Abstract
Background: It is estimated that over 1/3 of the world’s population and 18% of the US population is deficient in vitamin D. Currently, Healthcare Practitioners’ (HCPs) vitamin D testing and recommending beliefs and behaviors are poorly understood. This study aims to evaluate beliefs and practice regarding vitamin D among U.S. HCPs with an interest in nutrition, specifically assessing impact of Integrative Medicine (IM) fellowship training on these practice beliefs and behaviors.
Methods: An Internet-based 62-item survey was electronically provided to HCPs identified through the Andrew Weil Center for Integrative Medicine database that includes non-Fellows and Fellows of IM.
Results: Of 3,984 recipients of the survey, a total of 361 (9.1%) completed the survey. Of respondents, 221 (61.2%) completed an IM Fellowship. The vast majority of respondents (332, 93.5%) believe that vitamin D deficiency is widespread and affects the majority of the population. Three of four HCPs indicate that vitamin D status can be accurately assessed by measuring serum 25-hydroxyvitamin D (262; 74%), and that vitamin D supplementation improves overall health of patients (277; 77.4%). Most respondents, especially those with fellowship training in integrative medicine, both test and recommend vitamin D3 (cholecalciferol) for various chronic conditions and in at-risk populations.
Conclusions: There is widespread understanding of the role of vitamin D in health maintenance and in specific health conditions. Overall, primary care, physician-level training, length of time in practice, and IM fellowship training are the most significant predictors of beliefs and practices regarding vitamin D.
Keywords: Dietary supplements; Integrative medicine; Risk assessment; Surveys and questionnaires; Vitamin D; Vitamin D deficiency
Abbreviations
IM: Integrative Medicine; FIM: Fellowship in Integrative Medicine; HCP: Healthcare Practitioner; 25OHD: 25-Hydroxy- Cholecalciferol
Introduction
Vitamin D deficiency is a global health issue, designated in the US as a “nutrient of public health concern,” by the 2015 U.S. Dietary Guidelines [1]. In the US, 40% of the population has a blood concentration of 25-hydroxyvitamin D (25(OH)D) less than 30ng/mL indicating Vitamin D insufficiency [2]. Data from the 2014 NHANES report found that 18% of the U.S. population over the age of 1 year of age had 25(OH)D levels less than 20ng/mL and 5% had levels below 12 ng/mL [3]. Widespread use of sunscreens, reduced time spent outdoors, and diets with minimal consumption of vitamin-D rich foods contribute to vitamin D deficiency and insufficiency in the general population. Vitamin D deficiency is more common in individuals with dark skin pigmentation, young children (especially under age 2y), obesity, the elderly (over 70y), and institutionalized individuals [4,5,6]. Trends in vitamin D prescribing have changed significantly since the 2011 Institute of Medicine (IOM) recommendations increased the safe upper limit of vitamin D3 supplementation for people over 9y, from 2000IU (50mcg) to 4000IU (100mcg) daily [7]. This recommendation was largely based on evidence supporting the benefits of vitamin D for bone health and fracture risk reduction [8,9,10]. Vitamin D, a fat-soluble vitamin, has hormone-like pleotropic effects [11], influencing mineral homeostasis and bone metabolism [12], cell proliferation [13], immunity [14], adiposity [15], and inflammatory responses [16]. There appears to be no association between vitamin D status or supplementation and all-cause mortality [17], or cardiovascular events [18,19], Vitamin D supplementation has been associated with a 16% reduced risk of cancer death [20], While a cancer preventive effect is not yet established [21,22]. Vitamin D status may be inversely correlated with depression risk [23], although supplementation does not appear to attenuate the risk of depression [24]. Vitamin D deficiency may be associated with autoimmune disease severity [25]. Vitamin D deficiency is 35% higher in obese individuals, 24% higher in overweight individuals [26], and is implicated in poor glycemic control in people with type 2 diabetes [27] and metabolic syndrome [28]. Major medical societies have issued guidelines regarding testing and supplementation of vitamin D. In 2011, the IOM established a recommended daily allowance of 600IU (15mcg) vitamin D3, needed to sustain serum 25(OH)D above 20ng/mL (50nmol/L) and 4000IU (100mcg) per day as the safe UL for vitamin D intake [29]. This estimate has been criticized as insufficient due to various methodological errors used in the IOM analysis [30]. The American Academy of Family Physicians (AAFP) guidelines recommend against routine screening, citing variability in the sensitivity and reliability of vitamin D testing. The AAFP guidelines recommend against vitamin D supplementation in the general population noting lack of clinical trial evidence documenting that correction of vitamin D deficiency results in a reduced risk of cancer, mortaility diabetes type 2, or fractures in high-risk individuals [31]. The 2021 US Preventive Services Task Force recommendation is that there is insufficient evidence to determine the benefits and harms of screening for vitamin D deficiency in asymptomatic adults [32]. In contrast, the US Endocrine Society recommends vitamin D screening in individuals at risk and supplementation for those deficient in vitamin D (serum 25(OH)D </= 20ng/mL) and those with insufficient vitamin D (serum 25(OH)D between 21-29ng/mL) in order to achieve vitamin D sufficiency at 30ng/mL (75nmol/L). The US Endocrine Society sets the safe UL as 4000IU (100mcg) daily for children and 10,000IU (250mcg) daily for adults [33]. Underlying the divergence of these guidelines are challenges with vitamin D testing and the establishment of vitamin D cutoff values. There is established inaccuracy (10-15% coefficient of variation and bias as high as 30%) in vitamin D assays that rely upon immunoassay methodology [34]. Alternatively, LC-MS/MS testing may provide greater accuracy, but utilizes complex methodology, is also subject to error [35]. There is also concern that the serum 25(OH)D level does not necessarily correlate with tissue stores, is not the most accurate measure of vitamin D in individuals with dark skin pigmentation, nor represents levels sufficient for optimal physiology. Finally, there appears to be a U-shaped curve related to vitamin D with both lower and higher levels associated with increased risks of cardiovascular disease, vascular calcification, falls, frailty, and all-cause mortality [36,37]. Despite the presence of guidelines regarding vitamin D testing and prescribing, and likely due to confusion between guidelines, surveys suggest that vitamin D testing and recommending practices among physicians are inconsistent [38,39], There are limited surveys for vitamin D recommending practices and none exist among physicians with fellowship level training in Integrative Medicine (FIM), presumably a group highly aware of the evidence regarding vitamin D testing and supplementation.
Materials and Methods
This study set out to determine most common beliefs and testing and recommending practices regarding vitamin D and among healthcare practitioners with an interest in nutrition. The impact of integrative medicine training will be assessed by comparing respondents who have completed an IM fellowship to respondents who have expressed interest in IM fellowships, but have not enrolled in such. The predictive value of other factors, namely practitioner type, time in practice and the nature of practice on vitamin D beliefs and practices will also be assessed.
Questionnaire
This cross-sectional study was based on results from an Internetbased 62-item survey (see Table 2) developed by study investigators and reviewed by Center faculty. The survey included 5 sections: practice beliefs, practice behaviors, testing and recommending practices for specific diseases, and frequency of recommending common vitamin D dosages. Background characteristics (credentials, years in practice, practice type, community setting, and age) were also obtained. The practice belief scale included 8 items regarding the prevalence and criteria of vitamin deficiency, accuracy of testing, impact of vitamin D on bone density, premature mortality, and risks of high vitamin D levels. The practice behaviors scale included 11 items related to general testing, indications for recommending vitamin D, monitoring vitamin D recommendations, and type of vitamin D recommendations. All items were answered with Yes, No or I Don’t Know.
Participants
The survey was electronically provided through Qualtrics to non-Fellows and Fellows of Integrative Medicine (FIM) practitioners identified through the University of Arizona Andrew Weil Center for Integrative Medicine (AWCIM) database. Participants were offered $175 towards an AWCIM online educational offering upon completion of the survey. Enrollment goals were 200 FIM alumni and 100 HCPs who had not started the IM fellowship curriculum or had not yet progressed to curriculum containing information about nutrition and dietary supplements. All responses were de identified for analysis.
Statistical analysis
Descriptive statistics are presented for all survey items. Chisquare tests were conducted to examine differences in practice characteristics between the IM-trained vs. non-IM trained groups. To investigate the associations between IM-training and practice belief/behaviors, multinomial logistic regression models were used to predict practice beliefs and behaviors items. The response category ‘yes’ was used as the reference category for each question and the response categories “no” and “don’t know” were analyzed against the reference. The relevant predictors included in the models were MD credential, 15 years in medical practice, primary care, solo practice, and academic as the covariates to be controlled for, in addition to the main predictor of interest-IM trained vs. non-IM trained groups. Age was not included as it was strongly correlated with years in practice. Analyses were conducted using IBM®SPSS® Statistics Desktop V26.0 (Armonk, New York).
Results
Sample
Out of 3,984, a total of 361 (9.1%) completed the survey. Survey participant characteristics are presented in Table 1. Practice Characteristics by IM trained vs. non-IM trained. Statistically significant differences indicated FIM trained respondents were more likely to have MD/DO credentials (86% vs. 72%), be in practice over 15 years (62% vs. 44%), be a solo practitioner (28% vs. 13%), be over 50 years old (52% vs. 31%), and less likely to practice in academic settings (19% vs. 26%). There was a trend (p=0.054) for FIM respondents to be in primary care practice (65% vs. 55%).
Characteristic
Not completed IM Training N=140
IM Trained N=221
Total
Sig
N
%
N
%
N
%
Credentials
0.002
MD/DO
101
72%
190
86%
291
81%
Other non-MD/DO
39
28%
31
14%
70
19%
Years in Practice
0.001
Less than 15 years
79
56%
83
38%
162
45%
over 15 years
61
44%
137
62%
198
55%
Current practice type*
Hospital
36
26%
44
20%
80
22%
0.196
Multi-practitioner Clinic
82
59%
112
51%
194
54%
0.143
Solo Practitioner
18
13%
62
28%
80
22%
<0.001
Academic
35
25%
34
15%
69
19%
0.024
Do not have a clinical practice
5
4%
11
5%
16
4%
0.527
Type of community served*
Rural
40
29%
71
32%
111
31%
0.476
Urban
98
70%
151
68%
249
69%
0.738
Underserved
44
31%
62
28%
106
29%
0.493
Concierge
12
9%
19
9%
31
9%
0.993
Pediatric only
18
13%
16
7%
34
9%
0.075
Geriatric only
0
0%
1
0%
1
0%
0.425
Age
0.001
Under 30
9
6.50%
0
0.00%
9
3%
30 – 50
86
62.30%
105
47.70%
191
53%
Over 50
43
31.20%
115
52.30%
158
44%
Primary Care
0.054
Specialist includes Pediatrics
63
45%
77
35%
140
39%
Primary Care
77
55%
144
65%
221
61%
Table 1: Practice Characteristics by IM trained vs. non-IM trained.
Practice beliefs, practice behaviors, and dosing
The practice beliefs and behaviors of all participants is summarized in Table 2. Practice Belief & Practice Frequencies. The vast majority of respondents believe that vitamin D deficiency is widespread, affecting the majority of the population (n=332; 93.5%), that vitamin D status can be accurately assessed by measuring serum 25(OH)D (n=262; 74%), and that vitamin D supplementation improves the overall health of patients (n=277; 77.4%). HCPs recognize that serum 25(OH) D less than 20ng/mL (50nmol/L) is indicative of vitamin D deficiency (n=318; 90.1%); however, 239 (67.5%) also indicated that serum 25(OH)D less than 30ng/mL (75nmol/L) is indicative of deficiency. More than half (n=210; 59.3%) feel that vitamin D supplementation lowers the risk of premature mortality and only 65 (18.5%) feel that serum vitamin D levels greater than 50 ng/mL (50nmol/L) may have adverse health effects.
Practice Beliefs
Response
N
%
Vitamin D deficiency is widespread, affecting the majority of the population
Yes
332
93.50%
No
14
3.90%
Don't Know
9
2.50%
Vitamin D status is accurately assessed by measuring serum 25(OH) vitamin D level
Yes
262
74.00%
No
62
17.50%
Don't Know
30
8.50%
Monotherapy with Vitamin D is effective for improving bone density
Yes
70
19.90%
No
246
70.10%
Don't Know
35
10.00%
Vitamin D supplementation is only effective for improving bone density when supplemented along with calcium
Yes
128
36.30%
No
189
53.50%
Don't Know
36
10.20%
Vitamin D supplementation lowers the risk of premature mortality
Yes
210
59.30%
No
57
16.10%
Don't Know
87
24.60%
A serum 25(OH)D level of less than 30ng/mL (75nmol/L) is indicative of vitamin D deficiency
Yes
239
67.50%
No
102
28.80%
Don't Know
13
3.70%
A serum 25(OH)D level less than 20ng/mL (50nmol/L) is indicative of vitamin D deficiency
Yes
318
90.10%
No
22
6.20%
Don't Know
13
3.70%
A serum 25(OH)D level greater than 50ng/mL (125nmol/L) may have adverse effects including: increased risks of cardiovascular disease, vascular calcification, falls, frailty, and all-cause mortality
Yes
65
18.50%
No
204
58.00%
Don't Know
83
23.60%
Practice Behavior
Response
N
%
I routinely test almost all of my patients for serum 25(OH) vitamin D
Yes
182
50.80%
No
172
48.00%
Don't Know
4
1.10%
I almost never test my patients for serum 25(OH) vitamin D
Yes
58
16.40%
No
291
82.40%
Don't Know
4
1.10%
I routinely test serum 25(OH)D before prescribing/recommending vitamin D supplementation
Yes
235
65.80%
No
114
31.90%
Don't Know
8
2.20%
I prescribe/recommend vitamin D oral supplementation routinely to all of my patients
Yes
156
43.60%
No
199
55.60%
Don't Know
3
0.80%
I prescribe/recommend vitamin D oral supplementation only to patients who are deficient in vitamin D by laboratory testing
Yes
160
44.80%
No
190
53.20%
Don't Know
7
2.00%
I routinely prescribe/recommend vitamin D oral supplementation to patients with a history of osteoporosis or osteopenia regardless of their serum vitamin D level
Yes
187
52.50%
No
135
37.90%
Don't Know
34
9.60%
Vitamin D supplementation improves the overall health of my patients
Yes
277
77.40%
No
23
6.40%
Don't Know
58
16.20%
I follow my medical society vitamin D testing and prescribing guidelines
Yes
121
34.20%
No
176
49.70%
Don't Know
57
16.10%
When prescribing/recommending oral vitamin D, I routinely adjust the prescribed/recommended dose based on the results of serum 25(OH)D testing
Yes
280
78.90%
No
67
18.90%
Don't Know
8
2.30%
When prescribing/recommending vitamin D, I direct my patients to certain Brands based on the known quality of those brands
Yes
171
48.00%
No
178
50.00%
Don't Know
7
2.00%
The out-of-pocket patient expense of vitamin D supplements limits my willingness to prescribe vitamin D
Yes
42
11.70%
No
304
84.90%
Don't Know
12
3.40%
Table 2: Practice Belief & Practice Frequencies.
Predictors of practice beliefs and practice behaviors
To investigate the relationship between various participant characteristics and practice belief and behavior items, a multinomial logistic regression analysis was performed. This analysis determined the predictive value of being FIM trained, being a physician (MD or DO), having at least 15 years in practice, being in primary care practice, solo practice or being in an academic setting. This data is summarized in Table 3. Detailed Multinomial Logistic Regression Results for Practice Belief and Table 4. Detailed Multinomial Logistic Regression Results for Practice Behavior. Only a portion of practice beliefs had significant predictors. The belief that vitamin D supplementation is only effective for improving bone density when supplemented along with calcium was negatively associated with FIM training. FIM trained practitioners were most likely to disagree with this belief [OR for Yes vs. No, 0.54 (p-value=0.014)]. There was a trend of disagreement with this belief among primary care physicians [OR for Yes vs. No, 0.88 (p-value=0.60)]. The belief that vitamin D supplementation lowers the risk of premature mortality was negatively correlated with being a physician (MD/DO), with physicians more likely to say no to this belief [OR for Yes vs. No, 0.32 (p-value=0.026)]. Also, being in primary care practice predicted a no answer to this belief [OR for Yes vs. No, 0.38 (p-value = 0.006)]. Being in practice for at least 15 years predicted agreement with this belief compared to not knowing [OR for Yes vs. No, 2.22 (p-value = 0.003)]. Agreement with the belief that a serum level of 25(OH)D greater than 50ng/mL (125nmol/L) may have adverse health effects was predicted by FIM training [OR for Yes vs. No, 2.17 (p-value=0.032)].
Practice Belief
Multinomial logistic regression results
Controlling variables p value
Fellowship Alumni
Credential MD YN
15 years in medical practice
Primary Care Practice
Solo Practice
Academic
Vitamin D deficiency is widespread, affecting the majority of the population
likelihood ratio tests p value
0.523
0.965
0.439
Not included
0.214
0.585
Odds ratio (p value) No vs. Yes
1.51 (0.61)
1.06 (0.93)
0.49 (0.21)
1.13 (0.85)
0.62 (0.40)
Odds ratio (p value) Don't know vs. Yes
0.46 (0.31)
1.20 (0.80)
0.84 (0.80)
3.63 (0.068)
0.63 (0.52)
Vitamin D status is accurately assessed by measuring serum 25(OH) vitamin D level
likelihood ratio tests
0.66
0.037
0.280
0.610
0.720
0.058
Odds ratio (p value) No vs. Yes
1.38 (0.40)
1.31 (0.38)
1.40 (0.28)
0.72 (0.39)
0.77 (0.49)
0.55 (0.052)
Odds ratio (p value) Don't know vs. Yes
0.91 (0.84)
0.40 (0.028)
0.67 (0.32)
0.75 (0.59)
0.78 (0.63)
0.51 (0.10)
Monotherapy with Vitamin D is effective for improving bone density
likelihood ratio tests
0.900
0.160
0.150
0.500
0.690
0.270
Odds ratio (p value) No vs. Yes
0.90 (0.78)
0.63 (0.11)
1.61 (0.091)
1.26 (0.49)
1.10 (0.79)
0.63 (0.14)
Odds ratio (p value) Don't know vs. Yes
0.78 (0.64)
1.01 (0.98)
1.00 (1.00)
0.75 (0.61)
1.54 (0.40)
0.56 (0.20)
Vitamin D supplementation is only effective for improving bone density when supplemented along with calcium*
likelihood ratio tests
0.303
0.286
0.086
0.321
0.05
0.007
Odds ratio (p value) No vs. Yes
1.51 (0.17)
1.19 (0.47)
1.14 (0.60)
1.32 (0.35)
0.73 (0.32)
1.86 (0.014)
Odds ratio (p value) Don't know vs. Yes
1.74 (0.28)
1.90 (0.12)
0.49 (0.069)
0.63 (0.44)
2.10 (0.083)
0.68 (0.34)
Vitamin D supplementation lowers the risk of premature mortality*
likelihood ratio tests
0.046
0.009
0.016
0.177
0.589
0.665
Odds ratio (p value) No vs. Yes
3.12 (0.026)
0.65 (0.18)
2.64 (0.006)
0.753 (0.47)
1.48 (0.30)
0.92 (0.81)
Odds ratio (p value) Don't know vs. Yes
1.14 (0.70)
0.45 (0.003)
1.20 (0.50)
0.53 (0.075)
1.12 (0.73)
1.24 (0.44)
A serum 25(OH)D level of less than 30ng/mL (75nmol/L) is indicative of vitamin D deficiency
likelihood ratio tests
0.298
0.749
0.159
0.013
0.569
0.645
Odds ratio (p value) No vs. Yes
0.63 (0.12)
1.05 (0.86)
1.49 (0.12)
0.43 (0.012)
1.26 (0.44)
0.87 (0.58)
Odds ratio (p value) Don't know vs. Yes
0.79 (0.74)
0.66 (0.48)
0.59 (0.37)
0.25 (0.19)
0.63 (0.56)
0.61 (0.41)
A serum 25(OH)D level less than 20ng/mL (50nmol/L) is indicative of vitamin D deficiency
likelihood ratio tests
0.972
0.593
0.461
0.415
0.276
0.315
Odds ratio (p value) No vs. Yes
1.14 (0.82)
0.72 (0.47)
0.60 (0.26)
1.85 (0.22)
0.62 (0.47)
0.57 (0.23)
Odds ratio (p value) Don't know vs. Yes
0.96 (0.96)
0.64 (0.44)
0.69 (0.53)
0.69 (0.64)
0.27 (0.22)
0.55 (0.31)
A serum 25(OH)D level greater than 50ng/mL (125nmol/L) may have adverse effects including: increased risks of cardiovascular disease, vascular calcification, falls, frailty, and all-cause mortality*
likelihood ratio tests
0.410
0.180
0.092
0.071
0.320
0.010
Odds ratio (p value) No vs. Yes
1.59 (0.19)
1.26 (0.44)
0.85 (0.61)
1.01 (0.98)
0.58 (0.13)
1.06 (0.85)
Odds ratio (p value) Don't know vs. Yes
1.56(0.29)
0.76 (0.43)
0.50 (0.053)
0.43 (0.076)
0.62 (0.25)
0.46 (0.032)
Multinomial model significant, p < 0.05
Some predictors were not included to avoid the unexpected singularity problem.
Table 3: Detailed Multinomial Logistic Regression Results for Practice Beliefs.
Practice Behavior
Multinomial logistic regression results
Controlling variables p value
Fellowship Alumni
Credential MD YN
15 years in medical practice
Primary Care Practice
Solo Practice
Academic
I routinely test almost all of my patients for serum 25(OH) vitamin D*
likelihood ratio tests
0.002
Not included
0.083
<0.001
Not included
0.01
Odds ratio (p value) No vs. Yes
2.11 (0.013)
0.69 (0.10)
0.28 (< 0.001)
0.50 (0.004)
Odds ratio (p value) Don't know vs. Yes
0.098 (0.071)
0.16 (0.13)
1.75 (0.67)
0.28 (0.31)
I almost never test my patients for serum 25(OH) vitamin D*
likelihood ratio tests
0.053
Not included
0.149
0.391
0.299
0.155
Odds ratio (p value) No vs. Yes
0.80 (0.56)
1.45 (0.21)
1.56 (0.29)
0.59 (0.12)
1.69 (0.08)
Odds ratio (p value) Don't know vs. Yes
0.058 (0.028)
0.25 (0.28)
4.53 (0.27)
0.93 (0.96)
0.59 (0.68)
I routinely test serum 25(OH)D before prescribing/recommending vitamin D supplementation*
likelihood ratio tests
0.580
0.014
0.005
0.382
0.48
0.905
Odds ratio (p value) No vs. Yes
1.17 (0.61)
1.15 (0.57)
0.83 (0.43)
0.67 (0.18)
1.27 (0.40)
1.05 (0.85)
Odds ratio (p value) Don't know vs. Yes
0.49 (0.38)
0.086 (0.025)
0.062 (0.011)
0.63 (0.69)
0.44 (0.47)
0.74 (0.70)
I prescribe/recommend vitamin D oral supplementation routinely to all of my patients
likelihood ratio tests
0.065
Not included
0.518
Not included
0.849
0.328
Odds ratio (p value) No vs. Yes
1.57 (0.11)
1.17 (0.47)
1.06 (0.83)
0.72 (0.16)
Odds ratio (p value) Don't know vs. Yes
0.16 (0.15)
0.36 (0.43)
2.09 (0.57)
0.49 (0.58)
I prescribe/recommend vitamin D oral supplementation only to patients who are deficient in vitamin D by laboratory testing
likelihood ratio tests
0.246
0.167
0.140
0.851
Not included
0.934
Odds ratio (p value) No vs. Yes
0.64 (0.11)
1.26 (0.30)
0.90 (0.65)
0.87 (0.60)
1.01 (0.98)
Odds ratio (p value) Don't know vs. Yes
0.52 (0.47)
0.31 (0.18)
0.20 (0.063)
0.73 (0.78)
0.72 (0.74)
I routinely prescribe/recommend vitamin D oral supplementation to patients with a history of osteoporosis or osteopenia regardless of their serum vitamin D level*
likelihood ratio tests
0.690
0.993
<0.001
0.863
0.182
0.271
Odds ratio (p value) No vs. Yes
1.19 (0.56)
1.01 (0.97)
0.51 (0.006)
1.16 (0.60)
1.61 (0.12)
1.39 (0.20)
Odds ratio (p value) Don't know vs. Yes
0.79 (0.65)
1.05 (0.90)
0.023 (<0.001)
1.00 (0.99)
2.04 (0.15)
0.79 (0.59)
Vitamin D supplementation improves the overall health of my patients*
likelihood ratio tests
0.095
0.077
0.340
0.191
0.259
0.814
Odds ratio (p value) No vs. Yes
5.86 (0.09)
1.13 (0.80)
2.03 (0.16)
0.31 (0.12)
1.75 (0.27)
1.12 (0.82)
Odds ratio (p value) Don't know vs. Yes
1.12 (0.76)
0.51 (0.029)
1.11 (0.73)
0.78 (0.52)
1.63 (0.16)
0.84 (0.57)
I follow my medical society vitamin D testing and prescribing guidelines*
likelihood ratio tests
0.054
0.011
0.952
0.05
0.172
0.114
Odds ratio (p value) No vs. Yes
1.88 (0.052)
2.12 (0.003)
1.09 (0.75)
2.10 (0.022)
0.95 (0.86)
1.70 (0.046)
Odds ratio (p value) Don't know vs. Yes
0.82 (0.61)
1.26 (0.50)
1.05 (0.88)
1.25 (0.63)
1.86 (0.10)
1.11 (0.77)
When prescribing/recommending oral vitamin D, I routinely adjust the prescribed/recommended dose based on the results of serum 25(OH)D testing*
likelihood ratio tests
0.976
Not included
0.011
Not included
0.843
0.022
Odds ratio (p value) No vs. Yes
1.07 (0.84)
0.47 (0.006)
1.20 (0.60)
0.56 (0.042)
Odds ratio (p value) Don't know vs. Yes
0.94 (0.95)
0.35 (0.16)
1.31 (0.75)
0.20 (0.057)
When prescribing/recommending vitamin D, I direct my patients to certain Brands based on the known quality of those brands*
likelihood ratio tests
0.016
0.018
0.479
<0.001
Not included
0.003
Odds ratio (p value) No vs. Yes
2.12 (0.012)
1.78 (0.017)
1.12 (0.64)
0.31 (<0.001)
0.44 (0.001)
Odds ratio (p value) Don't know vs. Yes
0.47 (0.36)
0.39 (0.28)
0.44 (0.30)
0.50 (0.53)
0.55 (0.47)
The out-of-pocket patient expense of vitamin D supplements limits my willingness to prescribe vitamin D
likelihood ratio tests
0.915
0.362
0.936
Not included
Not included
0.1
Odds ratio (p value) No vs. Yes
0.99 (0.98)
1.18 (0.64)
0.94 (0.86)
1.89 (0.066)
Odds ratio (p value) Don't know vs. Yes
1.37 (0.72)
0.50 (0.32)
0.78 (0.72)
0.87 (0.85)
Table 4: Detailed Multinomial Logistic Regression Results for Practice Behavior.
In terms of practice behaviors, routinely testing all patients for serum 25(OH)D was inversely associated with being a physician (MD/DO) (OR for Yes vs. No, 0.47 (p-value=0.013)], but positively associated with being in solo practice [OR for Yes vs. No, 3.57 (p-value <0.001)] and FIM training [OR for Yes vs. No, 2.00 (p-value=0.004)]. Similarly, almost never testing patients for serum 25(OH)D levels was positively predicted by being a physician (MD/ DO) [OR for Yes vs. Don’t know, 17.24 (p-value=0.028) with a trend for OR Yes vs. No, 1.25 (p-value 0.56)]. Being in primary care practice predicted recommending vitamin D supplementation to patients with a history of osteoporosis or osteopenia regardless of serum vitamin D level [OR for Yes vs. No, 1.96 (p-value=0.006) and OR for Yes vs. Don’t know, 43.48 (p-value <0.001)]. There were several predictors related to following medical society vitamin D testing and prescribing guidelines. Being in practice for at least 15 years was associated with a 53% odds of not following guidelines [OR for Yes vs. No, 0.47 (p-value=0.003)], being in solo practice was associated with a 52% odds of not following guidelines [OR Yes vs. No, 0.48 (p-value=0.022)], and FIM training was associated with a 41% odds of not following guidelines [OR Yes vs. No, 0.59 (p-value=0.046)]. Routine adjustment of supplemented vitamin D based on the results of serum 25(OH)D testing was strongly predicted by being in a primary care practice [OR Yes vs. No, 2.13 (p-value=0.006)] and by FIM training [OR Yes vs. No, 1.79 (p-value =0.042)]. Directing patients to certain Brands of supplemental vitamin D was predicted by being in primary care practice [OR Yes vs. No, 3.23 (p-value <0.001)] and FIM training [OR Yes vs. No, 2.27 (p-value <0.001)] while being a physician (MD/DO) and having at least 15 years of practice were negatively associated with Brand-specific recommendations [OR Yes vs. No, 0.47 (p-value=0.012) and OR Yes vs. No, 0.56 (p-value 0.017) respectively]. The remaining practice beliefs and behaviors were not predicted by any of the variables.
Dosing
Oral dosing recommendations for Vitamin D3 are presented in Figure 1. Dosing Recommendations which also compares differences in relation to FIM training. The daily dose most likely to be recommended is 2000IU (50mcg), with the majority of FIM trained providers selected this as their typical dose. More FIM practitioners recommend vitamin D3 in doses greater than 800IU (50mcg) whereas non-FIM trained practitioners are slightly more likely to recommend doses lower than 800IU (50mcg). Most indicated out-of-pocket expense did not limit their willingness to recommend Vitamin D (84.9%). Participants were additionally surveyed about conditions for which oral vitamin D3 can be recommended (see Figure 2. Routine Recommendations per Condition). FIM-trained practitioners were consistently more likely to recommend vitamin D for the health conditions, than to not recommend or to respond with “Don’t know”. This pattern of responses held true across conditions including more well-known indications for vitamin D such as osteoporosis as well as lesser known indications such as mood disorders and metabolic syndrome. The survey also asked participants to indicate whether they routinely tested serum 25-hydroxy-vitamin D levels in patients for those same conditions (see Figure 3. Routinely Test per Condition). Consistent with recommended practices, these results indicate that FIM training results in more routine testing for vitamin D in patients with a variety of health conditions.
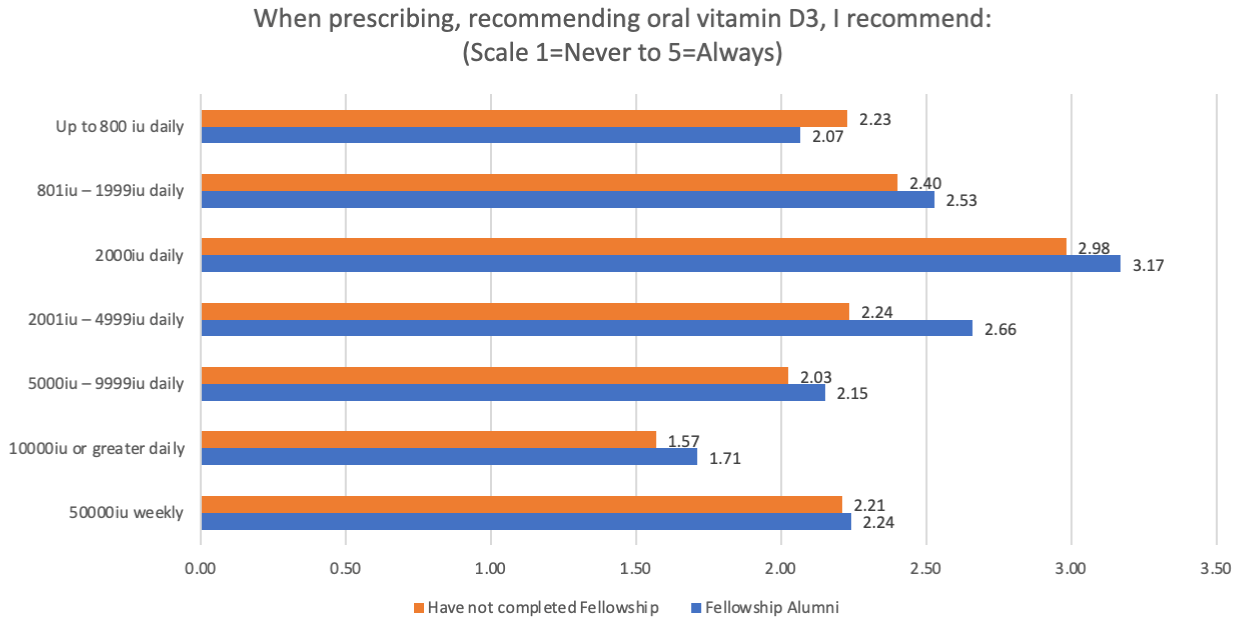
Figure 1: Dosing Recommendations.
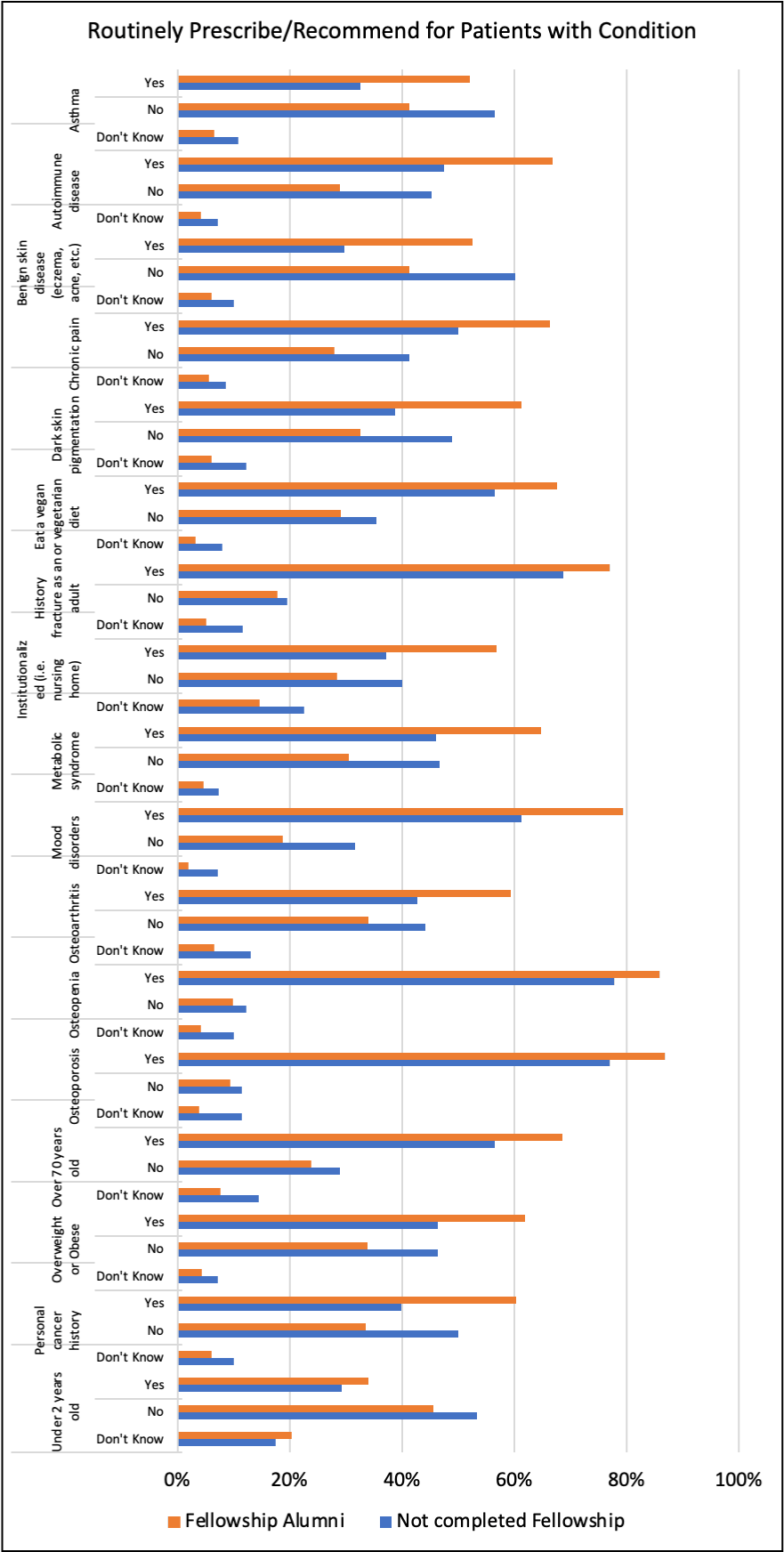
Figure 2: Routine Recommendations per Conditions.
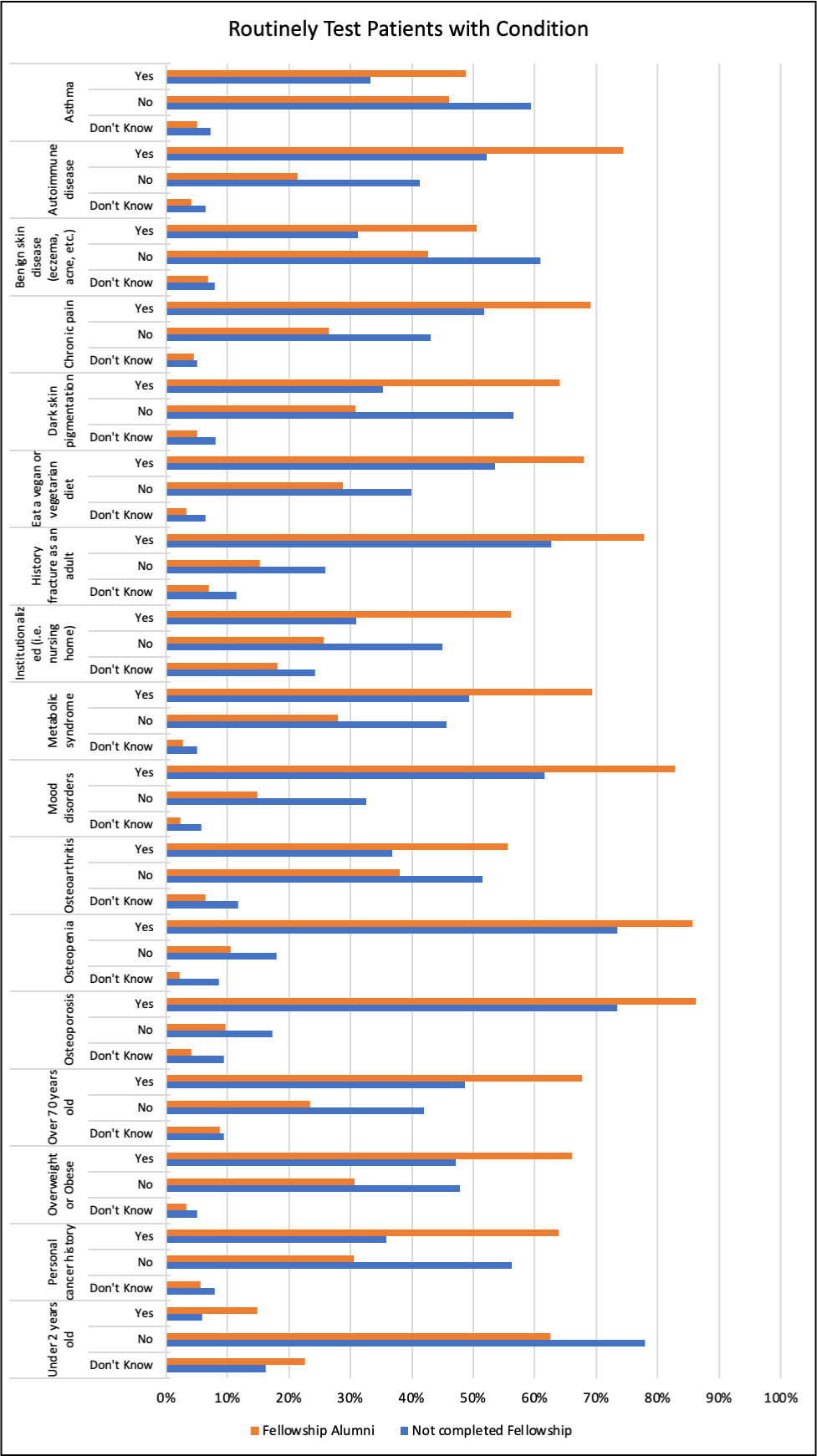
Figure 3: Routinely Test per Condition.
Discussion
In light of increased research and interest in vitamin D, it’s important to understand what influences vitamin D recommendations, especially among HCPs and those with extra training in nutrition, namely those FIM trained HCPs. This is notable given that the majority of participants do not follow their medical society guidelines when testing and prescribing vitamin D, particularly those longest in practice and with FIM training. The association of vitamin D deficiency with premature mortality is not endorsed by physicians or primary care providers, although there was a trend towards agreement with this association among FIM-trained practitioners, those in solo practice and those in practice over 15 years. These divergent beliefs are consistent with a contradictory body of research. A systematic review and meta-analysis published in the July 2019 issue of the British Medical Journal by Zhang Y, et al., which included 52 trials representing 75,454 participants, found that vitamin D supplementation (at varying levels) was not associated with allcause mortality, however it was associated with a 16% reduced risk of death from cancer. The observed lack of benefit on all-cause mortality is in contrast to an earlier 2014 Cochrane review which concluded that vitamin D3 supplementation was associated with a 6% reduction in overall mortality, with number needed to prevent one death equal to 150 people treated[ 41]. The vast majority of participants believe that the majority of the population have vitamin D deficiency. This is in contrast to the actual prevalence of vitamin D deficiency estimated to be 37% of the world’s population and even less in the US population [42]. This discrepancy may be explained by the fact that healthcare practitioners encounter a variety of conditions on a daily basis for which the identification of multiple contributing factors is an important component of management. Practitioners are likely to be familiar with the role of vitamin D in diverse health conditions given the large volume of studies on this topic, thus making vitamin D deficiency a common consideration. Most respondents understand vitamin D deficiency to be serum 25(OH)D < 20 ng/mL (50nmol/L); 2/3 of respondents also identified <30 ng/mL (75nmol/L) as being deficient. This confusion is most likely the result of the oft reported cut-off of 30 ng/mL to achieve desired outcomes [43,44]. This has led to the concept of vitamin D insufficiency, as opposed to deficiency. Vitamin D insufficiency is considered actionable by many HCPs and most often results in a vitamin D recommendation, as suggested in the survey; commonly 2000IU vitamin D3 orally. Those with FIM training are most likely to routinely test patients, across multiple conditions, for vitamin D status and to use testing to adjust vitamin D dosing recommendations. This is consistent with the precept of personalized medicine that is found in integrative medicine training. When recommending oral vitamin D3, FIM-trained practitioners as well as primary care practitioners are most likely to direct their patients to specific Brands. This suggests an awareness on the part of these practitioners of the influence of dietary supplement quality on the efficacy of vitamin D supplementation. FIM training and primary care practice were each negatively associated with the belief that vitamin D was only effective for improving bone density when used in combination with calcium. This suggests a high reliance on vitamin D for bone strengthening despite published data that suggests the combination of calcium and vitamin D are necessary. The evidence continues to grow that vitamin D supplementation, as a monotherapy, is not an evidence-based recommendation for preservation of bone density or for reducing fractures in non-osteoporotic older individuals with sufficient serum vitamin D [45]. Importantly, there is ample clinical evidence that supports the use of supplemental vitamin D with calcium, especially in older individuals who are insufficient in vitamin D (serum 25(OH) vitamin D lower than 30 nmol/L) to lower fracture risk [46,47,48]. Two conditions included in the survey, osteoarthritis and benign skin disease, are not associated with vitamin D deficiency or remediation with supplementation. These were included to test the discriminatory ability of the respondents. More than half of the FIM trained respondents routinely test and recommend vitamin D levels for these conditions in contrast to non-FIM trained practitioners. This could reflect a bias towards using vitamin D indiscriminately, however it may be explained by vitamin D being associated with pain reduction, which typically accompanies osteoarthritis and reduced inflammation which may underlie even benign skin conditions.
Limitations
The main study limitation is the lack of generalizability to all primary care HCPs. The self-selection bias of this group, HCPs who show an interest in IM, are more likely to be open to the idea of nutrition and vitamin D supplementation as beneficial. Another limitation is the heterogeneity in the FIM trained group compared to the non-FIM trained group. The FIM trained group were longer in practice, in solo practice and primary care, and there were more MD/DOs. However, the multinomial regression analysis was able to separate the influence of these characteristics on vitamin D beliefs and practices. Several study features are the primary strengths of this study, namely the availability of comparison groups: FIM vs. non- FIM, using multinomial regression to explore ‘don’t know’ answers regarding beliefs and behaviors in vitamin D clinical practices, and an adequate sample size in this high work-load population. Furthermore, this survey highlights the practice beliefs and patterns regarding vitamin D among a group of practitioners with extensive education in the safety and efficacy of prescribing supplements, as well as drug/nutrient interactions. These findings reliably identify vitamin D testing and recommending behaviors associated with increased awareness and training in this area. Given the significant amount of research on health impacts of vitamin D and the public health importance of adequacy, this survey demonstrates that HCPs believe that vitamin D deficiency is widespread, that testing 25(OH)D is an accurate way to assess vitamin D status and that recommending vitamin D is indicated in a variety of conditions. The favorable impression of the role of vitamin D in health optimization overall is evident.
Conclusion
This survey found that most HCPs routinely test and recommend vitamin D for their patients. Additionally, most HCPs test 25(OH) D levels and recommend vitamin D3 for diseases that are influenced by vitamin D status. The majority of HCPs rely on serum 25(OH)D levels as a reliable method to assess for vitamin D status. IM trained HCPs are more likely to test and recommend vitamin D3 for diseases associated with known vitamin D deficiency. Vitamin D insufficiency is considered actionable by many HCPs and most often results in a vitamin D recommendation, as suggested in the survey; commonly 2000IU vitamin D3 orally. Whether, and how, adherence to society guidelines would affect these beliefs and practices is hard to determine given the divergence between guidelines, and the conflictual literature upon which these guidelines are based. In light of this, practitioners must rely upon their own interpretation of the body of data on vitamin D. This data is voluminous precluding careful and comprehensive scrutiny by actively practicing practitioners. Thus, additional nutritional and integrative medicine training is one way to familiarize practitioners with this body of data. More instruction at all levels of education needs to be prioritized given the numerous health issues associated with vitamin D status.
Declarations
Acknowledgements: This study was reviewed by University of Arizona Research, Discovery & Innovation Human Subjects Protection Program on Jan. 24, 2020 and was given the regulatory status of: Exempt Approval 45 CFR 46.104(d) (2) and Limited IRB Review 45 CFR 46.111(a) (7) for Exempt 45 CFR 46.104(d) (2), 45 CFR 46.104(d) (3) or 45 CFR 46.104(d) (8).
Source of funding: This study was funded by Pharmavite, LLC.
Conflicts of interest: Prior to initiating this study, Lise Alschuler received consultancy fees from Pharmavite, LLC for her participation in a clinical communication workshop regarding soy isoflavones. The focus of that workshop did not include any discussions or information related to vitamin D or to the work reported here. Lise Alschuler has received speaking fees from Naturaceutical Corporation and from Gaia Herbs. Neither of these entities had any involvement in the work reported here. These interests have been disclosed to the University of Arizona and reviewed in accordance with its conflict of interest policies. Keri Marshall is the Director of Medical and Scientific Communications for Pharmavite, a company that manufactures vitamin D and which provided funding for this study.
Data availability statement: The data underlying this article are available in the article and any additional data will be shared on reasonable request to the corresponding author.
References
- U.S. Department of Health and Human Services and U.S. Department of Agriculture. 2015 – 2020 Dietary Guidelines for Americans. 8th Edition. December 2015.
- Parva NR, Tadepalli S, Singh P, Qian A, Joshi R, Kandal H, et al. Prevalence of Vitamin D Deficiency and Associated Risk Factors in the US Population (2011-2012). Cureus. 2018; 10: e2741.
- Herrick KA, Storandt RJ, Afful J, Pfeiffer CM, Schleicher RL, Gahche JJ, et al. Vitamin D status in the United States, 2011-2014. Am J Clin Nutr. 2019; 110: 150-157.
- Illescas-Montes R, Melguizo-Rodríguez L, Ruiz C, Costela-Ruiz VJ. Vitamin D and autoimmune diseases. Life Sci. 2019; 233: 116744.
- Samuel L, Borrell LN. The effect of body mass index on optimal vitamin D status in U.S. adults: the National Health and Nutrition Examination Survey 2001-2006. Ann Epidemiol. 2013; 23: 409-414.
- Hilger J, Friedel A, Herr R, Rausch T. A systematic review of vitamin D status in populations worldwide. Br J Nutr. 2014; 111: 23-45.
- Ross CA, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, et al. The 2011 Report on Dietary Reference Intakes for Calcium and Vitamin D from the Institute of Medicine: What Clinicians Need to Know. J Clin Endocrinol Metab. 2011; 96: 53-58.
- Chapuy MC, Arlot ME, Duboeuf F, Brun J, Crouzet B, Arnaud S, et al. Vitamin D3 and calcium to prevent hip fractures in the elderly women. New England Journal of Medicine. 1992; 327: 1637-1642.
- Chapuy MC, Pamphile R, Paris E, Kempf C, Schlichting M, Arnaud S, et al. Combined calcium and vitamin D3 supplementation in elderly women: confirmation of reversal of secondary hyperparathyroidism and hip fracture risk: the Decalyos II study. Osteoporosis International. 2002; 13: 257-264.
- Boonen S, Lips P, Bouillon R, Bishchoff-Ferrari H, Vanderschueren D, Haentjens P. Need for additional calcium to reduce the risk of hip fracture with vitamin D supplementation: Evidence from a comparative meta-analysis of randomized controlled trials. Journal of Clinical Endocrinology and Metabolism. 2007; 92: 1415-1423.
- Christakos S, Dhawan P, Verstuyf A, Verlinden L, Carmeliet G. Vitamin D: Metabolism, Molecular Mechanism of Action, and Pleiotropic Effects. Physiol Rev. 2016; 96: 365-408.
- Lips P. Vitamin D Physiology. Prog Biophys Mol Biol. 2006; 92: 4-8.
- Skrajnowska D, Bobrowska-Korczak B. Potential Molecular Mechanisms of the Anti-cancer Activity of Vitamin D. Anticancer Res. 2019; 39: 3353-3363.
- Prietl B, Treiber G, Pieber TR, Amrein K. Vitamin D and immune function. Nutrients. 2013; 5: 2502-2521.
- Mousa A, Naderpoor N, de Courten MPJ, Scragg R, de Courten B. 25-hydroxyvitamin D is associated with adiposity and cardiometabolic risk factors in a predominantly vitamin D-deficient and overweight/obese but otherwise healthy cohort. J Steroid Biochem Mol Biol. 2017; 173: 258-264.
- Colotta F, Jansson B, Bonelli F. Modulation of inflammatory and immune responses by vitamin D. J Autoimmun. 2017; 85: 78-97.
- Kahwati LC, LeBlanc E, Weber RP, Giger K, Clark R, Suvada K, et al. Screening for Vitamin D Deficiency in Adults: Updated Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA. 2021; 325: 1443-1463.
- Manson JE, Cook NR, Lee IM, Christen W, Bassuk SS, Mora S, et al. Vitamin D Supplements and Prevention of Cancer and Cardiovascular Disease. N Engl J Med. 2019; 380: 33-44.
- Zittermann A, Trummer C, Theiler-Schwetz V, Lerchbaum E, März W, Pilz S. Vitamin D and Cardiovascular Disease: An Updated Narrative Review. Int J Mol Sci. 2021; 22: 2896.
- Zhang Y, Fang F, Tang J, Jia L, Feng Y, Xu P, et al. Association between vitamin D supplementation and mortality: systematic review and metaanalysis. BMJ. 2019; 366: 14673.
- Manson JE. op. cit. 2019
- Scragg R, Khaw KT, Toop L, Sluyter J, Lawes CMM, Waayer D, et al. Monthly High-Dose Vitamin D Supplementation and Cancer Risk: A Post Hoc Analysis of the Vitamin D Assessment Randomized Clinical Trial. JAMA Oncol. 2018; 4: e182178.
- Toffanello ED, Sergi G, Veronese N, Perissinotto E, Zambon S, Coin A, et al. Serum 25-hydroxyvitamin d and the onset of late-life depressive mood in older men and women: the Pro.V.A. study. J Gerontol A Biol Sci Med Sci. 2014; 69:1554-1561.
- Okereke OI, Reynolds CF 3rd, Mischoulon D, Chang G, Vyas CM, Cook NR, et al. Effect of Long-term Vitamin D3 Supplementation vs Placebo on Risk of Depression or Clinically Relevant Depressive Symptoms and on Change in Mood Scores: A Randomized Clinical Trial. JAMA. 2020; 324: 471-480.
- Antico A, Tampoia M, Tozzoli R, Bizzaro N. Can supplementation with vitamin D reduce the risk or modify the course of autoimmune diseases? A systematic review of the literature. Autoimmun Rev. 2012; 12: 127-136.
- Pereira-Santos M, Costa PR, Assis AM, Santos CA, Santos DB. Obesity and vitamin D deficiency: a systematic review and meta-analysis. Obes Rev. 2015; 16: 341-349.
- Li X, Liu Y, Zheng Y, Wang P, Zhang Y. The Effect of Vitamin D Supplementation on Glycemic Control in Type 2 Diabetes Patients: A Systematic Review and Meta-Analysis. Nutrients. 2018; 10: 375.
- Prasad P, Kochhar A. Interplay of vitamin D and metabolic syndrome: A review. Diabetes Metab Syndr. 2016; 10: 105-112.
- Ross CA. op cit. 2011.
- Vieth R and Holick MF. Chapter 57B - The IOM-Endocrine Society Controversy on Recommended Vitamin D Targets: In Support of the Endocrine Society Position. Vitamin D (Fourth Edition), Vol. 1: Biochemistry, Physiology and Diagnostics, 2018: 1091-1107.
- LeFevre ML, LeFevre NM. Vitamin D Screening and Supplementation in Community-Dwelling Adults: Common Questions and Answers. Am Fam Physician. 2018; 97: 254-260.
- Kahwati LC. op. cit. 2021.
- Holick MF, Binkley NC, Bishoff-Ferrari HA, et al. Evaluation, Treatment, and Prevention of Vitamin D Deficiency: an Endocrine Society Clinical Practice Guideline. J Clin Endocrinol Metab. 2011; 96: 1911-1930.
- Carter GD. 25-hydroxyvitamin D: a difficult analyte. Clin Chem. 2012; 58: 486-488.
- Sempos CT, Heijboer AC, Bikle DD, Bollerslev J, Bouillon R, Brannon PM, et al. Vitamin D assays and the definition of hypovitaminosis D: results from the First International Conference on Controversies in Vitamin D. Br J Clin Pharmacol. 2018; 84: 2194-2207.
- Wang TJ, Pencina MJ, Booth SL, Jacques PF, Inglesson E, Lanier K, et al. Vitamin D deficiency and risk of cardiovascular disease. Circulation. 2008; 117: 503-511.
- Melamed ML, Michos ED, Post W, Astor B. 25-hydroxyl Vitamin D Levels and the Risk of Mortality in the General Population. Arch Intern Med. 2008; 168: 1629-1637.
- Mulcahy KB, Trigoboff E, Opler L, Demler TL. Physician Prescribing Practices of Vitamin D in a Psychiatric Hospital. Innov Clin Neurosci. 2016; 13: 21-27.
- Srinivasan S, O'Rourke J, Golas SB, Neumeyer A, Misra M. Calcium and Vitamin D Supplement Prescribing Practices among Providers Caring for Children with Autism Spectrum Disorders: Are We Addressing Bone Health? Autism Res Treat. 2016; 2016: 6763205.
- Zhang Y. op cit. 2019.
- Bjelakovic G, Gluud LL, Nikolova D, Whitfield K, Wetterslev J, Simonetti R, et al. Vitamin D supplementation for prevention of mortality in adults. Cochrane Database Syst Rev. 2014; 1: CD007470.
- Hilger J, Friedel A, Herr R, Rausch T. A systematic review of vitamin D status in populations worldwide. Br J Nutr. 2014; 111: 23-45.
- Cranney A, Horsley T, O'Donnell S, Weiler H, Puil L, Ooi D, et al. Effectiveness and safety of vitamin D in relation to bone health. Evid Rep Technol Assess (Full Rep). 2007; 158: 1-235.
- Leidig-Bruckner G, Roth HJ, Bruckner T, Lorenz A, Raue F, Frank-Raue K. Are commonly recommended dosages for vitamin D supplementation too low? Vitamin D status and effects of supplementation on serum 25-hydroxyvitamin D levels--an observational study during clinical practice conditions. Osteoporos Int. 2011; 22: 231-240.
- Burt LA, Billington EO, Rose MS, Raymond D, Hanley D, Boyd S. Effect of High-Dose Vitamin D Supplementation on Volumetric Bone Density and Bone Strength: A Randomized Clinical Trial. JAMA. 2019; 322:736-745.
- Chapuy MC. op cit. 1992.
- Chapuy MC. op cit. 2002.
- Boonen S. op cit. 2007.
