics and separately averaging agreement with the 6 favorable characteristics; the unfavorable average was then subtracted from the favorable average, such that higher scores indicated more favorable attitudes (possible range -4 to 4). Descriptive analytics were performed on this attitude score after dichotomizing to favorable (score >0) or unfavorable (score =0).
Chi-square test of proportions was used to test associations between dichotomized attitudes and physician and practice characteristics. Characteristics associated with a p-value =0.20 were retained for multivariable modeling. Backward elimination was used to select the most parsimonious multivariable logistic regression model [17]. All analyses were performed using SAS (SAS v9.3, SAS Institute, Cary, NC).
Secondary outcomes were specialists’ underlying trait beliefs about Medicaid patients. Although the 14 individual characteristics in our survey were intended to closely identify our participants’ views in different domains, our goal was to understand the foundational beliefs driving those answers. Exploratory factor analysis allows us to do this by determining the smallest number of factors that best describe the data. We used principal components analysis with varimax rotation, examining both eigenvalues (>1) and the interpretability of the factors for final selection. This approach revealed 13 of 14 characteristics fitting into four factors (Figure 2). Based on their content, we labeled them,“ accountableattitude outcome.86% of r (5 items), “complexattitude outcome.86% of r(3 items), “disreputableattitude outcome.86% of r (3 items), and“ disinhibitedattitude outcome.86% of r (2 items). The characteristic “appreciativeattitude outcome.86% of r did not align with any of the other four factors, and was kept as a fifth single item. After these five trait beliefs were identified, each participant was assigned a score for each one by calculating his/her average rating within that belief (e.g., Complex = [medical complexity + social complexity + mental health complexity ratings]/3). Descriptive analytics were performed after dichotomization to agree (score >0) versus disagree (score =0) on each trait belief. Chi-square test of proportions tested associations between dichotomized belief scores and physician and practice characteristics. For characteristics with a p-value =0.05, a referent category was selected and unadjusted logistic regression was performed to quantify differences between groups.
We examined participants’ responses to the open-ended question inviting them to further comment on the survey. These qualitative data were used to enrich or explain any unfavorable beliefs found in the quantitative results. For each of the five trait beliefs, we identified participants whose scores were clearly unfavorable (score over 1 in agreement with unfavorable beliefs, or ‹-1 with favorable beliefs) and used Atlas.ti (Atlas.ti v.7.5, GmbH, Berlin) to review their openended responses. Using codes created by an initial reviewer, a second reviewer (blinded to first reviewer’s coding) coded responses, and a third independent reviewer served as “tie-breakerattitude outcome.86% of r for discrepant coding between the first 2 reviewers.
Results and Discussion
Of the 1600 specialist physicians we attempted to recruit, 804 (50%) returned surveys with completed responses on key variables. Both non-responders and responders were 76% male and both groups’ average age was 53. As shown in Table 1, responders (participants) predominantly self-identified as white non-Hispanic (82%), in practice for ‹20 years (53%), and had ownership interest in their practices (72%). The majority of participants had some decisionmaking power around practice Medicaid acceptance (72%) and a majority reported accepting limited or no Medicaid patients (52%). Additional participant characteristics are shown in Table 1.
Attitude outcome
Analysis of overall attitude scores showed that 86% of participants had an unfavorable attitude toward Medicaid patients. Average characteristic scores showed agreement with 7 of 8 unfavorable characteristics (with exception of “threatening to provider or staffattitude outcome.86% of r), and disagreement with all 6 favorable characteristics describing Medicaid patients (Figure 3). Respondents most strongly agreed that Medicaid patients were socially complicated, medically complicated, and have poor adherence to lifestyle recommendations. Respondents most strongly disagree that Medicaid patients have strong family support.
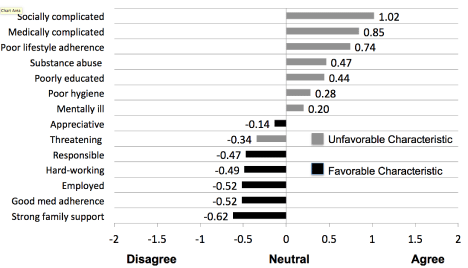
Figure 3: Average Respondent Agreement with Individual Characteristics of a “Typical Adult Medicaid Patientattitude outcome.86% of r.
Note that raw characteristic data is scored on a -2 to 2 scale, however the calculation for the primary attitude outcome (average score on favorable characteristics – average score on unfavorable characteristics) yields a -4 to 4 scale. For example, a respondent fully agreeing with all favorable characteristics (average=2) and fully disagreeing with all negative characteristics (average=-2), would have an attitude score of 2-(-2)=4.
Unadjusted analysis of the dichotomized attitude score revealed significant associations between an unfavorable (‹0) attitude score and 10-20 years in practice (p=0.02), independent solo or group practices (p‹0.01), level of income dependence on individual productivity (p=0.02), and specialty type (p=0.02) (Table 1). In multivariable analysis, associations remained between unfavorable attitudes and independent practice(p=0.03), income highly dependent on productivity (versus little/no dependence p=0.01; versus some dependence, p=0.07), and surgical or hospital-based versus medical specialty, (p=0.05 and p‹0.01, respectively). For these three practice characteristics, independently associated with unfavorable attitudes, Figure4 shows the proportion of participants with unfavorable attitudes in the multivariable analysis.

Figure 4: Percentage of specialty physicians with an unfavorable attitude
by employment, income and specialty type, in adjusted analysis, Colorado,
2014.
Beliefs outcome
Of the 5 beliefs, complex was most strongly endorsed (82%), followed by disreputable (69%), and accountable was most strongly rejected (74%). The beliefs that Medicaid patients are appreciative and disinhibited were more evenly distributed between endorsement and rejection (Figure 5).
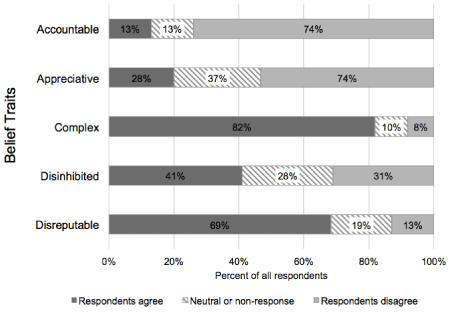
Figure 5: Distribution of adult specialty physician respondents’ agreement
with 5 belief traits describing Medicaid patients, Colorado, 2014.
Separate analyses tested physician and practice characteristics associated with each of the 5 beliefs. Chi-square tests found no significant difference in endorsement of any of the 5 beliefs by number of Medicaid patients seen daily, whether the specialist saw Medicaid patients during training, and whether the specialist has influence over the practice’s policy regarding Medicaid acceptance. A referent was chosen for independent variables found to be significantly associated with any of the 5 beliefs at p‹0.05. Odds ratios with confidence intervals for these significant associations are shown in Table 2. The most consistent associations were found with employment (specialists in independent practice were more likely to endorse disinhibited, and less likely to endorse accountable and appreciative) and specialty type (hospital-based and surgical specialists were more likely to endorse disinhibited, and less likely to endorse accountable and appreciative; surgical and OBGYN specialists were also more likely to endorse disreputable).
Unfavorable
Favorable
Sample Characteristics
(N=804)
Complex
Disreputable
Disinhibited
Accountable
Appreciative
Years in practice
<10 yrs
10-20 yrs
>20 yrs
1.1 (0.6,1.9)
Ref
0.7 (0.5,1.1)
0.8 (0.5,1.2)
Ref
1.1 (0.8,1.6)
1.0 (0.7,1.6)
Ref
0.9 (0.6,1.2)
0.8 (0.4,1.5)
Ref
1.3 (0.8,2.1)
1.6 (1.0,2.6)
Ref
1.6 (1.1,2.4)
Gender
Male
Female
Ref
1.9 (1.1,3.0)
Ref
0.9 (0.7,1.3)
Ref
0.9 (0.6,1.2)
Ref
1.1 (0.7,1.8)
Ref
1.2 (0.8,1.7)
Practice Setting
Urban
Suburban
Rural
Ref
1.0 (0.7,1.4)
1.4 (0.8,2.7)
Ref
0.9 (0.7,1.2)
1.9 (1.1,3.3)
Ref
0.8 (0.6,1.1)
1.3 (0.8,2.1)
Ref
0.9 (0.6,1.4)
0.8 (0.4,1.6)
Ref
0.9 (0.7,1.3)
0.6 (0.4,1.1)
Employer
Large organization
Independent practice
Ref
0.7 (0.4,1.2)
Ref
1.3 (0.9,2.0)
Ref
1.6 (1.1,2.5)
Ref
0.5 (0.3,0.8)
Ref
0.6 (0.4,1.0)
Ownership Interest
Yes
No
Ref
1.2 (0.8,1.7)
Ref
1.1 (0.8,1.5)
Ref
0.9 (0.7,1.3)
Ref
1.3 (0.8,2.0)
Ref
1.6 (1.2,2.3)
Income affected by productivity
Little or no effect
Significant effect
Large/complete effect
Ref
1.8 (1.0,3.3)
1.5 (0.9,2.4)
Ref
1.0 (0.6,1.7)
0.99 (0.6,1.6)
Ref
1.6 (0.9,2.6)
1.3 (0.8,2.0)
Ref
0.7 (0.4,1.4)
0.5 (0.3,0.8)
Ref
0.6 (0.3,1.0)
0.5 (0.3,0.8)
Specialty Type
Medical
Hospital-based
Surgical
OBGYN
Ref
0.7 (0.4,1.2)
0.6 (0.4,0.9)
1.2 (0.6,2.3)
Ref
1.4 (0.9,2.2)
1.6 (1.1,2.3)
2.0 (1.2,3.4)
Ref
2.1 (1.4,3.3)
1.9 (1.3,2.8)
1.9 (1.2,3.0)
Ref
0.4 (0.2,0.8)
0.6 (0.4,1.0)
0.9 (0.5,1.7)
Ref
0.3 (0.2,0.5)
0.5 (0.4,0.8)
0.9 (0.6,1.4)
Avg specialty salary, by quartile
Bottom quartile
2nd quartile
3rd quartile
Top quartile
Ref
0.7 (0.4,1.1)
0.8 (0.5,1.3)
0.7 (0.5,1.3)
Ref
1.0 (0.7,1.6)
1.1 (0.7,1.7)
1.2 (0.8,1.8)
Ref
1.1 (0.7,1.6)
1.4 (0.9,2.1)
1.4 (0.9,2.0)
Ref
1.1 (0.7,2.0)
0.5 (0.3,0.9)
0.7 (0.4,1.3)
Ref
0.7 (0.5,1.1)
0.5 (0.3,0.8)
0.7 (0.4,1.0)
Bold highlights variables with confidence intervals not crossing 1.
Table 2: Unadjusted Odds Ratios (CI) for Adult Specialty Physician Beliefs about Medicaid Patient by Physician and Practice Characteristics, Colorado, 2014.
Qualitative results
Open-ended comments were provided by 26% of the participants. There were 339 participants who strongly endorsed unfavorable beliefs (score>1) or strongly rejected favorable beliefs (score‹-1) about Medicaid patients. Of these, 29% (100) left comments (see Table 3 for examples by type of belief).Review of these comments showed that 37% used patient-blaming language, 35% used systemblaming language, and 38% specifically cited reimbursement problems. Examples of patient blaming language include “They are the toughest, most non-compliant, most litigious, least appreciative patient population.attitude outcome.86% of r Some comments (21%) were emotionally charged: “It is so simple and obvious. They are like coddled spoiled children who refuse to grow up, and their behavior is encouraged by the state. Why do you need a survey to tell you this? It is common sense.attitude outcome.86% of r
Trait Belief
Exemplary Quotes*
(not) Accountable
- “Scheduling is a nightmare, withfrequent no-shows.We commonly discharge them for noncomplianceand no- show rates. Even if the reimbursement was the same as Medicare rates, our practice would pass on care for them.attitude outcome.86% of r
- “they don't bring their copays!most have more financial support than they admitted - smoke/nice jewelry and clothes, etc. Fed/state pays better than working - why should they work? Many offer to pay cash - which, of course, we can't do (where do they get the money if they're indigent enough to be on Medicaid)attitude outcome.86% of r
(not) Appreciative
- “They are always asking for 'favors'… `difficult, self-entitled and threatening.attitude outcome.86% of r
- This population� is typically very demanding and tends to assume no…personal responsibility for care or consequences. They tend to be late, or miss appointments regularly. Quite simply, the medicaid patients� should be charged for their care so they assume responsibility for it. If something is free, you don't value it.attitude outcome.86% of r
Complex
- “I hope this survey is a sign of things to come - better care coordination; a central place we can call; improved mental health so that all these depressed, substance-abuse patients have a place to go; and a care manager they like....attitude outcome.86% of r
- “Medicaid patients are often very complicated medically, and have much fewer resources in terms of finances, social support. It makes a difficult situation extremely difficultattitude outcome.86% of r
Disinhibited
- “The only patients I have had steal from my office have been Medicaid patients. They berate and insult my staff if they don't get what they want. I get disability requests for trivial conditions. Even if reimbursement rises I would see very little b/c of these issues.attitude outcome.86% of r
- “I find that almost all of them want narcotics and have a history of opioid or other substance (ie, benzos) abuse. They are very unpleasant and can get really abusive verbally when you won't give them more narcotics which we should not have to put up with… a lot of these patients don't want to have a PCP because then their narcotics are monitored. They 'doctor shop' to get more drugs thinking that doctors don't communicate... They also don't want to get better oftentimes, and think that at age 25 they should be on permanent disability for something minor which is ridiculous. I don't know how they all became this entitled and drug addicted but it's awful and I refuse to play into it. Then they complain and we get written up.attitude outcome.86% of r
Disreputable
- “It is very difficult to care for patients who have no 'skin in the game'....who are noncompliant, feel entitled. Take much more time to care for due to numerous medical problems. Who often cause their problems by smoking, drinking, drugs, and ignoring recommendations? They are exhausting for doctors to care for, and the pay is terrible.attitude outcome.86% of r
- “The most difficult to take care of and the most unreliable and demanding. And litigious and unemployedattitude outcome.86% of r
*Quotes taken from sample of respondents with scores >1 in the unfavorable direction for stated belief trait. Italics authors’ emphasis – highlight themes recurring in qualitative data.
Table 3: Exemplary quotes among adult specialty physician respondents with unfavorable beliefs about Medicaid patients, Colorado, 2014.
Discussion
In this adult specialty physician survey, a vast majority of participants had unfavorable attitudes toward Medicaid patients, believing them to be complex, disreputable, disinhibited, unappreciative, and unaccountable.
Variability in specialty physician attitudes and beliefs about Medicaid patients is expected. However, this variability across specialties and practice cultures, in the presence of concomitant bias, may adversely affect quality or access. The culture of individual specialties and how physicians self-select into them may contribute to differential beliefs and attitudes. As medical students and trainees self-select, cultural and structural differences by specialty may promote certain behaviors and beliefs, with training and practice enhancing those differences. Beyond differences by specialty, we found systematic attitude and belief differences associated with employment type and income dependence on productivity.
Several studies have shown differences between Medicaid patient populations and other insured groups that may fuel this bias. Medicaid patients were less likely to follow through on specialty referrals [18] and more likely to miss appointments [19,20]. Individuals with Medicaid were typically of lower socioeconomic class, more medically complicated, more likely to have concomitant mental health diagnoses, and more likely to face barriers to health and healthcare access [21]. Population-level characteristics such as these might influence physicians’ views on Medicaid patients. Physicians may inappropriately generalize these population differences to all Medicaid patients, though our study cannot determine the presence of this behavior. Further, specific behavioral differences, such as missed appointments, may be generalized to negative underlying traits such as “irresponsibleattitude outcome.86% of r [22].
These results partially mirrored those of a prior survey of primary care physicians [23]. In that study, the primary care physicians identified high complexity of patient needs and limited patient acceptance of treatment options as barriers to providing care for Medicaid patients. Unfortunately, beyond these specific questions, no prior study has investigated physicians’ attitudes and beliefs about Medicaid patients. Nonetheless, a handful of studies indicated that physicians may have biases (overall negative attitudes) toward individuals with low socioeconomic status (SES), as reported by patients [24,25] or shown in assessments of physician attitudes [26- 29].
Although the subject of this study was Medicaid patients, research on other physician biases still may inform these findings. In this study, physician responses offered evidence of explicit (intentional or deliberate) negative attitudes and beliefs about patients who carry Medicaid insurance, a marker for low SES. Given the evidence on healthcare provider SES bias [24,27,30], Medicaid populations may experience quality of care problems, also similar to those found in provider racial bias studies. Evidence exists correlating physicianpatient relationships, clinical decision-making, patient adherence, and even patient symptoms with provider racial bias [4,28,31- 34]. Researchers are also increasingly looking at implicit bias because explicit racial or ethnic bias is very low among physicians [26,28,30,35]. It is significant that the current study revealed very strong explicit bias toward Medicaid patients, suggesting more explicit actions may follow.
Bias, based on Medicaid/SES, may limit specialty care access for patients. Insurance coverage increases have been encouraging; however, access gaps for Medicaid patients remain, due in part to many providers refusing to accept Medicaid in their practices. In 2011, before the ACA, 31% of office-based physicians declined new Medicaid patients [3], and many more practices accepted Medicaid in limited numbers. While federal regulations prohibit discrimination in provision of emergency healthcare, these laws have limited application to outpatient healthcare access. (Hill-Burton Act: Hospital Survey and Construction Act, 1946; Emergency Medical Treatment & Labor Act, 1986) Physicians with unfavorable attitudes and beliefs about Medicaid patients may choose not to accept Medicaid insurance in their practices, or not to advocate for acceptance with their clinic or institution administration. Reimbursement and system concerns may be the overt or stated reason for a practice to limit or deny Medicaid access and certainly contribute heavily [21,36-39], however physician attitudes and beliefs about Medicaid patients may contribute to limited practice acceptance and the widening specialty access gap, as supported in some provider statements found in Table 3.
This study focused on specialists not in primary care because of a dearth of research on bias in specialty care for Medicaid patients. Primary care providers cite lack of specialty care access as a problem and even a reason they limit Medicaid patient care [23,40]. Studies reveal early Medicaid expansion increased outpatient care demand with evidence that specialty care access fared worse than primary care access during this demand increase [41-46]. Despite this, existing research on Medicaid access problems is largely limited to the primary care setting, and does not substantially consider the role of bias [38,47-49].
Among the existing research on quality gaps between Medicaid and other insured patients, it is difficult to distinguish the causative factors. Studies of self-reported quality and satisfaction from Medicaid patients have varied results [14,50,51], however this is far from a comprehensive measure of quality of care. In cases where patients experienced stigma based on insurance status, this translated to experience of poor quality care, decreased access and changed patient behavior that affected the continuity of care considered foundational to good care [51]. Multiple studies have shown worse outcomes in Medicaid patients in surgical quality measures [52-54], quality indicators for patients receiving non-surgical medical treatment [55], as well as delayed diagnosis, under treatment and significantly worse survival for multiple types of cancer [56-61]. A portion of these outcomes can be attributed to socioeconomic determinants of health, however if treating providers harbor negative attitudes about patients, other factors may contribute to worse outcomes.
In recent years, a prominent national conversation has swelled around the sweeping effects of social bias in our society. Blaming specialists or physicians more generally for this unfavorable bias and the patient health ramifications will not change the reality. However, acknowledgement that a spectrum of bias exists among medical professionals is an important first step.
Understanding how bias affects population health must follow, starting with defining the connection between provider bias and the Medicaid access and quality gaps. Many unfavorable beliefs or perceptions identified in this study correlate directly to social determinants of health and barriers experienced primarily by those in lower SES classes. For example, Medicaid patients’ higher “no-show” rate is often due to barriers such as childcare and transportation problems [20]. Higher prevalence of diagnosed psychiatric disease is a barrier to medical adherence [21], especially when psychiatric disease is inadequately treated [62,63]. Supporting patients through system resources such as care coordinators, social workers, and mental health professionals could modify provider experience and perception, while improving the patient experience. Multidisciplinary approaches such as these will be essential in addressing the drivers of provider bias.
Limitations
Physicians self-report may not correlate perfectly with actual attitudes, beliefs or behavior. Our methods were designed to assess explicit (intentional or conscious) attitudes and beliefs only. Surveys on attitudes and beliefs are vulnerable to social favorability bias, although the presence of this bias would likely result in understating of our findings. Use of factor analysis requires the investigators to identify underlying belief patterns that may or may not reflect the respondents’ intent. Further research is merited into implicit (unintentional or unconscious) bias among specialists. Self-selection into CMS membership may result in limited generalizability to all specialists, due to sampling bias. However, the large CMS membership and absence of another accessible database of specialist physicians made this a unique resource. We considered the significant influence on practice policy reported by respondents as an asset given our broad interest in Medicaid specialty access. The attitude score reflects an intermediate outcome and future studies should look beyond attitudes and beliefs to provider willingness to care for Medicaid patients, actual proportion of patients seen, patient experiences, and both patient and provider outcomes. This survey was performed shortly after Medicaid expansion and views may change with more time post expansion. Finally, we acknowledge that respondents may have generalized endorsements to a class or socioeconomic bias, from which we are unable to separate bias specific just to Medicaid patients.
Conclusions
With broad Medicaid expansion, the healthcare system is challenged to provide comprehensive specialty care access and quality. The evolving national conversation around the role of Medicaid in our health system increases the need for clearer understanding of specialty physician beliefs and attitudes toward Medicaid and its insured population. In this first survey of the specialty workforce perspective on Medicaid patients, beliefs about those patients were notably negative. Future research is needed to determine whether these beliefs are associated with access and quality disparities for Medicaid patients in certain situations. Moving forward, acknowledging, addressing, and ultimately overcoming these negative attitudes and beliefs may be necessary for successful and equitable health care access through expanded Medicaid coverage.
Acknowledgements
The authors would like to thank the University of Colorado Primary Care Research Fellowship and participating fellows for their consistent support and contributions during study development and implementation.
References
- Medicaid & CHIP: April 2016 Monthly Applications, Eligibility Determinations and Enrollment Report. In: Services DoHaH, editor. Baltimore, MD: Centers For Medicare and Medicaid Services; 2016.
- Total Monthly Medicaid and CHIP Enrollment. 2016.
- Decker SL. In 2011 nearly one-third of physicians said they would not accept new Medicaid patients, but rising fees may help. Health Aff (Millwood). 2012; 31: 1673-1679.
- Paradies Y, Truong M, Priest N. A systematic review of the extent and measurement of healthcare provider racism. Journal of general internal medicine. 2014; 29: 364-387.
- Blair IV, Havranek EP, Price DW, Hanratty R, Fairclough DL, Farley T, et al. Assessment of biases against Latinos and African Americans among primary care providers and community members. American journal of public health. 2013; 103: 92-98.
- Sabin J, Nosek BA, Greenwald A, Rivara FP. Physicians' implicit and explicit attitudes about race by MD race, ethnicity, and gender. Journal of health care for the poor and underserved. 2009; 20: 896-913.
- Blair IV, Steiner JF, Fairclough DL, Hanratty R, Price DW, Hirsh HK, et al. Clinicians' implicit ethnic/racial bias and perceptions of care among Black and Latino patients. Annals of family medicine. 2013; 11: 43-52.
- Cooper LA, Roter DL, Carson KA, Beach MC, Sabin JA, Greenwald AG, et al. The associations of clinicians' implicit attitudes about race with medical visit communication and patient ratings of interpersonal care. American journal of public health. 2012; 102: 979-987.
- Penner LA, Dovidio JF, West TV, Gaertner SL, Albrecht TL, Dailey RK, et al. Aversive Racism and Medical Interactions with Black Patients: A Field Study. Journal of experimental social psychology. 2010; 46: 436-440.
- Stepanikova I. Racial-ethnic biases, time pressure, and medical decisions. Journal of health and social behavior. 2012; 53: 329-343.
- Green AR, Carney DR, Pallin DJ, Ngo LH, Raymond KL, Iezzoni LI, et al. Implicit bias among physicians and its prediction of thrombolysis decisions for black and white patients. Journal of general internal medicine. 2007; 22: 1231-1238.
- Sabin JA, Greenwald AG. The influence of implicit bias on treatment recommendations for 4 common pediatric conditions: pain, urinary tract infection, attention deficit hyperactivity disorder, and asthma. American journal of public health. 2012; 102: 988-995.
- Moskowitz GB, Stone J, Childs A. Implicit stereotyping and medical decisions: unconscious stereotype activation in practitioners' thoughts about African Americans. American journal of public health. 2012; 102: 996-1001.
- Nguyen KH, Sommers BD. Access and Quality of Care by Insurance Type for Low-Income Adults Before the Affordable Care Act. American journal of public health. 2016; 106: 1409-1415.
- Dillman DS J, Melani Christian L. Internet Mail and Mixed-Mode Surveys: The Tailored Design Method. Third ed. Hoboken, NJ: John Wiley and Sons, Inc; 2009.
- Medscape. Physician's Compensation Report: 2013. 2013.
- Hosmer DWL, Stanley Sturdivant, Rodney X. Applied logistic regression. 3rd ed. New Jersey: John Wiley & Sons; 2013.
- Forrest CB, Shadmi E, Nutting PA, Starfield B. Specialty referral completion among primary care patients: results from the ASPN Referral Study. Annals of family medicine. 2007; 5: 361-367.
- Calfee RP, Shah CM, Canham CD, Wong AH, Gelberman RH, Goldfarb CA. The influence of insurance status on access to and utilization of a tertiary hand surgery referral center. The Journal of bone and joint surgery American volume. 2012; 94: 2177-2184.
- Kaplan-Lewis E, Percac-Lima S. No-show to primary care appointments: why patients do not come. Journal of primary care & community health. 2013; 4: 251-255.
- Hahn Y. The effect of Medicaid physician fees on take-up of public health insurance among children in poverty. Journal of health economics. 2013; 32: 452-462.
- Hamilton DLS, JW Stereotypes. In: Wyer Jr. RSS, T.K., editor. Handbook of Social Cognition. 2. Hillsdale, NJ: Erlbaum; 1994.
- Long SK. Physicians may need more than higher reimbursements to expand medicaid participation: findings from Washington State. Health Aff (Millwood). 2013; 32: 1560-1567.
- Bird ST, Bogart LM. Perceived race-based and socioeconomic status (SES)- based discrimination in interactions with health care providers. Ethnicity & Disease. 2000; 11: 554-563.
- Ren XS, Amick BC, Williams DR. Racial/ethnic disparities in health: the interplay between discrimination and socioeconomic status. Ethnicity & disease. 1998; 9: 151-165.
- Haider AH, Schneider EB, Sriram N, Dossick DS, Scott VK, Swoboda SM, et al. Unconscious race and social class bias among acute care surgical clinicians and clinical treatment decisions. JAMA surgery. 2015; 150: 457- 464.
- Williams RL, Romney C, Kano M, Wright R, Skipper B, Getrich CM, et al. Racial, gender, and socioeconomic status bias in senior medical student clinical decision-making: a national survey. Journal of general internal medicine. 2015; 30: 758-767.
- Chapman EN, Kaatz A, Carnes M. Physicians and implicit bias: how doctors may unwittingly perpetuate health care disparities. Journal of general internal medicine. 2013; 28: 1504-1510.
- van Ryn M, Burke J. The effect of patient race and socio-economic status on physicians' perceptions of patients. Social science & medicine. 2000; 50: 813-828.
- Haider AH, Schneider EB, Sriram N, Scott VK, Swoboda SM, Zogg CK, et al. Unconscious Race and Class Biases among Registered Nurses: Vignette- Based Study Using Implicit Association Testing. Journal of the American College of Surgeons. 2015; 220: 1077-1086.e3.
- Bird ST, Bogart LM, Delahanty DL. Health-related correlates of perceived discrimination in HIV care. AIDS patient care and STDs. 2004; 18: 19-26.
- Burgess DJ, Grill J, Noorbaloochi S, Griffin JM, Ricards J, van Ryn M, et al. The effect of perceived racial discrimination on bodily pain among older African American men. Pain medicine (Malden, Mass). 2009; 10: 1341-1352.
- Haywood C, Jr., Lanzkron S, Bediako S, Strouse JJ, Haythornthwaite J, Carroll CP, et al. Perceived Discrimination, Patient Trust, and Adherence to Medical Recommendations Among Persons with Sickle Cell Disease. Journal of general internal medicine. 2014; 29: 1657-1662.
- Lutfey K. Evaluating sources and implications of doctor bias. Medical education. 2013; 47: 756-758.
- Shavers VL, Fagan P, Jones D, Klein WM, Boyington J, Moten C, et al. The state of research on racial/ethnic discrimination in the receipt of health care. American journal of public health. 2012; 102: 953-966.
- Cunningham PJ, O'Malley AS. Do reimbursement delays discourage Medicaid participation by physicians? Health Aff (Millwood). 2009; 28: w17-28.
- Long SH, Settle RF, Stuart BC. Reimbursement and access to physicians' services under Medicaid. Journal of health economics. 1986; 5: 236-251.
- Polsky D, Richards M, Basseyn S, Wissoker D, Kenney GM, Zuckerman S, et al. Appointment Availability after Increases in Medicaid Payments for Primary Care. The New England journal of medicine. 2015.
- https://www.ncbi.nlm.nih.gov/pubmed/22566429
- Rhodes KV, Bisgaier J, Lawson CC, Soglin D, Krug S, Van Haitsma M. "Patients who can't get an appointment go to the ER": access to specialty care for publicly insured children. Annals of emergency medicine. 2013; 61: 394-403.
- Gold R, Bailey SR, O'Malley JP, Hoopes MJ, Cowburn S, Marino M, et al. Estimating Demand for Care After a Medicaid Expansion: Lessons From Oregon. The Journal of ambulatory care management. 2014; 37: 282-292.
- https://www.ncbi.nlm.nih.gov/pubmed/23293397
- Center for Medicaid & CHIP. Medicaid & CHIP: October 2014 Monthly Applications, Eligibility Determinations and Enrollment Report. In: Services DoHaH, editor. December, 2014.
- Thompson JW. Findings from the Arkansas Medicaid Expansion Using Premium Assistance (the "Private Option"). Academy Health Annual Research Meeting; June 27, 2016; Boston, MA. 2016.
- Anandasivam NS, Wiznia DH, Kim CY, Save AV, Grauer JN, Pelker RR. Access of Patients With Lumbar Disc Herniations to Spine Surgeons: The Effect of Insurance Type Under the Affordable Care Act. Spine. 2017; 42: 1179-1183.
- Tipirneni R, Rhodes KV, Hayward RA, Lichtenstein RL, Reamer EN, Davis MM. Primary care appointment availability for new Medicaid patients increased after Medicaid expansion in Michigan. Health Aff (Millwood). 2015; 34: 1399-406.
- Decker SL. Two-thirds of primary care physicians accepted new Medicaid patients in 2011-12: a baseline to measure future acceptance rates. Health Aff (Millwood). 2013; 32: 1183-1187.
- Adams EK, Bronstein JM, Florence CS. The impact of Medicaid primary care case management on office-based physician supply in Alabama and Georgia. Inquiry: a journal of medical care organization, provision and financing. 2003; 40: 269-282.
- The Kaiser Commision on Medicaid and the Uninsured. Increasing Medicaid Primary Care Fees for Certain Physicians in 2013 and 2014: A Primer on the Health Reform Provision and Final Rule. Henry J Kaiser Family Foundation; 2012.
- Riffkin R. Americans With Government Health Plans Most Satisfied. Gallup; Nov 6, 2015.
- Martinez-Hume AC, Baker AM, Bell HS, Montemayor I, Elwell K, Hunt LM. "They Treat you a Different Way:" Public Insurance, Stigma, and the Challenge to Quality Health Care. Culture, medicine and psychiatry. 2016; 41: 161-180.
- Sawhney JS, Stephen AH, Nunez H, Lueckel SN, Kheirbek T, Adams CA, Jr., et al. Impact of Type of Health Insurance on Infection Rates among Young Trauma Patients. Surgical infections. 2016; 17: 541-546.
- Swenson CW, Kamdar NS, Levy H, Campbell DA, Jr., Morgan DM. Insurance Type and Major Complications After Hysterectomy. Female pelvic medicine & reconstructive surgery. 2017; 23: 39-43.
- Tanenbaum JE, Alentado VJ, Miller JA, Lubelski D, Benzel EC, Mroz TE. Association between insurance status and patient safety in the lumbar spine fusion population. The spine journal: official journal of the North American Spine Society. 2017; 17: 338-345.
- Cifaldi M, Renaud J, Ganguli A, Halpern MT. Disparities in care by insurance status for individuals with rheumatoid arthritis: analysis of the medical expenditure panel survey, 2006-2009. Current medical research and opinion. 2016; 32: 2029-2037.
- Wang J, Ha J, Lopez A, Bhuket T, Liu B, Wong RJ. Medicaid and Uninsured Hepatocellular Carcinoma Patients Have More Advanced Tumor Stage and Are Less Likely to Receive Treatment. Journal of clinical gastroenterology. 2018; 52: 437-443.
- Amini A, Rusthoven CG, Waxweiler TV, Jones BL, Fisher CM, Karam SD, et al. Association of health insurance with outcomes in adults ages 18 to 64 years with melanoma in the United States. Journal of the American Academy of Dermatology. 2016; 74: 309-316.
- Fossati N, Nguyen DP, Trinh QD, Sammon J, Sood A, Larcher A, et al. The Impact of Insurance Status on Tumor Characteristics and Treatment Selection in Contemporary Patients With Prostate Cancer. Journal of the National Comprehensive Cancer Network: JNCCN. 2015; 13: 1351-1358.
- Inverso G, Mahal BA, Aizer AA, Donoff RB, Chuang SK. Health Insurance Affects Head and Neck Cancer Treatment Patterns and Outcomes. Journal of oral and maxillofacial surgery: official journal of the American Association of Oral and Maxillofacial Surgeons. 2016; 74: 1241-1247.
- https://www.ncbi.nlm.nih.gov/pubmed/27500561
- Comey J. Hard Truths: Law Enforcement and Race 2015 [Georgetown University Commencement Speech].
- Bauer LK, Caro MA, Beach SR, Mastromauro CA, Lenihan E, Januzzi JL, et al. Effects of depression and anxiety improvement on adherence to medication and health behaviors in recently hospitalized cardiac patients. The American journal of cardiology. 2012; 109: 1266-1271.
- Paradise HT, Berlowitz DR, Ozonoff A, Miller DR, Hylek EM, Ash AS, et al. Outcomes of anticoagulation therapy in patients with mental health conditions. Journal of general internal medicine. 2014; 29: 855-861.
