Abstract
Primary care physicians manage a large portion of skin-related encounters, and scabies is an exceptionally common disease of the skin. It is highly likely that primary care physicians will encounter a patient with scabies in their clinic. For this reason, we provide a review of the scabies mite, the clinical presentation of human infestation, and the methods available for diagnosis and treatment of the disease.
pKeywords: Scabies; Sarcoptes Scabiei; Crusted Scabies; ; PermethrinIntroduction
One in three Americans are affected by skin disease at any given time [1]. Approximately half of skin complaints (52.9%) are initially evaluated by non-dermatologist providers. Family medicine practitioners manage 20.5% of all skin-related encounters, and 6.0- 8.0% of all outpatient visits for primary care physicians are skin complaints [1-3]. With an estimated prevalence of 200 million individuals worldwide, scabies is an exceptionally common skin disease [4]. Thus, it is vital for primary care physicians to be able to effectively diagnose and treat the condition. In our review, we discuss the scabies mite, the clinical presentation of human infestation, and the methods available for diagnosis and treatment of the disease.
The scabies mite: Scabies, caused by the mite Sarcoptes scabiei var. hominis, has plagued humanity for thousands of years and continues to do so despite the development of effective pharmacologic interventions [5,6]. The scabies mite is an unbiased pestilence that afflicts both men and women regardless of age, ethnicity, or socioeconomic status [7,8]. As obligate parasites, the mites undergo their entire life cycle on their human hosts [9]. They burrow into the skin at the level of the stratum corneum to feed on human tissue and deposit their eggs [9,10]. An allergic reaction occurs as the human immune system encounters components of the mite’s saliva, eggs, and feces [11]. This hypersensitivity reaction creates the classic clinical presentation of severe, generalized pruritus with a nocturnal predominance [12].
The scabies mite has a round, translucent body with protruding jaws and four pairs of brown legs [8,13]. The female mite, barely visible to the human eye at 0.3x0.5mm, is larger than the male [5]. All scabies mites require a host for survival. Once the mite inhabits a new host, it crawls along the skin before flattening its body to initiate penetration [14]. Using proteolytic secretions, the mite dissolves and consumes tissue to propel itself forward at a rate of 0.5 to 5.0 mm per day just beneath the stratum corneum [9,14]. As it tunnels, the mite creates a serpiginous burrow in the stratum corneum that is pathognomonic for the diagnosis of scabies. Unfortunately for clinicians, these burrows are rarely visible to the naked eye unless they are surrounded by significant inflammation or darkened by components of the mite or its waste [10].
The life of a female mite spans roughly four to six weeks [9]. Within hours of penetrating her host, the female lays her eggs at a rate of 2-4 eggs per day [9,13]. Two to four days later, her larvae hatch and move along the surface of the skin until they seek shelter and sustenance by burrowing into the skin in new areas [9,13]. Ten to fourteen days after hatching, the larvae develop into adult mites [5]. The adult mites are capable of surviving and remaining infective in isolation for 24 to 36 hours at standard room conditions (21°C and 40 to 80% relative humidity) before succumbing to desiccation [14]. In order to inhabit a new host, the mite must crawl to its victim attracted by both heat and odor as guiding stimuli [15].
Scabies is primarily transmitted by direct skin-to-skin contact through contact with infested individuals. It is commonly spread to sexual partners and throughout families or friends living in close proximity. Individuals attending or residing in institutional settings such as schools, prisons, and nursing homes are most commonly exposed, as close contact is unavoidable [5,6,16,17]. Since scabies mites can survive and remain infective for up to 36 hours, fomites can play a role in indirect transmission [14,15]. These fomites include bedding, clothing, furniture, and carpeting, albeit they play a much smaller role than direct contact with a host [6,18].
Clinical Presentation
Scabies patients classically report widespread, intense pruritus especially at night. They may also have a history of immunosuppression, residency in an institutional setting, or close contact with another pruritic individual [8,19]. Patients may be infested for up to 4-8 weeks before mounting an inflammatory response to mite antigens. This response leads to itching, and many patients are pruritic for an extended period of time before the appearance of skin lesions [13,20]. In subsequent infestations, the host is already sensitized, and symptoms may appear within one to two days [13].
When they appear, common primary lesions include papules, vesicles, pustules, and nodules [17] (Figure 1). Non-specific secondary lesions including excoriations (Figure 2), eczematous eruptions, and secondary bacterial infections (e.g. impetigo due to Streptococcus or Staphylococcus) are also commonly seen [5,11,16,17].
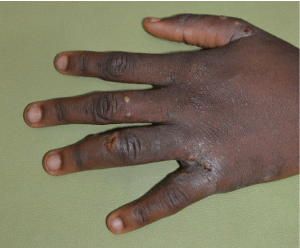
Figure 1: Typical scabies lesions (i.e. papules and vesicles with secondary
excoriation) in the interdigital web spaces in a male patient.
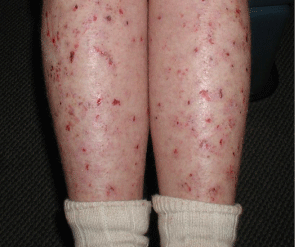
Figure 2: Excoriations as secondary lesions in a patient infested with scabies.
The papulovesicular variant with associated secondary lesions is the most common presentation [21]. Often, family members or anyone who lives with the affected patient are also infested (Figure 3a, 3b, 3c, and 3d). The papules are erythematous, domed lesions varying from 1-5 mm in size [21]. These lesions may be accompanied by burrows, scaly grey or erythematous curvilinear lines measuring 3-15 mm in length [17,21]. These burrows are pathognomonic but may be destroyed by scratching or go undetected by the unaided eye [10,22,23]. In adults, the lesions are often bilaterally symmetrical, usually sparing the face and head [8,17]. Typical locations include the finger webs, flexor surfaces of the wrists and elbows, anterior axilla, and abdominal areas within and surrounding the umbilicus [12]. The skin in these flexural areas is more easily penetrated by the burrowing mites. Areolar lesions are commonly observed in women, and penile and scrotal lesions are commonly seen in men [12,17]. In contrast, lesions in children are typically found on the face, scalp, palms and soles in addition to the trunk and extremities and may be accompanied by generalized eczema [17]. The nodular variant is less common and presents with firm, elevated papules and nodules temporally ranging in color from red to dark brown (Figure 4) [21,24]. These lesions are most commonly seen in the axilla and groin as well as on the male genitalia and may represent penetration of scabies mites into the dermis (Figure 5) [25]. These lesions may persist for up to a year following successful eradication of the active infestation [21,24].
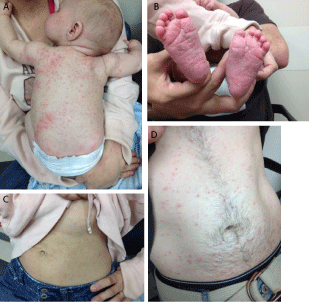
Figure 3: Papulovesicular eruptions of scabies on back (a), feet (b), and
abdomens (c and d) of a child, mother, and father.

Figure 4: This patient with widespread pruritus gradually worsening over 6
months has dozens of papules and nodules over his penis and medial thighs.
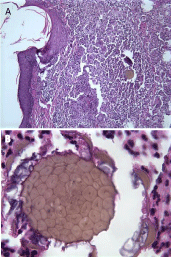
Figure 5: A scabies mite is noted within the center of an inflammatory nodule
in this punch biopsy specimen from the scrotum. Used with permission from
Tesner B, Williams NO, Brodell RT. The pathophysiologic basis of scabietic
nodules. J Am Acad Dermatol. 57: S56-57.
Norwegian scabies, more properly referred to as “crusted scabies,” is a variant that occurs in individuals in varying states of immunocompromise as well as in individuals with neurological conditions that render them physically incapacitated or intellectually disabled [17]. It is characterized by hyperkeratotic, psoriasiform lesions. Thick, crusted whitish-yellow plaques and erythematous scales can appear anywhere on the body, but the predominant sites are the hands, face, neck, scalp, and trunk (Figure 6) [5,11,21]. Pruritus may be mild, and the mite load may exceed one million [5,8]. This is in stark contrast to the intense pruritus and average mite load of twelve seen in classic scabies [17].
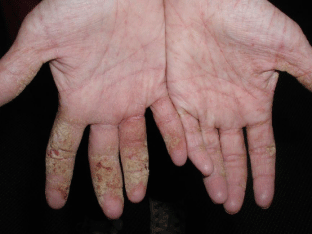
Figure 6: Thick, crusted, scaling patches with background erythema is
noted in this elderly nursing home patient who was found to have crusted
(Norwegian) scabies.
Diagnosis
Clinical suspicion of scabies should be raised in any patient with intense pruritus and a positive history of close contact with another pruritic individual [11].While many support a practical approach based on clinical suspicion and experience, absolute confirmation of the diagnosis requires the identification of the mite, of its eggs or feces, or of the ever-elusive yet pathognomonic burrow. Classic methods of screening and diagnosis include skin scraping, epidermal shave biopsy, the adhesive tape test, the burrow ink test, and dermoscopy. It is not uncommon for some of these methods to be combined when diagnosis is suspected yet difficult to achieve [8,10-12,22,23,26,27].
Skin scraping is performed by first applying mineral oil to one of the flexural regions where papular and papulovesicular lesions or burrows are present. Next, the oiled epidermis is scraped laterally and repetitively traditionally using a #15 scalpel blade. A 3mm disposable curette may be used as a substitute for the scalpel in pediatric settings in order to reduce fear of the procedure and thus increase tolerance (Figure 7) [28]. The contents of the burrow are now immersed in the oil, which is applied to a slide and cover-slipped before being examined under a light microscope. The goal is to identify the mite, its eggs, or its scybala (feces) (Figure 8). Potassium hydroxide preparations should be avoided as this chemical may dissolve the scybala. Skin scraping is extremely specific, but it is not highly sensitive. It is not always well tolerated by children due to the uncomfortable collection process [8,10,23]. For this reason, it may be more practical to test a pruritic adult close contact of the affected child.
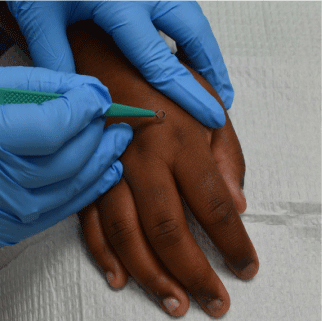
Figure 7: A curette (pictured) or a #15 blade can be used to collect a
specimen for scabies preparation from an involved area.
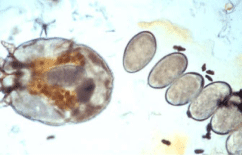
Figure 8: A scabies mite with her eggs and scybala visualized in this oil prep.
Used with permission from Harbor ID, Casamiquela K, Helms SE. Chapter
2: The Scabies Preparation in Tips and Tricks in Procedural Dermatology:
Efficient and Effective Approaches to Achieving Optimal Diagnostic and
Therapeutic Results. Editor-in-Chief: RT Brodell, Associate Eds: SE. Helms,
J Schulmeier, M Cosulich, AC Bhatia, W Abromovits, JD Jackson, JayPee
Publishers. 2019.
Epidermal shave biopsy is performed by identifying a likely site of infestation, grasping the region between the thumb and forefinger, and removing the uppermost layers of skin with a scalpel. The removed sample is then examined under the microscope with the same goal previously described for skin scraping. Epidermal shave biopsy confers multiple advantages over skin scraping. It allows for the visualization of mite fragments and excrement that are otherwise destroyed by vigorous scraping, and it improves the overall percentage of positive findings. When performed correctly, this precise removal of skin is more tolerable to the patient than the abrading nature of the skin scraping procedure. Additionally, the risk of laceration is less than that of skin scraping, as the blade is parallel rather than perpendicular to the skin. While this method can be technically advantageous in comparison to skin scraping, it shares the statistical pattern of a high specificity with a relatively low sensitivity [23,26].
Adhesive tape Test is performed by placing adhesive tape over pruritic regions. Due to persistent excoriation, mite residues are often scratched to the skin’s surface. The tape adheres to these residues and any live mites migrating along the epidermis. The tape is then examined under a microscope. The advantage to this method is its practicality and lack of discomfort during the procedure. It is inexpensive and requires little to no training to perform. It has a slightly higher sensitivity than skin scraping with an equal specificity. For all of these reasons, it is an excellent screening tool in resourcepoor settings [23].
Burrow ink test is performed by rubbing ink over suspected areas of infestation which then tracks down into the burrow. The ink on the surface of the skin is then removed with alcohol. A positive test reveals a dark, serpiginous path where the ink has found its way down into the burrow (Figure 9). This test serves as an excellent precursor for other tests such as skin scraping or shave biopsy. Once the burrow has been visualized, the clinician now has a high yield region in which to search for definitive evidence of infestation [22].
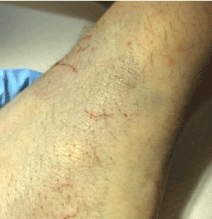
Figure 9: The burrow “magically” appears after ink is applied and wiped off
with an alcohol swab. After application of mineral oil, scraping using a #15
blade until the burrow is no longer visible should ensure that any contents of
the burrow are in the oil to be examined under the microscope. Photo courtesy
of Ira D. Harber, MD and Adam C. Byrd, MD, University of Mississippi Medical
Center, Jackson, MS.
Dermoscopy is performed using a hand-held dermatoscope at 10x magnification to identify mites or burrows. At higher magnifications, a clinician may also identify mite scybala and eggs. Burrows appear as erythematous, inflamed or whitish, scaly curvilinear structures. The mite is identified as a gray, triangular structure that corresponds to the anterior segment of the mite. This is commonly referred to as the ‘delta wing’ or ‘delta glider’ sign. When the ‘delta wing’ is visualized within a well-defined burrow, it is referred to as a ‘jetliner with its trail’ (Figure 10).

Figure 10: Dermatoscopic view of scabies showing the classic “delta wing”
sign. Photo courtesy of Rodolfo A. Trujillo, MD, University of Mississippi
Medical Center, Jackson, MS.
One disadvantage of dermoscopy is that it requires training to perform effectively. Another is that the classic findings may be difficult to visualize on darkly pigmented skin [12,23,27].
Other evolving diagnostic approaches include a PCR-based method that allows for the serologic detection of scabies. This method may prove useful when scabies is suspected but cannot be proven by the conventional methods described above [29,30]. Additionally, an enzyme-linked immunosorbent assay (ELISA) has been developed for the serologic detection of scabies antibodies in pigs [31].
Differential Diagnosis: Scabies presents in many forms (ie papulovesicular, nodular, crusted) and may mimic a variety of dermatologic diseases [32]. Unless one has identified the mite, its eggs, its scybala, or its burrows, all diseases associated with pruritus or ambiguous skin lesions must be considered [33]. The probability of certain diseases within your differential diagnosis will vary according to the patient’s age and demographics. The diagnoses most commonly considered in the differential diagnosis for scabies are listed in Table 1.
Atopic Dermatitis [11,19,28,32,33,43]
Contact Dermatitis [28,32,33,43]
Dermatitis Herpetiformis [19,28,32,33,43]
Eczema [11,32,43]
Other Insect Bites/Infections [19,28,33,43]
Urticaria Pigmentosa [11,19,39,43]
Pyoderma [11,33,43]
Psoriasis [11,19,32,43]
Bullous Pemphigoid [11,19,32,33,39]
Secondary Syphilis [19,32,43]
Pityriasis Rosea [28,32,43]
Prurigo Nodularis [28,43]
Tinea [11,19]
Darier’s Disease [32,43]
Senile Pruritus [39]
Langerhans Cell Histiocytosis [11,19,39,43]
Cutaneous Lymphoma [19,32,39]
Table 1: Differential Diagnoses in Scabies.
Treatment: Topical permethrin and oral ivermectin are the standard first line options for the treatment of scabies.34 However, ivermectin is not FDA approved for the treatment of scabies [35]. Second line therapies may be viewed in Table 2 [8,16,33,34,36-38]. Patients should be educated on the proper administration of therapy as well as warned about the post-treatment course of the disease. It can take as long as four to six weeks for the signs and symptoms of scabies to resolve as the allergic reaction may linger following successful eradication of the mite [16].
Medication
Dosage
Administration
Effectiveness
Comments
Permethrin
5% Cream
Day 1 and Day 8, rinsed off after 8-14 hours Shortened 2 hour application in Pregnancy
Most Effective Topical Therapy
- Safe and Well-tolerated
- Safe in Pregnancy
- Not for use in breast feeding women or children <2 months old
Ivermectin
200 μg/kg/dose
Day 1 and Day 7
Highly Effective Oral Therapy
- Excellent patient compliance
- Useful for mass treatment in institutional settings and treatment of close contacts
- Not for use in Pregnancy, Breast feeding, or children <15kg
Benzyl Benzoate
10% or 25% Lotion
One application rinsed off after 24 hours
Shortened to 12 hour application in Pregnancy
Effective
- Not commercially available in the United States
- Safe in pregnancy
- Inexpensive
Lindane
1% Cream or Lotion
Day 1 and Day 8, rinsed off after 6––-8 hours
Poor, Resistance common
- Due to potential for CNS toxicity, only for use when patient cannot tolerate or has failed other agents
- Not for use in pregnancy, breast feeding, or infants
- Inexpensive
Precipitated Sulfur
2––-10% Precipitate in Petroleum Base
Days 1-3 with 24-hour applications and baths between each successive application.
Questionable Efficacy
- Safe for use in pregnancy, breast feeding, and infants Inexpensive
- Messy, malodorous, and may stain bedding and clothing
Crotamiton
10% Cream
Day 1 and Day 2 rinsed off after 24 hours and then reapplied
Poor
- May have anti-pruritic benefits
- Inexpensive
*Table Sources Used: [8,16,33,34,36-38].
Table 2: Medications utilized to Treat Scabies.
Permethrin is a synthetic pyrethrin that disrupts the neurologic cell membranes of the mites and results in their paralysis and eventual death. It is considered to be the most effective topical option for the treatment of scabies [37]. A 5% formulation of permethrin is applied over the entire body from neck to toes in adults and should include the head and neck in infants. The cream is left for 8-14 hours and is then removed by bathing. Although one application is typically sufficient, another application eight days later is advised to ensure complete eradication [33,34,38]. Permethrin has minimal percutaneous absorption. Thus, it is generally well tolerated with the potential for a mild, local irritation of the skin. No major adverse effects are reported with its use [34,38]. However, those with a formaldehyde allergy should be cautioned that the cream contains 0.1% formaldehyde as a preservative. Application in these individuals may result in contact dermatitis [33,39]. Permethrin is safe for use in anyone over the age of two months, and it can be used in pregnancy (formerly Category B) with a shortened 2-hour application [33,34,39]. Due to its potential for excretion in breast milk, it is not recommended for use in nursing mothers [38]. Ivermectin is a commonly used anti-helminthic agent that blocks neurotransmission in the mites and results in paralysis and death. When used to treat scabies ivermectin is administered orally at 200μg/kg/dose and is commercially available as 3mg and 6mg tablets. It is taken twice for typical cases of scabies with a one-week interval between the doses [33,34,38]. Ivermectin does not cross a fully developed blood-brain barrier in humans. For this reason, it has a low side effect profile [33,38]. Minor side effects such as abdominal pain, anorexia, fatigue, nausea, vomiting, diarrhea, constipation, dizziness, pruritus, and conjunctivitis have been reported, but it is generally well tolerated [38]. Severe side effects have been reported in the treatment of filiariasis. In this setting the occurrence of fever, tachycardia, hypotension, edema, and arthralgias are thought to represent an allergic reaction to the dying parasite [38]. It is not for use in children weighing less than 15kg or pregnant and breastfeeding women as it has the potential to cross an incompletely developed blood-brain barrier [33]. Ivermectin is less cost effective than permethrin, but its advantage is related to ease of administration [36]. In patients who are unwilling or unable to apply topical solutions, ivermectin is an excellent choice of therapy [18,36]. It is particularly useful in institutional settings for treating many infested patients and their close contacts.
Crusted “Norwegian” scabies is treated with a combination of topical permethrin and oral ivermectin. A 5% formulation of permethrin is applied every 2-3 days for 1 to 2 weeks. Oral ivermectin is administered in three doses, five doses, or seven doses according to the severity of the infection. For mild Norwegian scabies, 200μg/kg/ dose of ivermectin is given on days 1, 2, and 8. For moderate infection, it is given on days 1, 2, 8, 9, and 15. Lastly, for the most severe cases, it is administered on days 1, 2, 8, 9, 15, 22, and 29 [40].
In a Cochrane review comparing these two first-line therapies, clearance rates were nearly identical at two and four weeks of treatment. After four weeks, ivermectin was associated with a slightly larger proportion of patients with at least one adverse event, however adverse events were rarely reported with either treatment option [41]. Treatment of Close Contacts: Many experts advise the empiric treatment of close contacts [5,16-8,32,33,36,39,42,43]. Other clinicians believe that, while treating all close contacts would be ideal, this fails to take into account the significant cost of both time and financial resources that this places on families [28]. In addition, ethical and professional dilemmas are inherent in the exposure of patients to potential side effects without first examining them in the clinic [18]. Wolf et al acknowledge the desire of some physicians to practice defensive medicine, but argue that treatment of close contacts is important nonetheless [18]. Their reasons include the high likelihood of spread to close contacts, the risk for reinfestation posed by allowing close contacts to harbor mites, the low side effect profiles of current therapies, and the fact that many other contagious diseases (i.e. sexually transmitted infections) are also treated with the prophylactic management of asymptomatic contacts.
Managing Fomites: In order to reduce the risk of reinfestation, all bedding, clothing, and towels encountered by the infested individual should be properly laundered. When possible, these items should be decontaminated by machine wash at least 60°C, machine dried using a heat cycle or dry cleaned. If this is not possible, items should be stored in a bag for ten days to ensure that no mites remain [5,33,43].
Population Health: Mass administration of ivermectin can significantly reduce the prevalence of scabies and impetigo in a population. A recent trial in which the population (26,188 people) of the Choiseul Province in the Solomon Islands was treated with ivermectin for scabies and impetigo as well as azithromycin for trachoma yielded an 88% relative reduction in prevalence of scabies and a 74% relative reduction in prevalence of impetigo. Their data supports the mass administration of ivermectin-based therapies in populations where scabies is considered a public health priority [44].
References
- Wilmer EN, Gustafson CJ, Ahn CS, Davis SA, Feldman SR, Huang WW. Most common dermatologic conditions encountered by dermatologists and nondermatologists. Cutis. 2014; 94: 285-292.
- Awadalla F, Rosenbaum DA, Camacho F, Fleischer AB, Feldman SR. Dermatologic disease in family medicine. Fam Med. 2008; 40: 507-511.
- Lowell BA, Froelich CW, Federman DG, Kirsner RS. Dermatology in primary care: prevalence and patient disposition. J Am Acad Dermatol. 2001; 45: 250- 255.
- World Health Organization. Neglected tropical diseases: scabies. 2019.
- Chosidow O. Scabies and pediculosis. Lancet. 2000; 355: 819-826.
- Arlian LG, Estes SA, Vyszenski-Moher DL. Prevalence of Sarcoptes scabiei in the homes and nursing homes of scabietic patients. J Am Acad Dermatol. 1988; 19: 806-811.
- Orkin M. Scabies: what’s new? Curr Probl Dermatol. 1995; 22: 105-111.
- Chosidow O. Scabies. N Engl J Med. 2006; 354: 1718-1727.
- Mellanby K. Biology of the parasite. In: Orkin M, Maibach H, eds. Cutaneous Infestations and Insect Bites. 1st ed. New York: CRC Press. 1985: 9-18.
- Arlian LG. Biology, host relations, and epidemiology of Sarcoptes scabiei. Annu Rev Entomol. 1989; 34: 139-161.
- Heukelbach J, Feldmeier H. Scabies. Lancet. 2006; 367: 1767-1774.
- Prins C, Stucki L, French L, Saurat J-H, Braun RP. Dermoscopy for the in vivo detection of sarcoptes scabiei. Dermatology. 2004; 208: 241-243.
- Mellanby K. Scabies in 1976. R Soc Health J. 1977; 97: 32-36.
- Arlian LG, Runyan RA, Achar S, Estes SA. Survival and infectivity of Sarcoptes scabiei var. canis and var. hominis. J Am Acad Dermatol. 1984; 11: 210-215.
- Arlian LG, Runyan RA, Sorlie LB, Estes SA. Host-seeking behavior of Sarcoptes scabiei. J Am Acad Dermatol. 1984; 11: 594-598.
- Orkin M, Epstein E, Maibach HI. Treatment of today’s scabies and pediculosis. JAMA. 1976; 236: 1136-1139.
- Johnston G, Sladden M. Scabies: diagnosis and treatment. BMJ. 2005; 331: 619-622.
- Wolf R, Davidovici B. Treatment of scabies and pediculosis: Facts and controversies. Clin Dermatol. 2010; 28: 511-518.
- Rosamilia LL. Scabies. Semin Cutan Med Surg. 2014; 33: 106-109.
- Hejazi N, Mehregan AH. Scabies: histological study of inflammatory lesions. Arch Dermatol. 1975; 111: 37-39.
- Fernandez N, Torres A, Ackerman AB. Pathologic findings in human scabies. Arch Dermatol. 1977; 113: 320-324.
- Woodley D, Saurat JH. The Burrow Ink Test and the scabies mite. J Am Acad Dermatol. 1981; 4: 715-722.
- Walter B, Heukelbach J, Fengler G, Worth C, Hengge U, Feldmeier H. Comparison of dermoscopy, skin scraping, and the adhesive tape test for the diagnosis of scabies in a resource-poor setting. Arch Dermatol. 2011; 147: 468-473.
- Orkin M. Today’s scabies. Arch Dermatol. 1975; 111: 1431-1432.
- Tesner B, Williams N, Brodell RT. Pathophysiologic basis of scabietic nodules. J Am Acad Dermatol. 2007; 57: S56-57.
- Martin WE, Wheeler CE. Diagnosis of human scabies by epidermal shave biopsy. J Am Acad Dermatol. 1979; 1: 335-337.
- Johr R, Stolz W. Dermoscopy from A to Z. In: Dermoscopy: An Illustrated Self-Assessment Guide. 2nd ed. China: McGraw-Hill Education. 2015: 23-24.
- Jacks SK, Lewis EA, Witman PM. The curette prep: a modification of the traditional scabies preparation. Pediatr Dermatol. 2012; 29: 544-545.
- Bezold G, Lange M, Schiener R, Palmedo G, Sander CA, Kerscher M, et al. Hidden scabies: diagnosis by polymerase chain reaction. Br J Dermatol. 2001; 144: 614-618.
- Delaunay P, Hérissé AL, Hasseine L, Chiaverini C, Tran A, Mary C, et al. Scabies PCR with standardized dry swab sampling Easy tool for cluster diagnosis of human scabies. Br J Dermatol. 2019.
- van der Heijden HM, Rambags PG, Elbers AR, van Maanen C, Hunneman WA. Validation of ELISAs for the detection of antibodies to Sarcoptes scabiei in pigs. Vet Parasitol. 2000; 89: 95-107.
- Chouela E, Abeldaño A, Pellerano G, Hernández MI. Diagnosis and treatment of scabies: a practical guide. Am J Clin Dermatol. 2002; 3: 9-18.
- Meinking T, Burkhart C, Burkhart C, Elgart G. Infestations. In: Bolognia J, Jorizzo J, Rapini R, eds. Dermatology. 2nd ed. Philadelphia: Elsevier. 2008; 1291-1295.
- Rasmussen J. Antiparasitic agents. In: Wolverton S, ed. Comprehensive Dermatologic Drug Therapy. United States: Saunders. 2001; 537-546.
- Scabies: Medications. Centers for Disease Control and Prevention. 2019.
- Monsel G, Chosidow O. Management of scabies. Skin Therapy Lett. 2012; 17: 1-4.
- Strong M, Johnstone P. Interventions for treating scabies. Cochrane Database Syst Rev. 2007; CD000320.
- Feldman S, Phelps K, Verzino K. Antiparasitics. In: Handbook of Dermatologic Drug Therapy. United Kingdom: Taylor & Francis Group. 2005: 161-166.
- Hicks MI, Elston DM. Scabies. Dermatol Ther. 2009; 22: 279-292.
- Currie BJ, McCarthy JS. Permethrin and Ivermectin for Scabies. N Engl J Med. 2010; 362: 717-725.
- Rosumeck S, Nast A, Dressler C. Evaluation of ivermectin vs permethrin for treating scabies - summary of a Cochrane review. JAMA dermatology. 2019; 155: 730-732.
- Chambliss ML. Treating asymptomatic bodily contacts of patients with scabies. Arch Fam Med. 2000; 9: 473-474.
- Fitzpatrick TB, Johnson RA, Wolff K, Polano MK, Suurmond D. Scabies. In: Fitzpatrick TB, Johnson RA, Wolff K, Polano MK, Suurmond D, eds. Color Atlas and Synopsis of Clinical Dermatology Common and Serious Diseases. 3rd ed. United States: McGraw-Hill. 1997: 842-849.
- Romani L, Marks M, Sokana O, Nasi T, Wand H, Cordell B, et al. Efficacy of mass drug administration with ivermectin for control of scabies and impetigo, with coadministration of azithromycin: a single-arm community intervention trial. Lancet Infect Dis. 2019; 19: 510-518.
