Abstract
Eagle syndrome is characterized by the compression of adjacent anatomical neck blood vessels and nerves due to the elongation of the styloid process or calcified stylohyoid ligament. This compressive effect leads to non-specific symptoms ranging from otalgia, dysphagia, hoarseness, Horner’s syndrome, cervicofacial neuralgia, syncope, and in extreme cases, transient ischemic attack or ischemic stroke. Here, we present the case of a patient with hypertension, morbid obesity, and hyperlipidemia who presented to the hospital with sudden onset weakness of the right side of the body with ipsilateral facial paresthesia consistent with transient ischemic attack versus ischemic stroke picture. Neurovascular imaging however established the diagnosis of vascular variant of Eagle syndrome. Although several cases of Eagle syndrome have been documented by other specialties, our documentation is the first reported in the family medicine literature. This case report offers insight about a rarely encountered condition among family medicine physicians and particularly underscores the effectiveness of conservative management.
Keywords: Vascular variant of Eagle syndrome; Transient ischemic attack (TIA); Presyncopal episodes; Elongated styloid process; Case report
Case Presentation
A 59-year-old male with a history of hypertension, morbid obesity, and hyperlipidemia presented to the hospital complaining of weakness on the right side of body with ipsilateral facial paresthesia of three days duration. Three days prior to presentation, patient was outdoors tending his garden when he suddenly noticed decreased strength on his right body, first in the right leg, then to his right arm. This episode lasted for a few minutes and was associated with ipsilateral facial paresthesia (shock-wave sensation), gait imbalance, near syncope, and dizziness. While symptoms of gait imbalance, dizziness, and near syncope have since resolved, his right-side weakness and facial paresthesia have persisted. There is no prior report of similar symptoms except for episodic headaches, which resolved with Tylenol. He has been non-compliant with his anti-hypertensive medications-skips doses and only takes them when he feels “unwell” or develops a headache. In addition, he recently started Hydroxycut supplement, which he took the morning the symptoms manifested. He otherwise denied speech deficit, nausea, vomiting, seizure, altered consciousness, fever, chills, diaphoresis, chest pain, visual changes, dysphagia, recent surgery, or illicit drug use.
Vital signs on admission were unremarkable except for elevated blood pressure of 165/88 (temp: 98, pulse rate: 79, respiratory rate: 18 with 99% saturation on room air). Physical examination showed an obese (BMI: 39.1), middle-aged male, not acutely distressed. Patient was alert and oriented to time, place, and person. Head, ear, nose, and throat; pulmonary; cardiovascular; and abdominal examinations were unremarkable. No tenderness or palpable mass in the tonsillar fossa. Comprehensive neurologic bedside exam showed normal except for decreased light touch sensation on the right side of face with right-side dysmetria on finger–nose coordination. National Institute of Health Stroke Scale (NIHSS) was 2 for decreased sensation on the right side of the body and one extremity ataxia.
Complete blood count and metabolic panel; thyroid panel; troponin; urinalysis; Vitamin B12; homocysteine; antinuclear antibody; urine drug and alcohol level screen were all unremarkable. EKG showed normal sinus rhythm, chest X-ray was normal, and transthoracic echo with bubble study showed an ejection fraction of 55%–59% with severe concentric left ventricular hypertrophy and mildly dilated left atrium, but without thrombus or patent foramen ovale. Neuroimaging with head computerized tomography (CT) showed no acute cortical infarction or acute intracranial hemorrhage. However, mild diffuse cerebral volume loss and mild chronic microvascular ischemic changes were noted. Finding was consistent with brain MRI w/o contrast report. Head and neck CT angiogram further showed no significant stenosis but did reveal a 5 x 6 x 9 mm (AP X TV X CC) outpouching along the anterior wall of left cervical internal carotid artery (ICA) with elongated left styloid process. The left styloid process measured approximately 4cm.
Imaging
TIA symptoms usually don't last more than 24 hours. However, with his carotid outpouching, this creates an area that can lead to persistent symptoms without an actual stroke. In the absence of overt infarct on imaging, treatment for transient ischemic attack (TIA) with high-dose aspirin and statin was initiated. Upon further review of neuroimaging studies with the neurology team, the Eagle syndrome diagnosis was made. Given no imminent risk for vascular injury and based on patient’s treatment preference, conservative management was started. Analgesic (Tylenol for mild pain, tramadol for moderate pain, and morphine for severe pain) with tapered dose of gabapentin (300mg tid x 1 month, then 300mg bid x1 week, and then 300mg po daily x 1 week) and structured physical therapy were instituted. To prevent future ischemic events in the setting of ICA pseudoaneurysm, aspirin and high-intensity statin were continued, and his home blood pressure regimen of amlodipine 10mg daily and lisinopril 10mg daily resumed. After 4 days of treatment with normal neurologic examination (NIHSS=0) and no report of symptoms recurrence, the patient was deemed stable for discharge. At 2-week and 1-month follow-ups, patient denied any equilibrium loss, hemiplegia, or paresthesia. However, during his 3-month follow-up with neurology, he reported intermittent radicular pain in the right upper extremity. Cervical spine MRI showed mild C4 and C5 cervical spondylosis, but no significant foraminal stenosis or signs of cord compression. Given recurrence of symptoms, he was referred for diagnostic cerebral angiogram and neurosurgery for left styloidectomy.
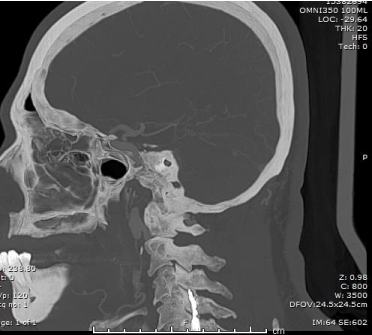
Figure 1: Sagittal view of head and neck CT angiogram showing left cervical
internal carotid artery (ICA) outpouching.
Discussion
The styloid process is a pointed piece of bone located bilaterally below the ears measuring less than 3.2cm in most adults [3,6,8]. It projects anteriorly and inferiorly from the inferior surface of the temporal bone and anchors to several muscles and ligaments of the tongue and larynx, including the stylohyoid muscle and ligament, styloglossus, stylomandibular, and stylopharyngeus muscles. Anatomically, the styloid process and stylohyoid ligament are bounded by the internal carotid and internal jugular vein within the carotid sheath, external carotid artery, and cranial nerves III, V, VII, VIII, IX, X, and XII. The elongation or ossification of the styloid bone or stylohyoid ligament can be unilateral or bilateral. While the exact etiology of Eagle syndrome remains unclear, some authors have hypothesized that congenital ossification or inflammatory proliferative changes occurring post styloid fracture or tonsillectomy may be responsible for these anatomical changes [5]. The first case of Eagle syndrome was documented in 1937 by Dr. Watt Eagle, an otorhinolaryngologist, and since then, additional cases have been reported by varied specialties, including neuroradiologists, oral-maxillofacial surgeons, and otolaryngologists. Our report is the first to be documented in a family medicine journal.
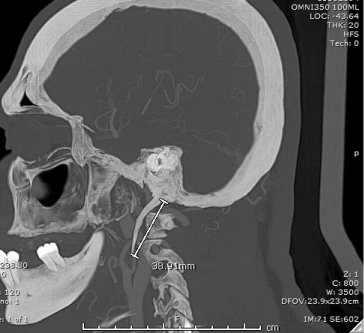
Figure 2a: Sagittal view of head and neck CT angiogram showing elongated
left styloid process (~4cm) as it runs beneath the ipsilateral ICA outpouching.
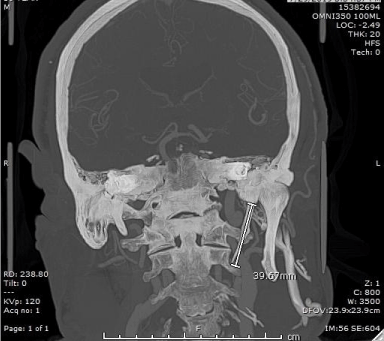
Figure 2b: Coronal view of head and neck CTA showing elongated left styloid
process (~4cm).
Although rare, Eagle syndrome is becoming a notable differential for syncope, TIA, or stroke of unclear etiology [3,8]. Of those incidentally noted to have an elongated styloid process or ossified stylohyoid ligament, only a small percentage (0.16%) become symptomatic and are diagnosed with Eagle syndrome [4], with cases being more predominant among women aged 30 to 50 years old and those with risk factors, including prior history of tonsillectomy or neck trauma. Two variants of Eagle syndrome exist: classic and vascular (carotid). The classic type presents with neuropathic symptoms as a result of cranial nerve (III, V, VII, VIII, IX, X, and XII) compression or overstimulation, whereas the vascular type affects the ICA, external carotid artery (ECA), and internal jugular vein (IJV). The vascular type is considered more dangerous, debilitating, and difficult to diagnose without vascular imaging. Although not clinically proven, one can assume the risk for injury to surrounding structures increases with the length, anatomical positioning, duration of occlusion, or extent of stimulation by the styloid bone or calcified stylohyoid ligament. With occlusion of the internal or external carotid artery, syncope, dizziness, aphasia, hemiparesis, ophthalmoplegia, and in extreme cases, TIA or stroke can result. Similarly, cervical nerve compression or overstimulation can lead to tinnitus, dysphagia, and loss of taste sensation, Horner’s syndrome, Bell's palsy, parietal headache, facial pain, or neuralgia. Given the non-specific symptoms and the similarity in presentation with other medical conditions-such as giant cell arteritis, temporo-mandibular jaw pain, glossopharyngeal neuralgia, psychosomatic disorder, or cervical spine degenerative arthritis [1-8] obtaining a detailed history and performing a comprehensive physical examination is warranted by the clinician.
Clinical histories that suggest Eagle syndrome include rapid onset of neurological symptoms that are often aggravated by sudden head motions. Physical examination with a focus on the central nervous system, head, neck, and oropharynx is imperative. Palpation of the tonsillar fossa of the neck and examination of the oropharynx to check for tenderness and to locate bony prominence or bulge [4] may be helpful. Bony prominence may sometimes not be appreciable, as seen in our presented case. Irrespective of these findings, if suspicion for Eagle syndrome remains high, then anterior–posterior, lateral, or panoramic view X-rays should be initially ordered. For clinicians practicing in low-resource settings or community health centers, this is a cost-effective imaging to diagnose this condition. Particularly in the case of vascular Eagle syndrome and to guide treatment modality, obtaining CT angiogram studies of the head and neck or color doppler flow imaging is important to assess vascular flow, presence of vascular insults, thrombus, outpouching, or narrowing [3,6].
The key to managing this condition relies on first identifying patients with imminent risk for vascular compromise or those who are hemodynamically unstable. If hemodynamically stable, conservative medical management, although not definitive, should be tried while planning elective surgical treatment with styloidectomy. In the case of our patient, treatment with analgesics (Tylenol, Naprosyn, tramadol), antidepressants (amitriptyline), neuralgic medications (gabapentin), and therapy-focused physical therapy led to significant clinical improvement and symptom resolution. Other studies have also reported good outcomes with analgesics (Tylenol, Naprosyn, tramadol), antidepressants (amitriptyline), neuralgic medications (gabapentin), therapy-focused physical therapy, and use of image-guided trans-oral steroids or local anesthetic injection [1,2]. Further, shared decision-making between the patient and interdisciplinary medical team (including neurology, neurosurgery and oral maxillofacial surgery) should be facilitated.
There is no substantial evidence about the length of the styloid process that should be managed with a surgical approach. In literature, styloidectomy was performed at lengths of 3 and 5.5cm. Nonetheless, the treatment decision relies on multiple factors, including the patient’s clinical status, patient preference, and a benefit versus risk assessment. In patients whose symptoms persist or remain unamenable to conservative management or show evidence of hemodynamic instability or risk for imminent vascular injury, total or partial styloidectomy is considered the mainstay treatment [3,8-10].
Conclusion
Vascular variant Eagle syndrome, although rare, presents with an aggregate of non-specific symptoms that mimics varied other conditions and has become a notable differential for syncope, TIA, or stroke of unidentified etiology. Appropriate diagnosis of this condition using detailed history and physical examination complemented with imaging studies is imperative for prompt treatment. This report provides perspective on the diagnosis and treatment of a condition that is rarely seen and managed by family medicine providers.
Acknowledgement
Many thanks to Dr Thomas Northrup and Dr Jude Des bordes for assistance with content edit and review, Dr Rajan Patel and Dr Maria Olga Patino, Department of Diagnostic and Interventional Radiology for assistance with image review and extraction.
References
- Han MK, Kim DW, Yang JY. Non surgical treatment of Eagle's syndrome – a case report. Korean J Pain. 2013; 26: 169–172.
- Wong ML, Rossi MD, Groff W, Castro S, Powell J. Physical therapy management of a patient with Eagle syndrome. Physiother Theory Pract. 2011; 27: 319–327.
- Aldakkan A, Dunn M, Warsi NM, Mansouri A, Marotta TR. Vascular Eagle’s syndrome: two cases illustrating distinct mechanisms of cerebral ischemia. J. Radiol. Case Rep. 2017; 11: 1–7.
- Murtagh RD, Caracciolo JT, Fernandez G. CT findings associated with Eagle syndrome. Am. J. Neuroradiol. 2001; 22: 1401–1402.
- Zhang FL, Zhou HW, Guo ZN, Yang Y. Eagle syndrome as a cause of cerebral venous sinus thrombosis. Can. J. Neurol. Sci. 2019; 46: 344–345.
- Li Z, Hua Y, Yang J, Li J. Ultrasound evaluation of transient ischemic attack caused by styloid process elongation: a case report. Front Neurol. 2019; 10: 26.
- Thoenissen P, Bittermann G, Schmelzeisen R, Oshima T, Fretwurst T. Eagle's syndrome-a non-perceived differential diagnosis of temporomandibular disorder. Int J Surg Case Rep. 2015; 15: 123–126.
- Demirtas H, Kayan M, Koyuncuoglu HR, Çelik AO, Kara M, Sengeze N. Eagle syndrome causing vascular compression with cervical rotation: case report. Pol J Radiol. 2016; 81: 277–280.
- Kapoor V, Jindal G, Garg S. Eagle's syndrome: a new surgical technique for styloidectomy. J Maxillofac Oral Surg. 2015; 14: 360–365.
- Constantinides F, Vidoni G, Bodin C, Di Lenarda R. Eagle’s syndrome: signs and symptoms. Cranio. 2013; 1: 56–60.
